CADTH Reimbursement Review
Pembrolizumab (Keytruda)
Sponsor: Merck Canada Inc.
Therapeutic area: Triple-negative breast cancer
This multi-part report includes:
Clinical Review
Pharmacoeconomic Review
Stakeholder Input
Clinical Review
Abbreviations
AE
adverse event
APaT
all patients as treated
CBCN
Canadian Breast Cancer Network
CI
confidence interval
CIV
central imaging vendor
CPS
combined positive score
CrI
credible interval
DOR
duration of response
ECOG PS
Eastern Cooperative Oncology Group Performance Status
EORTC QLQ-BR23
European Organisation for Research and Treatment of Cancer Breast Quality of Life Questionnaire – Breast Module 23
EORTC QLQ-C30
European Organisation for Research and Treatment of Cancer Quality of Life Questionnaire Core 30
EQ VAS
EQ visual analogue scale
ER
estrogen receptor
HR
hazard ratio
HRQoL
health-related quality of life
IA1
interim analysis 1
IA2
interim analysis 2
ITC
indirect treatment comparison
ITT
intention-to-treat
mBC
metastatic breast cancer
MID
minimal important difference
mTNBC
metastatic triple-negative breast cancer
NMA
network meta-analysis
OH-CCO
Ontario Health – Cancer Care Ontario
ORR
objective response rate
OS
overall survival
PD-1
programmed cell death 1 protein
PD-L1
programmed cell death 1 ligand 1
PFS
progression-free survival
PR
progesterone receptor
QoL
quality of life
RBC
Rethink Breast Cancer
RCT
randomized controlled trial
RECIST 1.1
Response Evaluation Criteria in Solid Tumours Version 1.1
SAE
serious adverse event
TNBC
triple-negative breast cancer
TOHCC
The Ottawa Hospital Cancer Centre
Executive Summary
An overview of the submission details for the drug under review is provided in Table 1.
Item | Description |
|---|---|
Drug product | Pembrolizumab (Keytruda), 200 mg IV every 3 weeks, or 400 mg IV every 6 weeks |
Indication | In combination with chemotherapy for the treatment of adult patients with locally recurrent unresectable or metastatic TNBC who have not received prior chemotherapy for metastatic disease and whose tumours express PD-L1 as determined by a validated test (CPS ≥ 10) |
Reimbursement request | As per indication |
Health Canada approval status | NOC |
Health Canada review pathway | Advance consideration under NOC/c |
NOC date | November 19, 2021 |
Sponsor | Merck Canada |
CPS = combined positive score; NOC = Notice of Compliance; NOC/c = Notice of Compliance with conditions; PD-L1 = programmed cell death 1 ligand 1; TNBC = triple-negative breast cancer.
Source: Sponsor-submitted reimbursement package.
Introduction
Triple-negative breast cancer (TNBC) is an invasive form of breast cancer affecting 10% to 20% of patients with breast cancer.1,2 TNBC is distinguished by the absence of an estrogen receptor (ER) and progesterone receptor (PR) and little to no expression of the gene for human epidermal growth factor receptor 2 (HER2).3-5 The disease is most common in females under 40 years of age, Black females, and females with a BRCA1 mutation.2,3 Diagnosis of metastatic triple-negative breast cancer (mTNBC) is based on imaging tests (i.e., mammogram, breast ultrasound, and MRI), clinical symptoms, and biopsy to confirm breast cancer with negative results on all 3 tests (ER, PR, and HER2). Metastatic TNBC differs from other types of invasive breast cancer in that it tends to grow and spread faster, has fewer treatment options, and tends to have a worse prognosis. The predicted 5-year survival rate is 12% for mTNBC compared to 77% for all TNBC and 89% for all breast cancer.6-8
The standard approach for mTNBC is treatment with single-drug chemotherapies such as taxanes and gemcitabine plus carboplatin.9 The median overall survival (OS) for patients with mTNBC treated with conventional chemotherapy is 9 to 13 months.10-13 Combination chemotherapy may be used in patients with progressive or higher burden of disease, such as rapidly progressive visceral disease.9 No approved targeted treatments are currently available.9 Immunotherapy (in combination with chemotherapy) is considered a potential targeted treatment option for patients who have programmed cell death 1 ligand 1 (PD-L1) expression. According to the experts consulted by CADTH, patients who have a higher PD-L1–positive combined positive score (CPS) may be more likely to benefit from treatment regimens that use immunotherapies in combination with chemotherapy compared with chemotherapy alone.
Pembrolizumab is an immunoglobulin G4 monoclonal antibody against programmed cell death 1 protein (PD-1). By inhibiting the PD-1 receptor from binding to its ligands expressed on T cells, pembrolizumab restores cytotoxic T-cell effector function.14 Combinations of pembrolizumab and chemotherapy have been studied in an effort to enhance the antitumour activity of single drugs by creating a tumour microenvironment that stimulates responses to immunotherapy.14
The objective of this report is to perform a systematic review of the beneficial and harmful effects of pembrolizumab plus chemotherapy in adult patients with locally recurrent unresectable or mTNBC who have not received prior chemotherapy for metastatic disease and whose tumours express PD-L1 as determined by a validated test (CPS ≥ 10).
Stakeholder Perspectives
The information in this section is a summary of input provided by the patient groups who responded to CADTH’s call for patient input and clinician group input, and from clinical experts consulted by CADTH for the purpose of this review.
Patient Input
Two patient groups, the Canadian Breast Cancer Network (CBCN) and Rethink Breast Cancer (RBC) provided input for this review. The CBCN collected patient input via 2 online surveys in patients in Canada with mTNBC (survey 1: 2017, n = 14; survey 2: 2012, n = 87 [71 patients and 16 caregivers]) and a grey literature search. None of the respondents from the CBCN surveys had direct experience with pembrolizumab. The RBC input was based on general observations and insights gathered through various ongoing initiatives (including patients’ blogs, virtual support groups, working groups, patient advisory boards, peer-support networks, Instagram, and scientific advisory committees), as well as online surveys (N = 78), Zoom videoconference interviews (n = 7), one-on-one interviews (n = 2; 1 had experience with pembrolizumab), and 2 testimonials from patients in Canada with mTNBC.
In the CBCN submission, patients highlighted the negative impacts of metastatic breast cancer symptoms, such as fatigue (reported by 54%), insomnia (39%), and pain (37%). The majority of respondents experienced metastases to their lungs (N = 10), followed by metastases to other parts of their bodies (e.g., bones, liver, and brain). These symptoms and metastases impose a heavy physical, emotional, psychosocial, and financial toll and can negatively affect health-related quality of life (HRQoL). Respondents from the CBCN surveys acknowledged that currently available treatments for mTNBC have only been shown to prolong the progression-free period and highlighted the decreasing response rates in later lines of therapy; while the disease will eventually progress, patients seek to live their remaining months and years with the best possible HRQoL. The input provided by RBC indicated that, particularly for patients who are diagnosed at a young age, TNBC may have detrimental effects on patient well-being in terms of fertility, childcare, relationships, body image, social activities, employment, and mental health.
Patients from both groups expressed a need for new treatments that prolong survival, control disease, and maintain quality of life. The RBC submission suggested that patients value long-term health outcomes over immediate concerns such as reducing symptoms or managing side effects. CBCN respondents expected new treatments to improve disease control and quality of life, delay disease progression, have minimal side effects, and be affordable with easy access to treatment.
One patient with mTNBC from RBC who had direct experience with pembrolizumab treatment stated that the drug had helped control the disease, shrink tumour size, and improve HRQoL.
Clinician Input
Input From Clinical Experts Consulted by CADTH
According to the clinical experts, improvement in survival and quality of life (QoL) remain the most important unmet needs in patients with mTNBC. The clinical experts agreed that pembrolizumab would be used in the first-line setting for the treatment of mTNBC. In the opinion of the clinical experts, pembrolizumab with chemotherapy would be the new standard of care and would replace current treatment (e.g., chemotherapy alone), rather than being reserved for patients who are intolerant to existing treatments. The clinical experts advised that patients best suited for treatment with pembrolizumab combined with chemotherapy are those who meet the inclusion criteria of the KEYNOTE-355 study. In particular, those patients with a CPS of 10 or higher would be eligible for pembrolizumab. The clinical experts advised that patients least suitable for pembrolizumab included those who are unfit, frail, have a poor Eastern Cooperative Oncology Group Performance Status (ECOG PS), or have active autoimmune disease. The experts indicated that radiological and clinical investigations are used to evaluate response on a regular basis. The experts also noted that PD-L1 status has proven to be predictive of benefit in metastatic cases. The most common assessment modality is shrinkage of tumour on clinical and/or radiological tests. The clinical experts stated that disease progression (tumour enlargement unless pseudoprogression is suspected) and the occurrence of intolerable adverse events (AEs) would be considered when choosing treatment discontinuation. The clinical experts stated that prescription decisions depend on the prescribing centre’s comfort level with administration of the drug and ability to handle side effects.
Clinician Group Input
Input from 3 clinician groups was provided: Ontario Health – Cancer Care Ontario (OH-CCO) Breast Cancer Drug Advisory Committee (based on input from 1 clinician); breast cancer medical oncologists in Canada, led by The Ottawa Hospital Cancer Centre (TOHCC) (based on input from 6 medical oncologists); and the Provincial Breast Tumour Group (Alberta) (based on input from 2 medical oncologists). OH-CCO’s Drug Advisory Committee provides timely evidence-based clinical and health-system guidance on drug-related issues in support of Cancer Care Ontario’s mandate, including the Provincial Drug Reimbursement Programs and the Systemic Treatment Program. The TOHCC group consists of medical oncologists throughout Canada with an expertise in breast oncology and in particular systemic therapies in advanced TNBC. The Provincial Breast Tumour Group (Alberta) is responsible for treating patients with TNBC in Alberta.
The clinician groups indicated that the current first-line treatment for mTNBC, cytotoxic chemotherapy (taxane, platinum, and anthracycline), showed limited benefit in fulfilling the treatment goal of delaying disease progression and improving both the duration and quality of a patient’s life. The clinician groups identified an unmet need for more effective and tolerable treatment options in the metastatic setting. OH-CCO emphasized that the lack of CPS testing within the province may delay delivery of test results and the diagnosis of TNBC. The clinician groups all mentioned that pembrolizumab in combination with chemotherapy would fit in the first-line setting in treating patients with mTNBC. The clinician groups anticipated that pembrolizumab with chemotherapy could shift the current treatment paradigm by replacing chemotherapy alone. Patients suitable for pembrolizumab with chemotherapy identified by the clinician groups were those who expressed PD-L1 (CPS ≥ 10), with an ECOG PS of 0 to 2, and time from completion of adjuvant treatment greater than 6 months, which were aligned with the KEYNOTE 355 trial inclusion criteria. Patients least suitable were those who do not have a CPS of 10 or higher in other lines of therapy or had received adjuvant and/or neoadjuvant pembrolizumab for early-stage disease within 12 months, and those with a high risk of adverse toxicity related to immunotherapy.
Clinician groups agreed that treatment response should be measured using assessments based on symptoms, laboratory markers, radiographic scans, and tumour measurements. The appropriate interval for assessments is 3 months. Improvement of organ function (bone, liver, and lung) and severity of symptoms, maintenance or improvement of performance status, tumour radiographic response with either stabilization of disease or response as measured by Response Evaluation Criteria in Solid Tumours Version 1.1. (RECIST 1.1) were considered clinically meaningful responses. Disease progression, intolerable or dangerous toxicity (grade 3 or higher immune-mediated toxicity), and patient preference or refusal should be considered when deciding whether to discontinue treatment of pembrolizumab with chemotherapy. Clinician groups agreed that outpatient settings, such as hospitals or specialty clinics that have oncology specialists (medical oncologists, chemotherapy nurses, or oncology pharmacists) to administer systemic cancer therapies and monitor and manage treatment-related toxicities, are appropriate for treatment. In addition, the clinician groups pointed out that a combination of pembrolizumab and chemotherapy is now considered a new standard of care by internationally accepted guidelines and has been shown to be well tolerated with a manageable toxicity profile and to be highly accepted and valued by patients in Canadian clinical practice; it is therefore imperative that Canadians have access to this treatment.
Overall, the views of the clinician groups were consistent with those of the clinical experts consulted by CADTH.
Drug Program Input
The drug programs provide input on each drug being reviewed through CADTH’s reimbursement review processes by identifying issues that may affect their ability to implement a recommendation. This includes considerations for initiation, discontinuation, and prescribing of therapy, and generalizability. The implementation questions and corresponding responses from the clinical experts consulted by CADTH are summarized in Table 4.
Clinical Evidence
Pivotal Study
Description of Study
The KEYNOTE-355 study is an ongoing, phase III, randomized, multicentre, double-blind, 2-part, placebo-controlled trial. The primary objective of the trial is to evaluate the efficacy and safety of pembrolizumab plus chemotherapy versus placebo plus chemotherapy for patients with locally recurrent inoperable or metastatic TNBC that has not been previously treated with chemotherapy for metastatic disease. The KEYNOTE-355 trial was initiated in August 2016 and has 251 participating centres across 29 countries in North America (5 sites in Canada, N = 34), South America, Europe, Asia, and Australia. The study was conducted in 2 parts. Part 1 was the safety run-in (N = 30), and part 2 was the efficacy evaluation (N = 847). Patients from part 1 were not included in part 2. For the purpose of this CADTH review, only part 2 was evaluated. The 2 primary efficacy outcomes were OS and progression-free survival (PFS) in all patients and patients with PD-L1–positive tumours. Secondary outcomes included objective response rate (ORR), duration of response (DOR), disease control rate, and HRQoL in all patients and patients with PD-L1–positive tumours. The study is considered to have met its primary objective if the combination of pembrolizumab and chemotherapy was superior to placebo and chemotherapy in either PFS or OS in either all patients or in patients with PD-L1–positive tumours (CPS ≥ 1 or CPS ≥ 10) at either an interim analysis or the final analysis (OS only). Given that the indication for the sponsor’s reimbursement request is for patients with a PD-L1 CPS of 10 or higher, this review focuses on patients with a PD-L1 CPS of 10 or higher and all patients for comparison. In total, 1,372 patients were screened, of which 847 were randomized via an interactive voice recognition system in the intention-to-treat (ITT) population at a 2:1 ratio between pembrolizumab plus chemotherapy (N = 566) and placebo plus chemotherapy (N = 281). Randomization was stratified based on 3 stratification factors:
type of chemotherapy on study (paclitaxel or nab-paclitaxel or gemcitabine and carboplatin)
PD-L1 expression at baseline (CPS ≥ 1 or < 1)
prior treatment with the same class of chemotherapy in the neoadjuvant or adjuvant setting (yes or no).
Treatment was to continue until confirmation of progressive disease or death. Both patients and investigators were blinded to study treatments administered during the trial. In total, 75.1% and 38.1% had a tumour-tissue PD-L1 CPS of 1 or higher and 10 or higher, respectively. All patients enrolled were female. The majority of patients were younger than 65 years of age, white, postmenopausal, and had an ECOG PS of 0. There were 3 planned efficacy interim analyses and a final analysis for part 2 of the KEYNOTE-355 trial. The final analysis of the study (data cut-off date of June 15, 2021) was event- and follow-up-time–driven and was to be conducted after approximately 500 OS events had been observed among all patients or after approximately 23 months since the last patient was randomized, whichever was later. The final analysis of ORR results was conducted at interim analysis 1 (IA1) and the final analysis of PFS was conducted at interim analysis 2 (IA2).
The focus of this CADTH review is the final analysis and its consistency with results from IA1 and IA2.
Efficacy
Table 2 presents a summary of efficacy results from the KEYNOTE-355 trial. All efficacy results are reported for the subset of patients with PD-L1–positive tumours (CPS ≥ 10).
Overall Survival
At the final analysis data cut-off (June 15, 2021), the KEYNOTE-355 trial met the success criterion for the primary hypothesis of OS in patients with locally recurrent inoperable or metastatic TNBC and PD-L1–positive tumours (CPS ≥ 10). The median OS was 23.0 months (95% CI, 19.0 to 26.3) in the pembrolizumab plus chemotherapy group and 16.1 months (95% CI, 12.6 to 18.8) in the placebo plus chemotherapy group. The hazard ratio (HR) obtained between pembrolizumab plus chemotherapy versus placebo plus chemotherapy was 0.73 (95% CI, 0.55 to 0.95; P = 0.0093; multiplicity-adjusted, 1-sided nominal alpha = 0.0113). Overall, pembrolizumab plus chemotherapy demonstrated a statistically significant and clinically meaningful improvement in OS that represented a 27% reduction in the risk of death for patients with PD-L1–positive tumours (CPS ≥ 10).
Health-Related Quality of Life
The following questionnaires were used to assess HRQoL: the European Organisation for Research and Treatment of Cancer Quality of Life Questionnaire Core 30 (EORTC QLQ-C30), European Organisation for Research and Treatment of Cancer Quality of Life Questionnaire – Breast Module 23 (EORTC QLQ-BR23) and the EQ visual analogue scale (EQ VAS). Overall, there were no differences between groups in terms of HRQoL on any of the questionnaires.
Progression-Free Survival
At the IA2 data cut-off (December 11, 2019), the KEYNOTE-355 trial met the coprimary end point of PFS in patients with PD-L1–positive tumours (CPS ≥ 10). At IA2, the median PFS was 9.7 months in the pembrolizumab plus chemotherapy and 5.6 months in the placebo plus chemotherapy group. The HR was 0.65, (95% CI, 0.49 to 0.86; 1-sided P value = 0.0012). Based on the prespecified success criteria (alpha = 0.00411), pembrolizumab plus chemotherapy statistical significantly improved PFS compared with placebo plus chemotherapy in patients with a CPS of 10 or higher.
The findings on PFS from the final analysis were consistent with the results at IA2. At the final analysis data cut-off (June 15, 2021), a total of 144 PFS events (65.5%) had occurred in the pembrolizumab plus chemotherapy group compared to 81 events (78.6%) in the placebo plus chemotherapy group in patients with PD-L1–positive tumours (CPS ≥ 10). The HR at final analysis was 0.66 (95% CI, 0.50 to 0.88; P = 0.0018) in patients with a PD-L1 CPS of 10 or higher. The median PFS was 9.7 months (95% CI, 7.6 to 11.3) in the pembrolizumab plus chemotherapy group compared to 5.6 months (95% CI, 5.3 to 7.5) in the placebo plus chemotherapy group in patients with PD-L1–positive tumours (CPS ≥ 10). Overall, pembrolizumab plus chemotherapy continued to show a statistically significant improvement in PFS compared with placebo plus chemotherapy in patients with PD-L1–positive tumours (CPS ≥ 10).
Objective Response Rate
At the final analysis data cut-off, 116 patients (52.7%) had an objective response (95% CI, 45.9 to 59.5%) in the pembrolizumab group compared to 42 patients (40.8%) with an objective response (95% CI, 31.2 to 50.9%) in the placebo group among those with a PD-L1 CPS of 10 or higher. The secondary hypotheses pertaining to ORR in all patients and in patients with a PD-L1 CPS of 1 or higher were tested at IA1 and not formally tested at the final analysis. The ORR for patients with a PD-L1 CPS of 10 or higher was not included in the multiplicity strategy. These ORR results from the final analysis are consistent with the IA1 results. Overall, pembrolizumab plus chemotherapy showed greater improvements in ORR (according to RECIST 1.1 by a blinded independent central review) compared with placebo plus chemotherapy in patients with a PD-L1 CPS of 10 or higher.
Duration of Response
In the final analysis, the median DOR was greater in the pembrolizumab plus chemotherapy group at 12.8 months compared to the placebo plus chemotherapy group at 7.3 months in patients with a PD-L1 CPS of 10 or higher. Median time to response was 1.9 months in both groups. DOR results from the final analysis were consistent with those in the previously reported IA2 results and showed a sustained DOR benefit in the pembrolizumab plus chemotherapy group over a longer duration of follow-up. The proportions of patients with an extended response at 6 months or later and 12 or later months by Kaplan-Meier estimation were 87.1% and 55.5% in the pembrolizumab plus chemotherapy group and 55.5% and 37.9% in the placebo plus chemotherapy group, respectively.
Harms
Table 2 presents a summary of key safety results from the KEYNOTE-355 trial. Overall, almost all patients in the pembrolizumab plus chemotherapy group (99.6%) and in the placebo plus chemotherapy and placebo group (98.2%) reported at least 1 AE by the June 15, 2021, data cut-off. Grade 3 or higher AEs were slightly more common in the pembrolizumab plus chemotherapy group (77.9%) compared to placebo plus chemotherapy (73.7%). The most common AEs in both groups were neutropenia, decreased neutrophil count, anemia, thrombocytopenia, decreased white blood cell count, and leukopenia.
Table 2: Summary of Key Results From Pivotal Study
Outcome | Patients with PD-L1 CPS ≥ 10 | |
|---|---|---|
Pembrolizumab plus chemotherapy | Placebo plus chemotherapy | |
Median follow-up time, months (minimum to maximum) | 20.2 (0.3 to 53.1) | |
Primary outcome — overall survival | ||
Number of events, n (%) | 155 (70.5) | 84 (81.6) |
Median overall survival (95% CI)a | 23.0 (19.0 to 26.3) | 16.1 (12.6 to 18.8) |
Hazard ratio (95% CI)b | 0.73 (0.55 to 0.95) | |
P value | 0.0093c | |
Overall survival rate at month 6, % (95% CI) | 88.6 (83.5 to 92.1) | 88.3 (80.4 to 93.2) |
Overall survival rate at month 12, % (95% CI) | 70.7 (64.1 to 76.2) | 64.1 (54.0 to 72.5) |
Overall survival rate at month 18, % (95% CI) | 58.3 (51.4 to 64.5) | 44.7 (34.9 to 53.9) |
Overall survival rate at month 24, % (95% CI) | 48.2 (41.4 to 54.6) | 34.0 (25.0 to 43.1) |
Secondary outcome — health-related quality of life | ||
EORTC QLQ-C30 | ||
Global health status | ||
Baseline, n | 201 | 94 |
Week 15. N | 166 | 70 |
Change from baseline at week 15, LS mean (95% CI)d | −2.69 (−5.86 to 0.48) | −0.88 (−5.41 to 3.64) |
Difference in LS means (95% CI) | −1.81 (−6.92 to 3.30) | |
P value | 0.4865e | |
Physical functioning | ||
Baseline, n | 201 | 94 |
Week 15. n | 166 | 70 |
Change from baseline at week 15, LS mean (95% CI)d | −6.76 (−9.89 to −3.62) | −5.71 (−10.41 to −1.01) |
Difference in LS means (95% CI) | −1.05 (−6.59 to 4.50) | |
P value | 0.7102e | |
Emotional functioning, n | ||
Change from baseline at week 15, LS mean (95% CI)d | −0.75 (−3.92 to 2.43) | 0.69 (−4.07 to 5.44) |
Difference in LS means (95% CI) | −1.43 (−7.03 to 4.16) | |
P value | 0.6149e | |
EQ VAS | ||
Baseline, n | 201 | 94 |
Week 15, n | 166 | 70 |
Change from baseline to week 15, LS mean (95% CI)d | −5.45 (−8.68 to −2.23) | −5.63 (−10.22 to −1.04) |
Difference in LS means (95% CI) | 0.18 (−5.04 to 5.39) | |
P value | 0.9468e | |
Primary outcome — progression-free survival by BICR assessment | ||
Number of events, n (%) | 144 (65.5) | 81 (78.6) |
Median PFS (95% CI)a | 9.7 (7.6 to 11.3) | 5.6 (5.3 to 7.5) |
Hazard ratio (95% CI)b | 0.66 (0.50 to 0.88) | |
P value | 0.0018f | |
PFS rate at month 3, % (95% CI) | 81.8 (76.0 to 86.4) | 80.2 (71.0 to 86.8) |
PFS rate at month 6, % (95% CI) | 65.0 (58.1 to 71.2) | 46.9 (36.5 to 56.6) |
PFS rate at month 9, % (95% CI) | 52.5 (45.2 to 59.2) | 36.6 (26.9 to 46.4) |
PFS rate at month 12, % (95% CI) | 39.1 (32.0 to 46.1) | 23.0 (14.7 to 32.3) |
Secondary outcome — objective response rate by BICR assessment | ||
Number of objective responses | 116 | 42 |
Objective response rate (%) (95% CI) | 52.7 (45.9 to 59.5) | 40.8 (31.2 to 50.9) |
Treatment difference vs. comparator estimate (95% CI)g | 12.1 (0.4 to 23.4) | |
P value | 0.0213h | |
Secondary outcome — duration of response | ||
Median duration of response | 12.8 (1.6+ to 45.9+) | 7.3 (1.5 to 46.6+) |
Median time to response (range) | 1.9 (1.2 to 11.7) | 1.9 (1.7 to 28.4) |
Extended responsea | ||
≥ 6 months | 82 (81.7) | 23 (59.5) |
≥ 12 months | 49 (55.5) | 14 (37.9) |
Harms | ||
1 or more AEs | 554 (98.6) | 276 (98.2) |
Toxicity grade 3 to 5 AEs | 438 (77.9) | 207 (73.7) |
SAEs | 169 (30.1) | 67 (23.8) |
Death | 17 (3.0) | 5 (1.8) |
WDAEs | 60 (10.7) | 15 (5.3) |
Notable harms | ||
Hypothyroidism | 89 (15.8) | 9 (3.2) |
Hyperthyroidism | 24 (4.3) | 3 (1.1) |
Infusion reactions | 21 (3.7) | 14 (5.0) |
Pneumonitis | 14 (2.5) | 0 |
Colitis | 10 (1.8) | 4 (1.4) |
Nephritis | 3 (0.5) | 0 |
Type 1 diabetes mellitus | 1 (0.2) | 0 |
AE = adverse event; CI = confidence interval; CPS = combined positive score; EORTC QLQ-C30 = European Organisation for Research and Treatment of Cancer Quality of Life Questionnaire Core 30; EQ VAS = EQ visual analogue scale; LS = least squares; PD-L1 = programmed cell death 1 ligand; 1; PFS = progression-free survival; SAE = serious adverse event; WDAE = withdrawal due to adverse event.
Notes: “+” indicates there is no progressive disease by the time of last disease assessment. Data cut-off: June 15, 2021 (final analysis).
aFrom product-limit (Kaplan-Meier) method for censored data.
bBased on Cox regression model with the Efron method of tie handling with treatment as a covariate stratified by chemotherapy on study (taxane vs. gemcitabine and/or carboplatin) and prior treatment with same class of chemotherapy in the (neo)adjuvant setting (yes vs. no).
cThe multiplicity-adjusted, 1-sided, prespecified P value boundary for statistical significance was P = 0.0113. One-sided P value based on log-rank test stratified by chemotherapy on study (taxane vs. gemcitabine and carboplatin) and prior treatment with same class of chemotherapy in the (neo)adjuvant setting (yes vs. no).
dBased on a constrained longitudinal data analysis model with the patient-reported outcome scores as the response variable, and treatment by time point interaction, and stratum (defined by stratification factors of chemotherapy on study [taxane vs. gemcitabine and carboplatin] and prior treatment with same class of chemotherapy in the (neo)adjuvant setting [yes vs. no]) as covariates.
eNominal P value (i.e., the type I error rate has not been controlled). Two-sided P value.
fNominal P value (i.e., the type I error rate has not been controlled); 1-sided P value based on log-rank test stratified by chemotherapy on study (taxane vs. gemcitabine and carboplatin) and prior treatment with same class of chemotherapy in the (neo)adjuvant setting (yes vs. no).
gBased on Miettinen and Nurminen method stratified by chemotherapy on study (taxane vs. gemcitabine and carboplatin) and prior treatment with same class of chemotherapy in the (neo)adjuvant setting (yes vs. no).
hNominal P value. One-sided P value for testing. Null hypothesis: difference in percentage of 0 vs. hypothesis 1: difference in percentage greater than 0. Confirmed responses are included.
Source: Clinical Study Report.15
AEs of grade 3 to 5 reported in at least 5% of patients were also generally similar in both treatment arms; these included neutropenia (30.1% versus 30.2%), decreased neutrophil count (18% versus 20.3%), anemia (18% versus 16.4%), thrombocytopenia (11.2% versus 11.7%), and decreased white blood cell count (10.5% versus 10.3%) in the pembrolizumab plus chemotherapy and pembrolizumab group and placebo plus chemotherapy and placebo group, respectively. Overall, 3.0% and 1.8% of AEs resulted in death in the pembrolizumab plus chemotherapy and the placebo plus chemotherapy groups, respectively. AEs leading to discontinuation of any study intervention were more common in the pembrolizumab plus chemotherapy group (10.7%) than in the placebo plus chemotherapy group (5.3%).
Notable harms were more common in the pembrolizumab plus chemotherapy group compared to placebo plus chemotherapy, except for infusion reactions. The most common notable harms in the pembrolizumab versus placebo chemotherapy group were hypothyroidism (15.8 versus 3.2%), hyperthyroidism (4.3% versus 1.1%), infusion reactions (3.7% versus 5.0%), and pneumonitis (2.5% versus 0).
Critical Appraisal
In the KEYNOTE-355 trial, the consistency between the interim results and final results helped strengthen the robustness of the findings at the final analysis. For example, PFS assessed at the final analysis was not formally tested based on the statistical hierarchy, yet the results were consistent with the results at IA2, in which a statistically significant result was demonstrated. OS and PFS are validated outcomes recommended by the FDA for trials that include patients with TNBC.16 The clinical experts considered these outcomes important for patients with mTNBC in Canadian practice.
A potential concern in the KEYNOTE-355 study included the lack of stratification randomization conducted on patients with a PD-L1 CPS of 10 or higher or lower than 10, which was the primary focus of this reimbursement review (subpopulation of PD-L1 CPS ≥ 10). This may have contributed to imbalances between the treatment arms, particularly potential unknown confounding covariates. The Health Canada Reviewer Report raised the same concern that was addressed by the sponsor by noting that an evaluation and sensitivity analysis of the potential for imbalance in the population with a CPS of 10 or higher was conducted. It was concluded that the impact of not having a CPS of 10 or higher as a stratification factor would be minimal, and the imbalances in baseline factors were limited and did not change the conclusion of the primary analysis. The Health Canada Reviewer Report acknowledged that the sponsor’s responses to this concern were detailed and adequate.17 The HRQoL surveys were conducted at week 15; however, this time point might not be able to capture an accurate picture of patients’ experiences with the combination of pembrolizumab plus chemotherapy for a prolonged period of time. The assessment time point at week 15 was selected to ensure at least 60% completion and 80% compliance with patient-reported outcome assessments to ensure validity of the longitudinal model of change in patient-reported outcome scores over time. Analyses performed on the patient-reported outcomes were noninferential.
The inclusion and exclusion criteria of the KEYNOTE-355 study were considered appropriate and the baseline and demographic characteristics were considered generalizable to Canadian practice by the clinical experts consulted by CADTH for this review. The magnitude of benefit of pembrolizumab in patients who did not meet the inclusion criteria outlined in the KEYNOTE-355 study is uncertain. The choice of chemotherapy and duration of follow-up implemented in the KEYNOTE-355 study were considered appropriate by the experts. The clinical experts noted that the concomitant medications allowed in the KEYNOTE-355 study were also commonly used in Canadian practice and were considered appropriate. The experts did not identify any major concerns and discrepancies between the trial and real-world settings in terms of concomitant medication use and duration of follow-up.
Indirect Treatment Comparison
Description and Methods of Published Network Meta-Analysis
The sponsor-submitted indirect treatment comparison (ITC) involved a systematic review and used a Bayesian NMA to evaluate the relative efficacy and safety of pembrolizumab plus chemotherapy compared to other treatments including nab-paclitaxel or paclitaxel, atezolizumab plus nab-paclitaxel, bevacizumab plus paclitaxel, carboplatin, docetaxel, ixabepilone plus bevacizumab, bevacizumab plus nab-paclitaxel, and pembrolizumab plus nab-paclitaxel or paclitaxel for the first-line treatment of patients, with previously untreated locally recurrent inoperable or metastatic TNBC. The efficacy outcomes of interest were PFS and OS.
Efficacy Results
The sponsor-submitted ITC reported that the results for OS favoured pembrolizumab plus chemotherapy over nab-paclitaxel or paclitaxel (HR = 0.54; 95% credible interval [CrI], 0.36 to 0.82), carboplatin (HR = 0.36; 95% CrI, 0.19 to 0.68) and docetaxel (HR = 0.30; 95% CrI, 0.17 to 0.55).
The sponsor-submitted ITC reported that the results for PFS favoured pembrolizumab plus chemotherapy over nab-paclitaxel or paclitaxel (HR = 0.51; 95% CrI, 0.33 to 0.78) However, pembrolizumab plus chemotherapy was not favoured versus other comparators included in the ITC for PFS.
Critical Appraisal
Due to limited data availability, the sponsor-submitted ITC was not able to obtain and compare baseline patient characteristics between the included trials; it was also not able to estimate between-trial heterogeneity due to the small number of trials in the network. Consequently, there is substantial uncertainty around the ITC results and firm conclusions cannot be drawn on the relative efficacy between pembrolizumab plus chemotherapy and relevant comparators, aside from direct evidence provided by the KEYNOTE-355 study.
Other Relevant Evidence
No long-term extension studies or other relevant studies were included in the sponsor’s submission to CADTH.
Conclusions
One pivotal study (KEYNOTE-355) and 1 sponsor-submitted ITC provided evidence for this review. The OS and PFS benefits observed with pembrolizumab plus chemotherapy versus placebo plus chemotherapy in patients with a PD-L1 CPS of 10 or higher in the KEYNOTE-355 trial were statistically significant, considered clinically meaningful by the clinical experts consulted by CADTH, and aligned with the outcomes important to patient groups. The secondary outcomes, ORR and DOR, were supportive of the observed OS and PFS results. There was no signal suggesting that the addition of pembrolizumab to chemotherapy resulted in a significant decrease in HRQoL from baseline to week 15. The results of the submitted ITC, which compared the efficacy of pembrolizumab plus nab-paclitaxel or paclitaxel to other comparators and results, suggested that OS favoured pembrolizumab plus chemotherapy in a comparison to nab-paclitaxel or paclitaxel, carboplatin, and docetaxel, and PFS favoured pembrolizumab plus chemotherapy in a comparison to nap-paclitaxel and/or paclitaxel, but not to other treatments. However, no firm conclusions could be drawn from the ITC results based on several limitations. No new safety concerns were identified for the use of pembrolizumab plus chemotherapy for the treatment of locally recurrent inoperable or metastatic TNBC. The clinical experts stated that there is experience using pembrolizumab for other indications, and oncologists are familiar with AEs due to pembrolizumab.
Introduction
Disease Background
Breast cancer is the most common cancer among females, with approximately 27,700 new cases reported in 2021.8 TNBC is an invasive form of breast cancer affecting 10% to 20% of patients.1,2 TNBC is most common in women under 40 years, Black females, and females with a BRCA-1 mutation.2,3 TNBC is distinguished by the absence of an ER, PR, and little to no expression of the HER2 gene.3-5 Breast cancer is clinically categorized into early-stage breast cancer (stage I to II), locally advanced (stage II to III), and metastatic breast cancer (stage IV).18 Diagnosis of mTNBC (stage IV) is based on imaging tests (i.e., mammogram, breast ultrasound, or MRI), clinical symptoms, and biopsy to confirm breast cancer, with negative results on all 3 tests (ER, PR, and HER2), as well as PD-L1 status.9 Approximately 5% of patients with TNBC are initially diagnosed with metastatic disease.19 The predicted 5-year survival is 12% for mTNBC compared to 77% for all TNBC and 89% for all breast cancer.7,8
TNBC has the same signs and symptoms as those reported with other common breast cancers, including breast changes such as firm or hard lumps, a lump in the armpit, changes in breast size and shape, changes to the nipple, and discharge from the nipples. Additional symptoms including bone pain, weight loss, nausea, appetite loss, shortness of breath, cough, headache, double vision, and muscle weakness may manifest with tumour size increase or spread to other organs.3,5 Cases of mTNBC differ from other types of invasive breast cancer in that mTNBC tends to grow and spread faster, has fewer treatment options, and tends to have a worse prognosis.3 Tumours in mTNBC often metastasize to the bloodstream, brain, and lungs rather than the bones and lymph nodes, which is common in breast cancers that are not triple-negative.20 The clinician groups consulted during the review emphasized that patients with TNBC have a higher risk of recurrence and death compared to those with other types of breast cancer. More than 50% of patients with mTNBC (stage IV) are likely to experience recurrence, of whom 37% will die in the first 5 years following surgery.1
Breast cancers can be diagnosed during screening exams using mammograms. In most Canadian provinces and territories, organized screening via mammography at 2- to 3-year intervals is available for females aged 50 to 74 years with an average risk of breast cancer. Imaging techniques available include breast ultrasounds and radionuclide imaging. Other diagnostic methods include tissue biopsy examinations, hormone receptor status testing, HER2-status testing, complete blood count, blood chemistry tests, tumour marker tests, X-rays, bone scans, and ductography. A repeat biopsy to reassess HER2, ER, and PR, and PD-L1 status is recommended for patients with mTNBC.9
Standards of Therapy
The clinical experts and clinician groups consulted during the CADTH review indicated that the standard approach for mTNBC is sequential cytotoxic chemotherapy, including paclitaxel, nab-paclitaxel, docetaxel, gemcitabine, carboplatin, cisplatin, and vinorelbine. Typically, monotherapy is used rather than combination therapy, with the exception of gemcitabine, which is frequently combined with a platinum drug. The median OS for patients with mTNBC treated with conventional chemotherapy is 9 months to 13 months.10-13 Often patients with more progressive disease are treated with combination chemotherapies. No targeted or immunotherapy has yet become standard of care in this population. Pembrolizumab is currently available through a compassionate access program as noted by the KEYNOTE 355 trial indications in the first-line setting.
Preferred treatment options outlined in the National Comprehensive Cancer Network guidelines for patients with TNBC include anthracyclines (doxorubicin or liposomal doxorubicin), taxanes (paclitaxel), and antimetabolites (capecitabine or gemcitabine). For patients with recurrent unresectable or metastatic TNBC who have received 2 prior therapies, the recommended systemic therapy is sacituzumab govitecan,19 which is currently the subject of negotiations by the pan-Canadian Pharmaceutical Alliance.
According to the clinical experts consulted for this review, the most important goal in this context is to improve survival, disease symptoms, function, and QoL. Tumour response for a prolonged duration has also been advocated as being important for patients, especially when this translates to improvements in QoL.
Drug
Pembrolizumab is an immunoglobulin G4 monoclonal antibody against PD-1. By inhibiting the PD-1 receptor from binding to its ligands expressed on T cells, pembrolizumab restores the cytotoxic T-cell effector function.14 Combinations of pembrolizumab and chemotherapy have been studied in an effort to enhance the antitumour activity of single drugs by creating a tumour microenvironment that stimulates responses to immunotherapy.14
Pembrolizumab underwent a standard review at Health Canada and obtained a Notice of Compliance with conditions on November 19, 2021, for the treatment (in combination with chemotherapy) of adult patients with locally recurrent unresectable or mTNBC who have not received prior chemotherapy for metastatic disease, and whose tumours express PD-L1 as determined by a validated test (CPS ≥ 10).21 The sponsor’s reimbursement request is line with the Health Canada indication. On November 13, 2020, the FDA authorized pembrolizumab in combination with chemotherapy for the treatment of patients with locally recurrent unresectable or mTNBC whose tumours express PD-L1 as determined by an FDA-approved test (CPS ≥ 10). Pembrolizumab has been previously reviewed by CADTH for other indications.
The Health Canada–recommended dosage of pembrolizumab in combination with chemotherapy is either 200 mg IV every 3 weeks or 400 mg IV every 6 weeks until disease progression, unacceptable toxicity, or up to 24 months. The alternative dosage is 35 doses for 200 mg or 18 doses for 400 mg, whichever is longer, in patients without disease progression.14 Additionally, the product monograph states that atypical responses (i.e., an initial transient increase in tumour size or small new lesions within the first few months followed by tumour shrinkage) have been observed. Clinically stable patients with initial evidence of disease progression may remain on treatment until disease progression is confirmed.
Key characteristics of commonly used therapies for mTNBC are shown in Table 3.
Table 3: Key Characteristics of Pembrolizumab and Paclitaxel
Characteristic | Pembrolizumab15 | Taxanes (e.g., paclitaxel)22 |
|---|---|---|
Mechanism of action | A high-affinity antibody against PD-1, which exerts dual ligand blockade of the PD-1 pathway, including PD-L1 and PD-L2, on antigen-presenting or tumour cells; by inhibiting the PD-1 receptor from binding to its ligands, pembrolizumab reactivates tumour-specific cytotoxic T lymphocytes in the tumour microenvironment | A novel antimicrotubule drug that promotes the assembly of microtubules from tubulin dimers and stabilizes microtubules by preventing depolymerization; this stability results in the inhibition of the normal dynamic reorganization of the microtubules network that is essential for vital interphase and mitotic cellular functions; in addition, paclitaxel induces abnormal arrays or “bundles” of microtubules throughout the cell cycle and multiple asters of microtubules during mitosis, and in vitro, paclitaxel exhibits cytotoxic activity against a wide variety of both human and rodent tumour cell lines |
Indicationa | In combination with chemotherapy, for the treatment of adult patients with locally recurrent unresectable or metastatic TNBC who have not received prior chemotherapy for metastatic disease and whose tumours express PD-L1 (CPS ≥ 10) as determined by a validated test | Adjuvant treatment of node-positive breast cancer is administered sequentially to standard combination therapy; and as second-line treatment of metastatic breast cancer resistant to the usual treatments |
Route of administration | IV | IV |
Recommended dosage | 200 mg IV fixed dose, every 3 weeks | Administered by continuous IV infusion over 3 hours at a dosage of 175 mg/m2 at 21-day intervals |
Serious adverse effects or safety issues | Immune-mediated adverse reactions such as endocrinopathies nephritis and renal dysfunction, hepatitis, colitis, pneumonitis, severe skin reactions, thyroid disorders, type 1 diabetes mellitus, hypophysis, and adrenal insufficiency | Hypersensitivity reactions. injection-site reactions, hypotension and bradycardia, peripheral neuropathy, arthralgia, or myalgia |
Other | NA | NA |
CPS = combined positive score; NA = not applicable; PD-1 = programmed cell death 1 protein; PD-L1 = programmed cell death 1 ligand 1; PD-L2 = programmed cell death 1 ligand 2; TNBC = triple-negative breast cancer.
aHealth Canada–approved indication.
Sources: Pembrolizumab product monograph14,21 and paclitaxel product monograph.22
Stakeholder Perspectives
Patient Group Input
This section was prepared by CADTH staff based on input provided by patient groups. The full patient group input is included in the Stakeholder section of this review.
Two patient groups, the CBCN and RBC, provided input for this review. The CBCN is a patient-directed charity and a member of the Canadian Cancer Action Network, whose mission is to ensure the best quality of care for all people in Canada affected by breast cancer through the promotion of information, education, and advocacy activities. RBC is a Canadian charity committed to educating, empowering, and advocating for system changes to improve the experience and outcomes of patients with breast cancer, especially for those in underserved groups such as those diagnosed at a younger age, with metastatic breast cancer, and who are systemically marginalized due to race, income, or other factors.
The CBCN collected patient input via 2 online surveys (survey 1: 2017, n = 14 patients in Canada with mTNBC; survey 2: 2012, n = 71 patients in Canada, and n = 16 caregivers of patients in Canada with metastatic breast cancer [mBC]; no respondents had direct experience with pembrolizumab), and a literature review of current studies and grey literature. The input from RBC was based on general observations and insights gathered through various activities (e.g., patient blogs, virtual support groups, working groups, patient advisory boards, peer-support networks, Instagram, and scientific advisory committee meetings); 1 online survey (September 2018 to April 2019, n = 78 patients with mBC); interviews (Zoom videoconferencing, 2022, n = 7 patients with TNBC; one-on-one interviews, 2022, n = 2 patients in Canada with mTNBC, 1 of whom had access to pembrolizumab and 1 of whom was excluded from the pembrolizumab trials due to prior cancer treatment); and meeting and written or online correspondence (2022, n = 1 patient with mTNBC). RBC also shared 2 testimonials from interviews with 2 patients in Canada.
In the CBCN submission, patients emphasized the negative impacts of mBC symptoms such as fatigue (54%), insomnia (39%), and pain (37%). According to the 2017 CBCN survey, of the 14 patients who indicated that they are living with mTNBC, the majority of respondents (10) experienced metastases to their lungs, followed by metastases to other parts of their bodies (6), their bones (5), their liver (3), and their brain (2). These symptoms and metastases impose a heavy physical, emotional, psychosocial, and financial toll, and negatively affect HRQoL. The input provided by RBC indicated that, particularly for patients who are diagnosed at a young age, TNBC may have detrimental effects on patients’ well-being in terms of fertility, childcare, relationships, body image, social activities, employment, and mental health.
According to the 2017 CBCN survey, all 14 patients had been or were currently being treated with chemotherapy, 11 patients previously had surgery, 12 had or were receiving radiation therapy, and 2 had or were currently receiving hormone therapy. The input from patient groups acknowledged that currently available treatments for mBC have only been shown to prolong the progression-free period and emphasized the decreasing response rates in later lines of therapy; while the disease will eventually progress, patients seek to live their remaining months and years with the best possible HRQoL. Patients from both groups identified an unmet need for new treatments for mBC that can prolong survival, control disease, and maintain QoL. The RBC submission suggested that patients value long-term health outcomes over immediate concerns such as reducing symptoms or managing side effects. Patient respondents from CBCN expected new treatments to improve disease control, delay disease progression, improve QoL, have minimal side effects, and be affordable and easy to access.
One patient with mTNBC from RBC who had direct experience with pembrolizumab treatment reported that the drug had helped control the disease, shrink tumour size, and improve HRQoL.
Clinician Input
Input From Clinical Experts Consulted by CADTH
All CADTH review teams include at least 1 clinical specialist with expertise in the diagnosis and management of the condition for which the drug is indicated. Clinical experts are a critical part of the review team and are involved in all phases of the review process (e.g., providing guidance on the development of the review protocol, assisting in the critical appraisal of clinical evidence, interpreting the clinical relevance of the results, and providing guidance on the potential place in therapy). The following input was provided by 2 clinical specialists with expertise in the diagnosis and management of mTNBC.
Unmet Needs
Patients with mTNBC have relatively poor prognoses compared to those with other breast cancer subtypes. Therefore, improvement in survival and/or its quality remain the most important unmet need for many years. Tumour response has also been described as being important for patients, particularly when associated with improvements in QoL. Effective treatments with better tolerance and convenience are sought by patients and oncologists treating mTNBC.
Place in Therapy
According to the clinical experts, pembrolizumab’s unique mechanism of action would create a shift in the treatment paradigm for this population. Pembrolizumab would be used in the first-line setting for the treatment of mTNBC. In the opinion of the clinical experts, pembrolizumab with chemotherapy would be the new standard of care and will replace current treatment (e.g., chemotherapy alone), rather than being reserved for patients that are intolerant to existing treatments. The clinical expert would not recommend patients try other treatments if they present with locally advanced mTNBC that has not previously been treated for that setting.
Patient Population
The clinical experts advised that patients best suited for treatment with pembrolizumab combined with chemotherapy are those who meet the inclusion criteria (e.g., PD-L1 score) of the KEYNOTE-355 study. Patients are identified though PD-L1 antigen testing. Those with a CPS of 10 of higher will be eligible for pembrolizumab. According to the clinical experts, mTNBC is easily diagnosed at most Canadian cancer centres, and no major issues are expected regarding misdiagnosis. Presymptomatic patients can be considered for treatment with pembrolizumab as these represent the majority of the cases. The clinical experts advised that patients least suitable for pembrolizumab included those who are unfit, frail, have a poor ECOG PS, or have active autoimmune disease regardless of tumour size and number nodes. According to the clinical experts, apart from a PD-L1 expression score of greater than 10%, which is a necessary criterion, there are no other reliable predictors of benefit.
Assessing Response to Treatment
The clinical experts indicated that radiological and clinical investigations are used to evaluate response on a regular basis. The experts also noted that PD-L1 status has been predictive of benefit in metastatic cases. The most common assessment modality is the shrinkage of tumour on clinical and/or radiological tests. Other assessments of clinical response include improvement (or no deterioration) of symptoms and patient ability to function and survival. The clinical experts advised that, as long as there is a response, its magnitude is not typically used in treatment decisions. Typical clinical practice is to assess every 3 to 4 cycles of cytotoxic chemotherapy (approximately every 3 months).
Discontinuing Treatment
The clinical experts stated that disease progression (tumour enlargement unless pseudoprogression is suspected) and the occurrence of intolerable AEs would be considered when deciding whether to discontinue treatment.
Prescribing Conditions
The clinical experts advised that prescribing depends on the comfort level of the centre with administration of the drug and handling side effects. Given that pembrolizumab has already been used for a few years in other diseases, most Canadian centres should have a relatively sophisticated understanding of how to deliver this drug safely.
Clinician Group Input
This section was prepared by CADTH staff based on the input provided by clinician groups. The full clinician group input is included in the Stakeholder section of this review.
Input from the following 3 clinician groups was provided: the OH-CCO Breast Cancer Drug Advisory Committee (providing input from 1 clinician), breast cancer medical oncologists in Canada, led by TOHCC (providing input from 6 medical oncologists), and Provincial Breast Tumour Group (Alberta) (providing input from 2 medical oncologists). The OH-CCO’s Drug Advisory Committee provides timely evidence-based clinical and health-system guidance on drug-related issues in support of Cancer Care Ontario’s mandate, including the Provincial Drug Reimbursement Programs and the Systemic Treatment Program. The TOHCC group consists of medical oncologists throughout Canada with an expertise in breast oncology and systemic therapies in advanced TNBC, in particular. The Provincial Breast Tumour Group (Alberta) is responsible for treating patients with TNBC in Alberta.
The clinician groups indicated that the current first-line treatment for mTNBC, cytotoxic chemotherapy (taxane, platinum, and anthracycline), showed limited benefit in delaying disease progression and improving both duration and QoL. The clinician groups identified an unmet need for more effective and tolerable treatment options in the metastatic setting. The OH-CCO noted that the lack of CPS testing within the province may delay the delivery of test results and the diagnosis of TNBC. The clinician groups mentioned that pembrolizumab would fit in the first-line metastatic setting in combination with chemotherapy in treating patients with TNBC. The clinician groups emphasized that pembrolizumab with chemotherapy would be expected to shift the current treatment paradigm by replacing chemotherapy alone. The patients suitable for pembrolizumab with chemotherapy identified by the clinician groups were those who expressed PD-L1 (CPS ≥ 10), with an ECOG PS of 0 to 2 and a time from completion of adjuvant treatment of greater than 6 months, which were aligned with inclusion criteria for the KEYNOTE-355 trial. Patients least suitable were those who do not have a CPS of 10 or higher, those in other lines of therapy, or those who had received adjuvant and/or neoadjuvant pembrolizumab for early-stage disease within 12 months and with a high risk of adverse toxicity related to immunotherapy.
Clinician groups agreed that treatment response should be measured using assessments based on symptoms, laboratory markers, radiographic scans, and tumour measurements. The appropriate interval for assessments is 3 months. Improvement of organ function (bone, liver, and lung) and severity of symptoms, maintenance or improvement of performance status, tumour radiographic response with either stabilization of disease or response by RECIST 1.1 were considered clinically meaningful responses. When deciding whether to discontinue pembrolizumab with chemotherapy treatment, disease progression, intolerable or dangerous toxicity (grade 3 or higher immune-mediated toxicity) and patient preference or refusal should be considered. Clinician groups agreed that outpatient settings, such as hospitals or specialty clinics that have oncology specialists (medical oncologists, chemotherapy nurses, or oncology pharmacists) to administer systemic cancer therapies and monitor and manage treatment-related toxicities, are appropriate. In addition, the clinician groups pointed out that the combination of pembrolizumab and chemotherapy has been considered a new standard of care by internationally accepted guidelines, has been shown to be well tolerated with a manageable toxicity profile, and is highly accepted and valued by patients in Canadian clinical practice; it is therefore imperative that Canadians have access to this treatment.
Drug Program Input
The drug programs provide input on each drug being reviewed through CADTH’s reimbursement review processes by identifying issues that may affect their ability to implement a recommendation. The implementation questions and corresponding responses from the clinical experts consulted by CADTH are summarized in Table 4.
Table 4: Summary of Drug Plan Input and Clinical Expert Response
Drug program implementation questions | Clinical expert responses |
|---|---|
Relevant comparators | |
For first-line treatment of mTNBC, cytotoxic chemotherapy is administered either as a single drug or in combination, particularly for rapidly progressive disease or patients with visceral disease. The most commonly used chemotherapy drugs in Canada include taxanes (paclitaxel, docetaxel, nab-paclitaxel), anthracyclines (doxorubicin or epirubicin), carboplatin or cisplatin plus gemcitabine, vinorelbine, and capecitabine. In some jurisdictions, nab-paclitaxel is only funded if the patient is not able to use a taxane due to a contraindication to the standard premedications or due to severe toxicity or a hypersensitivity reaction to the taxane. | For pERC consideration. |
Considerations for initiation of therapy | |
What is the specific definition of TNBC (i.e., cut-offs for determining ER and/or PR negativity and HER2 negativity) for eligibility for pembrolizumab? | According to the clinical expert, the cut-off value for ER and/or PR negative disease is a protein expression of < 1% on immunohistochemistry; the cut-off value for HER2-negative disease is an immunohistochemistry score of 0 and 1+ or a score of 2+, with a negative result for dual, fluorescence, or silver in situ hybridization. |
In the KEYNOTE-355 study, patients with TNBC cancer who previously completed treatment for stage I to III breast cancer were eligible if at least 6 months had elapsed between completion of treatment with curative intent (e.g., last dose of adjuvant chemotherapy administration if applicable) and documentation of local or distant disease recurrence. Would the same criteria be applicable for pembrolizumab eligibility in this group of patients at the time of diagnosis for advanced TNBC? | In the opinion of the clinical expert, the trial criteria are applicable to Canadian clinical practice. |
If a patient starts with chemotherapy first, can pembrolizumab be added later, provided all other eligibility criteria are met and no disease progression has occurred? (This is a time-limited question at the time of public funding in a province for patients who have started chemotherapy and meet all eligibility criteria, but pembrolizumab was not yet funded when chemotherapy was initiated.) | A short and reasonable window of time (such as within 6 weeks from the initiation of chemotherapy to match a commonly used frequency of pembrolizumab) may be allowed to add pembrolizumab after initiation of chemotherapy (i.e., chemotherapies as used in the KEYNOTE-355 trial in combination with pembrolizumab). |
If a patient received pembrolizumab in the neoadjuvant or adjuvant setting for early-stage TNBC, are they eligible to receive pembrolizumab again at the time of documented local or distant disease recurrence? If so, what time should elapse between completion of neoadjuvant or adjuvant pembrolizumab before being eligible for pembrolizumab again for mTNBC? | In the KEYNOTE-355 trial, 59.8% of patients received prior neoadjuvant or adjuvant chemotherapy. No patient received pembrolizumab in the neoadjuvant or adjuvant setting for early-stage TNBC in the KEYNOTE-355 trial. In the absence of data to inform this decision, the clinical experts noted that re-treatment with pembrolizumab may be reasonable if disease recurrence is ≥ 12 months postcompletion of neoadjuvant or adjuvant treatment with pembrolizumab. |
Considerations for discontinuation of therapy | |
Is there a minimum number of chemotherapy cycles that should be administered with pembrolizumab? If a patient experiences significant toxicity to chemotherapy, can chemotherapy be discontinued and pembrolizumab continued as a single drug? Should chemotherapy be continued for the same duration of pembrolizumab in the absence of unacceptable toxicity? | In the KEYNOTE-355 trial, in patients with a CPS ≥ 10, the median numbers of study treatment administrations were 35.1 and 22.6 in the pembrolizumab and placebo groups, respectively. The median numbers of administrations with each individual study treatment component (pembrolizumab plus chemotherapy vs. placebo plus chemotherapy) were pembrolizumab: 11.0 vs. 8.8, nab-paclitaxel: 23.5 vs. 15.0, paclitaxel: 19.0 vs, 14.0, gemcitabine: 13.0 vs. 14.0, and carboplatin: 13.0 vs. 14.0. According to the KEYNOTE-355 protocol, patients were allowed to discontinue chemotherapy due to toxicity and continue pembrolizumab alone or vice versa. In the trial, 10.7% of patients discontinued pembrolizumab due to an adverse event, and 3.9%, 2.8%, 6.6%, and 7.5% of patients discontinued nab-paclitaxel, paclitaxel, gemcitabine, and carboplatin, respectively, due to an adverse event in the pembrolizumab study group. The clinical experts noted that because no minimum number of chemotherapy cycles was specified in the KEYNOTE-355 trial, the same should apply in clinical practice. Because patients in the KEYNOTE-355 trial were allowed to discontinue chemotherapy due to toxicity and continue pembrolizumab alone or vice versa, the same criteria should apply in clinical practice. According to the KEYNOTE-355 protocol, patients had to discontinue from pembrolizumab or placebo once they completed 35 administrations of pembrolizumab or placebo. However, patients were allowed to continue chemotherapy treatment at the investigator’s discretion. In accordance with the KEYNOTE-355 trial criteria, the clinical experts felt that it should be left up to the discretion of the treating physician to determine if chemotherapy should be continued in clinical practice. |
The requested duration of treatment for pembrolizumab is until disease progression, unacceptable toxicity or up to 24 months (or 35 doses every 3 weeks or 18 doses every 6 weeks), whichever is longer, in patients without disease progression. If pembrolizumab is discontinued for reasons other than disease progression or intolerability after the initial 24 months of treatment, are patients eligible for an additional 12 months of treatment at the time of disease recurrence, similar to other indications for pembrolizumab? Should the same or different chemotherapy (if any) be administered in this situation? | The clinical experts felt that it would be reasonable to re-administer pembrolizumab at the time of relapse (up to 17 additional doses every 3 weeks or 1 year), with or without chemotherapy, at the discretion of the treating physician for patients who have discontinued pembrolizumab before any disease progression or disease progression during a treatment break. These criteria align with a re-treatment phase specified in the KEYNOTE-355 trial protocol (results not available yet). The clinical experts felt that resumption of the same chemotherapy protocol initially administered should be followed. These criteria align with a re-treatment phase specified in the KEYNOTE-355 trial protocol (results not available yet). |
Considerations for prescribing therapy | |
PAG would like to inform pERC that jurisdictions would plan on implementing pembrolizumab as weight-based dosing up to a cap (e.g., 2 mg/kg every 3 weeks to a maximum dose of 200 mg or 4 mg/kg every 6 weeks to a maximum of 400 mg), similar to other indications for consistency. | For pERC consideration. The clinical experts agreed with this approach. |
In the KEYNOTE-355 study, there was a choice of 3 chemotherapy regimens to be administered with pembrolizumab: nab-paclitaxel, paclitaxel, or gemcitabine plus carboplatin. Should the chemotherapy selection be at the discretion of the treating physician following local institutional standards for mTNBC? Is there a preferred chemotherapy? | The clinical expert felt that it was best to base clinical decisions on the evidence. The indication could be adapted as each province sees fit. |
In the KEYNOTE-355 study, patients who received taxane, gemcitabine, or platinum drugs in the neoadjuvant or adjuvant setting could be treated with the same class of chemotherapy if at least 12 months had elapsed between the completion of treatment with curative intent and the first documented local or distant disease recurrence. Should the same time frames be used in clinical practice to determine which chemotherapy backbone to prescribe with pembrolizumab? | The clinical expert agreed that the time frames used in the KEYNOTE-355 trial should be used in Canadian clinical practice as well. |
Generalizability | |
Only patients with an ECOG PS of 0 or 1 were eligible for the KEYNOTE-355 study. Should patients with an ECOG PS > 1 be eligible? | General practice is to allow up to ECOG PS 2. |
Should patients currently receiving chemotherapy for first-line treatment of mTNBC, but whose disease has not progressed, have pembrolizumab added provided all other criteria are met? (This question is in relation to any delays obtaining PD-L1 results or any other delay in accessing pembrolizumab, but where chemotherapy needs to be initiated before this information is available.) | A short and reasonable window of time (such as 6 weeks, to match a commonly used frequency of pembrolizumab) may be allowed to add pembrolizumab after initiation of first-line chemotherapy (i.e., chemotherapies as used in the KEYNOTE-355 trial in combination with pembrolizumab). |
Should patients who are currently receiving chemotherapy for mTNBC have pembrolizumab added to therapy (provided they have not previously been treated with immune checkpoint inhibitors), regardless of the line of therapy, provided they are PD-L1 CPS ≥ 10? | The clinical expert did not feel this was appropriate in the absence of evidence. |
Care provision issues | |
PD-L1 CPS testing for breast cancer needs to be operationalized and funded in some jurisdictions on or before pembrolizumab implementation. | For pERC consideration. |
System and economic issues | |
PAG is concerned about the overall budget impact of pembrolizumab given the volume of TNBC patients who may be eligible and the cost of pembrolizumab. Generic versions of all chemotherapy comparators, with the exception of nab-paclitaxel, are available. | For pERC consideration. |
CPS = combined positive score; ECOG PS = Eastern Cooperative Oncology Group Performance Status; ER = estrogen receptor; mTNBC = metastatic triple-negative breast cancer; PAG = Provincial Advisory Group; PD-L1 = programmed cell death 1 ligand 1; pERC = CADTH pan-Canadian Oncology Drug Review Expert Review Committee; PR = progesterone receptor; TNBC = triple-negative breast cancer.
Clinical Evidence
The clinical evidence included in the review of pembrolizumab (Keytruda) is presented in 2 sections. The first section, the systematic review, includes pivotal studies provided in the sponsor’s submission to CADTH and Health Canada, as well as those studies that were selected according to an a priori protocol. The second section includes a submitted ITC. No indirect evidence was identified in the literature that met the selection criteria specified for this CADTH review.
Systematic Review (Pivotal and Protocol-Selected Studies)
Objectives
To perform a systematic review of the beneficial and harmful effects of pembrolizumab (200 mg IV administered every 3 weeks or 400 mg every 6 weeks) for the treatment of adult patients with locally recurrent unresectable or mTNBC who have not received prior chemotherapy for metastatic disease and whose tumours express PD-L1 as determined by a validated test (CPS ≥ 10).
Methods
Studies selected for inclusion in the systematic review included pivotal studies provided in the sponsor’s submission to CADTH and Health Canada, as well as those meeting the selection criteria presented in Table 5. Outcomes included in the CADTH review protocol reflect outcomes considered to be important to patients, clinicians, and drug plans.
The literature search for clinical studies was performed by an information specialist using a peer-reviewed search strategy according to the PRESS Peer Review of Electronic Search Strategies checklist.23
Published literature was identified by searching the following bibliographic databases: MEDLINE All (1946–) via Ovid and Embase (1974–) via Ovid. All Ovid searches were run simultaneously as a multifile search. Duplicates were removed using Ovid deduplication for multifile searches, followed by manual deduplication in EndNote. The search strategy comprised both controlled vocabulary, such as the National Library of Medicine’s MeSH (Medical Patient Headings), and keywords. The main search concepts were Keytruda (pembrolizumab) and TNBC. Clinical trials registries searched included the US National Institutes of Health’s clinicaltrials.gov, WHO’s International Clinical Trials Registry Platform search portal, Health Canada’s Clinical Trials Database, and the European Union Clinical Trials Register.
Table 5: Inclusion Criteria for the Systematic Review
Criteria | Description |
|---|---|
Patient population | Adult patients with locally recurrent unresectable or mTNBC who have not received prior chemotherapy for metastatic disease and whose tumours express PD-L1 as determined by a validated test (CPS ≥ 10). Subgroups:
|
Intervention | Pembrolizumab (200 mg administered intravenously every 3 weeks or 400 mg administered intravenously every 6 weeks) in combination with chemotherapy |
Comparators | Single-drug chemotherapy:
|
Outcomes | Efficacy outcomes:
Harms outcomes:
|
Study design | Published and unpublished phase III and IV randomized controlled trials |
AE = adverse event; CPS = combined positive score; DOR = duration of response; ECOG PS = European Cooperative Oncology Group Performance Status; HRQoL = health-related quality of life; mTNBC = metastatic triple-negative breast cancer; ORR = overall response rate; OS = overall survival; PD-L1 = programmed cell death 1 ligand 1; PFS = progression-free survival; SAE = serious adverse event; TEAE = treatment-emergent adverse event; WDAE = withdrawal due to adverse event.
aThese outcomes were identified as being of particular importance to patients in the input received by CADTH from patient groups.
No filters were applied to limit the retrieval by study type. Retrieval was not limited by publication date or by language. Conference abstracts were excluded from the search results. Appendix 1 provides detailed search strategies.
The initial search was completed on June 27, 2022. Regular alerts updated the search until the meeting of the CADTH pan-Canadian Oncology Drug Review Expert Committee on November 9, 2022.
Grey literature (literature that is not commercially published) was identified by searching relevant websites from the Grey Matters: A Practical Tool For Searching Health-Related Grey Literature checklist.24 Included in this search were the websites of regulatory agencies (FDA and European Medicines Agency). Google was used to search for additional internet-based materials. Appendix 1 provides more information on the grey literature search strategy.
These searches were supplemented through contacts with appropriate experts. In addition, the sponsor of the drug was contacted for information regarding unpublished studies.
Findings From the Literature
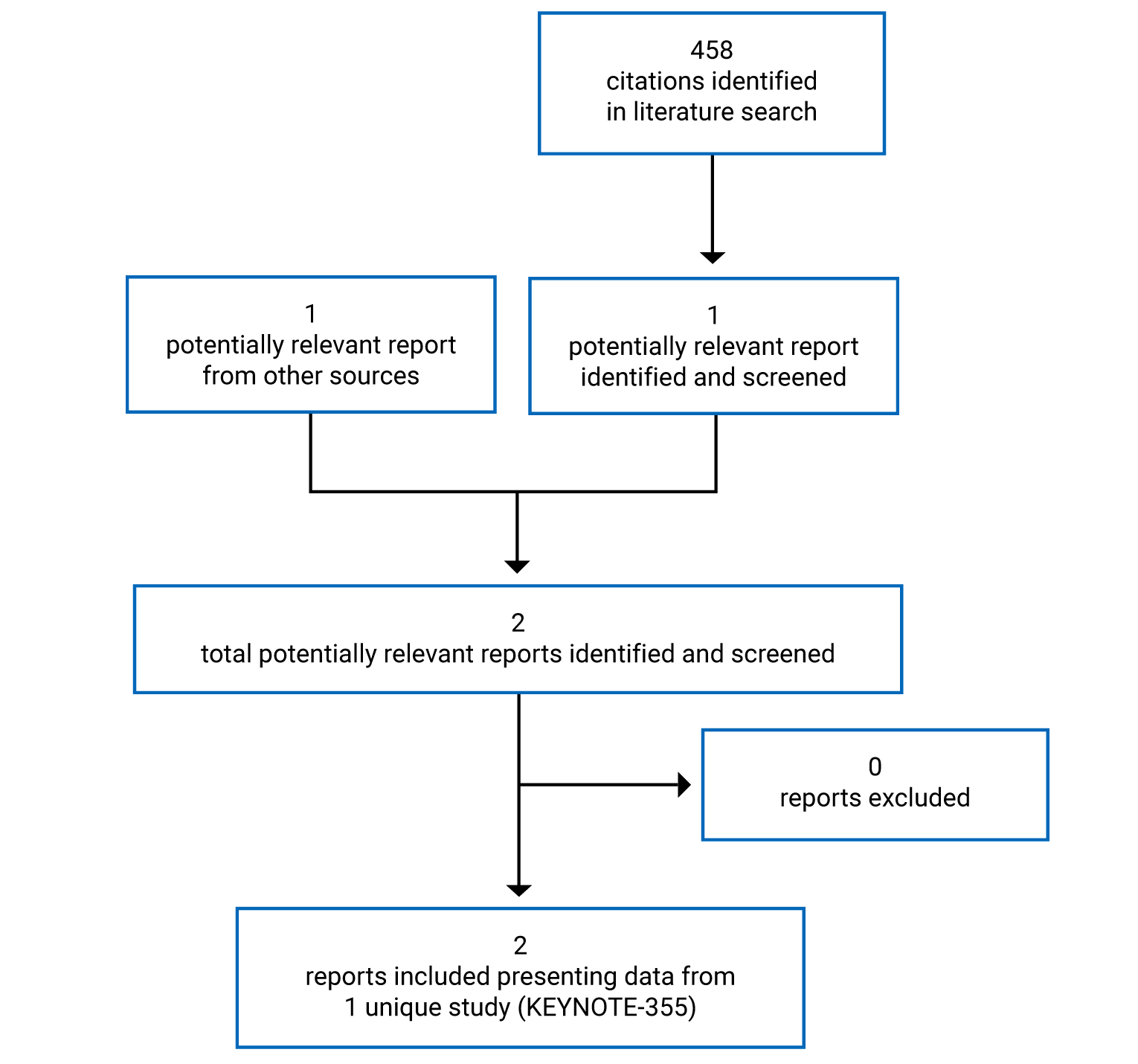
One report of a single study was identified from the literature for inclusion in the systematic review (Figure 1). The included study is summarized in Table 6.
Table 6: Details of Included Study
Detail | KEYNOTE-355 Trial |
|---|---|
Design and population | |
Study design | Multicentre, double-blind, parallel arm, randomized, phase III trial |
Locations | 251 centres in 29 countries: North America (5 sites in Canada; N = 34), South America, Europe, Asia, and Australia |
Study duration |
|
Enrolment dates |
|
Data cut-off date | Part 2 Interim analyses:
Final analysis: June 15, 2021; occurred after approximately 664 OS events among all patients and 240 OS events among patients with CPS ≥ 10 have been observed (final OS analysis) |
Randomized (N) |
|
Inclusion criteria |
|
Exclusion criteria |
|
Drugs | |
Intervention | Pembrolizumab (200 mg q.3.w) plus 1 of the following chemotherapies:
|
Comparator | Placebo (normal saline q.3.w.) plus chemotherapy (nab-paclitaxel, paclitaxel, or gemcitabine carboplatin):
|
Duration | |
Phase | |
Safety run-in | 21 to 28 days |
Intervention (part 2) | Every 3 weeks for up to 35 administrations (e.g., 105 weeks) |
Safety (part 1) | Pembrolizumab plus chemotherapy every 3 weeks |
Outcomes | |
Primary end points |
|
Secondary and exploratory end points | Secondary end points
Exploratory end points
|
Notes | |
Publicationsa | Cortes et al. (2021) |
AE = adverse event; ASCO = American Society of Clinical Oncology; AUC = area under the curve; CAP = College of American Pathologists; CHF = congestive heart failure; CIV = central imaging vendor; CNS = central nervous system; CPS = combined positive score; DCR = disease control rate; DOR = duration of response; ECOG = Eastern Cooperative Oncology Group Performance Status; EORTC QLQ-BR23 = European Organisation for Research and Treatment of Cancer Quality of Life Questionnaire – Breast Module 23; EORTC QLQ-C30 = European Organisation for Research and Treatment of Cancer Quality of Life Questionnaire Core 30; HRQoL = health-related quality of life; IA1 = first interim analysis; IA2 = second interim analysis; ORR = objective response rate; OS = overall survival; PD-1 = programmed cell death 1 protein; PD-L1 = programmed cell death 1 ligand 1; PFS = progression-free survival; q.3.w. = every 3 weeks; RECIST 1.1 = Response Evaluation Criteria in Solid Tumours Version 1.1; TNBC = triple-negative breast cancer.
Note: Data cut-off: June 15, 2021.
Source: Clinical Study Report15 and sponsor’s general submission materials.26
Description of Study
The KEYNOTE-355 trial is an ongoing, phase III, randomized, multicentre, double-blind, 2-part, placebo-controlled trial. The primary objective of the trial is to evaluate the efficacy and safety of pembrolizumab plus chemotherapy versus placebo plus chemotherapy for patients with locally recurrent inoperable or metastatic TNBC not been previously treated with chemotherapy for metastatic disease. The study was conducted in 2 parts (Figure 2). Part 1 was the safety run-in (N = 30) and part 2 was the efficacy evaluation (N = 847). For the purpose of this CADTH review, only part 2 was evaluated. The 2 coprimary efficacy outcomes of OS and PFS were assessed in all patients, and patients with PD-L1–positive tumours. Secondary outcomes included ORR, DOR, disease control rate, and HRQoL and were assessed in all patients and patients with PD-L1–positive tumours. The study was considered to have met its primary end point if the combination of pembrolizumab and chemotherapy was superior to placebo and chemotherapy in either PFS or OS in either all patients or in patients with PD-L1–positive tumours (CPS ≥ 1 or CPS ≥ 10) at either an interim analysis or the final analysis (OS only). In total, 75.1% and 38.1% had a tumour tissue PD-L1 expression score of CPS of 1 or higher and a CPS of 10 or higher, respectively. Given that the indication for the sponsor-submitted reimbursement request is for patients with a PD-L1 expression (CPS) of 10 or higher, this review focuses on patients with a PD-L1 CPS of 10 or higher and all patients. Efficacy results for patients with a PD-L1 CPS of 1 or higher can be found in Appendix 2. In total, 1,372 patients had been screened, of whom 847 were randomized via an interactive voice recognition system in the ITT population in a 2:1 ratio between the pembrolizumab plus chemotherapy and the placebo plus chemotherapy groups. In total, 566 patients were randomized to receive pembrolizumab plus chemotherapy and 281 to receive placebo plus chemotherapy. Randomization was stratified based on 3 factors:
type of chemotherapy on study (paclitaxel or nab-paclitaxel or gemcitabine and carboplatin)
PD-L1 expression at baseline (CPS ≥ 1 or < 1)
prior treatment with the same class of chemotherapy in the neoadjuvant or adjuvant setting (yes or no).
Patients already in the screening phase may have been enrolled even after the maximum sample size had been reached. A total of 843 patients received at least 1 dose of the study intervention and were included in the population of all patients as treated (APaT) (562 in the pembrolizumab plus chemotherapy group and 281 in the placebo plus chemotherapy group).
The KEYNOTE-355 trial was initiated in August 2016 and has 251 participating centres across 29 countries in North America (5 sites in Canada), South America, Europe, Asia, and Australia. Both patients and investigators were blinded to study treatments administered during the trial. All patients enrolled were female. Majority of patients were younger than 65 years of age, white, postmenopausal, and had an ECOG PS of 0.
Populations
Inclusion and Exclusion Criteria
Eligible patients included those at least 18 years of age with locally recurrent inoperable TNBC not previously treated with chemotherapy and that could not be treated with curative intent, or mTNBC not previously treated with chemotherapy. Patients were to have completed treatment for stage I to III breast cancer, if indicated, with at least 6 months between the completion of treatment with curative intent and first documented local or distant disease recurrence. Patients who received taxane, gemcitabine, or platinum drugs in the (neo)adjuvant setting could have been treated with the same class of chemotherapy and could participate if at least 12 months had elapsed between the completion of treatment with curative intent and first documented local or distant disease recurrence. Patients were required to have centrally confirmed TNBC as defined by American Society of Clinical Oncology or College of American Pathologists guidelines, measurable disease according to RECIST 1.1 by local radiology review, an ECOG PS of 0 or 1, and a predicted life expectancy of 12 weeks or longer from randomization. Patients were enrolled regardless of PD-L1 biomarker status but were required to provide a tumour tissue sample for central biomarker analysis.
Figure 2: KEYNOTE-355 Study Design
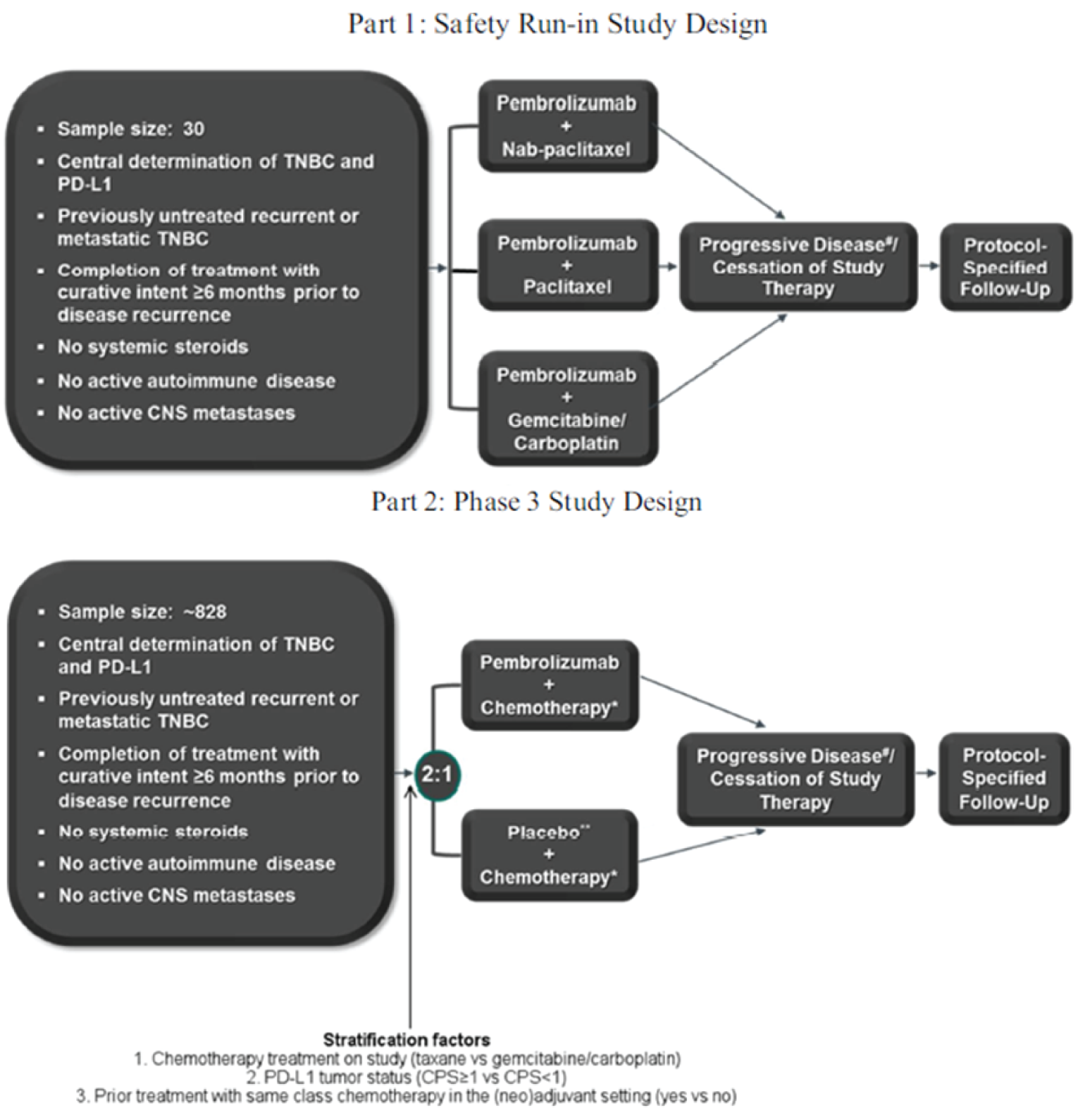
CNS = central nervous system; CPS = combined positive score; PD-L1 = programmed cell death 1 ligand 1; TNBC = triple-negative breast cancer.
Notes: Treatment was to continue until confirmation of progressive disease or death. Patients from part 1 (safety run-in) were not included in part 2 (efficacy evaluation). Data cut-off date: June 15, 2021.
Baseline Characteristics
All patients were female and most were younger than 65 years of age; white, non-Hispanic or non-Latino; postmenopausal; and had an ECOG PS of 0. Most patients entered the study with mTNBC (recurrent [66.9%] or de novo [29.8%] metastatic disease). More patients in the pembrolizumab group (21%) versus the placebo plus chemotherapy group (16.5%) had a disease-free interval of less than 12 months. Most patients (78.3%) who received prior neoadjuvant and/or adjuvant treatment were not treated with the same class of chemotherapy in the study. Most patients (75.1%) had a tumour-tissue PD-L1 CPS of 1 or higher, and 38.1% of patients had a tumour-tissue PD-L1 CPS of 10 or higher. In the ITT population for patients with a PD-L1 CPS of 10 or higher, demographics and other baseline characteristics data were generally well balanced between the 2 intervention groups and consistent with those of the APaT population. A majority of patients (approximately 54%) received gemcitabine and carboplatin as their chemotherapy in addition to pembrolizumab and placebo. A summary of baseline and demographic characteristics of patients enrolled in the KEYNOTE-355 study at final analysis is presented in Table 7.
Table 7: Summary of Baseline Characteristics at Final Analysis — ITT Population
Characteristic | Patients with CPS ≥ 10 | All patients | ||
|---|---|---|---|---|
Pembrolizumab plus chemotherapy N = 220 | Placebo plus chemotherapy N = 103 | Pembrolizumab plus chemotherapy N = 566 | Placebo plus chemotherapy N = 281 | |
Gender, n (%) | ||||
Female | 220 (100.0) | 103 (100.0) | 566 | 281 |
Age (years), n (%) | ||||
< 65 | 178 (80.9) | 79 (76.7) | 443 (78.3) | 224 (79.7) |
≥ 65 | 42 (19.1) | 24 (23.3) | 123 (21.7) | 57 (20.3) |
Median | 52.0 | 55.0 | 53.0 | 53.0 |
Range | 25 to 83 | 22 to 77 | 25 to 85 | 22 to 77 |
Race, n (%) | ||||
American Indian or Alaska Native [wording from original source] | 2 (0.9) | 0 | 11 (1.9) | 1 (0.4) |
Asian | 44 (20.0) | 20 (19.4) | 123 (21.7) | 52 (18.5) |
Black or African American | 9 (4.1) | 6 (5.8) | 20 (3.5) | 17 (6.0) |
Multiple | 6 (2.7) | 3 (2.9) | 11 (1.9) | 8 (2.8) |
White | 153 (69.5) | 70 (68.0) | 384 (67.8) | 195 (69.4) |
Missing | 6 (2.7) | 4 (3.9) | 17 (3.0) | 8 (2.8) |
Ethnicity, n (%) | ||||
Hispanic or Latino | 37 (16.8) | 21 (20.4) | 116 (20.5) | 48 (17.1) |
Not Hispanic or Latino | 174 (79.1) | 76 (73.8) | 423 (74.7) | 218 (77.6) |
Not reported | 6 (2.7) | 4 (3.9) | 17 (3.0) | 10 (3.6) |
Unknown | 2 (0.9) | 2 (1.9) | 9 (1.6) | 5 (1.8) |
Missing | 1 (0.5) | 0 | 1 (0.2) | 0 |
Geographic region, n (%) | ||||
Asia | 38 (17.3) | 18 (17.5) | 113 (20.0) | 47 (16.7) |
Europe | 108 (49.1) | 52 (50.5) | 263 (46.5) | 144 (51.2) |
Australia | 5 (2.3) | 2 (1.9) | 13 (2.3) | 8 (2.8) |
North America | 33 (15.0) | 12 (11.7) | 68 (12.0) | 40 (14.2) |
Rest of the world | 36 (16.4) | 19 (18.4) | 109 (19.3) | 42 (14.9) |
Chemotherapy on study (IVRS), n (%) | ||||
Nab-paclitaxel | 63 (28.6) | 36 (35.0) | 173 (30.6) | 95 (33.8) |
Paclitaxel | 33 (15.0) | 11 (10.7) | 82 (14.5) | 32 (11.4) |
Gemcitabine and carboplatin | 124 (56.4) | 56 (54.4) | 311 (54.9) | 154 (54.8) |
PD-L1 status (CPS cut-off of 10) | ||||
PD-L1 CPS ≥ 10 | 220 (100) | 103 (100) | 220 (38.9) | 103 (36.7) |
PD-L1 CPS < 10 | NA | NA | 346 (61.1) | 178 (63.3) |
PD-L1 status (CPS cut-off of 1) | ||||
PD-L1 CPS ≥ 1 | NA | NA | 425 (75.1) | 211 (75.1) |
PD-L1 CPS < 1 | NA | NA | 141 (24.9) | 70 (24.9) |
Prior treatment with same class of chemotherapy in the neoadjuvant or adjuvant setting (IVRS) | ||||
Yes | 46 (20.9) | 19 (18.4) | 124 (21.9) | 62 (22.1) |
No | 174 (79.1) | 84 (81.6) | 442 (78.1) | 219 (77.9) |
Prior treatment with same class of chemotherapy in the neoadjuvant or adjuvant setting (actual) | ||||
Yes | 44 (20.0) | 17 (16.5) | 124 (21.9) | 56 (19.9) |
No | 175 (79.5) | 86 (83.5) | 438 (77.4) | 225 (80.1) |
Missing | 1 (0.5) | 0 | 4 (0.7) | 0 |
Disease status | ||||
Metastatic, de novo | 69 (31.4) | 35 (34.0) | 168 (29.7) | 84 (29.9) |
Metastatic, recurrence | 143 (65.0) | 62 (60.2) | 382 (67.5) | 185 (65.8) |
Locally recurrent inoperable | 7 (3.2) | 6 (5.8) | 13 (2.3) | 12 (4.3) |
Missing | 1 (0.5) | 0 | 3 (0.5) | 0 |
ECOG PS | ||||
0 | 134 (60.9) | 62 (60.2) | 332 (58.7) | 173 (61.6) |
1 | 86 (39.1) | 41 (39.8) | 232 (41.0) | 108 (38.4) |
2 | 0 | 0 | 1 (0.2) | 0 |
Missing | 0 | 0 | 1 (0.2) | 0 |
HER2 status | ||||
0 to 1+ by IHC | 153(69.5) | 80 (77.7) | 414 (73.1) | 214 (76.2) |
2+ by IHC | 67 (30.5) | 23 (22.3) | 152 (26.9) | 76 (23.8) |
History of brain metastasis | ||||
Yes | 5 (2.3) | 6 (5.8) | 19 (3.4) | 9 (3.2) |
No | 215 (97.7) | 97 (94.2) | 546 (96.5) | 272 (96.8) |
Missing | 0 | 0 | 1 (0.2) | 0 |
Menopausal status | ||||
Premenopausal | 74(33.6) | 34 (33.0) | 178 (31.4) | 92 (32.7) |
Postmenopausal | 146 (66.4) | 69 (67.0) | 387 (68.4) | 189 (67.3) |
Missing | 0 | 0 | 1 (0.2) | 0 |
Disease-free interval | ||||
De novo metastasis | 69 (31.4) | 35 (34.0) | 168 (29.7) | 84 (29.9) |
< 12 months | 48 (21.8) | 17 (16.5) | 125 (22.1) | 54 (17.8) |
≥ 12 months | 102 (46.4) | 51 (49.5) | 270 (47.7) | 147 (52.3) |
Unknown | 1 (0.5) | 0 (0.0) | 3(0.5) | 0 |
Sum of target lesion size at baseline (central) (mm) | ||||
Patients with data | 200 | 99 | 525 | 255 |
Median | 56.0 | 59.0 | 55.0 | 54.0 |
Range | 11.0 to 290.0 | 15.0 to 271.0 | 11.0 to 368.0 | 11.0 to 289.0 |
Sum of target lesion size at baseline (investigator) (mm) | ||||
Patients with data | 217 | 103 | 561 | 281 |
Median | 60.0 | 66.0 | 61.0 | 56.0 |
Range | 10.0 to 352.0 | 10.0 to 237.1 | 10.0 to 406.8 | 10.0 to 410.0 |
Metastatic organ sites, n (%) | ||||
0 | 7 (3.2) | 6 (5.8) | 13 (2.3) | 12 (4.3) |
1 | 39 (17.7) | 21 (20.4) | 107 (18.9) | 59 (21.0) |
2 | 76 (34.5) | 35 (34.0) | 193 (34.1) | 95 (33.8) |
≥ 3 | 97 (44.1) | 41 (39.8) | 250 (44.2) | 115 (40.9) |
Missing | 1 (0.5) | 0 | 3 (0.5) | 0 |
Metastatic organ sites, n (%) | ||||
Patients with metastatic disease | 212 | 97 | 550 | 269 |
Bone | 53 (24.1) | 22 (21.4) | 170 (30.0) | 85 (30.2) |
Brain | 5 (2.3) | 6 (5.8) | 18 (3.2) | 9 (3.2) |
Breast | 17 (7.7) | 7 (6.8) | 35 (6.2) | 18 (6.4) |
Chest wall | 56 (25.5) | 15 (14.6) | 132 (23.3) | 45 (16.0) |
Liver | 62 (28.2) | 32 (31.1) | 171 (30.2) | 78 (27.8) |
Lung | 120 (54.5) | 55 (53.4) | 325 (57.4) | 162 (57.7) |
Lymph nodes | 169 (76.8) | 79 (76.7) | 417 (73.7) | 206 (73.3) |
Other metastasis | 46 (20.9) | 17 (16.5) | 110 (19.4) | 51 (18.1) |
Visceral disease, n (%) | ||||
Nonvisceral Only | 13 (5.9) | 9 (8.7) | 31 (5.5) | 23 (8.2) |
With brain metastasis | 0 | 0 | 0 | 0 |
Without brain metastasis | 13 (5.9) | 9 (8.7) | 31 (5.5) | 23 (8.2) |
Any visceral | 206 (93.6) | 94 (91.3) | 532 (94.0) | 258 (91.8) |
With brain metastasis | 5 (2.3) | 6 (5.8) | 18 (3.2) | 9 (3.2) |
Without brain metastasis | 201 (91.4) | 88 (85.4) | 514 (90.8) | 249 (88.6) |
Missing | 1 (0.5) | 0 | 3 (0.5) | 0 |
Prior neoadjuvant or adjuvant chemotherapy, n (%) | ||||
Yes | 131 (59.5) | 62 (60.2) | 357 (63.1) | 181 (64.4) |
Taxanes | 107 (48.6) | 50 (48.5) | 290 (51.2) | 156 (55.5) |
Platinum | 13 (5.9) | 6 (5.8) | 41 (7.2) | 24 (8.5) |
Anthracyclines | 115 (52.3) | 50 (48.5) | 318 (56.2) | 155 (55.2) |
Other | 118 (53.6) | 55 (53.4) | 329 (58.1) | 169 (60.1) |
No | 89 (40.5) | 41 (39.8) | 209 (36.9) | 100 (35.6) |
CPS = combined positive score; ECOG PS = Eastern Cooperative Oncology Group Performance Status; ITT = intention-to-treat; IVRS = interactive voice recognition system; PD-L1 = programmed cell death 1 ligand 1.
Notes: Breast, chest wall, and lymph node also include locally recurrent lesions. Data cut-off: June 15, 2021.
Source: Clinical Study Report.15
Interventions
Patients were randomized in a 2:1 ratio to the 2 study arms:
pembrolizumab (200 mg) every 3 weeks plus 1 of the following chemotherapies:
nab-paclitaxel (100 mg/m2 on days 1 and 8, and 15 every 28 days)
paclitaxel (90 mg/m2 on days 1 and 8, and 15 every 28 days)
gemcitabine and carboplatin (gemcitabine 1,000 mg/m2 with carboplatin at the area under the curve 2 on days 1 and 8 every 21 days)
placebo (normal saline) every 3 weeks plus 1 of the following chemotherapies as described in group 1 (e.g., nab-paclitaxel, paclitaxel, or gemcitabine and carboplatin), using the same dosing and schedule.
The chemotherapy for which each patient was eligible was determined by the previous chemotherapy use and the time elapsed since that use, as described in the inclusion criteria. If chemotherapy options included more than 1 regimen, the choice of study chemotherapy was at the physician’s discretion.
Treatment Administration
Chemotherapies were administered by an unblinded pharmacist, but patients, investigators, other study site staff, and the sponsor were blinded to the administration of pembrolizumab or placebo.
Pembrolizumab was administered at a 200 mg fixed dose via IV every 3 weeks until confirmed disease progression or cessation of study treatment. Patients were followed closely for unacceptable toxicities for 21 days in patients receiving gemcitabine and carboplatin chemotherapy or 28 days in patients receiving either taxane chemotherapy (i.e., paclitaxel or nab-paclitaxel) after the first administrations. According to the protocol of the KEYNOTE-355 trial, patients had to discontinue from pembrolizumab or placebo once they completed 35 administrations of pembrolizumab or placebo. However, patients were allowed to continue chemotherapy treatment at the investigator’s discretion.
Dose Modification and Interruptions
Dose reductions were not permitted for pembrolizumab. Dose modifications were conducted in a stepwise pattern and were based on maximum toxicity experienced during the previous treatment. Toxicity (except for alopecia) needed to resolve to no worse than grade 1 or baseline before resuming treatment with the same drug(s). A maximum of 2 dose modifications per chemotherapy (if applicable) for toxicities throughout the course of the study was permitted. Dose-modification strategies for other chemotherapy drugs were allowed in the study protocol. Local guidelines and practices were recommended if dosing was different from the sponsor’s recommendations. Dose reductions were not permitted for pembrolizumab.
In the event of drug-related toxicity, including severe or life-threatening AEs, pembrolizumab was withheld. Dosing interruptions were permitted in the case of medical or surgical events or logistical reasons not related to study therapy (e.g., elective surgery, unrelated medical events, patient vacation, and/or holidays). Chemotherapy administration was allowed to be interrupted due to AEs for a maximum of 4 weeks; pembrolizumab was allowed to be interrupted due to AEs for a maximum of 12 weeks. Patients were to resume study therapy within 3 weeks of the scheduled interruption, unless otherwise discussed with the sponsor.
Treatment Discontinuation Criteria
Patients were allowed to discontinue 1 or more components of the study treatment at the discretion of the investigator in case of undesirable effects. Study treatment was continued if 1 of the following occurred: central imaging vendor (CIV)-verified progressive disease as defined by RECIST 1.1, unacceptable toxicity, intercurrent illness that necessitated discontinuation of study treatment, investigator’s decision to withdraw the patient, pregnancy, patient noncompliance with study treatment or procedure requirements, withdrawal of consent to treatment, death, the end of the study, or other administrative reasons requiring cessation of treatment.
Concomitant Medications
In the trial, all treatments that the investigator considered necessary for a patient’s welfare may be administered at the discretion of the investigator in keeping with the community standards of medical care. All concomitant medications received within 30 days before randomization while on study treatment, and up to 30 days after the last dose of study treatment, were recorded. Rescue medications included the use of oral or IV treatment with corticosteroids, as well as additional anti-inflammatory drugs, if symptoms did not improve with administration of corticosteroids.
Patients were prohibited from receiving the following therapies during the screening, treatment, and re-treatment phase of this study:
antineoplastic systemic chemotherapy or biological therapy
immunotherapy not specified in this protocol
chemotherapy not specified in this protocol
investigational drugs other than pembrolizumab
radiation therapy within 2 weeks before randomization; however, radiation therapy for a symptomatic solitary lesion or the brain may be allowed after consultation with sponsor (except during screening).
herbal supplements
live vaccines within 30 days before randomization and while participating in the study; examples of live vaccines include, but are not limited to: measles, mumps, rubella, varicella, herpes zoster, yellow fever, rabies, Bacillus Calmette–Guérin, and typhoid (oral) vaccines; seasonal influenza vaccines for injection are generally killed virus vaccines and are allowed; however, intranasal influenza vaccines (e.g., Flu-Mist) are live attenuated vaccines, and are not allowed
glucocorticoids for any purpose other than the following:
to modulate symptoms from an AE of suspected immunologic etiology
inhaled steroids for management of asthma
physiologic doses of prednisone 10 mg (or equivalent) per day
use of prophylactic corticosteroids to avoid allergic reactions (e.g., to paclitaxel and/or IV contrast dye) is permitted.
any medication prohibited in combination with chemotherapy as described in the respective product labels for nab-paclitaxel, paclitaxel, gemcitabine, and carboplatin.
Outcomes
A list of efficacy end points identified in the CADTH review protocol that were assessed in the clinical trials included in this review is provided in Table 8 and summarized in the following section. A detailed discussion and critical appraisal of the outcome measures is provided in Appendix 3.
Table 8: Summary of Outcomes of Interest Identified in the CADTH Review Protocol
Outcome measure | KEYNOTE-355 trial end point | Included in hierarchical multiple-testing procedure |
|---|---|---|
Overall survival | Primary | Yes |
Health-related quality of life
| Secondary and exploratory (EQ VAS) | No |
Progression-free survival | Primary | Yes |
Objective response rate | Secondary | Yes |
Duration of response | Secondary | No |
Safety | Safety (e.g., AEs, SAEs, WDAE, notable harms) | No |
AE = adverse event; EORTC QLQ-BR23 = European Organisation for Research and Treatment of Cancer Quality of Life Questionnaire – Breast Model 23; EORTC QLQ-C30 = European Organisation for Research and Treatment of Cancer Quality of Life Questionnaire Core 30; EQ VAS = EQ visual analogue scale; SAE = serious adverse event.
Source: Clinical Study Report.15
Primary Outcomes
Overall Survival
Overall survival was a coprimary outcome of the KEYNOTE-355 trial. OS was defined as the time from randomization to death due to any cause. Patients without documented death at the time of the analysis were censored at the date of the last follow-up.
Health-Related Quality of Life
HRQoL measures were a secondary outcome of the KEYNOTE-355 trial. HRQoL measures were assessed using the EORTC QLQ-C30, EORTC QLQ-BR23, and EQ-5D questionnaires. A detailed discussion and critical appraisal of the EORTC QLQ-C30 and EORTC QLQ-BR23 is available in Appendix 3; the EQ VAS is a commonly used and validated measure in oncology trials. The primary patient-reported outcome analysis time point is defined as the latest time point at which the completion and compliance rates are still high enough based on blinded data review (approximately 60% completion and 80% compliance rates). The resulting time frame was 15 weeks in this case; the minimum completion and compliance rates were required to minimize the impact of missing data assumptions on patient-reported outcome analysis outcomes. The key patient-reported outcome end point was the mean score changes from baseline to the primary analysis time point in EORTC QLQ-C30 global health status and QoL score.
Supportive patient-reported outcome end points included the following: the mean score changes from baseline to the primary analysis time point in EQ VAS as measured by the EQ-5D questionnaire; the mean score changes from baseline to the primary analysis time point for the QLQ-C30 physical and emotional functioning scales; time to deterioration defined as the time from start of treatment to first onset of 10 points or more worsening from baseline the EORTC QLQ-C30 global health status and QoL score and physical and emotional functioning scales; the mean score changes from baseline to the primary analysis time point for other items or scales of the EORTC QLQ-C30 and EORTC QLQ-BR23 as appropriate.
The patient-reported outcomes were assessed every 3 weeks (e.g., every cycle of treatment). After the third cycle and until the end of year 1, patient-reported outcomes were collected every third cycle (every 9 weeks) until progressive disease, while the patient was receiving study treatment. During year 2, they will occur every fourth cycle (every 12 weeks) until progressive disease, while the patient is receiving study treatment. For the analysis, patient-reported outcomes assessed at visits of “end of treatment” and “safety follow-up” will be mapped into different time points according to the actual visit time. If there are multiple patient-reported outcome collections within the time window of a specific visit, the collection closest to the target day will be used in the analysis.
The EORTC QLQ-C30 is a multidimensional, cancer-specific, self-administered measure of HRQoL. The EORTC QLQ-C30 is composed of both multi-item scales and single-item measures. These include 5 functional scales (physical, role, cognitive, emotional, and social), 3 symptom scales (fatigue, pain, and nausea and vomiting), a global health status or QoL scale, and 6 single items assessing additional symptoms commonly reported by cancer patients (dyspnea, loss of appetite, insomnia, constipation and diarrhea) as well as perceived financial impact of the disease.28 The EORTC QLQ-C30 uses a 1-week recall period to assess functional status and symptoms. All scales and single-item measures are scored from 0 to 100. Scale sum scores are transformed such that a high score on the functional scales represents a high or healthy level of functioning, a high score on the symptom scales represents a high level of symptomatology and a high score on the global health status or QoL scale represents a high HRQoL.29
The EORTC QLQ-BR23 includes an additional 23 items that are specific to breast cancer, with 5 multi-item scales assessing systemic therapy side effects, group symptoms, breast symptoms, body image, and sexual functioning, as well as single items assessing sexual enjoyment, hair loss, and future perspective.30 All scales range in score from 0 to 100, and higher scores represent higher responses. A high score for functioning represents high functioning while a high symptom score represents a high symptom burden. The EORTC QLQ-BR23 is not a freestanding instrument as it does not measure a multidimensional construct of body image; instead, it is administered in conjunction with the EORTC QLQ-C30.30
The 5-Level EQ-5D questionnaire consists of 2 separate elements: the utility score (or descriptive system) that captures health states across 5 dimensions: mobility; self-care; usual activities, pain and/or discomfort; and anxiety and/or depression. Each unique health state is defined by combining response levels from each of the 5 dimensions. The second component, a vertical visual analogue scale, records the respondent’s self-rated health on a scale ranging from 0 to 100, for which the end points are “best imaginable health state” (100) and “worst imaginable health state” (0).26
Progression-Free Survival
PFS was a coprimary outcome of the KEYNOTE-355 trial. PFS was defined as the time from randomization to the first documented disease progression as defined by RECIST 1.1 based on assessments by a CIV or death due to any cause, whichever occurs first. Table 9 provides PFS censoring rules.
Patients were evaluated with radiographic imaging at baseline, after randomization at weeks 8, 16, and 24, then every 9 weeks for the remainder of year 1, and every 12 weeks thereafter to assess response to treatment.
Table 9: Censoring Rules for the Primary and Sensitivity Analyses of PFS
Situation | Primary analysis | Sensitivity analysis 1 | Sensitivity analysis 2 |
|---|---|---|---|
No PD and no death; and new anticancer treatment is not initiated | Censored at last disease assessment | Censored at last disease assessment | Progressed at treatment discontinuation due to reasons other than complete response; otherwise censored at last disease assessment if still on study treatment or completed study treatment |
No PD and no death; new anticancer treatment is initiated | Censored at last disease assessment before new anticancer treatment | Censored at last disease assessment | Progressed at date of new anticancer treatment |
PD or death documented after ≤ 1 missed disease assessment, and before new anticancer therapy, if any | Progressed at date of documented PD or death | Progressed at date of documented PD or death | Progressed at date of documented PD or death |
PD or death documented immediately after ≥ 2 consecutive missed disease assessments or after new anticancer therapy, if any | Censored at last disease assessment before the earlier date of ≥ 2 consecutive missed disease assessment and new anticancer therapy, if any | Progressed at date of documented PD or death | Progressed at date of documented PD or death |
PD = progressive disease; PFS = progression-free survival.
Source: Clinical Study Report.15
Objective Response Rate
The ORR was a secondary outcome of the KEYNOTE-355 trial. The ORR was defined as the proportion of the patients in the analysis population with a complete or partial response. Responses are based on assessments by a CIV as defined by RECIST 1.1.
Duration of Response
The DOR was a secondary outcome of the KEYNOTE-355 trial. For patients who demonstrate a complete or partial response, DOR was defined as the time from first documented evidence of a complete or partial response until disease progression or death due to any cause, whichever occurs first, based on CIV assessments according to RECIST 1.1. Table 10 provides DOR censoring rules.
Sensitivity analyses were performed for DOR based on site investigator or local radiology review.
Table 10: Censoring Rules for the Analysis of Duration of Response
Situation | Date of progression or censoring | Outcome |
|---|---|---|
No PD nor death, no new anticancer therapy initiated | Last adequate disease assessment | Censor (nonevent) |
No PD nor death, new anticancer therapy initiated | Last adequate disease assessment before new anticancer therapy initiated | Censor (nonevent) |
Death or PD immediately after ≥ 2 consecutive missed disease assessments or after new anticancer therapy, if any | Earlier date of last adequate disease assessment before ≥ 2 missed adequate disease assessments and new anticancer therapy, if any | Censor (nonevent) |
Death or PD after ≤ 1 missed disease assessments and before new anticancer therapy, if any | PD or death | End of response (event) |
PD = progressive disease.
Note: A missed disease assessment includes any assessment that is not obtained or is considered inadequate for evaluation of response.
Source: Clinical Study Report.15
Harms Outcomes
Safety parameters such as incidence of AEs, SAEs including fatal SAEs, immune-related AEs, laboratory abnormalities, rates of dose interruption and discontinuation due to AEs, and events of clinical interest were monitored throughout the trial.
Schedule of Events
The end-of-treatment visit occurred at the time all study treatments are discontinued for any reason. The safety follow-up visit occurred 30 days after the last dose of all study treatments or before the initiation of a new anticancer treatment, whichever came first. Patients who are eligible for re-treatment with pembrolizumab may have up to 2 safety follow-up visits: 1 after the treatment period and 1 after the second course phase. Patients who discontinued all study treatments for a reason other than disease progression were moved into the disease status follow-up phase and were assessed according to the already-followed tumour-imaging schedule.
Statistical Analysis
Sample Size and Power Calculation
A total sample size of approximately 828 patients was initially planned for the study. It was expected that approximately 664 OS events among all patients and approximately 240 OS events among patients with a CPS of 10 or higher would be observed at the final analysis.
PFS in all patients: At IA2, the trial had approximately 89% power at a 1-sided 0.111% alpha level if the true HR is 0.70. At IA2, with approximately 634 events, the HR at boundary for success was approximately 0.77. At IA2, PFS in all patients could only be tested if both hypotheses of PFS in patients with a CPS of 10 or higher and PFS in patients with a CPS of 1 or higher were supported.
PFS in patients with a CPS of 10 or higher: at IA2 the trial had approximately 86% power at a 1-sided 0.411% alpha level if the true HR was 0.60. At IA2, with approximately 235 events, the HR at boundary for success was approximately 0.69 (approximately 2.4 months improvement over control median PFS of 5.5 months).
OS in all patients: the trial had approximately 60% power at a 1-sided 0.75% alpha level, if the true HR was 0.80. With approximately 664 events, the HR at boundary for success at final analysis was approximately 0.81 (approximately 4.0 months improvement over control median OS of 17.5 months). After IA1, OS in all patients could be tested if the hypothesis of OS in patients with a CPS of 1 or higher was supported.
OS in patients with a CPS of 10 or higher: the trial had approximately 79% power at a 1-sided 1.011% alpha level if the true HR was 0.65. With approximately 240 events, the HR at boundary for success at final analysis was approximately 0.72 (approximately 6.8 months improvement over control median OS of 17.5 months).
Primary Outcome Analyses
Overall Survival
The nonparametric Kaplan-Meier method was used to estimate the survival curves. The treatment difference in survival was assessed by the stratified log-rank test. A stratified Cox proportional hazards model with the Efron method of tie handling was used to assess the magnitude of the treatment difference (i.e., the HR). The HR and its 95% CI from the stratified Cox model with a single treatment covariate was reported. The stratification factors used for randomization were applied, as stratification factors for analysis, to both the stratified log-rank test and the stratified Cox model. Patients in the placebo plus chemotherapy group were expected to discontinue treatment earlier than would patients in the pembrolizumab plus chemotherapy group and were not allowed to cross over to the pembrolizumab plus chemotherapy group; however, they were allowed to be treated with another anti–PD-1 drug following the verification of progressive disease by blinded CIV. Exploratory analyses (adjustments) were performed to determine the impact on patients in the placebo group who were treated with an anti–PD-1 drug following progressive disease. Sensitivity analyses for OS were conducted to check the robustness of the data using the ITT principle. Table 12 provides an overview of the statistical analyses of efficacy end points.
Progression-Free Survival
The nonparametric Kaplan-Meier method was used to estimate the PFS curve in each treatment group. The treatment difference in PFS will be assessed by the stratified log-rank test. A stratified Cox proportional hazard model with the Efron method of tie handling will be used to assess the magnitude of the treatment difference (i.e., HR) between the treatment arms. The HR and its 95% CI, from the stratified Cox model with the Efron method of tie handling and with a single treatment covariate will be reported. The stratification factors used for randomization were applied, as stratification factors used for analysis, to both the stratified log-rank test and the stratified Cox model.
For patients who have progressive disease, the true date of disease progression will be approximated by the date of the first assessment at which progressive disease is objectively documented based on RECIST 1.1 as assessed by a CIV. Death is always considered a confirmed progressive-disease event. Patients who do not experience a PFS event will be censored at the last disease assessment.
In addition, 1 primary and 2 sensitivity analyses with a different set of censoring rules will be performed to assess the robustness of the PFS results. The first sensitivity analysis followed the ITT principle, whereby progressive diseases and/or deaths were counted as events regardless of missed study visits or initiation of new anticancer therapy. The second sensitivity analysis considered initiation of new anticancer treatment or discontinuation of treatment due to reasons other than complete response to be a progressive-disease event for patients without documented progressive disease or death. The censoring rules for primary and sensitivity analyses are summarized in Table 9. If a patient meets multiple criteria for censoring, the censoring criterion that occurs earliest was applied.
Multiplicity Testing
The multiplicity strategy was applied to the 6 primary hypotheses and the 2 secondary hypotheses of part 2: primary hypotheses of superiority of pembrolizumab plus chemotherapy compared to placebo plus chemotherapy in PFS and OS in all patients and in patients with PD-L1–positive tumours (for CPS ≥ 1 and CPS ≥ 10 separately), and secondary hypotheses of superiority of pembrolizumab plus chemotherapy compared to placebo plus chemotherapy in ORR in all patients and in patients with PD-L1–positive tumours (CPS ≥ 1).
The familywise type I error rate for this study was controlled at 2.5% (1-sided) across all 6 primary hypotheses on PFS and OS as well as 2 secondary hypotheses on ORR. A summary of the revised initial alpha allocation before any alpha reallocation is presented in Table 11. Based on emerging biomarker data external to this study, the initial alpha allocation among the 6 primary hypotheses and 2 secondary hypotheses was revised after IA1. The revision was based on emerging biomarker data external to the study (outlined in Amendment 5).
Table 11: Initial Alpha Allocation
Hypothesis | Initial alpha allocation |
|---|---|
1: PFS in all patients | 0.043% allocated at IA1 (already spent at IA1) 0% allocated at IA2 |
2: PFS in patients with CPS ≥ 1 | 0.046% allocated at IA1 (already spent at IA1) 0% allocated at IA2 |
3: PFS in patients with CPS ≥ 10 | 0.411% allocated at IA2 only |
4: OS in all patients | 0.039% allocated at IA1 (already spent at IA1) 0% allocated at IA2/IA3/final analysis (group sequential) |
5: OS in patients with CPS ≥ 1 | 0.75% allocated to IA1/IA2/IA3/final analysis (group sequential), which includes 0.036% spent at IA1 |
6: OS in patients with CPS ≥ 10 | 1.011% allocated to IA2/IA3/ final analysis (group sequential) |
7: ORR in all patients | 0.1% allocated at IA1 only (already spent at IA1) |
8: ORR in patients with CPS ≥ 1 | 0.1% allocated at IA1 only (already spent at IA1) |
IA1 = interim analysis 1; IA2 = interim analysis 2; ORR = objective response rate; OS = overall survival; PFS = progression-free survival.
Source: Clinical Study Report.15
Figure 3 displays the revised multiplicity strategy diagram of the study. The initial 1-sided alpha allocation for each hypothesis is shown in the rectangle representing the hypothesis. The weights for reallocation from each hypothesis to the others are represented in the numbers along the lines connecting hypotheses. Overall, 0.5% alpha was allocated to PFS end points, a 1.8% alpha was allocated to OS end points, and a 0.2% alpha was allocated to ORR end points.
Subgroup Analyses
To determine whether the treatment effect was consistent across various subgroups, the between-group treatment effect (with a nominal 95% CI) for the primary end points was estimated and plotted within each category of the following classification variables in all patients and in patients with PD-L1–positive tumours (CPS ≥ 1 and CPS ≥ 10):
chemotherapy on study (nab-paclitaxel versus paclitaxel versus gemcitabine and carboplatin; taxane versus gemcitabine and carboplatin)
tumour PD-L1 status (positive versus negative). Note: this subgroup analysis will only be conducted in the “all patients” population
prior treatment with same class of chemotherapy in the (neo)adjuvant setting (yes versus no).
prior (neo)adjuvant chemotherapy (yes versus no)
prior (neo)adjuvant taxane treatment (yes versus no)
prior (neo)adjuvant platinum treatment (yes versus no)
menopausal status (for females only; premenopausal versus postmenopausal)
age (< 65 years versus ≥ 65 years)
geographic region (Europe, Israel, North America, or Australia versus Asia versus rest of world)
ethnic origin (Hispanic versus non-Hispanic)
ECOG PS (0 versus 1)
HER2 status (2+ by immunohistochemistry versus 0 to 1+ by immunohistochemistry)
disease-free interval (de novo metastasis versus < 1 2 months versus ≥ 12 months)
number of metastatic sites (< 3 versus ≥ 3)
visceral disease (yes versus no)
lactate dehydrogenase (≥ 2.0 × upper limit of normal versus < 2.0 × upper limit of normal).
The subgroups that aligned with the CADTH review protocol included the following: ECOG PS, prior treatment with the same class of chemotherapy in the adjuvant or neoadjuvant setting, and chemotherapy on study. Only those subgroups identified in the CADTH review protocol are reported in the efficacy section.
Figure 3: Multiplicity Strategy for the KEYNOTE-355 Trial
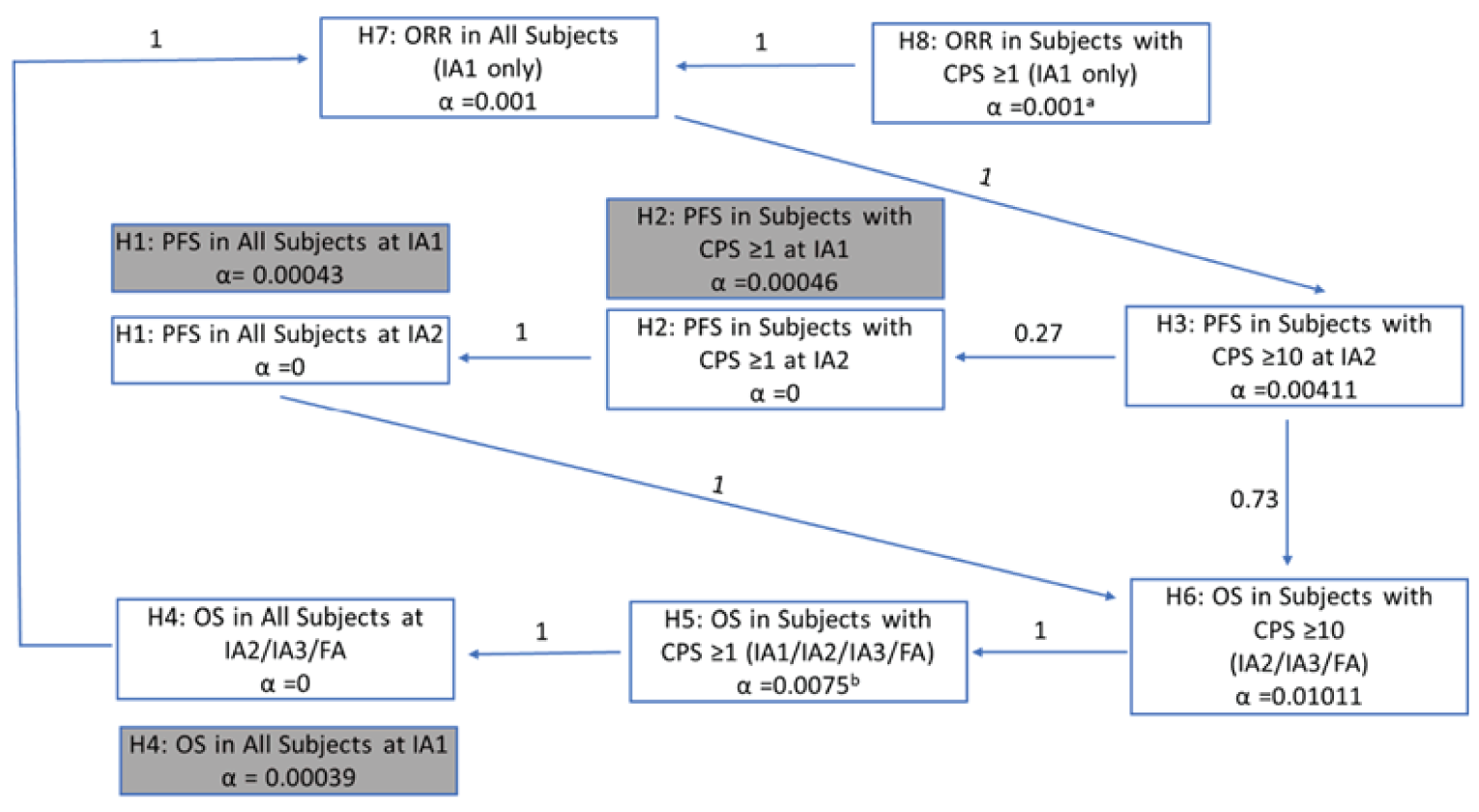
CPS = combined positive score; final analysis = final analysis; FA = final analysis; H = hypothesis; IA1 = interim analysis 1; IA2 = interim analysis 2; IA3 = interim analysis 3; ORR = objective response rate; OS = overall survival; PD-L1 = programmed cell death 1 ligand 1; PFS = progression-free survival.
Note: The shaded boxes represent the alpha that has already been spent at IA1 and will be considered lost for future analyses. These alphas will no longer be reallocated to other hypotheses under the graphical approach, nor can they be used to account for correlation among group sequential tests within each end point across different time points.
a Nominal alpha for testing will be calculated based on the Spiessens and Debois method accounting for correlation between ORR in all patients and ORR in patients with CPS ≥ 1. While the nominal alpha will be calculated and used for testing, the allocated alpha (0.001) will be passed to H7 when applicable.
b H5 alpha = 0.0075, which includes 0.00036 already spent at IA1.
Source: Clinical Study Report.15
Secondary Outcome Analyses
Health-Related Quality of Life
The patient-reported outcomes were considered secondary and exploratory objectives in this study, and no formal hypotheses were formulated. Nominal P values without multiplicity adjustment were provided and should be interpreted with caution. The treatment effect on patient-reported outcome score change from baseline was evaluated at the primary analysis time point. Between-group comparisons were performed and the differences in the least squares mean change from baseline at the primary analysis time point were reported, together with 95% CIs and nominal P values. In addition, model-based least squares mean scores with corresponding 95% CIs were provided by treatment group at the primary analysis time point.
Patients with confirmed progressive disease or those feeling worse due to a drug-related AE may have missing patient-reported outcome assessments. The missing data were handled using the constrained longitudinal data analysis model to obtain valid statistical analysis results. This method implicitly treats missing data as missing at random.
Descriptive statistics (e.g., mean and standard error) of change from baseline with no imputation for missing data of the following score/scales were also plotted: EORTC QLQ-C30 global health status and QoL, EORTC QLQ-C30 physical and emotional functioning, and EQ VAS.
Objective Response Rate
The stratified Miettinen and Nurminen method was used for the comparison of ORR between 2 treatment arms. The difference in ORR and its 95% CI from the stratified Miettinen and Nurminen method with strata weighting by sample size was reported. The stratification factors used for randomization were applied to the analysis.
The ORR hypotheses were tested according to the hypotheses testing plan. Sensitivity analyses were performed for ORR based on site investigator or local radiology review.
The ORR was included in the multiplicity testing strategy and is described in Table 11.
Duration of Response
The DOR was summarized descriptively using the nonparametric Kaplan-Meier method. Only the subset of patients who achieved complete or partial response was included in this analysis.
Table 12: Statistical Analysis of Efficacy End Points
End point | Statistical model | Sensitivity analyses |
|---|---|---|
Primary end points | ||
OS in all patients (hypothesis 3) and patients with PD-L1–positive tumours (hypothesis 4) |
|
|
PFS based on RECIST 1.1 assessed by a blinded CIV in all patients (hypothesis 1) and in patients with PD-L1–positive tumours (hypothesis 2) |
|
|
Secondary end points | ||
ORR based on RECIST 1.1 assessed by a blinded CIV in all patients and in patients with PD-L1–positive tumours | Stratified by Miettinen and Nurminen method | Patients with relevant data missing were considered nonresponders |
DOR based on RECIST 1.1 assessed by a blinded CIV in all patients and in patients with PD-L1–positive tumours | Summary statistics using Kaplan-Meier method | Table 10 provides censoring rules |
CIV = central imaging vendor; DOR = duration of response; ORR = objective response rate; OS = overall survival; PD-1 = programmed cell death 1 protein; PD-L1 = programmed cell death 1 ligand 1; PFS = progression-free survival; RECIST 1.1 = Response Evaluation Criteria in Solid Tumours Version 1.1.
Note: For stratified analyses, the stratification factors used for randomization were used as stratification factors for analysis.
Source: Clinical Study Report.15
Harms
Safety parameters were assessed via point estimates with 95% CIs provided for between-group comparisons using the Miettinen and Nurminen method. In addition, point estimates were provided by treatment group. Some adverse experiences (specific terms as well as system organ class terms) required that at least 4 patients in any treatment group exhibit the event. Given that many 95% CIs may be provided without adjustment for multiplicity, the CIs were regarded as a helpful descriptive measure to be used in review, not a formal method for assessing the statistical significance of the between-group differences in adverse experiences and predefined limits of change.
Planned Analyses
Three efficacy interim analyses were planned in addition to the final analysis for part 2 of the KEYNOTE-355 trial. Patients from part 1 (safety run-in) were not included in part 2 (efficacy evaluation).
Interim Analysis 1 (Final ORR Analysis)
The primary purpose of IA1 was to perform the final ORR, interim PFS, and interim OS analyses. The ORR analysis at IA1 is considered the final ORR analysis of the study. IA1 was to be performed after enrolment is completed, and approximately 9 months after the first 640 patients were randomized to part 2.
At IA1, ORR analyses were based on data from the first approximately 640 patients randomized to part 2 and were to be tested in all patients and patients with PD-L1–positive tumours. All patients randomized on or before the date the 640th patient in part 2 were randomized were to be included in the ORR analysis.
The success boundary to demonstrate ORR superiority at IA1 corresponds to an observed ORR difference of approximately 12.6% at 1-sided an alpha of 0.1% for all patients, and an observed ORR difference of approximately 14.1% at a nominal 1-sided alpha of approximately 0.145% for patients with PD-L1–positive tumours, if there were 640 patients in all patients and 480 patients in patients with PD-L1–positive tumours available for analysis (assuming a PD-L1 positivity prevalence of 75%).
Interim Analysis 2 (Final PFS Analysis)
The primary purpose of efficacy IA2 (data cut-off date: December 11, 2019) was to evaluate the superiority of pembrolizumab plus chemotherapy versus placebo plus chemotherapy in OS, and to perform the final PFS analysis. The analysis was performed approximately 12 months after the last patient was randomized.
Interim Analysis 3
The primary purpose of efficacy interim analysis 3 was to evaluate the superiority of pembrolizumab plus chemotherapy versus placebo plus chemotherapy in OS. The analysis was to be performed approximately 17 months after the last patient randomized.
Final Analysis (Final Overall Survival Analysis)
The final analysis of the study was driven by events and follow-up times, and was to be conducted after approximately 500 OS events have been observed among all patients, or after approximately 23 months since the last patient was randomized, whichever occurred later. The final analysis may be delayed for up to 4 months if fewer than 360 OS events have been observed among patients with PD-L1–positive tumours. The success boundary to demonstrate OS superiority at final analysis corresponds to an observed HR of approximately 0.80 (approximately 4.5 months improvement over control median OS of 17.5 months) at a 1-sided alpha of approximately 0.84% for all patients, and an observed HR of approximately 0.77 (approximately 5.4 months of improvement over a control median OS of 17.5 months) at a 1-sided alpha of approximately 0.84% for patients with PD-L1–positive tumours, if the planned numbers of OS events were analyzed, respectively.
A summary of the timing, sample size, and decision guidance of the 3 efficacy interim analyses and final analysis, assuming no alpha reallocation between hypotheses, is presented in Table 13. ORR boundaries assumed 640 randomized patients and a 75% PD-L1 prevalence and may be updated at the time of the analyses using the actual observed numbers. PFS and OS boundaries were based on the estimated number of events and may be updated at the time of the analyses according to the actual observed number of events, spending functions, and the spending time approach as noted above.
Table 13: Summary of Timing, Sample Size, and Decision Guidance of Efficacy Interim Analyses and Final Analysis
Analysis | Criteria for conduct of analysis | End point and testing population | Parameter | Efficacy bara | Futility barb |
|---|---|---|---|---|---|
Interim analysis 1: final ORR, interim PFS and interim OS analysis | IA1 will be conducted when enrolment is completed, and approximately 9 months after first 640 patients were randomized in part 2 | ORR in all patients | P value (1-sided) at boundary ORR difference at boundary | 0.001 12.6 percentage points | NA NA |
ORR inpatients with PD-L1–positive tumours | P value (1-sided) at boundary ORR difference at boundary | Approximately 0.00145c 14.1 percentage points | NA NA | ||
It is estimated that at IA1 approximately 500 PFS events among all patients, approximately 360 PFS events among patients with PD-L1–positive tumours, approximately 260 OS events among all patients, and approximately 185 OS events among patients with PD-L1–positive tumours will have been observed IA1 is estimated to occur approximately 4 months after last patient randomized | PFS in all patients | P value (1-sided) at boundary HR at boundary | 0.0005 Approximately 0.73 | NA NA | |
PFS in patients with PD-L1–positive tumours | P value (1-sided) at boundary HR at boundary | 0.0005 Approximately 0.69 | NA NA | ||
OS in all patients | P value (1-sided) at boundary HR at boundary | 0.0004 Approximately 0.64 | 0.5824 Approximately 1.03 | ||
OS in patients with PD-L1–positive tumours | P value (1-sided) at boundary HR at boundary | 0.0004 Approximately 0.59 | 0.5764 Approximately 1.03 | ||
Interim analysis 2: interim OS analysis, and final PFS analysis | IA2 will be conducted when approximately 12 months after last patient has been randomized It is estimated that at IA2 approximately 615 PFS events among all patients, approximately 445 PFS events among patients with PD-L1–positive tumours, approximately 380 OS events among all patients, and approximately 272 OS events among patients with PD-L1–positive tumours will have been observed | PFS in all patients | P value (1-sided) at boundary HR at boundary | 0.0008 Approximately 0.76 | NA NA |
PFS in patients with PD-L1–positive tumours | P value (1-sided) at boundary HR at boundary | 0.0008 Approximately 0.73 | NA NA | ||
OS in all patients | P value (1-sided) at boundary HR at boundary | 0.0032 Approximately 0.74 | 0.1566 Approximately 0.90 | ||
OS in patients with PD-L1–positive tumours | P value (1-sided) at boundary HR at boundary | 0.0031 Approximately 0.70 | 0.1498 Approximately 0.88 | ||
Interim analysis 3: interim OS analysis | IA3 will be conducted approximately 17 months after last patient is randomized It is estimated that at IA3 approximately 440 OS events among all patients, and 316 OS events among patients with PD-L1–positive tumours will have been observed | OS in all patients | P value (1-sided) at boundary HR at boundary | 0.0054 Approximately 0.77 | 0.0502 Approximately 0.85 |
OS in patients with PD-L1–positive tumours | P value (1-sided) at boundary HR at boundary | 0.0053 Approximately 0.74 | 0.0479 Approximately 0.82 | ||
Final analysis: final OS analysis | Final analysis will be conducted after approximately 500 OS events have been observed among all patients, or after approximately 23 months since the last patient is randomized, whichever occurs laterd It is estimated that at final analysis approximately 360 OS events will have been observed among patients with PD-L1–positive tumours | OS in all patients | P value (1-sided) at boundary HR at boundary | 0.0084 Approximately 0.80 | 0.0084 Approximately 0.80 |
OS in patients with PD-L1–positive tumours | P value (1-sided) at boundary HR at boundary | 0.0084 Approximately 0.77 | 0.0084 Approximately 0.77 |
HR = hazard ratio; IA1 = interim analysis 1; IA2 = interim analysis 2; IA3 = interim analysis 3; NA = not applicable; ORR = overall response rate; OS = overall survival; PD-L1 = programmed cell death 1 ligand 1; PFS = progression-free survival.
Source: Clinical Study Report.15
Analysis Populations
Efficacy Analysis Populations
The ITT population was analyzed for primary efficacy analyses. All randomized patients were included in this population in the treatment group to which they were randomized. The ITT population was further analyzed by subgroups of a CPS of 1 or higher and a CPS of 10 or higher.
Safety Analysis Populations
The APaT population was used for the analysis of safety data in the KEYNOTE-355 trial. The APaT population consisted of all randomized patients who received at least 1 study treatment. Patients were included in the treatment group corresponding to the study treatment they actually received for the analysis of safety data using the APaT population. At least 1 laboratory or vital sign measurement obtained subsequent to at least 1 dose of the study treatment is required as well as a baseline measurement for inclusion in the analysis of each specific parameter.
Patient-Reported Outcomes Analysis Populations
Patient-reported outcome analyses (for HRQoL) were based on the patient-reported outcome final analysis population, defined as all randomized patients who received at least 1 dose of study intervention and had completed at least 1 patient-reported outcome assessment analyses and who received at least 1 study treatment.
Protocol Amendments
The original protocol was approved on April 21, 2016. The final protocol was approved October 4, 2019. Five protocol amendments were made before the final analysis data-cut-off. No changes were made after the unblinding of data.
Amendment 1 (December 6, 2016) harmonized the pneumonitis exclusion criterion throughout the pembrolizumab program.
Amendment 2 (February 5, 2018) aligned the protocol with the most current label and safety information for pembrolizumab and added guidelines for dose modification in the event of myocarditis and updated guidelines for several other conditions.
Amendment 3 (August 31, 2018) adjusted the allocation of alpha over the primary end points and key secondary end points to allocate the initial alpha to ORR hypotheses and allow testing of ORR hypothesis at IA1 independent of the outcome of the other hypotheses.
Amendment 4 (March 20, 2019) changed the timing of the final analysis from OS-driven to both OS-event– and follow-up-time–driven to ensure adequate follow-up duration at time of the final analysis.
Amendment 5 (October 4, 2019) changed the objectives, hypotheses, and statistical analysis plan to include patients with PD-L1–positive tumours with a higher CPS cut-off (≥ 10).
Results
Patient Disposition
By the final analysis data cut-off (June 15, 2021), 1,372 patients had been screened, 525 patients had failed screening, and 847 patients had been successfully randomized in a 2:1 ratio to receive either pembrolizumab plus chemotherapy (N = 566) or placebo plus chemotherapy (N = 281). All but 4 randomized patients received at least 1 dose of the study intervention. A summary of the patient disposition at the final analysis data cut-off is presented in Table 14.
As of the final analysis data cut-off, a total of 707 patients had discontinued the study. The major reason for discontinuation in the subset of patients with a PD-L1 CPS of 10 or higher was death (68.6% versus 79.6% in the pembrolizumab and placebo group, respectively). Similarly, a total of 778 (92.3%) patients had discontinued treatment. The discontinuation rate was similar between the 2 treatment groups in all patients and in patients with a PD-L1 CPS of 10 or higher. The most common reason for discontinuation of treatment in the subset of patients with a PD-L1 CPS of 10 or higher was progressive disease (58% pembrolizumab group versus 68.9% placebo group) followed by clinical progression (58% pembrolizumab group versus 68.9% placebo group).
Table 14: Patient Disposition at Final Analysis — Intention-to-Treat Population
Characteristic | Patients with PD-L1 CPS ≥ 10 | All patients | ||
|---|---|---|---|---|
Pembrolizumab plus chemotherapy | Placebo plus chemotherapy | Pembrolizumab plus chemotherapy | Placebo plus chemotherapy | |
Screened, n | 1,372 | |||
Randomized, n | 220 | 103 | 566 | 281 |
Discontinued in treatment, n (%) | 189 (86.6) | 95 (92.2) | 514 (91.5) | 264 (94.0) |
Progressive disease | 127 (58.0) | 71 (68.9) | 362 (64.4) | 197 (70.1) |
Clinical progression | 17 (7.8) | 11 (10.7) | 58 (10.3) | 38 (13.5) |
Adverse event | 21 (9.6) | 5 (4.9) | 46 (8.2) | 15 (5.3) |
Withdrawal by patient | 14 (6.4) | 4 (3.9) | 32 (5.7) | 10 (3.6) |
Physician decision | 7 (3.2) | 3 (2.9) | 12 (2.1) | 3 (1.1) |
Complete response | 3 (1.4) | 1 (1.0) | 4 (0.7) | 1 (0.4) |
Status not recorded | 3 (1.4) | 3 (2.9) | 9 (1.6) | 5 (1.8) |
Discontinued study, n (%) | 160 (72.7) | 84 (81.6) | 468 (82.7) | 239 (8 5.1) |
Death | 151 (68.6) | 82 (79.6) | 447 (79.0) | 233 (82.9) |
Withdrawal by patient | 9 (4.1) | 2 (1.9) | 21 (3.7) | 6 (2.1) |
Status not recorded | 60 (27.3) | 19 (18.4) | 98 (17.3) | 42 (14.9) |
Intention-to-treat population, n | 220 | 103 | 566 | 281 |
Patient-reported outcome population | 216 | 100 | 555 | 278 |
Safety/APaT population, n (%) | 220 | 103 | 562 | 281 |
APaT = all patients as treated; CPS = combined positive score; PD-L1 = programmed cell death 1 ligand 1.
Notes: Clinical progression and progressive disease were based on investigator assessments and may be different from the data used in the primary analysis. Progressive disease refers to disease progression based on Response Evaluation Criteria in Solid Tumours Version 1.1 and does not include clinical progression. Study medication discontinuation refers to discontinuation of all study medications. Patients without a completed study medication discontinuation form or without a completed study disposition form were labelled “status not recorded.” Data cut-off date: June 15, 2021.
Source: Clinical Study Report.15
Premature Unblinding
In total, 150 premature unblinding events occurred due to the following reasons:
sponsor-approved nonemergency unblinding request for discontinued patients to determine subsequent therapy in patients failing study intervention; N = 119
inadvertent unblinding; N = 15
emergency unblinding through the call centre; N = 16.
Protocol Deviations
Important protocol deviations are highlighted in Table 15. Overall, the number of clinically important protocol deviations was low in both groups (3.5% in the pembrolizumab group and 2.5% in the placebo group).
Table 15: Summary of Protocol Deviations Considered to Be Clinically Important by Trial Investigators at Final Analysis — ITT Population
Protocol deviation | Pembrolizumab plus chemotherapy | Placebo plus chemotherapy | ||
|---|---|---|---|---|
n | (%) | n | (%) | |
Patients in population:
| 566 20 546 | (3.5) (96.5) | 281 7 274 | (2.5) (97.5) |
Inclusion/exclusion criteria | 17 | (3.0) | 5 | (1.8) |
Patients who do not have centrally confirmed TNBC, as defined by the most recent ASCO or CAP guidelines. | 3 | (0.5) | 1 | (0.4) |
Patients who do not have completed treatment for stage I to III breast cancer, if indicated, and for whom at least 6 months has elapsed between the completion of treatment with curative intent (date of primary breast tumour surgery or date of last adjuvant chemotherapy administration, whichever occurred last) and first documented local or distant disease recurrence. Patients who received taxane, gemcitabine, or platinum drugs in the (neo)adjuvant setting can only be treated with same class of chemotherapy, if 12 months or more have elapsed between the completion of treatment with curative intent (date of primary breast tumour surgery or date of last adjuvant chemotherapy administration, whichever occurred last) and first documented local or distant disease recurrence. | 11 | (1.9) | 3 | (1.1) |
Patients who do not have locally recurrent inoperable breast cancer not previously treated with chemotherapy and which cannot be treated with curative intent or do not have metastatic breast cancer not previously treated with chemotherapy. Some patients with a history of locally recurrent breast cancer, which was previously treated with curative intent, may be eligible. | 3 | (0.5) | 1 | (0.4) |
Informed consent Patient had no documented initial consent to enter the trial. | 2 | (0.4) | 1 | (0.4) |
2 | (0.4) | 1 | (0.4) | |
Safety reporting | 1 | (0.2) | 1 | (0.4) |
Patient had a reportable safety event and/or follow-up safety event information that was not reported per the timelines outlined in the protocol. | 1 | (0.2) | 1 | (0.4) |
ASCO = American Society of Clinical Oncology; CAP = College of American Pathologists; ITT = intention-to-treat; TNBC = triple-negative breast cancer.
Notes: Every patient is counted a single time for each applicable row and column. Data cut-off date: June 15, 2021.
Source: Clinical Study Report.15
Exposure to Study Treatments
A summary of drug exposure is presented in Table 16 and a summary of the duration of exposure is presented in Table 17. The median duration of exposure to study intervention for all drugs in all patients was generally similar between the pembrolizumab plus chemotherapy group (26.4 weeks; range = 0.1 to 212.1 weeks) and the placebo plus chemotherapy group (23.1 weeks; range = 0.1 to 224.1weeks). The median exposure time of all drugs in patients with a PD-L1 CPS of 10 or higher was ||||||||||||||||||||||||||| in patients in the pembrolizumab plus chemotherapy group versus the placebo plus chemotherapy group, respectively.
In the subpopulation with a PD-L1 CPS of 10 or higher, the median number of weeks on therapy was ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||| for placebo in pembrolizumab versus placebo groups, respectively. The companion chemotherapies such as nab-paclitaxel ||||||||||||||||||||||||||||||||||||) and paclitaxel (|||||||||||||||||||||||||||||||||||| were all consistently higher in the median number of weeks on treatment in the pembrolizumab group than in the placebo group. Gemcitabine and carboplatin were roughly balanced with or a little higher than the placebo group and these patterns of differences in treatment exposure between the 2 groups were consistently observed in all patients.
As of the final analysis data cut-off, median duration of follow-up in the ITT population was 16.7 months (range, 0.2 to 53.1 months) and was similar for both treatment groups. Median duration of follow-up was |||||||||||||||||||||||||||||||||||||||||||||) in patients with a PD-L1 CPS of 10 or higher.
Table 16: Summary of Drug Exposure in Patients With PD-L1 CPS ≥ 10 and All Patients at Final Analysis — APaT Population
Timing | Patients with PD-L1 CPS ≥ 10 | All patients | ||
|---|---|---|---|---|
Pembrolizumab plus chemotherapy | Placebo plus chemotherapy | Pembrolizumab plus chemotherapy | Placebo plus chemotherapy | |
Patients in population | 219 | 103 | 562 | 281 |
All drugs | ||||
Number of weeks on therapy | ||||
n | ||||||||| | ||||||||| | 562 | 281 |
Median | ||||||||| | ||||||||| | 26.4 | 23.1 |
Range | ||||||||| | ||||||||| | 0.1 to 212.1 | 0.1 to 224.1 |
Pembrolizumab and placebo | ||||
Number of weeks on therapy | ||||
n | ||||||||| | ||||||||| | 562 | 281 |
Median | ||||||||| | ||||||||| | 24.2 | 22.1 |
Range | ||||||||| | ||||||||| | 0.1 to 140.1 | 0.1 to 119.6 |
Number of administrations | ||||
n | ||||||||| | ||||||||| | 562 | 281 |
Median | ||||||||| | ||||||||| | 8.0 | 8.0 |
Range | ||||||||| | ||||||||| | 1.0 to 35.0 | 1.0 to 35.0 |
Nab-paclitaxel | ||||
Number of weeks on therapy | ||||
n | ||||||||| | ||||||||| | 174 | 95 |
Median | ||||||||| | ||||||||| | 23.1 | 18.1 |
Range | ||||||||| | ||||||||| | 0.1 to 212.1 | 0.1 to 208.1 |
Number of administrations | ||||
n | ||||||||| | ||||||||| | 174 | 95 |
Median | ||||||||| | ||||||||| | 18.0 | 14.0 |
Range | ||||||||| | ||||||||| | 1.0 to 159.0 | 1.0 to 143.0 |
Paclitaxel | ||||
Number of weeks on therapy | ||||
n | ||||||||| | ||||||||| | 81 | 32 |
Median | ||||||||| | ||||||||| | 21.6 | 17.4 |
Range | ||||||||| | ||||||||| | 1.1 to 108.9 | 0.1 to 224.1 |
Number of administrations | ||||
n | ||||||||| | ||||||||| | 81 | 32 |
Median | ||||||||| | ||||||||| | 16.0 | 13.5 |
Range | ||||||||| | ||||||||| | 2.0 to 79.0 | 1.0 to 167.0 |
Gemcitabine | ||||
Number of weeks on therapy | ||||
n | ||||||||| | ||||||||| | 309 | 154 |
Median | ||||||||| | ||||||||| | 22.1 | 23.1 |
Range | ||||||||| | ||||||||| | 0.1 to 199.1 | 0.1 to 215.7 |
Number of administrations | ||||
n | ||||||||| | ||||||||| | 309 | 154 |
Median | ||||||||| | ||||||||| | 12.0 | 13.0 |
Range | ||||||||| | ||||||||| | 1.0 to 98.0 | 1.0 to 137.0 |
Carboplatin | ||||
Number of weeks on therapy | ||||
n | ||||||||| | ||||||||| | 309 | 154 |
Median | ||||||||| | ||||||||| | 22.1 | 22.9 |
Range | ||||||||| | ||||||||| | 0.1 to 199.1 | 0.1 to 215.7 |
Number of administrations | ||||
n | ||||||||| | ||||||||| | 309 | 154 |
Median | ||||||||| | ||||||||| | 12.0 | 13.0 |
Range | ||||||||| | ||||||||| | 1.0 to 98.0 | 1.0 to 137.0 |
APaT = all patients as treated; CPS = combined positive score; NA = not applicable; PD-L1 = programmed cell death 1 ligand 1.
Notes: Patients who did not have neoadjuvant treatments but had surgery were included in the APaT population in neoadjuvant phase. Patients who had postsurgery radiation therapy but did not have adjuvant treatment were included in the APaT population in the adjuvant phase. Data cut-off date: June 15, 2021.
Sources: Clinical Study Report15 and sponsor’s additional information package.31
Table 17: Exposure by Duration in All Patients — APaT Population
Exposure | Pembrolizumab plus chemotherapy (N = 562) | Placebo plus chemotherapy (N = 281) | ||
|---|---|---|---|---|
n | Person-months | n | Person-months | |
Treatment duration | ||||
> 0 month | 562 | 5,059.1 | 281 | 2,189.6 |
≥ 1 month | 534 | 5,048.7 | 266 | 2,182.5 |
≥ 3 months | 440 | 4,860.9 | 214 | 2,075.2 |
≥ 6 months | 282 | 4,176.4 | 125 | 1,685.4 |
≥ 12 months | 143 | 2,981.4 | 47 | 1,035.4 |
APaT = all patients as treated.
Notes: Each patient is counted once on each applicable duration category row. Duration of exposure is the time from the first dose date to the last dose date.
Source: Clinical Study Report.15
A summary of concomitant medication use (incidence > 30% in 1 or more treatment groups) is presented in Table 18.
The reported concomitant medications were generally balanced between the 2 treatment groups in part 2, with the exception that the following were higher (≥ 5 percentage point difference) in the pembrolizumab plus chemotherapy group:
antidiarrheals, intestinal anti-inflammatory or anti-infective medications (17.1% versus 9.3%)
medications for constipation (30.6% versus 24.6%)
systemic antibacterial medications (56.2% versus 47.3%)
topical corticosteroids (18.3% versus 12.5%)
thyroid therapy (25.1% versus 13.5%).
Table 18: Patients With Specific Concomitant Medication at Final Analysis (Incidence ≥ 30% in 1 or More Treatment Groups) in Patients With PD-L1 CPS ≥ 10 and All Patients — APaT Population
Medication | Patients with PD-L1 CPS ≥ 10 | All patients | ||
|---|---|---|---|---|
Pembrolizumab plus chemotherapy n (%) | Placebo plus chemotherapy n (%) | Pembrolizumab plus chemotherapy n (%) | Placebo plus chemotherapy n (%) | |
Patients in population | ||||||||| | ||||||||| | 562 | 281 |
with one or more concomitant medications | ||||||||| | ||||||||| | 561 (99.8) | 281 (100.0) |
with no concomitant medication | ||||||||| | ||||||||| | 0 | 0 |
Alimentary tract and metabolism | ||||
Antiemetics and antinauseants | ||||||||| | ||||||||| | 432 (76.9) | 208 (74.0) |
Ondansetron | ||||||||| | ||||||||| | 252 (44.8) | 115 (40.9) |
Antineoplastic and immunomodulating drugs | ||||
Immunostimulants | ||||||||| | ||||||||| | 174 (31.0) | 92 (32.7) |
Filgrastim | ||||||||| | ||||||||| | 139 (24.7) | 71 (25.3) |
Nervous system | ||||
Analgesics | ||||||||| | ||||||||| | 384 (68.3) | 191 (68.0) |
Acetaminophen | ||||||||| | ||||||||| | 248 (44.1) | 111 (39.5) |
Systemic hormonal preparations, excluding sex hormones and insulins | ||||
Corticosteroids for systemic use | ||||||||| | ||||||||| | 440 (78.3) | 210 (74.7) |
Dexamethasone | ||||||||| | ||||||||| | 306 (54.4) | 142 (50.5) |
APaT = all patients as treated; CPS = combined positive score; PD-L1 = programmed cell death 1 ligand 1.
Notes: Every patient is counted a single time for each applicable specific concomitant medication. A patient with multiple concomitant medications within a medication category is counted a single time for that category. Database cut-off date: June 15, 2021
Sources: Clinical Study Report15 and sponsor’s additional information package.31
A summary of subsequent therapy use is presented in Table 19. A lower percentage of patients in the pembrolizumab plus chemotherapy group received subsequent anticancer treatment compared with the placebo plus chemotherapy group in all patients (60.5% versus 69.0%, respectively) and in patients with PD-L1–positive tumours (||||||||||||||||||||||||||||||||||||). The most common type of subsequent therapy administered in both treatment groups was antineoplastic drugs. More patients in the placebo plus chemotherapy group received subsequent immunotherapy than did patients in the pembrolizumab plus chemotherapy group in the subset of patients with PD-L1–positive tumours (CPS ≥ 10) (||||||||||||||||||||||||||||||||||||||||||||||||||||||).
Table 19: Patients With Subsequent Antineoplastic Therapy or Immunotherapy Use (Incidence > 10% in 1 or More Treatment Groups) in Patients With PD-L1 CPS ≥ 10 and All Patients — APaT Population
Medication | Patients with PD-L1 CPS ≥ 10 | All patients | ||
|---|---|---|---|---|
Pembrolizumab plus chemotherapy | Placebo plus chemotherapy | Pembrolizumab plus chemotherapy | Placebo plus chemotherapy N = 281 | |
Patients in population, n (%) | ||||||||| | ||||||||| | 562 | 281 |
with 1 or more subsequent antineoplastic therapy | ||||||||| | ||||||||| | 340 (60.5) | 194 (69.0) |
with no subsequent antineoplastic therapy | ||||||||| | ||||||||| | 222 (39.5) | 87 (31.0) |
Antineoplastic and immunomodulating drugs | ||||
Antineoplastic drugs | ||||||||| | ||||||||| | 339 (60.3) | 193 (68.7) |
Capecitabine | ||||||||| | ||||||||| | 179 (31.9) | 104 (37.0) |
Carboplatin | ||||||||| | ||||||||| | 75 (13.3) | 42 (14.9) |
Cyclophosphamide | ||||||||| | ||||||||| | 87 (15.5) | 51 (18.1) |
Doxorubicin | ||||||||| | ||||||||| | 53 (9.4) | 26 (9.3) |
Eribulin mesylate | ||||||||| | ||||||||| | 94 (16.7) | 53 (18.9) |
Gemcitabine | ||||||||| | ||||||||| | 66 (11.7) | 39 (13.9) |
Paclitaxel | ||||||||| | ||||||||| | 82 (14 0.6) | 43 (15.3) |
Vinorelbine tartrate | ||||||||| | ||||||||| | 59 (10.5) | 38 (13.5) |
Immunotherapy | ||||
Patients in population | ||||||||| | ||||||||| | 562 | 281 |
with 1 or more subsequent immunotherapy | ||||||||| | ||||||||| | 13 (2.3) | 27 (9.6) |
with no subsequent immunotherapy | ||||||||| | ||||||||| | 549 (97.7) | 254 (90.4) |
APaT = all patients as treated; CPS = combined positive score; PD-L1 = programmed cell death 1 ligand 1.
Notes: Every patient is counted a single time for each applicable specific medication. A patient with multiple medications within a medication category is counted a single time for that category. A medication class or specific medication appears on this report only if its incidence in 1 or more of the columns meets the incidence criterion in the report title, after rounding. Data cut-off date: June 15, 2021.
Sources: Clinical Study Report15 and sponsor’s additional information package.31
Efficacy
Only those efficacy outcomes and analyses of subgroups identified in the review protocol are reported. Additional efficacy results for patients with a PD-L1 CPS > 1 are provided in Appendix 2.
Overall Survival
A summary of OS results at the final analysis data cut-off are presented in Table 20 and Figure 4. By the final analysis data cut-off, in patients with a PD-L1 CPS of 10 or higher, 155 of 220 predefined events had occurred in the pembrolizumab group, representing approximately 70.5% of OS events compared to 81.6% in the placebo group. The HR between groups was 0.73 (95% CI, 0.55 to 0.95) and the observed 1-sided P value of P = 0.0093 successfully crossed the prespecified efficacy boundary at the final analysis (the multiplicity-adjusted, 1-sided, nominal alpha level was 0.0113). The primary end point of OS was therefore met in patients with PD-L1–positive tumours (CPS ≥ 10). However, there was no significant difference in OS events in the all patients group (HR = 0.89, 95% CI, 0.76 to 1.05; P = 0.0797). The OS results for all patients were not formally tested given the OS results for patients with a PD-L1 CPS of 1 or higher did not reach statistical significance as defined by the prespecified analysis plan. The median OS was longer for patients with PD-L1–positive tumours (CPS ≥ 10) in the pembrolizumab plus chemotherapy group (23 months, 95% CI, 19 to 26.3) compared with the placebo plus chemotherapy group (16.1 months, 95% CI, 12.6 to 18.8).
Table 20: Overall Survival at Final Analysis in Patients With PD-L1 CPS ≥ 10 and All Patients — ITT Population
Overall survival | Patients with PD-L1 CPS ≥ 10 | All patients | ||
|---|---|---|---|---|
Pembrolizumab plus chemotherapy (N = 220) | Placebo plus chemotherapy (N = 103) | Pembrolizumab plus chemotherapy (N = 566) | Placebo plus chemotherapy (N = 281) | |
Number of events (%) | 155 (70.5) | 84 (81.6) | 460 (81.3) | 238 (84.7) |
Kaplan-Meier estimates (months)a | ||||
Median (95% CI) | 23.0 (19.0 to 26.3) | 16.1 (12.6 to 18.8) | 17.2 (15.3 to 19.0) | 15.5 (13.9 to 17.2) |
First quartile to third quartile | 10.3 to NR | 8.6 to 30.3 | 8.9 to 32.9 | 9.0 to 27.6 |
Person-months | 5,430.4 | 2,091.1 | 11,759.5 | 5,422.7 |
Event rate per 100 person-months | 2.9 | 4.0 | 3.9 | 4.4 |
Hazard ratio (95% CI)b | 0.73 (0.55 to 0.95) | 0.89 (0.76 to 1.05) | ||
P value | 0.0093c | 0.0797d | ||
OS rate at month 6, % (95% CI) | 88.6 (83.5 to 92.1) | 88.3 (80.4 to 93.2) | 86.4 (83.2 to 88.9) | 87.9 (83.4 to 91.2) |
OS rate at month 12, % (95% CI) | 70.7 (64.1 to 76.2) | 64.1 (54.0 to 72.5) | 64.5 (60.4 to 68.3) | 62.2 (56.2 to 67.5) |
OS rate at month 18, % (95% CI) | 58.3 (51.4 to 64.5) | 44.7 (34.9 to 53.9) | 47.8 (43.6 to 51.9) | 41.8 (36.0 to 47.5) |
OS rate at month 24, % (95% CI) | 48.2 (41.4 to 54.6) | 34.0 (25.0 to 43.1) | 35.5 (31.6 to 39.5) | 30.4 (25.1 to 35.8) |
CI = confidence interval; ITT = intention-to-treat; NR = not reached; OS = overall survival.
Note: Data cut-off date: June 15, 2021
aFrom product-limit (Kaplan-Meier) method for censored data.
bBased on Cox regression model with the Efron method of tie handling with treatment as a covariate stratified by chemotherapy on study (taxane vs. gemcitabine and carboplatin) and prior treatment with same class of chemotherapy in the (neo)adjuvant setting (yes vs. no).
cThe multiplicity-adjusted, 1-sided, prespecified P value boundary for statistical significance was P = 0.0113. One-sided P value based on log-rank test stratified by chemotherapy on study (taxane vs. gemcitabine and carboplatin) and prior treatment with same class of chemotherapy in the (neo)adjuvant setting (yes vs. no).
dNominal P value (i.e., not multiplicity-adjusted).
Source: Clinical Study Report.15
Subgroup Analyses
A summary of OS results by subgroup in patients with a PD-L1 CPS of 10 or higher is presented in Table 21. The HR of OS across the different subgroups analyzed was generally consistent with the primary finding in the main analysis. Overall results within subgroups were similar, except for chemotherapy on study. Patients who received taxanes as chemotherapy (e.g., nab-paclitaxel and paclitaxel) had lower OS HRs (0.63 and 0.34, respectively) compared with those given gemcitabine and carboplatin (0.88). However, given the exploratory nature, small sample sizes, and lack of statistical testing, subgroup results should be interpreted with caution.
Figure 4: Kaplan-Meier Estimates of OS at Final Analysis in Patients With PD-L1 CPS ≥ 10 — ITT Population
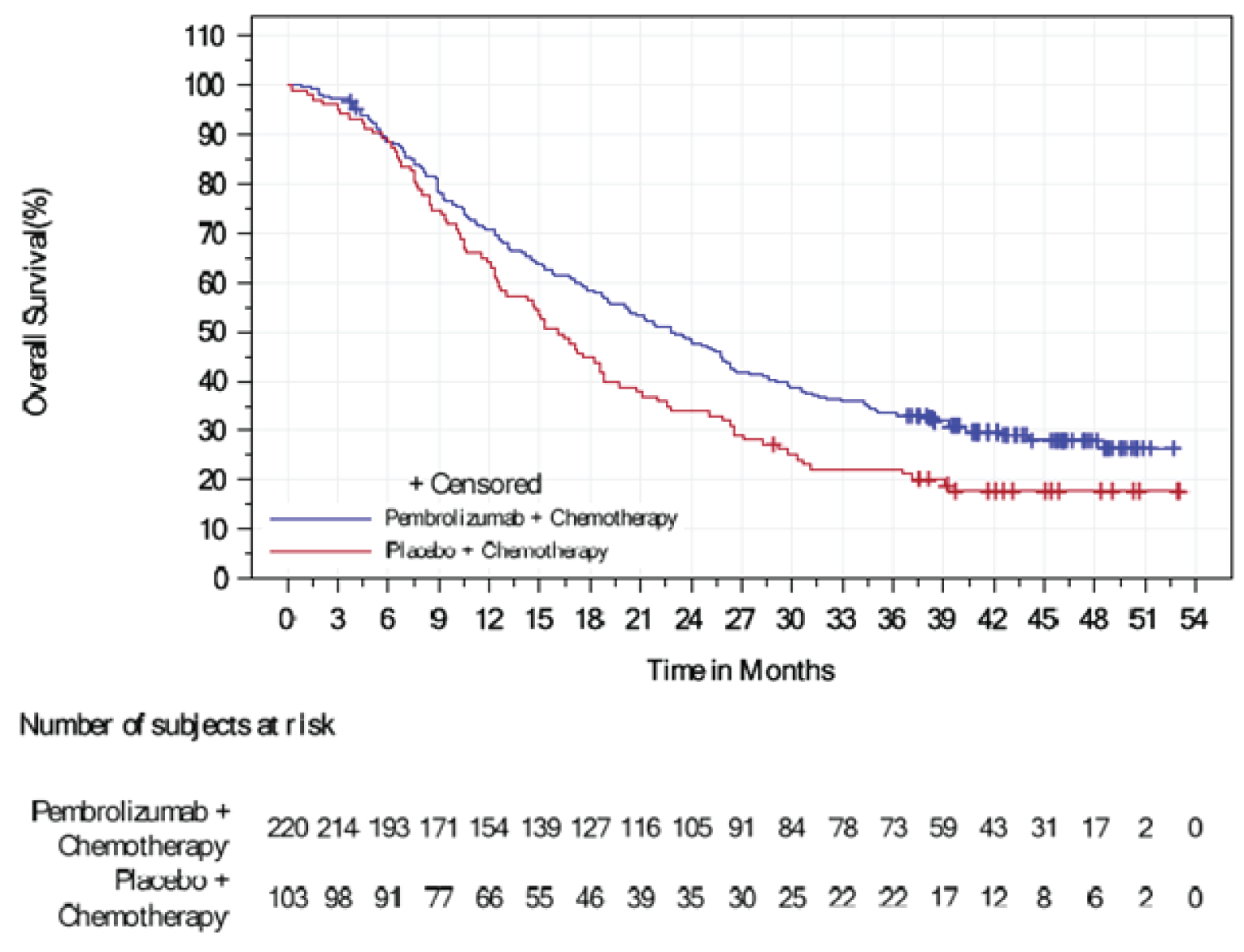
CPS = combined positive score; ITT = intention-to-treat; OS = overall survival; PD-L1 = programmed cell death 1 ligand 1.
Table 21: Subgroup Analysis of OS in Patients With PD-L1 CPS ≥ 10 — ITT Population
Subgroups | Pembrolizumab plus chemotherapy (N = 220) | Placebo plus chemotherapy (N = 103) | Pembrolizumab plus chemotherapy vs. placebo plus chemotherapy | ||||
|---|---|---|---|---|---|---|---|
N | Number of events | (%) | N | Number of events | (%) | Hazard ratio (95% CI)a | |
Primary analysis (PD-L1 CPS ≥ 10) | 220 | 155 | 70.5 | 103 | 84 | 81.6 | 0.73 (0.55 to 0.95) |
Chemotherapy on study (IVRS) | |||||||
Nab-paclitaxel | 63 | 39 | 61.9 | 36 | 29 | 80.6 | 0.63 (0.39 to 1.03) |
Paclitaxel | 33 | 22 | 66.7 | 11 | 10 | 90.9 | 0.34 (0.16 to 0.72) |
Gemcitabine and carboplatin | 124 | 94 | 75.8 | 56 | 45 | 80.4 | 0.88 (0.61 to 1.25) |
Prior treatment with same class of chemotherapy in the adjuvant or neoadjuvant setting (IVRS) | |||||||
Yes | 46 | 31 | 67.4 | 19 | 16 | 84.2 | 0.60 (0.32 to 1.09) |
No | 174 | 124 | 71.3 | 84 | 68 | 81.0 | 0.74 (0.55 to 1.00) |
ECOG PS | |||||||
0 | 134 | 85 | 63.4 | 62 | 48 | 77.4 | 0.70 (0.49 to 1.00) |
1 | 86 | 70 | 81.4 | 41 | 36 | 87.8 | 0.70 (0.47 to 1.05) |
CI = confidence interval; CPS = combined positive score; ECOG PS = European Cooperative Oncology Group Performance Status; ITT = intention-to-treat; IVRS = integrated voice recognition system; OS = overall survival; PD-L1 = programmed cell death 1 ligand 1.
Note: Data cut-off date: June 15, 2021.
aAnalysis (hazard ratio and 95% CI) in the overall population is based on Cox regression model with the Efron method of tie handling with treatment as a covariate stratified by chemotherapy on study (taxane vs. gemcitabine and carboplatin), tumour PD-L1 status (CPS ≥ 1 vs. CPS < 1) and prior treatment with same class of chemotherapy in the (neo)adjuvant setting (yes vs. no); analysis in the subgroups is based on the unstratified Cox model. If any level of a subgroup variable has fewer than 30 patients, subgroup analysis is not performed in that level of the subgroup variable.
Source: Clinical Study Report.15
Health-Related Quality of Life
Findings presented are for the final analysis data cut-off using the final analysis population.
EORTC QLQ-C30
Compliance rates were similar at baseline for the EORTC QLQ-C30 in both the pembrolizumab plus chemotherapy and placebo plus chemotherapy groups (≥ 93%). After 15 weeks, compliance rates were 87.7% and 81.1% in the pembrolizumab and placebo groups, respectively. HRQoL estimates measured up to week 15 may not provide an accurate picture of patients’ experiences with the pembrolizumab plus chemotherapy combination for a prolonged period of time.
Change from baseline for the EORTC QLQ-C30 global health status and QoL emotional and physical functioning scales, and symptom or item scales at week 15 in patients with a PD-L1 CPS of 10 or higher are presented in Figure 5 and Figure 6, respectively. Over 15 weeks of follow-up, there was either no decrease or a similar decrease in the prespecified global health status and QoL physical and emotional functioning scores observed for both treatment groups. Among patients with PD-L1–positive tumours (CPS ≥ 10), the least squares mean change from baseline to week 15 in scores for the EORTC QLQ-C30 global health status and QoL and symptom scales were similar between the 2 treatment groups. Similar results were observed among all patients.
Analysis of time to deterioration for the EORTC QLQ-C30 across the emotional functioning, physical functioning, and global health status scales are presented in Table 23. Overall, there was no difference in time to deterioration in the EORTC QLQ-C30 global health status and QoL emotional and physical functioning scores between the pembrolizumab plus chemotherapy and placebo plus chemotherapy groups.
Table 22: Analysis of Change From Baseline in EORTC QLQ-C30 Global Health Status and QoL at Week 15 in Patients With PD-L1 CPS ≥ 10 — Final Analysis Population
Treatment | Pembrolizumab plus chemotherapy (N = 216) | Placebo plus chemotherapy (N = 100) |
|---|---|---|
Global health status | ||
Baseline, n | 201 | 94 |
Mean (SD) | 67.54 (21.865) | 64.54 (21.514) |
Week 15, n | 166 | 70 |
Mean (SD) | 66.32 (19.318) | 66.07 (22.085) |
Change from baseline at week 15, LS mean (95% CI)a | −2.69 (−5.86 to 0.48) | −0.88 (−5.41 to 3.64) |
Difference in LS means (95% CI) | −1.81 (−6.92 to 3.30) | |
P value | 0.4865b | |
Physical functioning, n | ||
Baseline, n | 201 | 94 |
Mean (SD) | 81.56 (18.074) | 78.30 (19.843) |
Week 15, n | 166 | 70 |
Mean (SD) | 76.91 (21.268) | 75.33 (24.273) |
Change from baseline at week 15, LS mean (95% CI)a | −6.76 (−9.89 to −3.62) | −5.71 (−10.41 to −1.01) |
Difference in LS means (95% CI) | −1.05 (−6.59 to 4.50) | |
P value | 0.7102 | |
Emotional functioning | ||
Baseline, n | 201 | 94 |
Mean (SD) | 73.34 (19.131) | 72.52 (19.774) |
Week 15, n | 166 | 70 |
Mean (SD) | 74.55 (22.422) | 74.29 (24.399) |
Change from baseline at week 15, LS mean (95% CI)a | −0.75 (−3.92 to 2.43) | 0.69 (−4.07 to 5.44) |
Difference in LS means (95% CI) | −1.43 (−7.03 to 4.16) | |
P value | 0.6149 | |
CI = confidence interval; CPS = combined positive score; EORTC QLQ-C30 = European Organisation for Research and Treatment of Cancer Quality of Life Questionnaire Core 30; LS = least squares; PD-L1 = programmed cell death 1 ligand 1; QoL = quality of life; SD = standard deviation.
Notes: For baseline and week 15, N is the number of patients in each treatment group with nonmissing assessments at the specific time point; for change from baseline, N is the number of patients in the analysis population in each treatment group. Data cut-off date: June 15, 2021.
aBased on a constrained longitudinal data analysis model with the patient-reported outcome scores as the response variable, and treatment by time point interaction, and stratum (defined by stratification factors of chemotherapy on study [taxane vs. gemcitabine and carboplatin] and prior treatment with same class of chemotherapy in the [neo]adjuvant setting [yes vs. no]) as covariates.
bNominal P value (i.e., the type I error rate has not been controlled); 2-sided P value.
Source: Clinical Study Report.15
Figure 5: Change From Baseline for EORTC QLQ-C30 Global Health Status and QoL and Functional Scales at Week 15 (LS Mean Change and 95% CI) in Patients With PD-L1 CPS ≥ 10 — Final Analysis Population
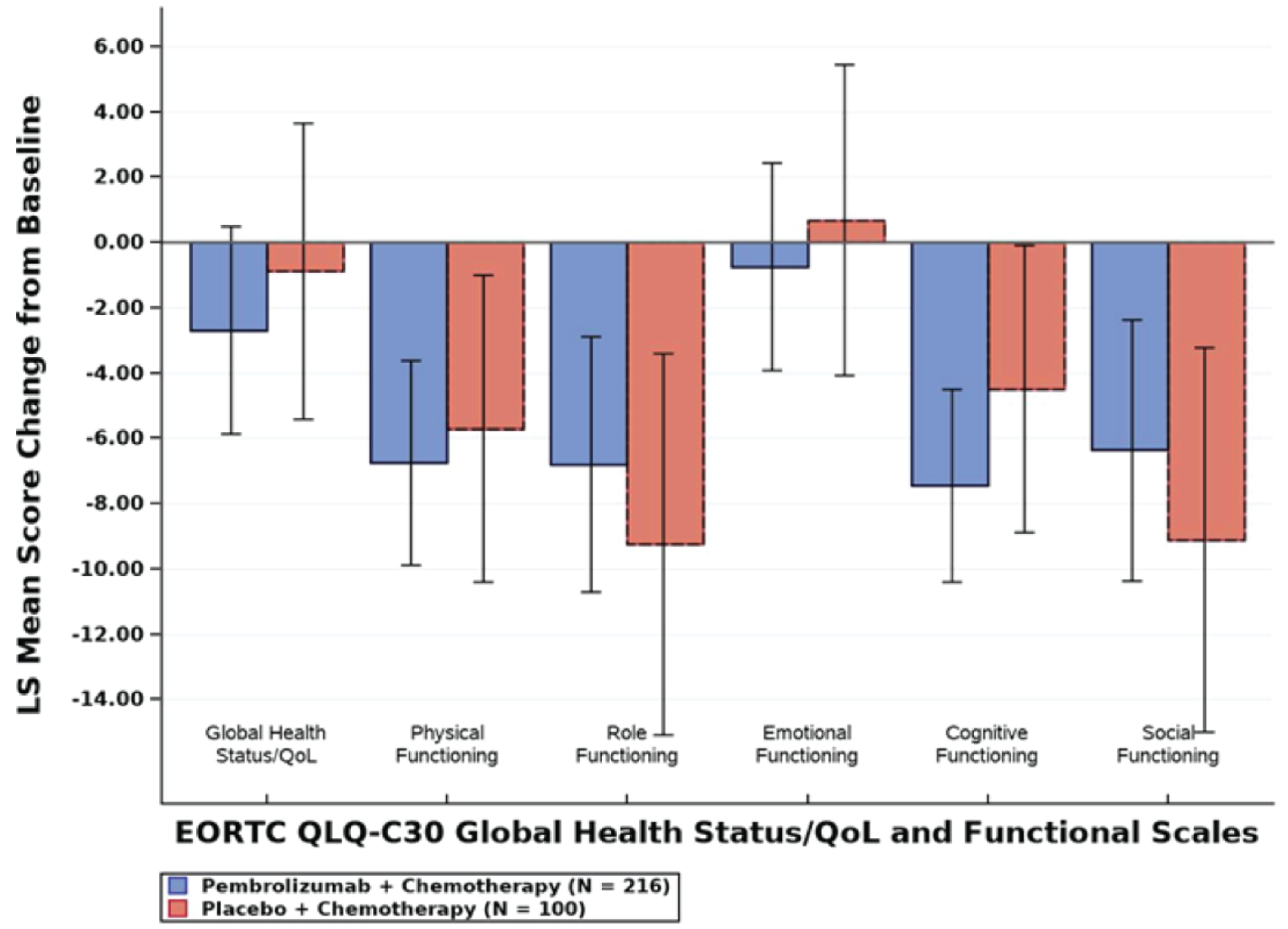
CI = confidence interval; CPS = combined positive score; EORTC QLQ-C30 = European Organisation for Research and Treatment of Cancer Quality of Life Questionnaire Core 30; QoL = quality of life; PD-L1 = programmed cell death 1 ligand 1.
Notes: For global health status and QoL scores and all functional scales, a higher score denotes better health-related QoL or function. For symptoms scales, a higher score denotes worse symptoms. Data cut-off date: June 15, 2021.
Source: Clinical Study Report.15
Figure 6: Change From Baseline for EORTC QLQ-C30 Symptom Scales and Items at Week 15 (LS Mean Change and 95% CI) in Patients With PD-L1 CPS ≥ 10 — Final Analysis Population
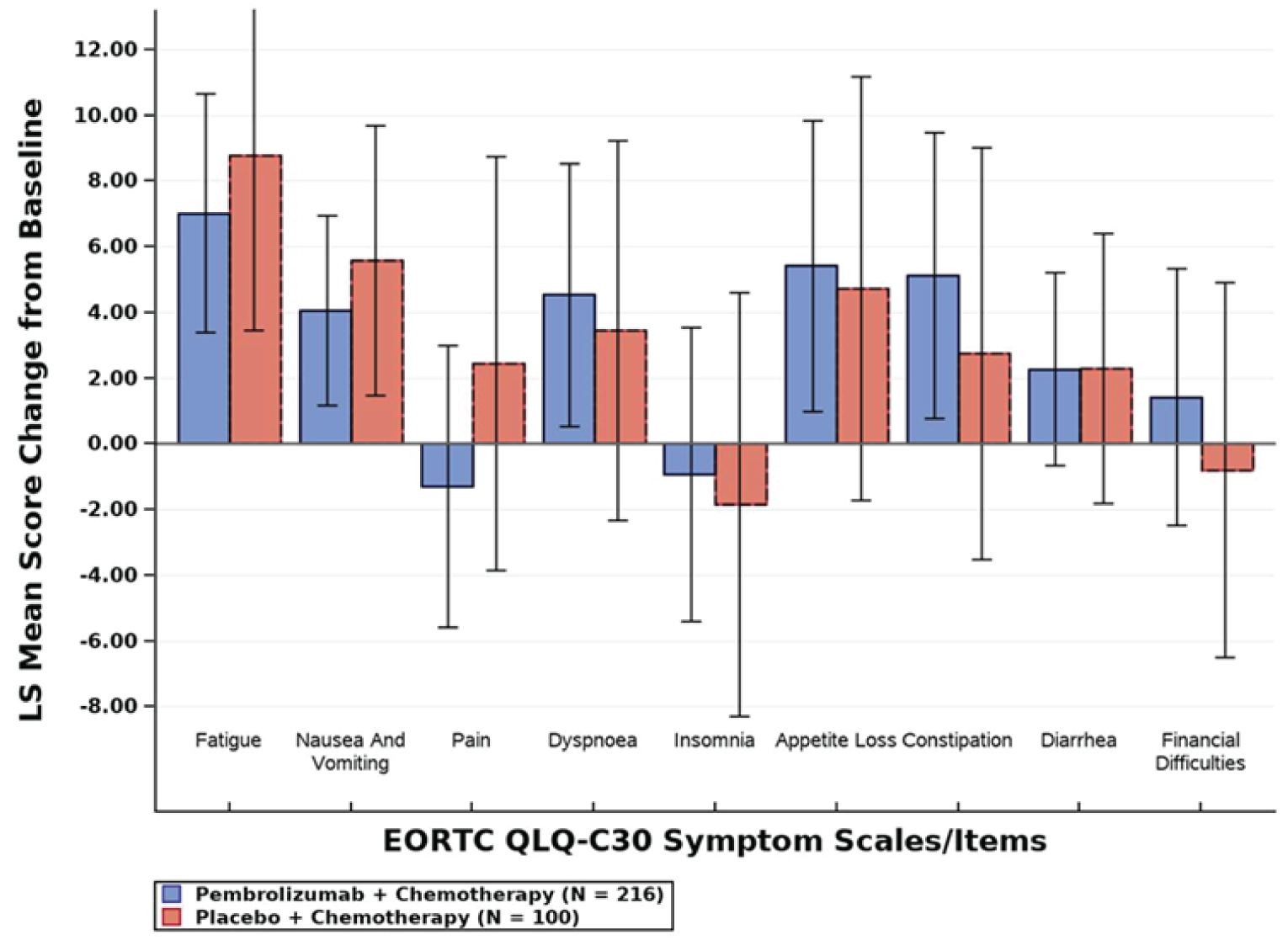
CI = confidence interval; CPS = combined positive score; EORTC QLQ-C30 = European Organisation for Research and Treatment of Cancer Quality of Life Questionnaire Core 30; LS = least squares; PD-L1 = programmed cell death 1 ligand 1; QoL = quality of life.
Notes: For global health status and QoL and all functional scales, a higher score denotes better health-related QoL or function. For symptoms scales, a higher score denotes worse symptoms. Data cut-off date: June 15, 2021.
Source: Clinical Study Report.15
Table 23: Analysis of Time to Deterioration for EORTC QLQ-C30 in Patients With PD-L1 CPS ≥ 10 Across Different Scales — Final Analysis Population
Time to deterioration analysis | Pembrolizumab plus chemotherapy (N = 217) | Placebo plus chemotherapy (N = 100) |
|---|---|---|
Emotional functioning | ||
Number of events (%) | 108 (49.8) | 38 (38.0) |
Kaplan-Meier estimates, monthsa | ||
Median (95% CI) | 9.3 (6.4 to 11.7) | 15.3 (5.6 to NR) |
First quartile to third quartile | 1.9 to 24.1 | 3.5 to NR |
vs. placebo plus chemotherapy | ||
Hazard ratio (95% CI)b | 1.28 (0.88 to 1.85) | |
P value | 0.9039c | |
Physical functioning | ||
Number of events (%) | 136 (62.7) | 47 (47.0) |
Kaplan-Meier estimates, monthsa | ||
Median (95% CI) | 5.6 (4.0 to 6.9) | 5.8 (3.7 to 14.5) |
First quartile to third quartile | 1.4 to 11.8 | 1.5 to NR |
vs. placebo plus chemotherapy | ||
Hazard ratio (95% CI)b | 1.26 (0.90 to 1.77) | |
P value | 0.9194c | |
Global health status | ||
Number of events (%) | 123 (56.7) | 49 (49.0) |
Kaplan-Meier estimates, monthsa | ||
Median (95% CI) | 5.8 (3.7, 8.1) | 5.6 (3.7, 9.7) |
First quartile to third quartile | 1.4 to 18.4 | 1.4 to 17.7 |
vs. placebo plus chemotherapy | ||
Hazard ratio (95% CI)b | 1.00 (0.72 to 1.40) | |
P value | 0.5137c | |
CI = confidence interval; CPS = combined positive score; EORTC QLQ-C30 = European Organisation for Research and Treatment of Cancer Quality of Life Questionnaire Core 30; NR = not reached; PD-L1 = programmed cell death 1 ligand 1; QoL = quality of life; SD = standard deviation.
Notes: A high score in a functional scale represents a high or healthy level of functioning; a high score in the global health status and QoL represents a high QoL, and a high score for a symptom scale or item represents a high level of symptomatology or problems. Time to deterioration (event) is defined as time to first onset of 10 points or more worsening from baseline. Data cut-off date: June 15, 2021.
aFrom product-limit (Kaplan-Meier) method for censored data.
bBased on Cox regression model with the Efron method of tie handling with treatment as a covariate stratified by chemotherapy on study (taxane vs. gemcitabine and carboplatin) and prior treatment with same class of chemotherapy in the (neo)adjuvant setting (yes vs. no).
cP value has not been adjusted for multiple testing (i.e., the type I error rate has not been controlled). One-sided P value based on log-rank test stratified by chemotherapy on study (taxane vs. gemcitabine and carboplatin) and prior treatment with same class of chemotherapy in the (neo)adjuvant setting (yes vs. no).
Source: Clinical Study Report.15
EORTC QLQ-BR23
Compliance rates at baseline were similar for the EORTC QLQ-BR23 in both the pembrolizumab and placebo arms (93.5% versus 95.0%, respectively). The change from baseline in EORTC QLQ-BR23 functional and symptom scales and items at week 15 are presented in Figure 7 and Figure 8.
After 15 weeks of follow-up, the compliance rate was 87% versus 81.4% in the pembrolizumab and placebo arms, respectively. In patients with PD-L1–positive tumours (CPS ≥ 10), the least squares mean change from baseline to week 15 in scores for both the EORTC QLQ-BR23 functional scales and items (body image, sexual functioning, sexual enjoyment, and future perspective) and the EORTC QLQ-BR23 symptom scales (systemic therapy side effects, breast symptoms, group symptoms, and upset by loss of hair) were similar between the 2 treatment groups. The analyses of domains of the EORTC QLQ-BR23 demonstrate that the addition of pembrolizumab to chemotherapy did not result in a significant decrease in HRQoL. Similar results were observed among all patients.
Figure 7: Change From Baseline for EORTC QLQ-BR23 Functional Scales and Items at Week 15 (LS Mean Change and 95% CI) in Patients With PD-L1 CPS ≥ 10 — Final Analysis Population
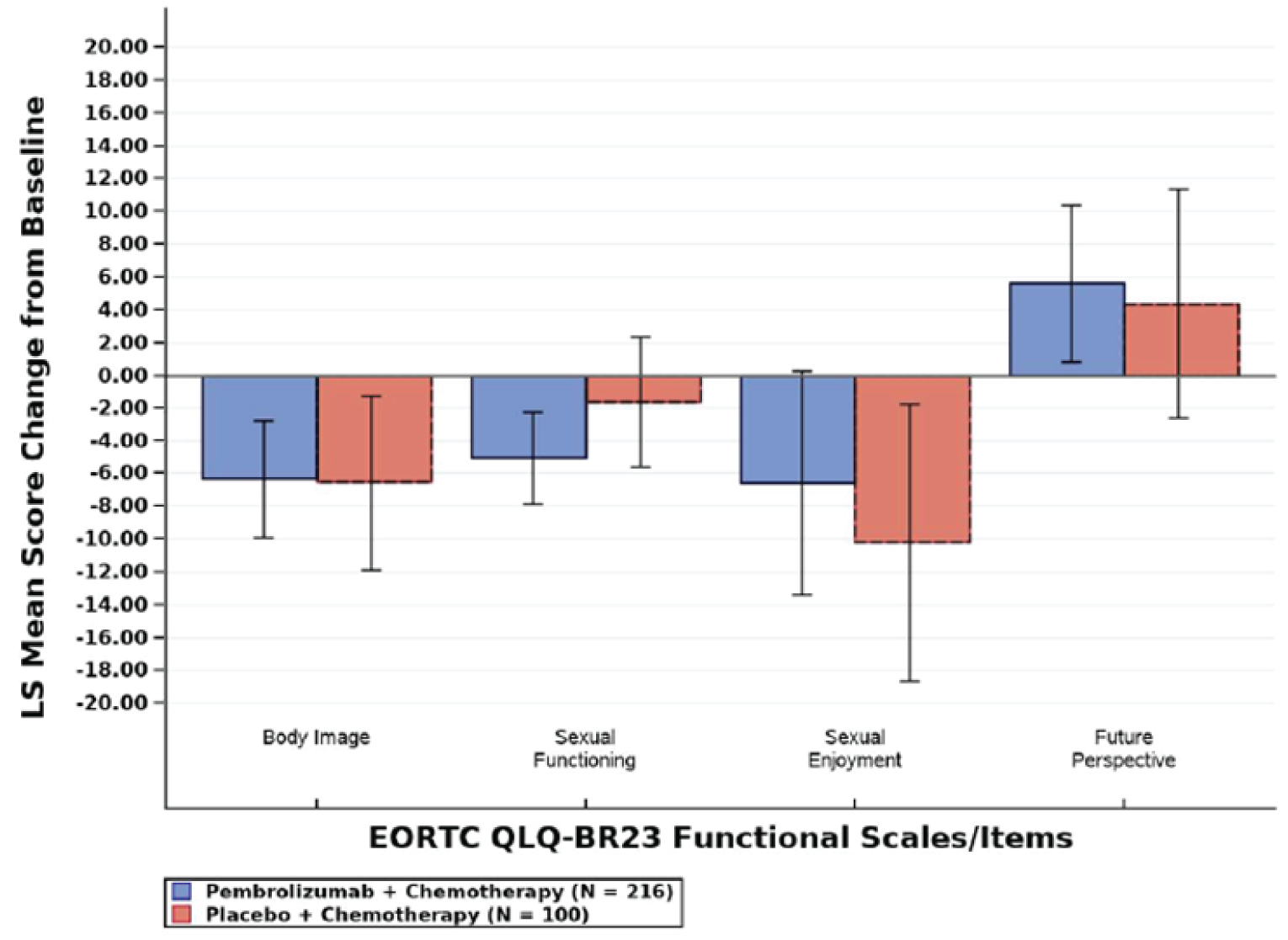
CI = confidence interval; CPS = combined positive score; EORTC QLQ-BR23 = European Organisation for Research and Treatment of Cancer Quality of Life Questionnaire – Breast Module 23; LS = least squares; PD-L1 = programmed cell death 1 ligand 1.
Notes: For functional scales and items, a higher score denotes better function. For symptom scales and items, a higher score denotes worse symptom. N is the number of patients in the analysis population in each treatment group. Data cut-off date: June 15, 2021.
Source: Clinical Study Report.15
Figure 8: Change From Baseline for EORTC QLQ-BR23 Symptom Scales and Items at Week 15 (LS Mean Change and 95% CI) in Patients With PD-L1 CPS ≥ 10 — Final Analysis Population
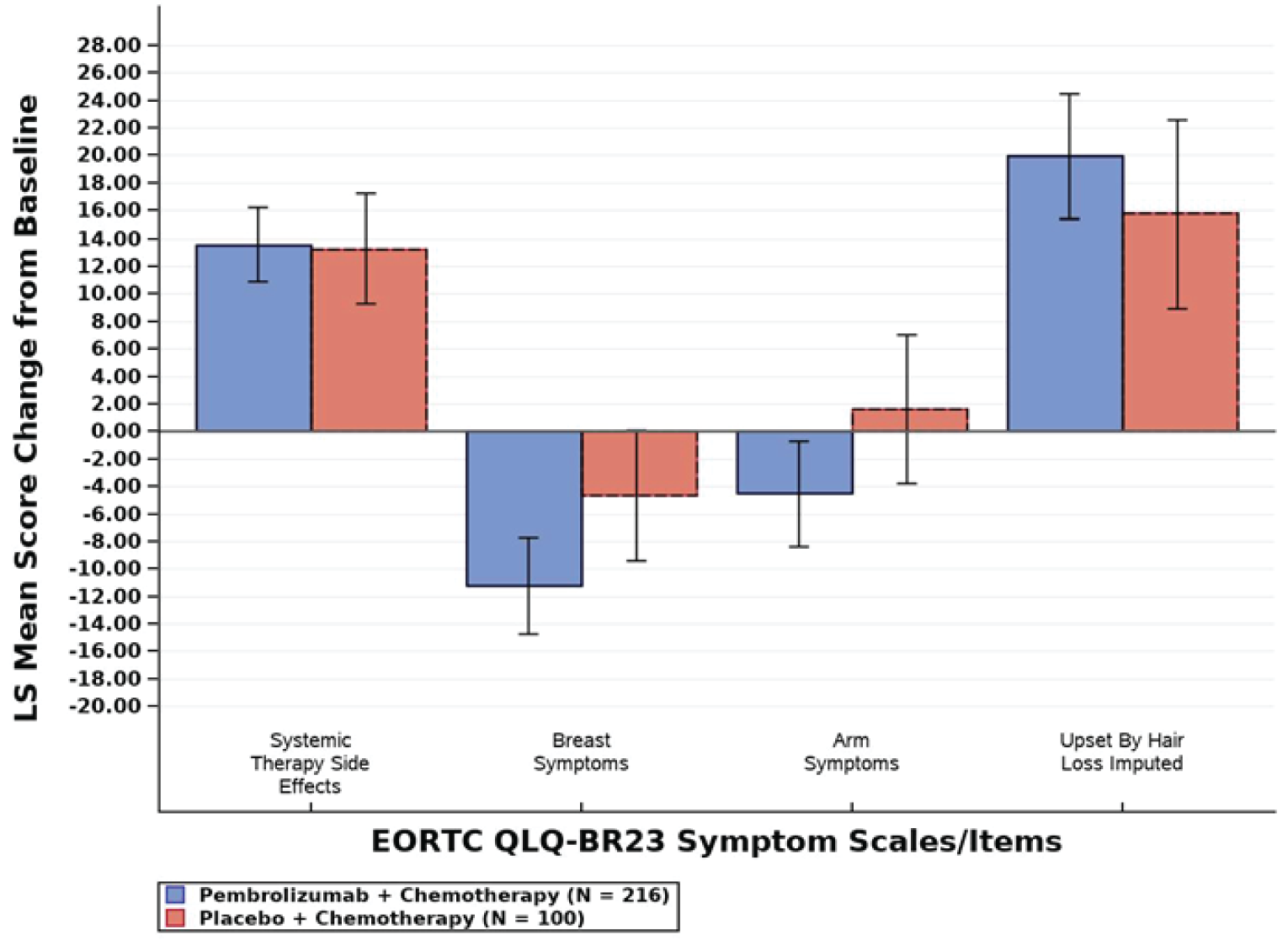
CI = confidence interval; CPS = combined positive score; EORTC QLQ-BR23 = European Organisation for Research and Treatment of Cancer Quality of Life Questionnaire – Breast Module 23; LS = least squares; PD-L1 = programmed cell death 1 ligand 1; QoL = quality of life.
Notes: For global health status and QoL score and all functional scales, a higher score denotes better health-related QoL or function. For symptoms scales, a higher score denotes worse symptoms. If a patient did not lose any hair, then upset by hair loss was imputed as lowest score (0). Data cut-off date: June 15, 2021.
Source: Clinical Study Report.15
EQ Visual Analogue Scale
At the final analysis data cut-off, compliance rates were similar at baseline for EQ VAS in both the pembrolizumab and placebo plus arms (92.8% versus 96.3% respectively). After 15 weeks of follow-up, the compliance rate was 87% versus 81.4% in the pembrolizumab and placebo arms, respectively. Over 15 weeks of follow-up, patients receiving pembrolizumab plus chemotherapy and placebo plus chemotherapy had similar small decreases (worsening) in prespecified EQ VAS scores. Similar results were observed among all patients. A summary of change from baseline in the EQ VAS at week 15 is presented in Table 24 and Figure 9.
Table 24: Summary of Change From Baseline in EQ VAS at Week 15 in Patients With PD-L1 CPS ≥ 10 — Final Analysis Population
Treatment | Pembrolizumab plus chemotherapy | Placebo plus chemotherapy |
|---|---|---|
Baseline, N | 202 | 96 |
Mean (SD) | 72.19 (20.271) | 72.56 (19.887) |
Week 15, n | 166 | 70 |
Mean (SD) | 69.16 (19.495) | 68.80 (20.879) |
Change from baseline to week 15, LS mean (95% CI)a | −5.45 (−8.68 to −2.23) | −5.63 (−10.22 to −1.04) |
Difference in LS means (95% CI) | 0.18 (−5.04 to 5.39) | |
P value | 0.9468b | |
CI = confidence interval; CPS = combined positive score; EQ VAS = EQ visual analogue scale; LS = least squares; PD-L1 = programmed cell death 1 ligand 1; SD = standard deviation.
Notes: For baseline and week 15, N is the number of patients in each treatment group with nonmissing assessments at the specific time point; for change from baseline, N is the number of patients in the analysis population in each treatment group. Data cut-off date: June 15, 2021.
aBased on constrained longitudinal data analysis model with the patient-reported outcomes scores as the response variable, and treatment by time point interaction, and stratum (defined by stratification factors of chemotherapy on study [taxane vs. gemcitabine and carboplatin] and prior treatment with same class of chemotherapy in the (neo)adjuvant setting [yes vs. no]) as covariates.
bP value has not been adjusted for multiple testing (i.e., the type I error rate has not been controlled); 2-sided P value.
Source: Clinical Study Report.15
Progression-Free Survival
A summary of PFS results at the final analysis data cut-off are presented in Table 25. At IA2 (December 11, 2019), the KEYNOTE-355 trial met the success criterion for the primary hypothesis of PFS in patients with PD-L1–positive tumours (CPS ≥ 10). The analyses performed at IA2 were the final prespecified analyses for PFS and updated data were provided at the final analysis, with nominal P values. At IA2, the median PFS was 9.7 months in the pembrolizumab plus chemotherapy and 5.6 months in the placebo plus chemotherapy group. The HR for progression or death, was 0.65, (95% CI, 0.49 to 0.86; 1-sided P = 0.0012). Based on the prespecified success criteria (alpha = 0.00411), pembrolizumab plus chemotherapy significantly improved PFS compared with placebo plus chemotherapy in patients with CPS ≥ 10.
The findings from the final analysis were consistent with the results at IA2. At the final analysis data cut-off, a total of 144 (65.5%) events had occurred in the pembrolizumab plus chemotherapy group and 81 events (78.6%) in the placebo plus chemotherapy group in patients with PD-L1–positive tumours (CPS ≥ 10). The PFS stratified HR at final analysis was 0.66 (95% CI, 0.50 to 0.88; P = 0.0018) in patients with a PD-L1 CPS of 10 or higher. Median PFS was 9.7 months (95% CI, 7.6 to 11.3) in the pembrolizumab plus chemotherapy group compared to 5.6 months (95% CI, 5.3 to 7.5) in the placebo plus chemotherapy group in patients with PD-L1–positive tumours (CPS ≥ 10).
Pembrolizumab plus chemotherapy continued to show a statistically significant improvement in PFS compared with placebo plus chemotherapy in patients with PD-L1–positive tumours (CPS ≥ 10).
Figure 9: Empirical Mean Change From Baseline in EQ VAS Across Time in Patients With PD-L1 CPS ≥ 10 — Final Analysis Population
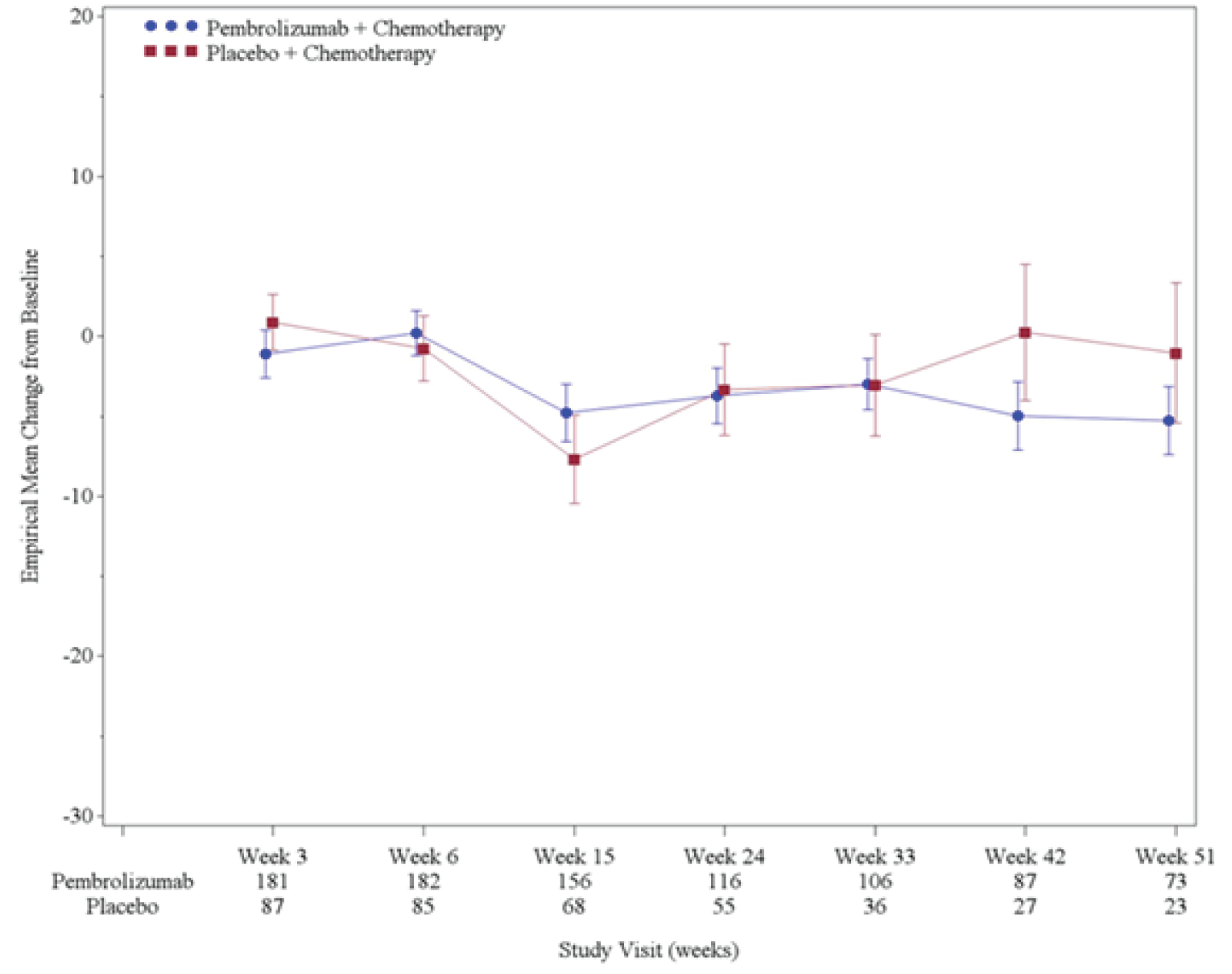
CI = confidence interval; CPS = combined positive score; EQ VAS = EQ visual analogue scale; PD-L1 = programmed cell death 1 ligand 1.
Note: Data cut-off date: June 15, 2021.
Source: Clinical Study Report.15
Table 25: PFS Based on BICR Assessment According to RECIST 1.1 in Patients With PD-L1 CPS ≥ 10 and All Patients — ITT Population
Outcomes | Patients with PD-L1 CPS ≥ 10 | All patients | ||
|---|---|---|---|---|
Pembrolizumab plus chemotherapy (N = 220) | Placebo plus chemotherapy (N = 103) | Pembrolizumab plus chemotherapy (N = 566) | Placebo plus chemotherapy (N = 281) | |
Number of events (%) | 144 (65.5) | 81 (78.6) | 406 (71.7) | 217 (77.2) |
Kaplan-Meier estimates (months)a | ||||
Median (95% CI) | 9.7 (7.6 to 11.3) | 5.6 (5.3 to 7.5) | 7.5 (6.3 to 7.7) | 5.6 (5.4 to 7.2) |
First quartile to third quartile | 3.9 to 27.8 | 3.6 to 11.8 | 3.5 to 14.5 | 3.5 to 9.9 |
Person-months | 2,714.5 | 940.6 | 5,234.4 | 2,209.2 |
Event rate per 100 person-months | 5.3 | 8.6 | 7.8 | 9.8 |
Hazard ratio (95% CI)b | 0.66 (0.50 to 0.88) | 0.82 (0.70 to 0.98) | ||
P value | 0.0018c | 0.0120c | ||
PFS rate at month 3, % (95% CI) | 81.8 (76.0 to 86.4) | 80.2 (71.0 to 86.8) | 76.9 (73.1 to 80.2) | 80.3 (75.1 to 84.5) |
PFS rate at month 6, % (95% CI) | 65.0 (58.1 to 71.2) | 46.9 (36.5 to 56.6) | 55.4 (51.0 to 59.6) | 47.4 (41.1 to 53.4) |
PFS rate at month 9, % (95% CI) | 52.5 (45.2 to 59.2) | 36.6 (26.9 to 46.4) | 42.0 (37.6 to 46.4) | 32.9 (27.0 to 38.9) |
PFS rate at month 12, % (95% CI) | 39.1 (32.0 to 46.1) | 23.0 (14.7 to 32.3) | 29.3 (25.2 to 33.5) | 20.8 (15.6 to 26.4) |
BICR = blinded independent central review; CI = confidence interval; CPS = combined positive score; ITT = intention-to-treat; PD-L1 = programmed cell death 1 ligand 1; PFS = progression-free survival; RECIST 1.1 = Response Evaluation Criteria in Solid Tumours Version 1.1.
Notes: According to the statistical analysis plan, multiplicity-adjusted analysis of PFS was conducted at interim analysis 2. Results from the final analysis were consistent with results from interim analysis 2. Data cut-off date: June 15, 2021.
aFrom product-limit (Kaplan-Meier) method for censored data.
bBased on Cox regression model with the Efron method of tie handling with treatment as a covariate stratified by chemotherapy on study (taxane vs. gemcitabine and carboplatin) and prior treatment with same class of chemotherapy in the (neo)adjuvant setting (yes vs. no).
cNominal P value (i.e., the type I error rate has not been controlled); 1-sided P value based on log-rank test stratified by chemotherapy on study (taxane vs. gemcitabine and carboplatin) and prior treatment with same class of chemotherapy in the (neo)adjuvant setting (yes vs. no).
Source: Clinical Study Report.15
Subgroup Analyses for PFS
A summary of PFS results by subgroup in the population with a PD-L1 CPS of 10 or higher is presented in Table 26. The treatment benefit in PFS for pembrolizumab plus chemotherapy compared with placebo plus chemotherapy in patients with PD-L1–positive tumours (CPS ≥ 10) was also generally consistent across the different subgroups analyzed and when applying 2 prespecified sensitivity censoring rules. Patients who received taxanes as their chemotherapy (e.g., nab-paclitaxel and paclitaxel) had lower PFS HRs (0.63 and 0.34, respectively) than did those receiving gemcitabine and carboplatin (0.88). However, given the exploratory nature, small sample sizes, and lack of statistical testing, subgroup results should be interpreted with caution.
Objective Response Rate
A summary of ORR results at the final analysis data cut-off is presented in Table 27. At the final analysis data cut-off, there were 116 objective responses (52.7%; 95% CI, 45.9 to 59.5) in the pembrolizumab group compared to 42 objective responses (40.8%; 95% CI, 31.2 to 50.9) in the placebo group in patients with a PD-L1 CPS of 10 or higher. The secondary hypotheses pertaining to ORR were tested at IA1 and not formally tested at the final analysis. The ORR was formally tested in all patients and patients with a PD-L1 CPS of 1 or higher and not in patients with a CPS of 10 or higher. The success criterion for ORR hypotheses were not met at IA1. These ORR results from the final analysis were consistent with IA1 and did not show a significant difference between the 2 treatment groups (nominal P value = 0.0213). Overall, pembrolizumab plus chemotherapy showed greater improvements in ORR (as defined by RECIST 1.1 and determined by blinded independent central review) compared with placebo plus chemotherapy in patients with PD-L1–positive tumours (CPS ≥ 10).
Subgroup Analyses of ORR
A summary of ORR results by subgroup in the PD-L1 CPS ≥ 10 population is presented in Table 28. The treatment benefit in ORR for pembrolizumab plus chemotherapy compared with placebo plus chemotherapy in patients with PD-L1–positive tumours (CPS ≥ 10) was also generally consistent across the different subgroups analyzed. Subgroup results were similar in the all patients population. Given the exploratory nature, small sample sizes, and lack of statistical testing, subgroup results should be interpreted with caution.
Figure 10: Kaplan-Meier Estimates of PFS Based on BICR Assessment According to RECIST 1.1 in Patients With PD-L1 CPS ≥ 10 — ITT Population
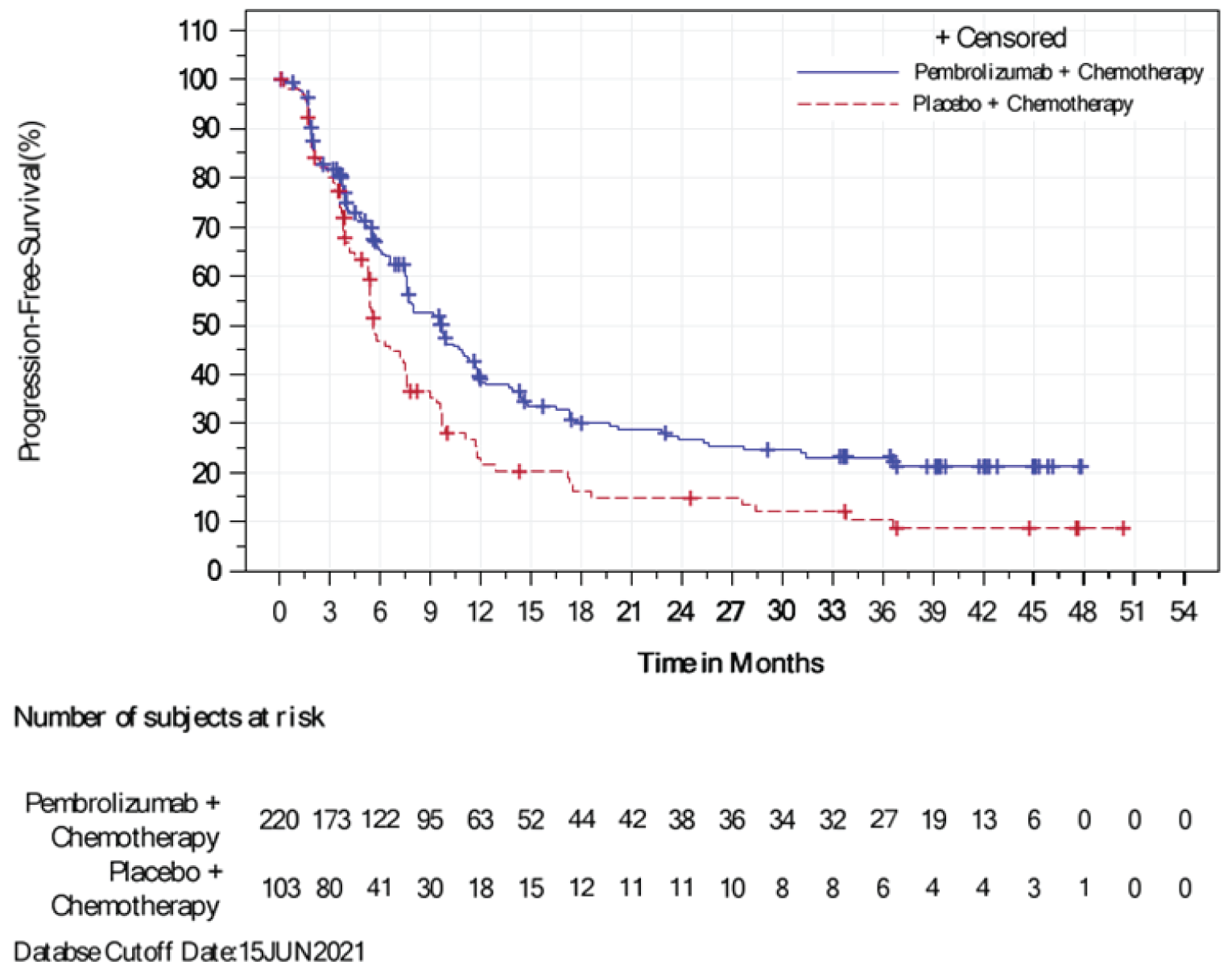
BICR = blinded independent central review; CPS = combined positive score; ITT = intention-to-treat; PD-L1 = programmed cell death 1 ligand 1; PFS = progression-free survival; RECIST 1.1 = Response Evaluation Criteria in Solid Tumours Version 1.1.
Note: Data cut-off date: June 15, 2021.
Source: Clinical Study Report.15
Table 26: PFS by Subgroups at Final Analysis in Patients With PD-L1 CPS ≥ 10 — ITT Population
Progression-free survival | Pembrolizumab plus chemotherapy (N = 220) | Placebo plus chemotherapy (N = 103) | Pembrolizumab plus chemotherapy vs. placebo plus chemotherapy | ||||
|---|---|---|---|---|---|---|---|
N | Number of events | (%) | N | Number of events | (%) | Hazard ratio (95% CI)a | |
Overall | 220 | 144 | 65.5 | 103 | 81 | 78.6 | 0.66 (0.50 to 0.88) |
Chemotherapy on study (IVRS) | |||||||
Nab-paclitaxel | 63 | 36 | 57.1 | 36 | 28 | 77.8 | 0.57 (0.35 to 0.95) |
Paclitaxel | 33 | 18 | 54.5 | 11 | 9 | 81.8 | 0.33 (0.14 to 0.75) |
Gemcitabine and carboplatin | 124 | 90 | 72.6 | 56 | 44 | 78.6 | 0.79 (0.55 to 1.13) |
Prior treatment with same class of chemotherapy in the adjuvant or neoadjuvant setting (IVRS) | |||||||
Yes | 46 | 29 | 63.0 | 19 | 14 | 73.7 | 0.60 (0.32 to 1.15) |
No | 174 | 115 | 66.1 | 84 | 67 | 79.8 | 0.67 (0.50 to 0.91) |
ECOG PS | |||||||
0 | 134 | 85 | 63.4 | 62 | 47 | 75.8 | 0.72 (0.51 to 1.03) |
1 | 86 | 59 | 68.6 | 41 | 34 | 82.9 | 0.52 (0.33 to 0.79) |
CPS = combined positive score; ECOG PS = European Cooperative Oncology Group Performance Status; IVRS = interactive voice recognition system; PD-L1 = programmed cell death 1 ligand 1.
Note: Data cut-off date: June 15, 2021.
aAnalysis (hazard ratio and 95% CI) in the overall population is based on Cox regression model with the Efron method of tie handling with treatment as a covariate stratified by chemotherapy on study (taxane vs. gemcitabine and carboplatin), tumour PD-L1 status (CPS ≥ 1 vs. CPS < 1) and prior treatment with same class of chemotherapy in the (neo)adjuvant setting (yes vs. no); analysis in the subgroups is based on the unstratified Cox model. If any level of a subgroup variable has fewer than 30 patients, subgroup analysis is not performed in that level of the subgroup variable.
Source: Clinical Study Report.15
Objective Response Rate
A summary of ORR results at the final analysis data cut-off is presented in Table 27. At the final analysis data cut-off, there were 116 objective responses (52.7%; 95% CI, 45.9 to 59.5) in the pembrolizumab group compared to 42 objective responses (40.8%; 95% CI, 31.2 to 50.9) in the placebo group in patients with a PD-L1 CPS of 10 or higher. The secondary hypotheses pertaining to ORR were tested at IA1 and not formally tested at the final analysis. The ORR was formally tested in all patients and patients with a PD-L1 CPS of 1 or higher and not in patients with a CPS of 10 or higher. The success criterion for ORR hypotheses were not met at IA1. These ORR results from the final analysis were consistent with IA1 and did not show a significant difference between the 2 treatment groups (nominal P value = 0.0213). Overall, pembrolizumab plus chemotherapy showed greater improvements in ORR (as defined by RECIST 1.1 and determined by blinded independent central review) compared with placebo plus chemotherapy in patients with PD-L1–positive tumours (CPS ≥ 10).
Subgroup Analyses of ORR
A summary of ORR results by subgroup in the PD-L1 CPS ≥ 10 population is presented in Table 28. The treatment benefit in ORR for pembrolizumab plus chemotherapy compared with placebo plus chemotherapy in patients with PD-L1–positive tumours (CPS ≥ 10) was also generally consistent across the different subgroups analyzed. Subgroup results were similar in the all patients population. Given the exploratory nature, small sample sizes, and lack of statistical testing, subgroup results should be interpreted with caution.
Duration of Response
A summary of DOR results at the final analysis data cut-off is presented in Table 29. The median DOR was greater in the pembrolizumab plus chemotherapy group at 12.8 months compared to the placebo plus chemotherapy group at 7.3 months in patients with PD-L1–positive tumours (CPS ≥ 10). The median time to response was 1.9 months in both groups. DOR results from the final analysis were consistent with the previously reported IA2 results and show a sustained DOR benefit in the pembrolizumab plus chemotherapy group over a longer follow-up (Figure 11). The proportions of patients with an extended response at 6 months or later by Kaplan-Meier estimation were 87.1% in the pembrolizumab plus chemotherapy group and 55.5% in the placebo plus chemotherapy group. At 12 months or later the ongoing response at the data cut-off was again higher for the pembrolizumab plus chemotherapy group (55.5%) compared with the placebo plus chemotherapy group (37.9%) by Kaplan-Meier estimation.
Table 27: Analysis of ORR Based on BICR Assessment According to RECIST 1.1 in Patients With PD-L1 CPS ≥ 10 and All Patients — ITT Population
Treatment | Patients with PD-L1 CPS ≥ 10 | All patients | ||
|---|---|---|---|---|
Pembrolizumab plus chemotherapy (N = 220) | Placebo plus chemotherapy (N = 103) | Pembrolizumab plus chemotherapy (N = 566) | Placebo plus chemotherapy (N = 281) | |
Number of objective responses | 116 | 42 | 231 | 104 |
ORR, % (95% CI) | 52.7 (45.9 to 59.5) | 40.8 (31.2 to 50.9) | 40.8 (36.7 to 45.0) | 37.0 (31.4 to 42.9) |
Treatment difference vs. comparator estimate (95% CI)a | 12.1 (0.4 to 23.4) | 3.8 (−3.2 to 10.6) | ||
P value | 0.0213b | 0.1413b | ||
Number of complete responses, n | 38 | 14 | 77 | 31 |
Complete responses, % (95% CI) | 17.3 (12.5 to 22.9) | 13.6 (7.6 to 21.8) | 13.6 (10.9 to 16.7) | 11.0 (7.6 to 15.3) |
Number of partial responses, n (%) | 78 | 28 | 207 | 108 |
Partial responses, % (95% CI) | 35.5 (29.1 to 42.2) | 27.2 (18.9 to 36.8) | 36.6 (32.6 to 40.7) | 38.4 (32.7 to 44.4) |
BICR = blinded independent central review; CI = confidence interval; CPS = combined positive score; ORR = overall response rate; RECIST 1.1 = Response Evaluation Criteria in Solid Tumours Version 1.1.
Note: Data cut-off date: June 15, 2021.
aBased on Miettinen and Nurminen method stratified by chemotherapy on study (taxane vs. gemcitabine and carboplatin) and prior treatment with same class of chemotherapy in the (neo)adjuvant setting (yes vs. no).
bNominal P value. One-sided P value for testing. Null hypothesis: difference in percentage of 0 vs. hypothesis 1: difference in percentage greater than 0. Confirmed responses are included.
Source: Clinical Study Report.15
Table 28: ORR by Subgroup at Final Analysis in Patients With PD-L1 CPS ≥ 10 — ITT Population
ORR | Pembrolizumab plus chemotherapy (N = 220) | Placebo plus chemotherapy (N = 103) | Differencea | ||||||
|---|---|---|---|---|---|---|---|---|---|
N | n | (%) | 95% CI | N | n | (%) | 95% CI | (%) 95% CI | |
Primary analysis (PD-L1 CPS ≥ 10) | 220 | 116 | 52.7 | (45.9 to 59.5) | 103 | 42 | 40.8 | (31.2 to 50.9) | 12.1 (0.4 to 23.4) |
Chemotherapy on study (IVRS) | |||||||||
Nab-paclitaxel | 63 | 33 | 52.4 | (39.4 to 65.1) | 36 | 13 | 36.1 | (20.8 to 53.8) | 16.3 (−4.3 to 35.0) |
Paclitaxel | 33 | 21 | 63.6 | (45.1 to 79.6) | 11 | 3 | 27.3 | (6.0 to 61.0) | 36.4 (1.9 to 61.1) |
Gemcitabine and carboplatin | 124 | 62 | 50.0 | (40.9 to 59.1) | 56 | 26 | 46.4 | (33.0 to 60.3) | 3.6 (−12.1 to 18.9) |
Prior treatment with same class of chemotherapy in the adjuvant or neoadjuvant setting (IVRS) | |||||||||
Yes | 46 | 23 | 50.0 | (34.9 to 65.1) | 19 | 4 | 21.1 | (6.1 to 45.6) | 28.9 (2.5 to 49.1) |
No | 174 | 93 | 53.4 | (45.7 to 61.0) | 84 | 38 | 45.2 | (34.3 to 56.5) | 8.2 (−4.8 to 20.9) |
ECOG PS | |||||||||
0 | 134 | 75 | 56.0 | (47.1 to 64.5) | 62 | 29 | 46.8 | (34.0 to 59.9) | 9.2 (−5.8 to 23.8) |
1 | 86 | 41 | 7.7 | (36.8 to 58.7) | 41 | 13 | 31.7 | (18.1 to 48.1) | 16.0 (−2.5 to 32.5) |
CI = confidence interval; CPS = combined positive score; ECOG PS = European Cooperative Oncology Group Performance Status; IVRS = interactive voice recognition system; ORR = objective response rate; PD-L1 = programmed cell death 1 ligand 1.
Note: Data cut-off date: June 15, 2021.
aAnalysis (ORR difference and 95% CI) in the overall population is based on the Miettinen and Nurminen method stratified by chemotherapy on study (taxane vs. gemcitabine and carboplatin), tumour PD-L1 status (CPS ≥ 1 vs. CPS < 1) and prior treatment with same class of chemotherapy in the (neo)adjuvant setting (yes vs. no); analysis in the subgroups is based on the unstratified Miettinen and Nurminen method. If any level of a subgroup variable has fewer than 30 patients, subgroup analysis is not performed in that level of the subgroup variable.
Source: Clinical Study Report.15
Table 29: Summary of Time to Response and DOR Based on BICR Assessment (RECIST 1.1) in Patients With CPS ≥ 10 and All Patients With Confirmed Response — ITT Population
Outcome | Patients with PD-L1 CPS ≥ 10 | All patients | ||
|---|---|---|---|---|
Pembrolizumab plus chemotherapy (N = 220) | Placebo plus chemotherapy (N = 103) | Pembrolizumab plus chemotherapy (N = 566) | Placebo plus chemotherapy (N = 281) | |
Patients with response,a n (%) | 116 | 42 | 231 | 104 |
Time to response (months) | ||||
Median (range) | 1.9 (1.2 to 11.7) | 1.9 (1.7 to 28.4) | 1.9 (1.2 to 11.7) | 2.0 (1.6 to 42.1) |
Response duration (months) | ||||
Median (range) | 12.8 (1.6+ to 45.9+) | 7.3 (1.5 to 46.6+) | 10.1 (1.0+ to 45.9+) | 6.5 (1.5 to 46.6+) |
Number (%)b of patients with extended response duration | ||||
≥ 6 months | 82 (81.7) | 23 (59.5) | 152(76.9) | 50 (56.8) |
≥ 12 months | 49 (55.5) | 14 (37.9) | 81 (46.1) | 26 (33.3) |
BICR = blinded independent central review; CPS = combined positive score; DOR = duration of response; PD-L1 = programmed cell death 1 ligand 1; RECIST 1.1 = Response Evaluation Criteria in Solid Tumours Version 1.1.
Notes: “+” indicates there is no progressive disease by the time of last disease assessment. Data cut-off date: June 15, 2021.
aIncludes patients with confirmed complete response or partial response.
bFrom product-limit (Kaplan-Meier) method for censored data.
Source: Clinical Study Report.1.5
Figure 11: Kaplan-Meier Estimates of DOR in Patients With Confirmed Response based on BICR Assessment According to RECIST 1.1 in Patients With PD-L1 CPS ≥ 10 — ITT Population
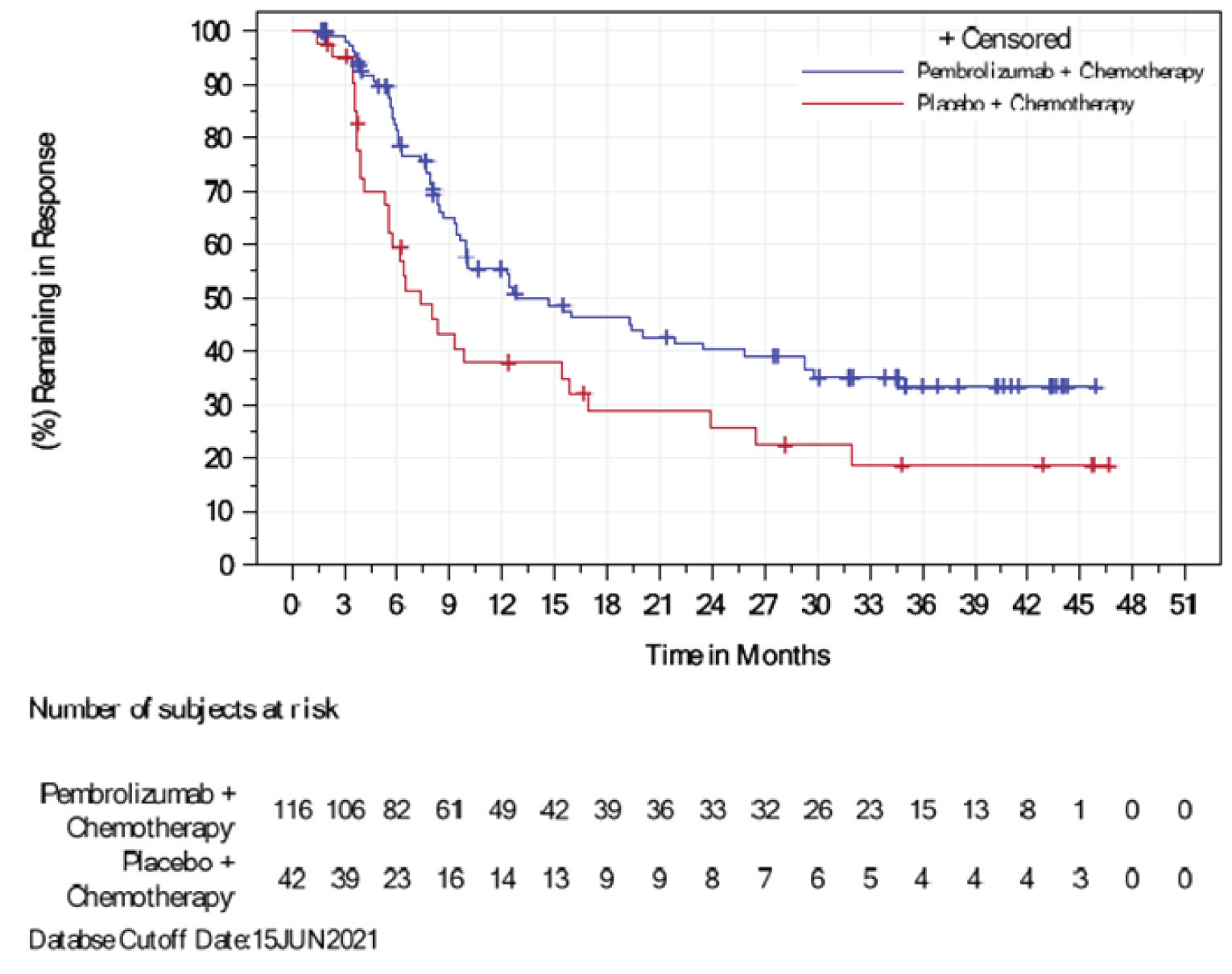
BICR = blinded independent central review; CPS = combined positive score; DOR = duration of response; ITT = intention-to-treat; PD-L1 = programmed cell death 1 ligand 1; PFS = progression-free survival; RECIST 1.1 = Response Evaluation Criteria in Solid Tumours Version 1.1.
Note: Data cut-off date: June 15, 2021.
Source: Clinical Study Report.15
Harms
Only those harms identified in the CADTH review protocol are reported in this section and in Table 30.
Adverse Events
Overall, 98.6% of patients enrolled in the pembrolizumab plus chemotherapy group and 98.2% in the placebo plus chemotherapy reported at least 1 AE by the final analysis data cut-off. Table 30 presents an overview of AEs in the pembrolizumab plus chemotherapy group and the placebo plus chemotherapy and placebo group. Overall, incidences of common AEs were similar between the 2 treatment groups. The most frequently reported AEs (occurring in > 30% of patients) receiving treatment in the pembrolizumab plus chemotherapy group and the placebo plus chemotherapy were anemia, nausea, neutropenia, alopecia, and fatigue. The incidence of hypothyroidism was greater in the pembrolizumab plus chemotherapy group (15.8%) compared to the placebo plus chemotherapy group (3.2%).
Serious Adverse Events
By the final analysis data cut-off, the incidence of SAEs was 30.1% of patients in the pembrolizumab plus chemotherapy group and 23.8% in the placebo plus chemotherapy group. The most common SAEs (approximately 2.0% of patients) in the pembrolizumab and placebo group were anemia (2.0%), pneumonia (2.0%), thrombocytopenia (2.0%), and vomiting (1.8%).
Table 30: Summary of Adverse Events — All Patients as Treated Population
Category | Pembrolizumab plus chemotherapy (N = 562) | Placebo plus chemotherapy (N = 281) |
|---|---|---|
Patients with > 1 adverse event | ||
1 or more adverse events, n (%)a | 554 (98.6) | 276 (98.2) |
Anemia | 300 (53.4) | 143 (50.9) |
Nausea | 251 (44.7) | 132 (47.0) |
Neutropenia | 233 (41.5) | 109 (38.8) |
Alopecia | 190 (33.8) | 97 (34.5) |
Fatigue | 180 (32.0) | 97 (34.5) |
Diarrhea | 157 (27.9) | 66 (23.5) |
Constipation | 155 (27.6) | 77 (27.4) |
Vomiting | 145 (25.8) | 63 (22.4) |
Increased alanine transaminase | 142 (25.3) | 55 (19.6) |
Increased aspartate transaminase | 134 (23.8) | 47 (16.7) |
Decrease neutrophil count | 128 (22.8) | 75 (26.7) |
Arthralgia | 121 (21.5) | 50 (17.8) |
Decreased appetite | 120 (21.4) | 40 (14.2) |
Cough | 117 (20.8) | 49 (17.4) |
Thrombocytopenia | 116 (20.6) | 57 (20.3) |
Leukopenia | 114 (20.3) | 50 (17.8) |
Headache | 112 (19.9) | 67 (23.8) |
Rash | 110 (19.6) | 34 (12.1) |
Asthenia | 107 (19.0) | 48 (17.1) |
Decreased white blood cell count | 106 (18.9) | 54 (19.2) |
Pyrexia | 104 (18.5) | 56 (19.9) |
Decreased platelet count | 90 (16.0) | 44 (15.7) |
Hypothyroidism | 89 (15.8) | 9 (3.2) |
Pruritus | 85 (15.1) | 32 (11.4) |
Back pain | 73 (13.0) | 42 (14.9) |
Dyspnea | 69 (12.3) | 38 (13.5) |
Peripheral edema | 66 (11.7) | 29 (10.3) |
Peripheral neuropathy | 62 (11.0) | 35 (12.5) |
Upper respiratory tract infection | 59 (10.5) | 25 (8.9) |
Myalgia | 58 (10.3) | 34 (12.1) |
Pain in extremity | 57 (10.1) | 4 1 (14.6) |
Patients with ≥ 1 SAE | ||
N %b | 169 (30.1) | 67 (23.8) |
Anemia | 11 (2.0) | 6 (2.1) |
Pneumonia | 11 (2.0) | 7 (2.5) |
Thrombocytopenia | 11 (2.0) | 4 (1.4) |
Vomiting | 10 (1.8) | 6 (2.1) |
Febrile neutropenia | 7 (1.2) | 3 (1.1) |
Pulmonary embolism | 7 (1.2) | 3 (1.1) |
Pyrexia | 7 (1.2) | 4 (1.4) |
Pneumonitis | 6 (1.1) | 0 |
Sepsis | 6 (1.1) | 3 (1.1) |
Neutropenia | 5 (0.9) | 4 (1.4) |
Pleural effusion | 5 (0.9) | 3 (1.1) |
Nausea | 3 (0.5) | 3 (1.1) |
Patients who stopped treatment due to adverse events | ||
N (%) | 60 (10.7) | 15 (5.3) |
Increased alanine transaminase | 12 (2.1) | 4 (1.4) |
Increased aspartate transaminase | 9 (1.6) | 2 (0.7) |
Pneumonitis | 7 (1.2) | 0 |
Abnormal hepatic function | 3 (0.5) | 0 |
Decreased neutrophil count | 2 (0.4) | 0 |
Pulmonary embolism | 2 (0.4) | 0 |
Acute myocardial infarction | 1 (0.2) | 0 |
Adrenal insufficiency | 1 (0.2) | 0 |
Anemia | 1 (0.2) | 0 |
Arthralgia | 1 (0.2) | 0 |
Autoimmune hepatitis | 1 (0.2) | 0 |
Increased bilirubin conjugated | 1 (0.2) | 0 |
Increased blood alkaline phosphatase | 1 (0.2) | 0 |
Increase blood bilirubin | 1 (0.2) | 0 |
Increased blood creatinine | 1 (0.2) | 2 (0.7) |
Increased blood lactate dehydrogenase | 1 (0.2) | 0 |
Cheilitis | 1 (0.2) | 0 |
Colitis | 1 (0.2) | 0 |
Cystoid macular edema | 1 (0.2) | 0 |
Death | 1 (0.2) | 0 |
Device related sepsis | 1 (0.2) | 0 |
Guillain-Barré syndrome | 1 (0.2) | 0 |
Hepatic encephalopathy | 1 (0.2) | 0 |
Hepatitis | 1 (0.2) | 0 |
Hypertension | 1 (0.2) | 0 |
Hypertensive emergency | 1 (0.2) | 0 |
Leukopenia | 1 (0.2) | 0 |
Liver disorder | 1 (0.2) | 0 |
Abnormal liver function test | 1 (0.2) | 0 |
Malaise | 1 (0.2) | 0 |
Multiple organ dysfunction syndrome | 1 (0.2) | 0 |
Myalgia | 1 (0.2) | 0 |
Myocarditis | 1 (0.2) | 0 |
Peripheral neuropathy | 1 (0.2) | 0 |
Palmar-plantar erythrodysesthesia syndrome | 1 (0.2) | 0 |
Pancreatitis | 1 (0.2) | 0 |
Decreased platelet count | 1 (0.2) | 0 |
Pneumonia | 1 (0.2) | 2 (0.7) |
Polyarthritis | 1 (0.2) | 0 |
Pyrexia | 1 (0.2) | 0 |
Renal failure | 1 (0.2) | 0 |
Sepsis | 1 (0.2) | 0 |
Staphylococcal infection | 1 (0.2) | 0 |
Thrombocytopenia | 1 (0.2) | 1 (0.4) |
Venous thrombosis limb | 1 (0.2) | 0 |
Cardiac failure | 0 | 1 (0.4) |
Chronic inflammatory demyelinating polyradiculoneuropathy | 0 | 1 (0.4) |
Hemorrhagic stroke | 0 | 1 (0.4) |
Respiratory failure | 0 | 1 (0.4) |
Scleroderma | 0 | 1 (0.4) |
Toxicity grade 3 to 5 adverse event | ||
N (%)b | 438 (77.9) | 207 (73.7) |
Neutropenia | 169 (30.1) | 85 (30.2) |
Anemia | 101 (18.0) | 46 (16.4) |
Decreased neutrophil count | 101 (18.0) | 57 (20.3) |
Thrombocytopenia | 63 (11.2) | 33 (11.7) |
Decreased white blood cell count | 59 (10.5) | 29 (10.3) |
Leukopenia | 57 (10.1) | 31 (11.0) |
Increased alanine transaminase | 44 (7.8) | 16 (5.7) |
Decreased platelet count | 36 (6.4) | 20 (7.1) |
Increased aspartate transaminase | 32 (5.7) | 11 (3.9) |
Fatigue | 17 (3.0) | 10 (3.6) |
Vomiting | 16 (2.8) | 9 (3.2) |
Hypertension | 13 (2.3) | 5 (1.8) |
Lymphopenia | 13 (2.3) | 3 (1.1) |
Pneumonia | 13 (2.3) | 7 (2.5) |
Asthenia | 12 (2.1) | 2 (0.7) |
Decreased lymphocyte count | 11 (2.0) | 6 (2.1) |
Nausea | 10 (1.8) | 5 (1.8) |
Diarrhea | 9 (1.6) | 5 (1.8) |
Dyspnea | 9 (1.6) | 3 (1.1) |
Febrile neutropenia | 9 (1.6) | 3 (1.1) |
Arthralgia | 8 (1.4) | 2 (0.7) |
Increased blood alkaline phosphatase | 8 (1.4) | 2 (0.7) |
Increased gamma-glutamyl transferase | 8 (1.4) | 4 (1.4) |
Hypokalemia | 8 (1.4) | 5 (1.8) |
Peripheral sensory neuropathy | 8 (1.4) | 2 (0.7) |
Pulmonary embolism | 8 (1.4) | 4 (1.4) |
Back pain | 7 (1.2) | 0 |
Hyperglycemia | 6 (1.1) | 3 (1.1) |
Hypophosphatasemia | 6 (1.1) | 2 (0.7) |
Decreased neutrophil percentage | 6 (1.1) | 1 (0.4) |
Pleural effusion | 6 (1.1) | 4 (1.4) |
Pneumonitis | 6 (1.1) | 0 |
Rash maculo-papular | 6 (1.1) | 0 |
Sepsis | 6 (1.1) | 3 (1.1) |
Alopecia | 5 (0.9) | 3 (1.1) |
Neuropathy peripheral | 5 (0.9) | 4 (1.4) |
Pyrexia | 3 (0.5) | 3 (1.1) |
Deaths due to adverse events | ||
N (%) | 17 (3.0) | 5 (1.8) |
Cardiorespiratory arrest | 2 (0.4) | 0 |
Pneumonia | 2 (0.4) | 1 (0.4) |
Septic shock | 2 (0.4) | 0 |
Acute kidney injury | 1 (0.2) | 0 |
Acute myocardial infarction | 1 (0.2) | 0 |
Assisted suicide | 1 (0.2) | 0 |
Cardiac arrest | 1 (0.2) | 0 |
Cardiopulmonary failure | 1 (0.2) | 0 |
Death | 1 (0.2) | 0 |
Hepatic encephalopathy | 1 (0.2) | 0 |
Multiple organ dysfunction syndrome | 1 (0.2) | 0 |
Pulmonary embolism | 1 (0.2) | 0 |
Sepsis | 1 (0.2) | 0 |
Hemorrhagic shock | 1 (0.2) | 0 |
Cardiac failure | 0 | 1 (0.4) |
Hemorrhagic stroke | 0 | 1 (0.4) |
Respiratory failure | 0 | 1 (0.4) |
Vascular device infection | 0 | 1 (0.4) |
Notable harms | ||
Hypothyroidism | 89 (15.8) | 9 (3.2) |
Hyperthyroidism | 24 (4.3) | 3 (1.1) |
Infusion reactions | 21 (3.7) | 14 (5.0) |
Pneumonitis | 14 (2.5) | 0 |
Colitis | 10 (1.8) | 4 (1.4) |
Nephritis | 3 (0.5) | 0 |
Type 1 diabetes mellitus | 1 (0.2) | 0 |
aFrequency greater than 10% in either treatment group.
bFrequency greater than 1% in either treatment group.
Note: Data cut-off date: June 15, 2021.
Source: Clinical Study Report.15
Grade 3 to 5 Adverse Events
By the final analysis data cut-off, AEs of grade 3 or higher occurred in 77.9% of patients in the pembrolizumab plus chemotherapy group and 73.7% in the placebo plus chemotherapy group. The most frequent grade 3 to 5 AEs (occurring in ≥ 10% of patients in either arm) reported in both arms included neutropenia, decreased neutrophil count, anemia, thrombocytopenia, decreased white blood cell count, and leukopenia.
Mortality
By the final analysis data cut-off, the overall incidences of AEs resulting in death were 3.0% in the pembrolizumab plus chemotherapy group and 1.8% in the placebo plus chemotherapy group and were similar between groups. Common causes of mortality in the treatment group were cardiorespiratory arrest (0.4%), pneumonia (0.4%), and septic shock (0.4%). Two AEs resulting in death pneumonia and acute kidney injury), were considered related to pembrolizumab plus nab-paclitaxel and pembrolizumab, respectively. No AEs resulting in death were considered related to chemotherapy. The Health Canada reviewer noted that no new safety signals were identified upon review of these fatal events.17
Discontinuations due to Adverse Events
By the final analysis data cut-off, discontinuations due to AEs were higher in the pembrolizumab plus chemotherapy group compared to placebo plus chemotherapy and placebo. The overall incidence of AEs resulting in the discontinuation of any study intervention during the combined phases was higher in the pembrolizumab plus chemotherapy group (10.7%) compared to the placebo plus chemotherapy group (5.3%). The most frequently reported AEs (incidence ≥ 1%) resulting in discontinuation in the pembrolizumab plus chemotherapy group were increased alanine transaminase (2.1%), increased aspartate transaminase (1.6%), and pneumonitis (1.2%). The most frequently reported AEs resulting in discontinuation in the placebo plus chemotherapy group were increased alanine transaminase (1.4%), increased aspartate transaminase (0.7%), increased blood creatinine (0.7%), and pneumonia (0.7%).
Notable Harms
The overall incidence of notable harms was higher in the pembrolizumab plus chemotherapy group compared with the placebo plus chemotherapy group. The most common notable harms in the pembrolizumab plus chemotherapy group were hypothyroidism (15.8%), hyperthyroidism (4.3%), infusion reactions (3.7%), and pneumonitis (2.5%). The most common notable harms in the placebo plus chemotherapy were infusion reactions (5%), hypothyroidism (3.2%), colitis (1.4%), and hyperthyroidism (1.1%). The Health Canada Reviewer Report noted that the types of AEs of special interest were consistent overall with the known safety profile of pembrolizumab monotherapy.17
Critical Appraisal
Internal Validity
The KEYNOTE-355 trial is a randomized, double-blind, placebo-controlled, phase III study. Patients and investigators were blinded to the treatment regimens. Baseline characteristics were well balanced across treatment groups. The study was designed to perform a stratification randomization on a PD-L1 CPS of 1 or higher or less than 1 but not on 10 or higher or less than 10. Given that the primary focus of this reimbursement review was the subpopulation of patients with a PD-L1 CPS of 10 or higher, a potential concern was the lack of stratification randomization on patients with a PD-L1 CPS of 10 or higher. This may have contributed to imbalances between the treatment arms, particularly potential unknown confounding covariates. For example, in the subpopulation with a PD-L1 CPS of 10 or higher, a HER2 status of 2+ (a potential prognostic factor for breast cancer) was reported in 30.5% versus 22.3% of patients in the pembrolizumab and placebo groups, respectively. Similarly, there were imbalances between the 2 treatment groups in the number of patients whose disease status was metastatic de novo or metastatic recurrent, the disease-free interval < 12 months, the use of subtype of chemotherapies on study, as well as prior same class chemotherapies (Table 7). The Health Canada Reviewer Report raised the same concern, which the sponsor addressed by noting that an evaluation and sensitivity analysis of the potential for imbalance was conducted in the patient population with a CPS of 10 or higher. It was concluded that the impact of not having a CPS of 10 or higher as a stratification factor would be minimal, and the imbalances in baseline factors were limited and did not change the conclusion of the primary analysis. The Health Canada Reviewer Report acknowledged that the sponsor’s responses to this concern were deemed detailed and adequate.17 HRQoL analyses were based on the full analysis set. Overall, there were no significant differences in all domains and symptom subcategories in the EORTC QLQ-C30, EORTC QLQ-BR23, and EQ VAS scores. The surveys were conducted at week 15; however, this time point may not be able to capture an accurate picture of patients’ experiences with the pembrolizumab plus chemotherapy combination for a prolonged period of time. The assessment time point at week 15 was selected to ensure at least 60% completion and 80% compliance with patient-reported outcome assessments to ensure validity of the longitudinal model of change in patient-reported outcome scores over time. Analyses performed on the patient-reported outcomes were noninferential.
The study-designed interim analyses were performed by an independent data monitoring committee. The consistency of interim results with final analysis would help strengthen the robustness of the findings at final analyses. For example, PFS assessed at the final analysis was not formally tested based on the statistical hierarchy, yet the results were consistent with the results at IA2, in which the statistical significance testing was conducted. The type I error rate was adjusted during the analyses using the overall familywise error rate. Sensitivity analyses and adjustments for covariates were conducted for OS and PFS and the findings were consistent with the primary analysis of the ITT population. In particular, the final analysis results on the coprimary end points were consistent across interim analyses.
Protocol deviations and premature unblinding were reported for patients receiving either 1 of the study treatments in the KEYNOTE-355 study. Overall, 150 patients of patients (17.7%) experienced premature unblinding. Fifteen of these unblindings were inadvertent. The proportion of patients with significant protocol deviations was slightly higher in the pembrolizumab plus chemotherapy group (3.0%) compared to placebo plus chemotherapy and placebo (1.8%). The most common reasons were violation of inclusion criteria and patients dispensed study interventions other than what was assigned by the trial schedule. With regard to protocol violations, a high percentage of unblinding during the course of the trial could have biased the subjective outcomes, such as HRQoL.
More patients in the placebo plus chemotherapy group received subsequent immunotherapy and antineoplastic therapies than did patients in the pembrolizumab plus chemotherapy group in the subpopulation with a PD-L1 CPS of 10 or higher (11.7% versus 3.7% in placebo versus pembrolizumab, respectively) and these were similar in all patients. The higher percentage of subsequent therapies received in the placebo group after disease progression may have biased the OS estimates against pembrolizumab. A higher proportion of patients discontinued the treatment in the placebo group than in the pembrolizumab group due to progressive disease (68.9 versus 58.0%) in patients with a PD-L1 CPS of 10 or higher and in all patients. Informative censoring in PFS could arise when patients were censored for initiation of an effective anticancer treatment before a protocol-defined progression, and these patients are at a different risk for treatment failure than those who continue on therapy. In both arms, the main reason for patient dropout from the study was death. However, more patients in the pembrolizumab group discontinued the study with status unknown at the final analysis cut-off date (27.3 versus 18.4%) compared to the placebo group in patients with a CPS of 10 or higher. This informative censoring may affect the accurate estimation of treatment effect.
External Validity
The KEYNOTE-355 trial was conducted at 220 sites in 29 countries, including 5 sites in Canada (N = 34). The inclusion and exclusion criteria of the KEYNOTE-355 trial were considered appropriate by the clinical experts. The clinical experts considered the baseline characteristics generalizable to patients in the Canadian setting. The clinical experts consulted by CADTH noted that the choice of chemotherapies used in the KEYNOTE-355 study was appropriate and reflective of treatments administered in this setting.
The dosage of pembrolizumab aligns with the Health Canada Notice of Compliance indication. Dose modifications were allowed for all study drugs used in the KEYNOTE-355 trial except pembrolizumab (it was recommended that pembrolizumab be withheld in case of drug-related toxicities) as outlined in the protocol. The clinical experts consulted by CADTH considered the chemotherapy regimens administered during the trial appropriate and reflective of Canadian practice. The clinical experts also highlighted that drug discontinuations are expected in practice, although clinicians will generally encourage patients to complete all cycles of chemotherapy by implementing dose reductions in situations of toxicity.
The clinical experts consulted by CADTH considered the duration of follow-up implemented in the KEYNOTE-355 study appropriate. The clinical experts noted that the concomitant medications allowed in the KEYNOTE-355 study were also commonly used in Canadian practice and were considered appropriate. The experts did not identify any major concerns and discrepancies between the trial and real-world settings in terms of concomitant medication use and duration of follow-up.
Indirect Evidence
Objectives and Methods for the Summary of Indirect Evidence
The sponsor conducted an ITC to estimate the efficacy of the combination of pembrolizumab and chemotherapy relative to alternative treatments for TNBC patients in the first-line metastatic setting. CADTH also conducted a literature search to identify other potentially relevant ITCs in adults with TNBC. A focused literature search for ITCs dealing with breast neoplasms was run in MEDLINE All (1946–) on June 28, 2022. No search limits were applied. Titles, abstracts, and full-text articles were screened for inclusion by 1 reviewer based on the population, intervention, comparator, and outcome criteria outlined in the CADTH systematic review protocol (Table 5). As the systematic review did not identify any relevant ITC in the literature, this section appraises the sponsor-submitted ITC.
One sponsor-submitted ITC was summarized and critically appraised. The sponsor-submitted ITC was used to inform the pharmacoeconomic model.
Description of ITC
The sponsor-submitted ITC, which is a network meta-analysis (NMA), aimed to evaluate the relative efficacy and safety of the combination of pembrolizumab and chemotherapy versus other regimens for first-line treatment of locally recurrent inoperable or metastastic TNBC in adult patients. The sponsor performed a systematic review to identify relevant studies for inclusion in the ITC. Outcomes that were included in the review were efficacy, safety, and QoL measures. The population, intervention, comparators, outcomes, and design of studies included in the sponsor’s ITC are provided in detail in Table 31.
Table 31: Study Selection Criteria and Methods for ITCs
Study selection criteria | Sponsor-submitted indirect treatment comparison |
|---|---|
Population | Previously untreated locally recurrent inoperable or metastatic TNBC |
Intervention | Chemotherapy combinations:
Chemotherapy single drugs (preferred):
Chemotherapy single drugs (other):
Immunotherapy drugs:
|
Comparator | Any of the listed interventions |
Outcome | Efficacy outcomes:
Safety outcomes:
Patient-reported outcomes, including quality-of-life measures:
|
Study design | Phase II and III randomized controlled trials:
|
Publication characteristics | English language |
Exclusion criteria | Studies were excluded if they did not include at least 2 treatment groups with interventions or comparators of interest; they enrolled exclusively TNBC patients and did not report at least 1 outcome of interest; and they enrolled patients from a broader breast cancer population and did not report at least 1 outcome in a subgroup composed of > 90% TNBC patients |
Databases searched | MEDLINE, Embase, CENTRAL, clinicaltrials.gov, clinicaltrialsregister.eu, American Society of Clinical Oncology, European Society of Medical Oncology, San Antonio Breast Cancer Symposium |
Selection process | Articles screened independently by 2 researchers |
Data extraction process | Data extraction was performed by pairs of reviewers and compared for discrepancies by a third reviewer |
Quality assessment | Scottish Intercollegiate Guidelines Network for MEDLINE and Embase |
EORTC QLQ-BR23 = European Organisation for Research and Treatment of Cancer Quality of Life Questionnaires – Breast Module 23; EORTC QLQ-C30 = European Organisation for Research and Treatment of Cancer Quality of Life Questionnaire Core 30; FACT-BSI = Functional Assessment of Cancer Therapy – Breast Symptom Index; mTNBC = metastatic = triple-negative breast cancer; TNBC = triple-negative breast cancer.
Source: Sponsor-submitted indirect treatment comparison.32
Methods of Sponsor-Submitted ITC
Study Selection Methods
As part of the sponsor’s ITC, a systematic literature review was conducted to identify the available evidence in terms of clinical efficacy and safety of pembrolizumab plus chemotherapy versus competing interventions for first-line treatment of locally recurrent inoperable or metastatic TNBC in adults. In the absence of direct head-to-head comparisons of treatments of interest, an NMA of relevant interventions was performed. Although direct evidence is available on the efficacy and safety of pembrolizumab plus chemotherapy versus nab-paclitaxel, paclitaxel, and gemcitabine in combination with carboplatin, comparative efficacy studies versus other chemotherapies of interest were not identified in the systematic literature search. As such, the systematic review and NMA were conducted in adherence to the principles of the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA).
Two reviewers, operating independently, reviewed all abstracts and proceedings identified by the search according to the selection criteria, except outcome criteria. The outcome criteria were applied only during the screening of full-text publications. Studies deemed eligible during abstract screening were then screened at a full-text stage by the same 2 reviewers. The full-text studies identified at this stage were included for subsequent data extraction. After reconciliation between the 2 reviewers, a third reviewer was involved to reach a consensus for any remaining discrepancies.
The search strategy was based on the criteria in Table 31. The study population was defined as adult patients with locally recurrent inoperable or metastatic TNBC.
Published phase II and III randomized controlled trials (RCTs) of any size and duration and with any blinding status were eligible for inclusion in the analysis. Studies must include at least 2 treatment groups with interventions or comparators of interest. Due to an expected lack of studies conducted exclusively in TNBC patients, studies were eligible if they enrolled exclusively TNBC patients and reported at least 1 outcome of interest or if they enrolled patients from a broader breast cancer population and reported at least 1 outcome in a subgroup composed of at least 90% TNBC patients.
MEDLINE, Embase, and the Cochrane Central Register of Controlled Trials were searched for relevant studies. The searches were executed on July 27, 2021. The study design criteria recommended by the Scottish Intercollegiate Guidelines Network for MEDLINE and Embase were used to identify clinical trials. The US National Institute of Health Clinical Trials Registry (clinicaltrials.gov) and the European Union Clinical Trial Registry (clinicaltrialsregister.eu) were also searched to identify completed RCTs that met the criteria with results available that were not yet published. Manual searches of the most recent proceedings of the several conferences were conducted to identify studies that have not yet been published including American Society of Clinical Oncology (2020 to 2021), European Society of Medical Oncology (2020), and San Antonio Breast Cancer Symposium (2020).
Study characteristics that were extracted from the identified studies included study name, year, authors, design, inclusion criteria, exclusion criteria, year of initiation and close, location, follow-up period, sample size, outcome definitions, and quality assessment. Intervention characteristics were extracted included treatment regimen, treatment dose, method of administration, frequency of administration, duration of treatment, and concomitant and/or background therapies. Patient characteristics that were extracted included sample size at baseline, age, gender, race and ethnicity, performance status (Eastern Cooperative Oncology Group or Karnofsky), disease stage, histology, comorbidities, and lines of prior treatment. Outcomes that were extracted included DOR, ORR, OS, PFS, drug-related AEs, grade 3 to 5 AEs (all, drug-related), discontinuations due to AE, SAEs, patient-reported outcomes (e.g., EQ-5D, EORTC QLQ-C30, immune-related AEs [for immunotherapy only]), and immune-related grade 3 to 5 AEs (for immunotherapy only).
ITC Analysis Methods
A summary of the ITC’s analysis methods is included in Table 32. The authors of the submitted ITC used a Bayesian NMA approach. Both fixed-effect and random-effect models were considered. However, because only 1 trial connected each treatment in the evidence network, between-study heterogeneity could not be estimated. NMAs were conducted with a fixed-effects assumption.
To assess the appropriateness of conducting an NMA, a feasibility assessment was conducted and included: determination of whether the trial evidence for the interventions of interest from 1 evidence network for each population and outcome of interest; and assessment of the distribution of treatment, outcomes, study, and patient characteristics that may affect treatment effects across direct comparisons of the evidence networks.
The NMA of reported HRs in terms of PFS and OS under the assumption of proportional hazards between treatments was conducted using a regression model with a contrast-based normal likelihood for the log HR (and corresponding standard error) of each study (or comparison) in the network. Normal noninformative prior distributions for the parameters were estimated with a mean of 0 and a variance of 10,000.
The Cochrane Collaboration risk-of-bias tool was used to evaluate the risk of bias in included RCTs.
The results of the NMA for PFS and OS were presented with estimates for treatment effects of each intervention relative to the reference pembrolizumab plus chemotherapy treatment combination. The posterior distributions of relative treatment effects were summarized by the median and 95% CrIs. The results of the NMA were presented in the form of cross-tables with relative treatment effect estimates (HRs) between all interventions of interest along with 95% CrIs for all outcomes. The methods were consistent with guidelines recommended by the National Institute for Health and Care Excellence Decision Support Unit.
Table 32: ITC Analysis Methods
Analysis method | ITC1 |
|---|---|
ITC methods | Fixed-effects network meta-analysis under a Bayesian framework |
Priors | Normal noninformative prior distributions with a mean of 0 and a variance of 10,000 |
Assessment of model fit | Deviance information criterion |
Assessment of consistency | Not reported |
Assessment of convergence | Not reported |
Outcomes | PFS, OS, ORR, HRQoL, AEs, discontinuation due to AEs |
Follow-up time points | Not reported |
Construction of nodes | Not reported |
Sensitivity analyses | Not reported |
Subgroup analysis | Not conducted |
Methods for pairwise meta-analysis | Not conducted |
AE = adverse event; HRQoL = health-related quality of life; ITC = indirect treatment comparison; ORR = objective response rate; OS = overall survival; PFS = progression-free survival.
Source: Sponsor-submitted ITC.32
Results of Sponsor-Submitted ITC
Summary of Included Studies
A systematic literature review was conducted and 2,057 citations were identified. After removing 532 duplicates, 1,525 citations were screened resulting in 142 citations eligible for full-text review. Of these, 19 citations pertaining to 8 unique trials conducted in patients with locally recurrent inoperable or metastatic TNBC patients receiving first-line treatment met the inclusion criteria for the NMA. The sponsor’s assumption that paclitaxel and nab-paclitaxel have similar efficacy aligns with the option of the clinical experts consulted by CADTH for this review. Consequently, paclitaxel and nab-paclitaxel are treated as the same node in the networks and as a result, only 633-38 out of 839,40 unique trials were used to inform the NMA. A summary of the studies included in the NMA is presented in Figure 12.
Study Characteristics
Of the 19 citations pertaining to 8 unique trials that were identified, 4 were phase III RCTs and 1 was a phase II and III RCT. Three trials were double-blind, and the remaining 5 trials were open-label. The number of patients enrolled ranged from 191 to 902. All trials were conducted in more than 1 site. In most of the trials, patients from the US, Canada, and Europe were well represented; some trials included patients from Asian and South American countries.
Figure 12: Network of Trials Included in the Network Meta-Analysis
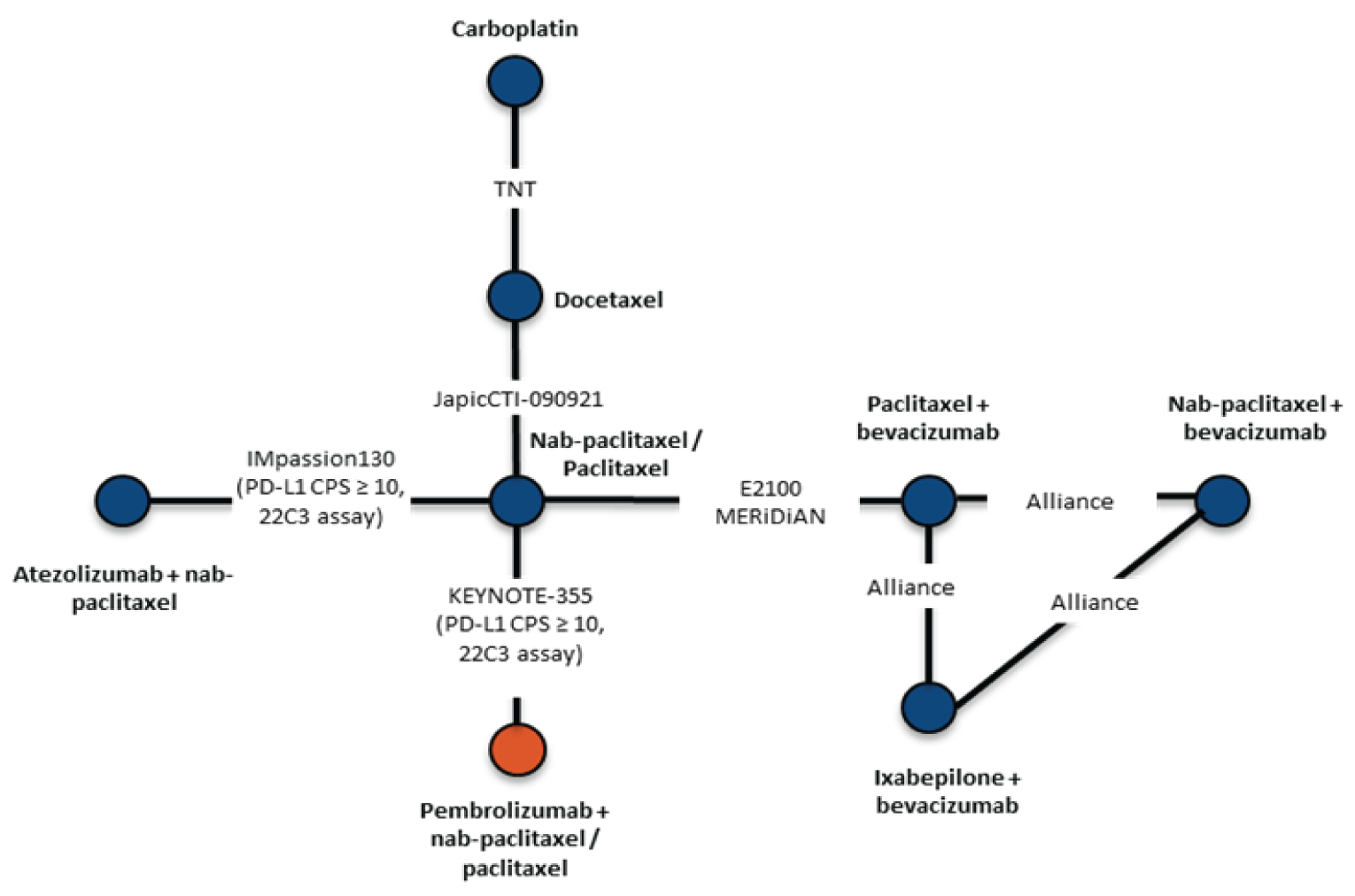
CPS = combined positive score; PD-L1 = programmed cell death 1 ligand 1; TNT = total neoadjuvant therapy.
Source: Sponsor-submitted indirect treatment comparison. Copyright 2017. Licensed under CC BY 4.0: https://creativecommons.org/licenses/by/4.0/
Treatment Characteristics
In the included trials, nab-paclitaxel and paclitaxel were the most frequently used interventions. Nab-paclitaxel (n = 5) and paclitaxel (n = 4) were included in 7 of the 8 trials. In 1 trial, bevacizumab was given as an optional treatment, with 97% of the patients opting to receive bevacizumab. The ixabepilone plus bevacizumab group did not match the population, intervention, comparison, and outcomes (PICOS) criteria and therefore was not of interest to this ITC and excluded. The chemotherapy combination of nab-paclitaxel plus bevacizumab, a second treatment group in another trial, was also not listed in the PICOS criteria but was included based on paclitaxel plus bevacizumab being of interest to this ITC and nab-paclitaxel being an approved substitute for paclitaxel for the treatment of metastatic HER2-negative breast cancer. Of the 18 treatment groups included in the network, 3 evaluated paclitaxel plus bevacizumab, 2 evaluated nab-paclitaxel alone, 2 evaluated paclitaxel, 2 evaluated docetaxel, and 1 evaluated carboplatin alone. The remaining groups involved unique chemotherapy combinations.
Baseline Patient Characteristics
The median age of patients in the selected trials ranged from 53 to 60 years. Caucasian was the predominant race, ranging from 66.7% to 89.9% in trials that reported patient ethnicity. The proportion of patients with an ECOG PS of 0 ranged from 51.5% to 88.8%. The proportion of patients with an ECOG PS of 1 ranged from 11.2% to 48.5%. Three trials enrolled TNBC patients exclusively. The proportion of TNBC patients in the remaining trials ranged from 15.2% to 95.8%. Prior neoadjuvant or adjuvant chemotherapy was reported in 7 RCTs, ranging from 30.3% to 78.2%.
Reported Outcomes
All RCTs reported PFS, 4 trials reported OS, and 4 trials reported ORR for TNBC patients. Across all intervention arms, median PFS ranged from 3.1 months to 8.8 months and median OS ranged from 12 months to 27.1 months. ORRs ranged from 31.4% to 58.9%. HRQoL was only reported in 1 trial. The incidence of AEs was reported in 4 trials. The incidence of any grade of AEs ranged from 98.2% to 100%. Discontinuation due to AEs ranged from 4.3% to 45%.
Quality Assessment
Results of the Cochrane risk-of-bias assessment demonstrated that, overall, the trials had a low risk of bias.
Results
Because only 1 trial connected each treatment in the evidence network, between-trial heterogeneity could not be reliably estimated. Therefore, the NMA was conducted with a fixed-effects model. The feasibility assessment of the sponsor-submitted ITC included: assessment of whether the RCT evidence for the interventions of interest forms 1 evidence network for each population and outcome of interest and assessment of the distribution of treatment, outcomes, trial, and patient characteristics that could modify treatment effects across direct comparisons of the evidence networks. The results of the feasibility assessment were not reported. Clinical heterogeneity was present in the analysis due to varying study eligibility criteria, treatment regimens administered, and some patient characteristics.
Overall Survival
OS was reported in 4 trials pertaining to 5 unique treatments (Figure 13). The NMA shows that pembrolizumab plus nab-paclitaxel or paclitaxel showed a favourable OS over nab-paclitaxel or paclitaxel (HR = 0.54; 95% CrI, 0.36 to 0.82), carboplatin (HR = 0.36; 95% CrI, 0.19 to 0.68), and docetaxel (HR = 0.30; 95% CI, = 0.17 to 0.55), but not atezolizumab plus nab-paclitaxel. The point estimate of the HR for pembrolizumab plus nab-paclitaxel or paclitaxel was numerically superior to atezolizumab plus nab-paclitaxel. The complete NMA results for OS are presented in Table 33.
Figure 13: Network of Trials Included in the Network Meta-Analysis for Overall Survival
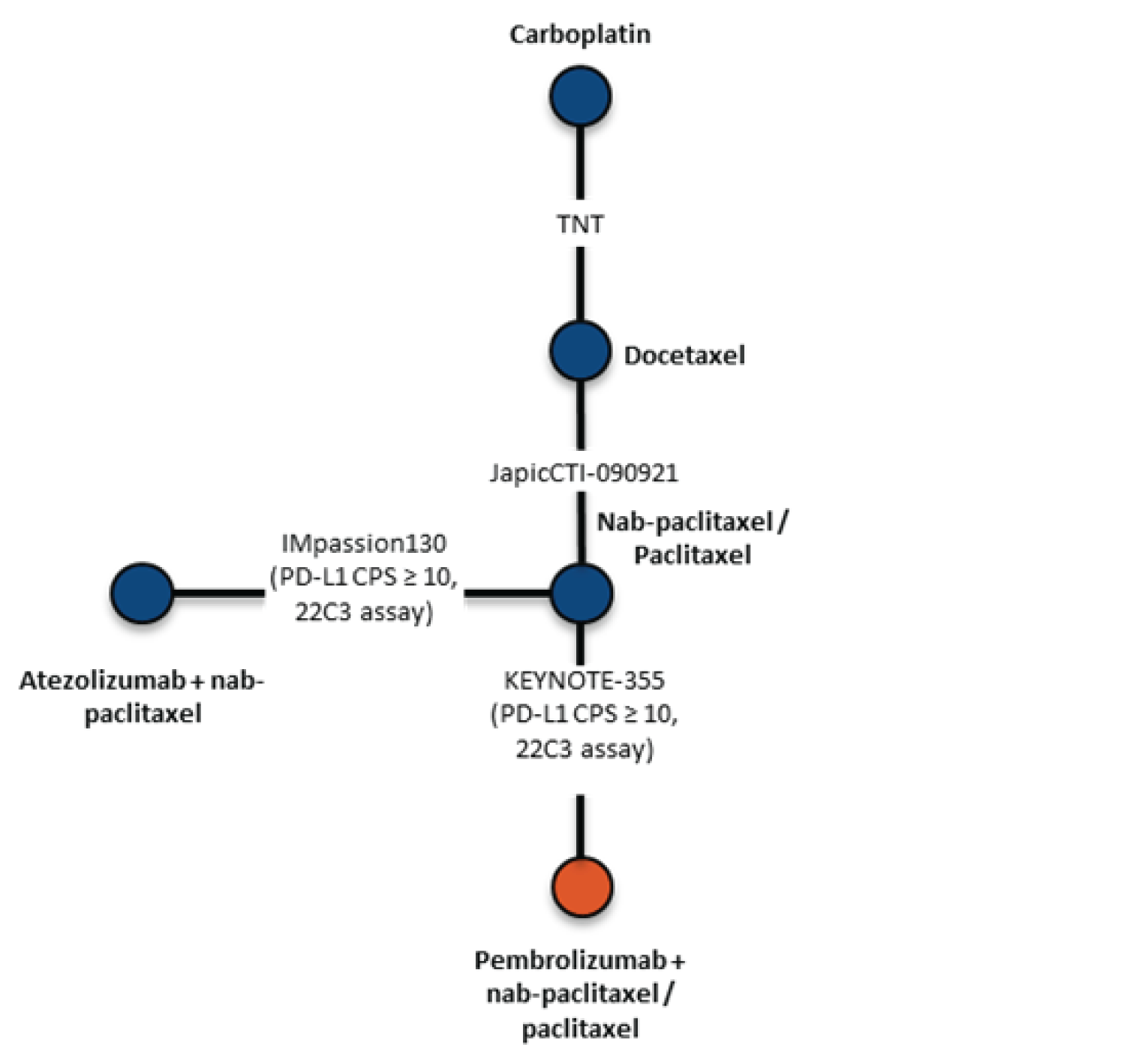
CPS = combined positive score; PD-L1 = programmed cell death 1 ligand 1; TNT = total neoadjuvant therapy.
Table 33: Fixed-Effect Indirect Treatment Comparison Results for Overall Survival
Treatment HR (95% CrI) | Nab-paclitaxel and/or paclitaxel | Atezolizumab plus nab-paclitaxel | Carboplatin | Docetaxel | Pembrolizumab plus nab-paclitaxel and/or paclitaxel |
|---|---|---|---|---|---|
Nab-paclitaxel and/or paclitaxel | — | 1.30 (0.97 to 1.75) | 0.66 (0.40 to 1.09) | 0.56 (0.36 to 0.86) | 1.85 (1.23 to 2.79) |
Atezolizumab plus nab-paclitaxel | 0.77 (0.57 to 1.04) | — | 0.51 (0.28 to 0.91) | 0.43 (0.26 to 0.73) | 1.42 (0.86 to 2.37) |
Carboplatin | 1.52 (0.92 to 2.51) | 1.97 (1.10 to 3.53) | — | 0.85 (0.66 to 1.10) | 2.81 (1.47 to 5.39) |
Docetaxel | 1.78 (1.16 to 2.74) | 2.32 (1.38 to 3.91) | 1.18 (0.91 to 1.52) | — | 3.30 (1.82 to 6.00) |
Pembrolizumab plus nab-paclitaxel and/or paclitaxel | 0.54 (0.36 to 0.82) | 0.70 (0.42 to 1.17) | 0.36 (0.19 to 0.68) | 0.30 (0.17 to 0.55) | — |
CrI = credible interval; HR = hazard ratio.
Notes: Each cell represents the comparison (hazard ratio and 95% credible interval) of the row treatment vs. the column treatment. All bolded values are statistically meaningful at a 0.05 significance level.
Source: Sponsor-submitted indirect treatment comparison.32
Progression-Free Survival
PFS was reported in all 6 trials pertaining to 8 unique treatments (Figure 14). Pembrolizumab plus nab-paclitaxel or paclitaxel showed a favourable PFS over nab-paclitaxel or paclitaxel (HR = 0.51; 95% CI, = 0.33 to 0.78) but not atezolizumab plus nab-paclitaxel, bevacizumab plus paclitaxel, carboplatin, docetaxel, ixabepilone plus bevacizumab, and bevacizumab plus nab-paclitaxel. The point estimate of the HR was numerically superior to atezolizumab plus nab-paclitaxel, bevacizumab plus paclitaxel, carboplatin, docetaxel, and ixabepilone plus bevacizumab. The complete NMA results for PFS are presented in Table 34.
Figure 14: Network of Trials Included in the Network Meta-Analysis for Progression-Free Survival
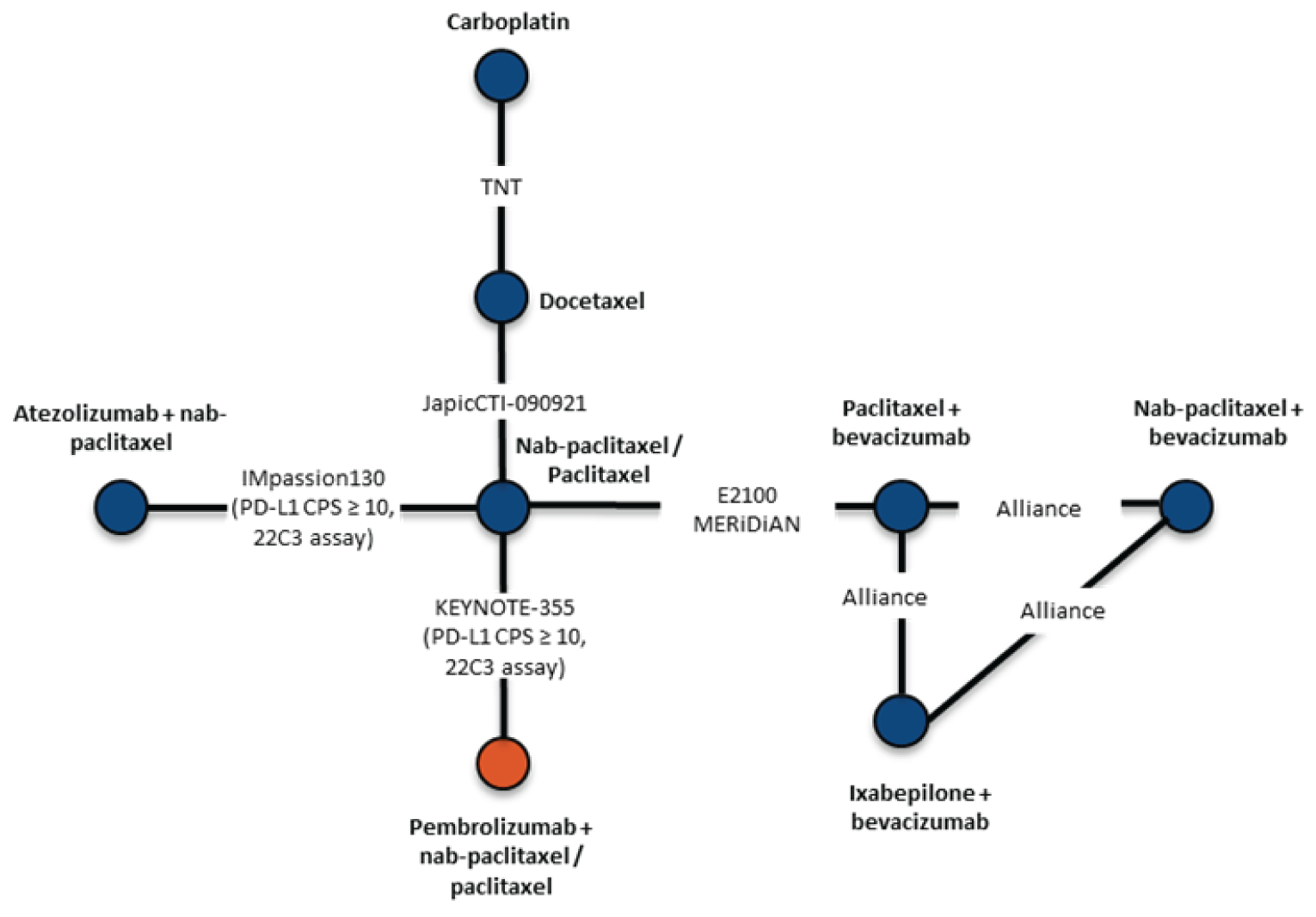
CPS = combined positive score; PD-L1 = programmed cell death 1 ligand 1; TNT = total neoadjuvant therapy.
Table 34: Fixed-Effect Indirect Treatment Comparison Results for Progressive-Free Survival
Treatment HR (95% CrI) | Nab-paclitaxel and/or paclitaxel | Atezolizumab plus nab-paclitaxel | Bevacizumab + paclitaxel | Carboplatin | Docetaxel | Ixabepilone + bevacizumab | Bevacizumab + nab-paclitaxel | Pembrolizumab + nab-paclitaxel and/or paclitaxel |
|---|---|---|---|---|---|---|---|---|
Nab-paclitaxel and/or paclitaxel | — | 1.41 (1.10 to 1.80) | 1.82 (1.41 to 2.33) | 1.15 (0.73 to 1.81) | 1.20 (0.80 to 1.80) | 1.31 (0.86 to 1.99) | 2.30 (1.49 to 3.55) | 1.96 (1.28 to 3.01) |
Atezolizumab plus nab-paclitaxel | 0.71 (0.56 to 0.91) | — | 1.29 (0.91 to 1.83) | 0.82 (0.49 to 1.37) | 0.85 (0.53 to 1.36) | 0.93 (0.57 to 1.51) | 1.63 (0.99 to 2.69) | 1.39 (0.85 to 2.28) |
Bevacizumab + paclitaxel | 0.55 (0.43 to 0.71) | 0.78 (0.55 to 1.10) | — | 0.64 (0.38 to 1.07) | 0.66 (0.41 to 1.06) | 0.72 (0.51 to 1.01) | 1.27 (0.89 to 1.81) | 1.08 (0.66 to 1.78) |
Carboplatin | 0.87 (0.55 to 1.37) | 1.22 (0.73 to 2.05) | 1.57 (0.94 to 2.65) | — | 1.04 (0.84 to 1.28) | 1.13 (0.61 to 2.11) | 1.99 (1.06 to 3.74) | 1.70 (0.91 to 3.18) |
Docetaxel | 0.83 (0.56 to 1.25) | 1.17 (0.73 to 1.89) | 1.51 (0.94 to 2.43) | 0.96 (0.78 to 1.19) | — | 1.09 (0.61 to 1.95) | 1.91 (1.06 to 3.47) | 1.63 (0.91 to 2.95) |
Ixabepilone + bevacizumab | 0.77 (0.50 to 1.17) | 1.08 (0.66 to 1.76) | 1.39 (0.99 to 1.96) | 0.88 (0.47 to 1.65) | 0.92 (0.51 to 1.65) | — | 1.76 (1.24 to 2.49) | 1.50 (0.82 to 2.75) |
Bevacizumab + nab-paclitaxel | 0.44 (0.28 to 0.67) | 0.61 (0.37 to 1.01) | 0.79 (0.55 to 1.13) | 0.50 (0.27 to 0.94) | 0.52 (0.29 to 0.94) | 0.57 (0.40 to 0.81) | — | 0.85 (0.46 to 1.57) |
Pembrolizumab + nab-paclitaxel and/or paclitaxel | 0.51 (0.33 to 0.78) | 0.72 (0.44 to 1.18) | 0.93 (0.56 to 1.52) | 0.59 (0.31 to 1.10) | 0.61 (0.34 to 1.10) | 0.67 (0.36 to 1.22) | 1.17 (0.64 to 2.15) | — |
Notes: Each cell represents the comparison (hazard ratio and 95% credible interval) of the row treatment vs. the column treatment. All bolded values are statistically meaningful at the 0.05 significance level.
Source: Sponsor-submitted indirect treatment comparison.32
Critical Appraisal of Sponsor-Submitted ITC
The sponsor’s rationale for conducting the ITC (i.e., absence of head-to-head studies that compared pembrolizumab plus chemotherapy relative to competing interventions of interest for the first-line treatment of previously untreated locally recurrent inoperable or metastatic TNBC) was clearly specified. From the ITC, comparators carboplatin, docetaxel, nab-paclitaxel, paclitaxel, and pembrolizumab are relevant to the Canadian clinical context while atezolizumab and bevacizumab are not. A comprehensive systematic review was performed. The efficacy outcomes of interest were PFS and OS.
The search and selection of the systematic review were restricted to trials published in English, which increases the risk of non–English-language publications not being identified. The impact of potential publication bias was also not explored in the review.
Clinical heterogeneity was present in the analysis due to varying eligibility criteria, treatment regimens administered, and some patient characteristics. Such heterogeneity likely resulted in bias and undermined the validity of the NMA results.
The sponsor-submitted ITC did not apply adjustments or conduct subgroup analyses to minimize heterogeneity.
The use of subgroup data from several comparator trials inhibits the ability to compare baseline patient characteristics for the population of interest. Five of the included trials33-35,37,39 enrolled a broader population of patients with breast cancer and, although subgroup data for patients with TNBC was used in the analyses, baseline patient characteristics were not reported by subgroup. As a result, between-trial comparisons of baseline patient characteristics depend on the assumption that the baseline characteristics for the overall study population are reflective of the subgroup of interest. This assumption was not investigated and is unlikely to hold, which means there could be a considerable amount of undetected clinical heterogeneity and/or treatment-effect modifiers that could bias the results of the NMA.
Due to limited data availability, only 1 study connected each treatment in the evidence network. As a result, between-trial heterogeneity could not be statistically estimated. The NMA was therefore performed using a fixed-effects assumption, which is less plausible than a random-effects assumption.
Given the differences in patient characteristics such as historical use of chemotherapy, present disease, and treatment indication, and potential heterogeneity, exchangeability of patients in the trials included of the NMA was not guaranteed.
Inconsistency of the network was not reported, likely due to the limited ability to do so given the network only had 1 closed loop.
As most trials did not provide Kaplan-Meier curves for the population of interest, it was not possible to evaluate the proportional hazards assumption. The NMA was conducted with a proportional hazard ratios model, which may not reflect changes in hazard ratios between treatments over time.
Several relevant outcomes, including safety, HRQoL, and ORR, were not assessed in the sponsor-submitted ITC, and no justification was provided for why they were not assessed.
Given these limitations, the results from the sponsor-submitted ITC are at risk of considerable bias. The CADTH review team concluded that the reported comparative efficacy of pembrolizumab plus chemotherapy over relevant comparators is subject to uncertainty and not reliable.
Summary
The sponsor-submitted ITC conducted a systematic review and used a Bayesian NMA to evaluate the relative efficacy and safety of pembrolizumab plus chemotherapy and other comparators, including nab-paclitaxel or paclitaxel, atezolizumab plus nab-paclitaxel, bevacizumab plus paclitaxel, carboplatin, docetaxel, ixabepilone plus bevacizumab, bevacizumab plus nab-paclitaxel, and pembrolizumab plus nab-paclitaxel or paclitaxel for the first-line treatment of patients with previously untreated locally recurrent inoperable or metastatic TNBC. The NMA was based on a systematic review of the literature, and data from 6 studies33-38 were used to inform the analyses. The efficacy outcomes of interest were PFS and OS.33-38
The sponsor-submitted ITC reported that the results for OA favoured pembrolizumab plus chemotherapy over nab-paclitaxel or paclitaxel (HR = 0.54; 95% CrI, 0.36 to 0.82), carboplatin (HR = 0.36; 95% CrI, 0.19 to 0.68), and docetaxel (HR = 0.30; 95% CrI, 0.17 to 0.55).
The sponsor-submitted ITC reported that the results for PFS favoured pembrolizumab plus chemotherapy over nab-paclitaxel or paclitaxel (HR = 0.51; 95% CrI, 0.33 to 0.78). However, pembrolizumab plus chemotherapy was not favoured versus other comparators included in the ITC for PFS.
Due to limited data availability, the sponsor-submitted ITC was not able to obtain and compare baseline patient characteristics between the included trials; it was also not able to estimate between-trial heterogeneity due to the small number of trials in the network. Consequentially, there is substantial uncertainty around the ITC results and firm conclusions cannot be drawn about the relative efficacy between pembrolizumab plus chemotherapy and relevant comparators, aside from direct evidence provided by the KEYNOTE-355 study.
Discussion
Summary of Available Evidence
The CADTH systematic review included 1 pivotal trial (KEYNOTE-355) submitted by the sponsor and 1 sponsor-submitted ITC. Additional input from 2 patient groups, 3 clinician groups, and 2 clinical experts was also considered during the review.
The KEYNOTE-355 study is an ongoing, phase III, randomized, multicentre, double-blind, placebo-controlled trial. The primary objective of the trial was to evaluate the efficacy and safety of pembrolizumab plus chemotherapy versus placebo plus chemotherapy for patients with locally recurrent inoperable or metastatic TNBC not been previously treated with chemotherapy. The KEYNOTE-355 study was initiated in August 2016 at 291 participating centres across 29 countries in North America (5 centres in Canada; N = 34), South America, Europe, Asia, and Australia.
Enrolled patients were female, 18 years and older, and had locally recurrent inoperable TNBC not previously treated with chemotherapy, and which could not be treated with curative intent, or mTNBC not previously treated with chemotherapy. Patients were to have completed treatment for stage I to III breast cancer, if indicated, with 6 or more months between the completion of treatment with curative intent and first documented local or distant disease recurrence. Patients were randomized in a 2:1 ratio into either of the 2 trial arms (566 patients were randomized to receive pembrolizumab plus chemotherapy and 281 to receive placebo plus chemotherapy) based on 3 stratification factors: type of chemotherapy on study (paclitaxel or nab-paclitaxel or gemcitabine and carboplatin), PD-L1 expression at baseline (CPS ≥ 1 or < 1), and prior treatment with the same class of chemotherapy in the neoadjuvant or adjuvant setting (yes or no). Coprimary end points investigated in the KEYNOTE-355 trial were OS and PFS assessed by blinded independent central review. ORR, DOR, HRQoL, and safety outcomes were secondary outcomes assessed in the trial. Utility as assessed by the EQ VAS was an exploratory outcome.
By the final analysis data cut-off date (June 15, 2021), 847 patients were randomized in the ITT population. In total, 75.1% and 38.1% had a tumour tissue PD-L1 expression (CPS) of 1 or higher and 10 or higher, respectively. All patients enrolled were female. The majority of patients were younger than 65 years of age, white, postmenopausal, and had an ECOG PS of 0.
The sponsor-submitted ITC conducted a systematic review and used a Bayesian NMA to evaluate the relative efficacy and safety of pembrolizumab plus chemotherapy and other comparators, including nab-paclitaxel or paclitaxel, atezolizumab plus nab-paclitaxel, bevacizumab plus paclitaxel, carboplatin, docetaxel, ixabepilone plus bevacizumab, bevacizumab plus nab-paclitaxel, and pembrolizumab plus nab-paclitaxel or paclitaxel for the first-line treatment of previously untreated locally recurrent inoperable or mTNBC in adults. The efficacy outcomes of interest were PFS and OS.
Interpretation of Results
Efficacy
The CADTH review protocol identified OS, PFS, ORR, DOR, HRQoL, and safety as important outcomes. All outcomes included in the CADTH protocol were prespecified in the KEYNOTE-355 protocol before final analysis data cut-off (June 15, 2021) and the findings are presented in this review. The type I error rate was adequately accounted for during the analyses of OS, PFS, and ORR using the familywise error rate. The stopping rules were presented in the statistical analysis plan. Sensitivity analyses were conducted for PFS to assess the robustness of the data and, overall, the results were consistent with the primary analyses.
Based on results from the final analysis, pembrolizumab plus chemotherapy provided a statistically significant and clinically meaningful improvement in OS compared with placebo plus chemotherapy for patients with PD-L1–positive tumours (CPS ≥ 10) (HR = 0.73; 95% CI, 0.55 to 0.95; P = 0.0093). The clinical experts consulted by CADTH during the review considered the observed OS benefit with pembrolizumab plus chemotherapy group (median of 23.0 versus 16.1 months) compared to chemotherapy alone to be clinically meaningful in the target patient population with an incurable and aggressive disease that lacks biomarkers for targeted therapeutic interventions. This benefit was much smaller in all patients of the trial (median of 17.2 versus 15.5 months). As the subpopulation of interest for reimbursement was not stratification-randomized, there was potential bias due to an imbalance between treatment groups. However, the Health Canada Reviewer Report noted that an evaluation and sensitivity analyses of the potential for imbalance in the population with a CPS of 10 or higher had been conducted by the sponsor. The conclusion was that the impact of not having a CPS of 10 or higher as a stratification factor was minimal, and the imbalances in baseline factors were limited and did not change the conclusion of the primary analysis.17
PFS was assessed as a coprimary outcome in the KEYNOTE-355 trial. The consistency in the improvement of PFS would strengthen the robustness of the PFS findings from this trial. At IA2, pembrolizumab plus chemotherapy demonstrated a statistically significant and clinically meaningful improvement in PFS compared with placebo plus chemotherapy in patients with a PD-L1 CPS of 10 or higher. The PFS obtained at the final analysis data cut-off (June 15, 2021) was consistent with IA2, although it was not tested according to the statistical hierarchy. The HR obtained between pembrolizumab plus chemotherapy versus placebo plus chemotherapy was 0.66 (95% CI, 0.50 to 0.88; P = 0.0018) in patients with a PD-L1 CPS of 10 or higher. Median PFS was greater by almost 4 months in the pembrolizumab group compared to the placebo group. The clinical experts considered the findings to be clinically meaningful in this patient population, in which delaying disease progression is important as it is associated with higher burden of disease symptoms and a decrease in quality of life.
The ORR and DOR results supported the results found for OS and PFS.
The clinician and patient groups consulted during the CADTH review highlighted improvement in HRQoL as an important treatment goal for patients with mTNBC. HRQoL was measured using 3 questionnaires (EORTC QLQ-C30, EORTC QLQBR23, and 5-Level EQ-5D) and no differences were observed. However, there were several limitations on the assessment of this outcome. HRQoL estimates measured up to week 15 may not provide an accurate picture of patient experiences with the combination of pembrolizumab plus chemotherapy for a prolonged period of time. An assessment time point at week 15 was selected to ensure at least 60% completion and 80% compliance with patient-reported outcome assessments to ensure validity of the longitudinal model of change in patient-reported outcome scores over time. Over the relatively short time period studied, there was no signal suggesting that the addition of pembrolizumab to chemotherapy resulted in a significant decrease in HRQoL. The experts consulted by CADTH noted that they expected to see decreases in HRQoL in practice for patients with metastatic disease over the course of their disease duration.
All subgroup analyses were prespecified before the interim data cut-offs; however, no analyses of between-groups differences were conducted. The findings were therefore considered exploratory, and no definitive conclusions were made. The clinical experts consulted by CADTH commented on the differential treatment effects among chemotherapies in subgroup analyses, with greater treatment benefit observed with pembrolizumab plus taxanes compared to pembrolizumab plus gemcitabine and carboplatin. The clinical experts indicated that a combination of chemotherapies in the metastatic setting would be used in patients with a high burden of disease in clinical practice, which means those patients receiving gemcitabine and carboplatin were likely sicker and had a poorer prognosis. However, the clinical experts repeated that no definitive conclusions can be drawn regarding the possible synergistic benefit for pembrolizumab and chemotherapies used in the study, given the exploratory nature of this analysis and lack of statistical testing.
The KEYNOTE-355 study eligibility criteria included only patients with an ECOG PS of 0 or 1. As a result, the benefit and safety of the pembrolizumab plus chemotherapy in the metastatic setting is unknown in patients with an ECOG PS greater than 1, particularly patients with an ECOG PS of 2, in the real-world setting that may be considered for therapy. The clinical experts consulted by CADTH generally agreed that patients with mTNBC and an ECOG PS of 2 would benefit from treatment with the pembrolizumab combination, although they would not consider patients with an ECOG PS of 3 or greater eligible for pembrolizumab treatment. The clinical experts consulted by CADTH noted that amendment 5, which shifted the primary analysis to a focus on patients with a PD-L1 CPS of 10 or higher, was a logical choice, given that this is the target of pembrolizumab’s mechanism of action.
The sponsor-submitted ITC reported that there was evidence of improvements of pembrolizumab plus chemotherapy over nab-paclitaxel or paclitaxel (HR = 0.54; 95% CrI, 0.36 to 0.82), carboplatin (HR = 0.36; 95% CrI, 0.19 to 0.68), and docetaxel (HR = 0.30; 95% CI, = 0.17 to 0.55) for OS. In addition, PFS was improved in pembrolizumab plus chemotherapy over nab-paclitaxel or paclitaxel (HR = 0.51; 95% CI = 0.33 to 0.78); but not over other treatments. The sponsor-submitted ITC had several limitations, including limited data availability, an inability to obtain and compare baseline patient characteristics between the included trials, and an inability to estimate between-trial heterogeneity due the small number of trials in the network. Consequentially, there is substantial uncertainty around the ITC results and firm conclusions cannot be drawn on the relative efficacy between the pembrolizumab combination and relevant comparators, aside from direct evidence provided by the KEYNOTE-355 study.
Harms
Overall, pembrolizumab in combination with chemotherapy had a manageable safety profile, which is consistent with the known safety profiles of pembrolizumab monotherapy and the administered chemotherapies (taxane [paclitaxel or nab-paclitaxel] or gemcitabine and carboplatin). No new safety concerns were identified for the use of pembrolizumab plus chemotherapy for the treatment of locally recurrent inoperable or metastatic TNBC. The safety results at the final analysis were generally consistent with those observed at IA2.
Almost all patients enrolled in both study arms of the KEYNOTE-355 trial reported at least 1 AE by the final analysis data cut-off (June 15, 2021). AEs of grade 3 or higher were slightly more common in the pembrolizumab plus chemotherapy group (77.9%) compared to placebo plus chemotherapy and placebo (73.7%). The most common AEs in both groups were neutropenia, decreased neutrophil count deceased, anemia, thrombocytopenia, decreased white blood cell count, and leukopenia. Approximately 15% more SAEs were reported in patients receiving pembrolizumab plus chemotherapy compared to patients receiving placebo plus chemotherapy and placebo.
Overall, AEs resulting in death in the pembrolizumab plus chemotherapy group (3.0%) were consistent with those in the placebo plus chemotherapy group (1.8%). AEs leading to discontinuation of any study intervention was higher in the pembrolizumab plus chemotherapy group (10.7%) compared to the placebo plus chemotherapy and placebo group (5.3%). Notable harms were more common in the pembrolizumab plus chemotherapy group compared to placebo plus chemotherapy and placebo. The most common notable harms in the pembrolizumab versus placebo chemotherapy group were hypothyroidism (15.8 versus 3.2%), hyperthyroidism (4.3% versus 1.1%), infusion reactions (3.7% versus 5.0%), and pneumonitis (2.5% versus 0%). The clinical experts consulted by CADTH noted that they would expect more AEs in the pembrolizumab group given that an additional treatment has been added to the regimen.
The clinical experts consulted by CADTH agreed that the toxicity profile of pembrolizumab plus chemotherapy was manageable in practice, and they emphasized the importance of immune-related AEs associated with the use of pembrolizumab. The experts noted that pembrolizumab is currently being used in practice for other indications and AEs, particularly immune-related AEs specific to pembrolizumab already known to clinicians. As a result, the therapy can be managed in practice and no extra activities to manage AEs are needed.
Conclusions
One pivotal study (KEYNOTE-355) and 1 sponsor-submitted ITC provided evidence for this CADTH review. The OS and PFS benefits observed with pembrolizumab plus chemotherapy versus placebo plus chemotherapy in patients with a PD-L1 CPS of 10 or higher in the KEYNOTE-355 trial were statistically significant, considered clinically meaningful by the clinical experts, and aligned with the outcomes important to patient groups. The secondary outcomes, ORR and DOR, were supportive of the observed OS and PFS results. There was no signal suggesting that the addition of pembrolizumab to chemotherapy resulted in a significant decrease in HRQoL from baseline to week 15. The submitted ITC compared the efficacy of pembrolizumab plus nab-paclitaxel or paclitaxel to other comparators, and results suggested that OS favoured pembrolizumab plus chemotherapy in the comparison to nab-paclitaxel or paclitaxel, carboplatin, and docetaxel, and PFS favoured pembrolizumab plus chemotherapy in the comparison to nab-paclitaxel or paclitaxel but not to other treatments. However, no firm conclusions could be drawn from the ITC results due to several limitations. No new safety concerns were identified for the use of pembrolizumab plus chemotherapy for the treatment of locally recurrent inoperable or metastatic TNBC. The clinical experts stated that there is experience using pembrolizumab for other indications, and oncologists are familiar with the AEs associated with the use of pembrolizumab.
References
1.Costa RLB, Gradishar WJ. Triple-negative breast cancer: current practice and future directions. J Oncol Pract. 2017;13(5):301-303. PubMed
2.Brouckaert O, Wildiers H, Floris G, Neven P. Update on triple-negative breast cancer: prognosis and management strategies. Int J Womens Health. 2012;4:511-520. PubMed
3.American Cancer Society. Types of cancer: triple-negative breast cancer. 2022; https://www.cancer.org/cancer/breast-cancer/about/types-of-breast-cancer/triple-negative.html#written_by. Accessed 2022 Apr 25.
4.National Comprehensive Cancer Network. Breast cancer metastatic. (NCCN guidelines for patients). Plymouth Meeting (PA): National Comprehensive Cancer Network; 2022: https://www.nccn.org/patients/guidelines/content/PDF/stage_iv_breast-patient.pdf. Accessed 2022 Apr 25.
5.Canadian Cancer Society. Breast cancer. 2022; https://cancer.ca/en/cancer-information/cancer-types/breast. Accessed 2022 Apr 25.
6.National Cancer institute. Cancer stat facts: female breast cancer subtypes. [2022]; https://seer.cancer.gov/statfacts/html/breast-subtypes.html. Accessed 2022 Oct 17.
7.American Cancer Society. Types of breast cancer: triple-negative breast cancer. 2022; https://www.cancer.org/cancer/breast-cancer/about/types-of-breast-cancer/triple-negative.html. Accessed 2022 Apr 25.
8.Canadian Cancer Statistics Advisory Committee. Canadian cancer statistics. Toronto (ON): Canadian Cancer Society; 2021: https://cancer.ca/Canadian-Cancer-Statistics-2021-EN. Accessed 2022 Apr 25.
9.Anders CK, Carey LA. ER/PR negative, HER2-negative (triple-negative) breast cancer. In: Post TW, ed. UpToDate. Waltham (MA): UpToDate; 2022: www.uptodate.com. Accessed 2022 Oct 17.
10.Kassam F, Enright K, Dent R, et al. Survival outcomes for patients with metastatic triple-negative breast cancer: implications for clinical practice and trial design. Clin Breast Cancer. 2009;9(1):29-33. PubMed
11.Khosravi-Shahi P, Cabezón-Gutiérrez L, Custodio-Cabello S. Metastatic triple-negative breast cancer: optimizing treatment options, new and emerging targeted therapies. Asia Pac J Clin Oncol. 2018;14(1):32-39. PubMed
12.Seung SJ, Traore AN, Pourmirza B, Fathers KE, Coombes M, Jerzak KJ. A population-based analysis of breast cancer incidence and survival by subtype in Ontario women. Curr Oncol. 2020;27(2):e191-e198. PubMed
13.Thientosapol ES, Tran TT, Della-Fiorentina SA, et al. Survival times of women with metastatic breast cancer starting first-line chemotherapy in routine clinical practice versus contemporary randomised trials. Intern Med J. 2013;43(8):883-888. PubMed
14.Keytruda (pembrolizumab): solution for infusion 100 mg/4 mL vial; Antineoplastic agent, monoclonal antibody [product monograph]. Kirkland (QC): Merck Canada Inc.; 2021 Nov 19.
15.Clinical Study Report: P355V03MK3475. A randomized, double-blind, phase iii study of pembrolizumab (MK-3475) plus chemotherapy vs. placebo plus chemotherapy for previously untreated locally recurrent inoperable or metastatic triple-negative breast cancer – (KEYNOTE-355) [internal sponsor's report]. Rahway (NJ): Merck Sharp & Dohme Corp.; 2021 Sep 13.
16.Clinical trial end points for the approval of cancer drugs and biologics: guidance for industry. Silver Spring (MD): U.S. Food and Drug Administratioin; 2018: https://www.fda.gov/media/71195/download?msclkid=13ae9943b6a611ec8c85e1611aaf5d94. Accessed 2022 Sep 20.
17.Health Canada reviewer's report: Keytruda (pembrolizumab) [internal sponsor's report]. In: Drug Reimbursement Review sponsor submission: Keytruda (pembrolizumab), 100 mg/4 mL vial; solution for infusion. Kirkland (QC): Merck Canada Inc.; 2022 Jun 20.
18.Canadian Cancer Society. Stages of breast cancer. [2022]: https://cancer.ca/en/cancer-information/cancer-types/breast/staging. Accessed 2022 Sep 20.
19.Abrams Kaplan D. Overview of the updated NCCN guidelines on triple-negative breast cancer. (Sponsored special report) 2021; https://www.hmpgloballearningnetwork.com/site/jcp/jcp-special-report/overview-updated-nccn-guidelines-triple-negative-breast-cancer. Accessed 2022 Sep 20.
20.Canadian Cancer Society. Triple-negative and basal-like breast cancers. 2022; https://cancer.ca/en/cancer-information/cancer-types/breast/what-is-breast-cancer/cancerous-tumours/triple-negative-breast-cancer. Accessed 2022 Sep 20.
21.Keytruda (pembrolizumab): solution for infusion 100 mg/4 mL vial. Antineoplastic agent, monoclonal antibody [product monograph]. Kirkland (QC): Merck Canada Inc.; 2022 Apr 5.
22.TAXOL (paclitaxel): injection, 6 mg/mL; Antineoplastic agent [product monograph]. Montreal (QC): Bristol-Myers Squibb Canada; 2010 Feb 22.
23.McGowan J, Sampson M, Salzwedel DM, Cogo E, Foerster V, Lefebvre C. PRESS Peer Review of Electronic Search Strategies: 2015 guideline statement. J Clin Epidemiol. 2016;75:40-46. PubMed
24.Grey matters: a practical tool for searching health-related grey literature. Ottawa (ON): CADTH; 2019: https://www.cadth.ca/grey-matters. Accessed 2022 Oct 17.
25.Merck Sharp & Dohme LLC. NCT02819518: Study of pembrolizumab (MK-3475) plus chemotherapy vs. placebo plus chemotherapy for previously untreated locally recurrent inoperable or metastatic triple-negative breast cancer (MK-3475-355/KEYNOTE-355). ClinicalTrials.gov. Bethesda (MD): U.S. National Library of Medicine; 2016: https://clinicaltrials.gov/ct2/show/study/NCT02819518. Accessed 2022 Sep 20.
26.Drug Reimbursement Review sponsor submission: Keytruda (pembrolizumab), 100 mg/4 mL vial; solution for infusion [internal sponsor's package]. Kirkland (QC): Merck Canada Inc.; 2022 Jun 20.
27.Schmid P, Salgado R, Park YH, et al. Pembrolizumab plus chemotherapy as neoadjuvant treatment of high-risk, early-stage triple-negative breast cancer: results from the phase 1b open-label, multicohort KEYNOTE-173 study. Ann Oncol. 2020;31(5):569-581. PubMed
28.Aaronson NK, Ahmedzai S, Bergman B, et al. The European Organisation for Research and Treatment of Cancer QLQ-C30: a quality-of-life instrument for use in international clinical trials in oncology. J Natl Cancer Inst. 1993;85(5):365-376. PubMed
29.Fayers P, Bottomley A. Quality of life research within the EORTC-the EORTC QLQ-C30. European Organisation for Research and Treatment of Cancer. Eur J Cancer. 2002;38 Suppl 4:S125-133. PubMed
30.Sprangers MA, Groenvold M, Arraras JI, et al. The European Organisation for Research and Treatment of Cancer breast cancer-specific quality-of-life questionnaire module: first results from a three-country field study. J Clin Oncol. 1996;14(10):2756-2768. PubMed
31.Merck Canada response to 2022 Aug 26 DRR request for additional information regarding Keytruda (pembrolizumab) for the treatment of metastatic triple-negative breast cancer (mTNBC) DRR review [internal additional sponsor's information]. Kirkland (QC): Merck Canada Inc.; 2022 Sep 1.
32.Systematic literature review and network meta-analysis of interventions for the first-line treatment of locally recurrent inoperable, or metastatic triple-negative breast cancer [internal sponsor's report]. In: Drug Reimbursement Review sponsor submission: Keytruda (pembrolizumab), 100 mg/4 mL vial; solution for infusion. Kirkland (QC): Merck Canada Inc.; 2022 Jun 20.
33.Tutt A, Tovey H, Cheang MCU, et al. Carboplatin in BRCA1/2-mutated and triple-negative breast cancer BRCAness subgroups: the TNT Trial. Nat Med. 2018;24(5):628-637. PubMed
34.Tamura K, Inoue K, Masuda N, et al. Randomized phase II study of nab-paclitaxel as first-line chemotherapy in patients with HER2-negative metastatic breast cancer. Cancer Sci. 2017;108(5):987-994. PubMed
35.Miles D, Cameron D, Bondarenko I, et al. Bevacizumab plus paclitaxel versus placebo plus paclitaxel as first-line therapy for HER2-negative metastatic breast cancer (MERiDiAN): A double-blind placebo-controlled randomised phase III trial with prospective biomarker evaluation. Eur J Cancer. 2017;70:146-155. PubMed
36.Rugo HS, Schmid P, Cescon DW, et al. Abstract GS3-01: Additional efficacy end points from the phase 3 KEYNOTE-355 study of pembrolizumab plus chemotherapy vs. placebo plus chemotherapy as first-line therapy for locally recurrent inoperable or metastatic triple-negative breast cancer. Cancer Res. 2021;81(4_Supplement):GS3-01-GS03-01.
37.Rugo HS, Barry WT, Moreno-Aspitia A, et al. Abstract GS3-06: Long-term follow-up of CALGB 40502/NCCTG N063H (Alliance): A randomized phase III trial of weekly paclitaxel (P) compared to weekly nanoparticle albumin bound nab-Paclitaxel (NP) or ixabepilone (Ix) +/− bevacizumab as first-line therapy for locally recurrent or metastatic breast cancer (MBC). Cancer Res. 2018;78(4_Supplement):GS3-06-GS03-06.
38.Cortes Castan J, Guo Z, Karantza V, Aktan G. KEYNOTE-355: Randomized, double-blind, phase III study of pembrolizumab (pembro) + chemotherapy (chemo) vs. placebo (pbo) + chemo for previously untreated, locally recurrent, inoperable or metastatic triple-negative breast cancer (mTNBC). Ann Oncol. 2017;28(Supplement 10):x25.
39.Miller K, Wang M, Gralow J, et al. Paclitaxel plus bevacizumab versus paclitaxel alone for metastatic breast cancer. N Engl J Med. 2007;357(26):2666-2676. PubMed
40.Yardley DA, Coleman R, Conte P, et al. nab-Paclitaxel plus carboplatin or gemcitabine versus gemcitabine plus carboplatin as first-line treatment of patients with triple-negative metastatic breast cancer: results from the tnAcity trial. Ann Oncol. 2018;29(8):1763-1770. PubMed
41.Letellier ME, Dawes D, Mayo N. Content verification of the EORTC QLQ-C30/EORTC QLQ-BR23 with the International Classification of Functioning, Disability and Health. Qual Life Res. 2015;24(3):757-768. PubMed
42.McLachlan SA, Devins GM, Goodwin PJ. Validation of the European Organisation for Research and Treatment of Cancer Quality of Life Questionnaire (QLQ-C30) as a measure of psychosocial function in breast cancer patients. Eur J Cancer. 1998;34(4):510-517. PubMed
43.Landis JR, Koch GG. The measurement of observer agreement for categorical data. Biometrics. 1977;33(1):159-174. PubMed
44.Groenvold M, Klee MC, Sprangers MA, Aaronson NK. Validation of the EORTC QLQ-C30 quality of life questionnaire through combined qualitative and quantitative assessment of patient-observer agreement. J Clin Epidemiol. 1997;50(4):441-450. PubMed
45.Musoro JZ, Coens C, Fiteni F, et al. Minimally important differences for interpreting EORTC QLQ-C30 scores in patients with advanced breast cancer. JNCI Cancer Spectr. 2019;3(3):pkz037. PubMed
46.Kawahara T, Taira N, Shiroiwa T, et al. Minimal important differences of EORTC QLQ-C30 for metastatic breast cancer patients: Results from a randomized clinical trial. Qual Life Res. 2022;31(6):1829-1836. PubMed
47.Ousmen A, Conroy T, Guillemin F, et al. Impact of the occurrence of a response shift on the determination of the minimal important difference in a health-related quality of life score over time. Health Qual Life Outcomes. 2016;14(1):167. PubMed
48.Osoba D, Rodrigues G, Myles J, Zee B, Pater J. Interpreting the significance of changes in health-related quality-of-life scores. J Clin Oncol. 1998;16(1):139-144. PubMed
49.Bjelic-Radisic V, Cardoso F, Cameron D, et al. An international update of the EORTC questionnaire for assessing quality of life in breast cancer patients: EORTC QLQ-BR45. Ann Oncol. 2020;31(2):283-288. PubMed
Appendix 1: Literature Search Strategy
Note that this appendix has not been copy-edited.
Clinical Literature Search
Overview
Interface: Ovid
Databases:
MEDLINE All (1946–)
Embase (1974–)
Note: Patient headings and search fields have been customized for each database. Duplicates between databases were removed in Ovid.
Date of search: June 27, 2022
Alerts: Bi-weekly search updates until project completion
Search filters applied: No filters were applied to limit the retrieval by study type
Limits:
Conference abstracts: excluded
Syntax | Description |
|---|---|
/ | At the end of a phrase, searches the phrase as a Patient heading |
MeSH | Medical Patient Heading |
exp | Explode a Patient heading |
* | Before a word, indicates that the marked Patient heading is a primary topic; or, after a word, a truncation symbol (wildcard) to retrieve plurals or varying endings |
# | Truncation symbol for one character |
? | Truncation symbol for one or no characters only |
adj# | Requires terms to be adjacent to each other within # number of words (in any order) |
.ti | Title |
.ot | Original title |
.ab | Abstract |
.hw | Heading word; usually includes Patient headings and controlled vocabulary |
.kf | Keyword heading word |
.rn | Registry number |
.nm | Name of substance word (MEDLINE) |
.yr | Publication year |
medall | Ovid database code: MEDLINE All, 1946 to present, updated daily |
oemezd | Ovid database code; Embase, 1974 to present, updated daily |
cctr | Ovid database code; Cochrane Central Register of Controlled Trials |
Multi-Database Strategy
(Keytruda* or pembrolizumab* or lambrolizumab* or MK 3475 or MK3475 or Merck 3475 or HSDB 8257 or HSDB8257 or Sch 900475 or Sch900475 or DPT0O3T46P).ti,ab,kf,ot,hw,rn,nm.
exp breast neoplasms/
(((breast* or mamma or mammar* or lobular*) adj5 (cancer* or carcinoid* or carcinoma* or carcinogen* or adenocarcinoma* or adeno-carcinoma* or malignan* or metasta* or neoplas* or sarcoma* or tumo?r* or mass* or triple-negative)) or mBC or m-BC or LABC or TNBC or mTNBC).ti,ab,kf,ot,hw.
2 or 3
1 and 4
5 use medall
*pembrolizumab/
(Keytruda* or pembrolizumab* or lambrolizumab* or MK 3475 or MK3475 or Merck 3475 or HSDB 8257 or HSDB8257 or Sch 900475 or Sch900475).ti,ab,kf,dq.
7 or 8
exp breast tumour/
(((breast* or mamma or mammar* or lobular*) adj5 (cancer* or carcinoid* or carcinoma* or carcinogen* or adenocarcinoma* or adeno-carcinoma* or malignan* or metasta* or neoplas* or sarcoma* or tumo?r* or mass* or triple-negative)) or mBC or m-BC or LABC or TNBC or mTNBC).ti,ab,kf,dq.
10 or 11
9 and 12
13 use oemezd
14 not (conference abstract or conference review).pt.
6 or 15
remove duplicates from 16
Clinical Trials Registries
ClinicalTrials.gov
Produced by the US National Library of Medicine. Targeted search used to capture registered clinical trials.
[Search terms: pembrolizumab OR Keytruda AND triple-negative breast cancer OR TNBC]
WHO ICTRP
International Clinical Trials Registry Platform, produced by the World Health Organization. Targeted search used to capture registered clinical trials.
[Search terms: pembrolizumab OR Keytruda AND triple-negative breast cancer OR TNBC]
Health Canada’s Clinical Trials Database
Produced by Health Canada. Targeted search used to capture registered clinical trials.
[Search terms: pembrolizumab OR Keytruda AND triple-negative breast cancer OR TNBC]
EU Clinical Trials Register
European Union Clinical Trials Register, produced by the European Union. Targeted search used to capture registered clinical trials.
[Search terms: pembrolizumab OR Keytruda AND triple-negative breast cancer OR TNBC]
Grey Literature
Search dates: July 28, 2022, to July 6, 2022
Keywords: [Keytruda OR pembrolizumab AND triple-negative breast cancer OR TNBC]
Limits: No search limits
Updated: Search updated prior to the completion of stakeholder feedback period
Relevant websites from the following sections of the CADTH grey literature checklist Grey Matters: A Practical Tool for Searching Health-Related Grey Literature were searched:
Health Technology Assessment Agencies
Health Economics
Clinical Practice Guidelines
Drug and Device Regulatory Approvals
Advisories and Warnings
Drug Class Reviews
Clinical Trials Registries
Databases (free)
Health Statistics
Internet Search
Open Access Journals
Appendix 2: Efficacy Analyses in Patients With PD-L1 CPS ≥ 1
Note that this appendix has not been copy-edited.
Table 36: Analysis of OS in Patients With PD-L1 CPS ≥ 1 and All Patients — ITT Population
Analysis measurement | Patients with PD-L1 CPS ≥ 1 | All patients | ||
|---|---|---|---|---|
Pembrolizumab plus Chemotherapy (N = 425) | Placebo plus Chemotherapy (N = 211) | Pembrolizumab plus Chemotherapy (N = 566) | Placebo plus Chemotherapy (N = 281) | |
Number of Events (%) | 336 (79.1) | 177 (83.9) | 460 (81.3) | 238 (84.7) |
Kaplan-Meier Estimates (Months)a | ||||
Median (95% CI) | 17.6 (15.5 to 19.5) | 16.0 (12.8 to 17.4) | 17.2 (15.3 to 19.0) | 15.5 (13.9 to 17.2) |
Q1, Q3 | 8.9 to 34.3 | 9.5 to 27.4 | 8.9 to 32.9 | 9.0 to 27.6 |
Person-Months | 9,043.9 | 4,109.1 | 11,759.5 | 5,422.7 |
Event Rate / 100 Person-Months | 3.7 | 4.3 | 3.9 | 4.4 |
Hazard Ratio (95% CI)b | 0.86 (0.72 to 1.04) | 0.89 (0.76 to 1.05) | ||
P valuec | 0.0563 | 0.0797 | ||
OS Rate at Month 6 (%) (95% CI) | 86.5 (82.9 to 89.5) | 89.1 (84.0 to 92.6) | 86.4 (83.2 to 88.9) | 87.9 (83.4 to 91.2) |
OS Rate at Month 12 (%) (95% CI) | 64.3 (59.5 to 68.6) | 63.3 (56.4 to 69.5) | 64.5 (60.4 to 68.3) | 62.2 (56.2 to 67.5) |
OS Rate at Month 18 (%) (95% CI) | 48.4 (43.5 to 53.0) | 41.4 (34.7 to 48.0) | 47.8 (43.6 to 51.9) | 41.8 (36.0 to 47.5) |
OS Rate at Month 24 (%) (95% CI) | 37.7 (33.1 to 42.3) | 29.5 (23.5 to 35.8) | 35.5 (31.6 to 39.5) | 30.4 (25.1 to 35.8) |
CI = confidence interval; CPS = combined positive score; ITT = intention-to-treat; OS = overall survival; PD-L1 = programmed cell death 1 ligand 1.
aFrom product-limit (Kaplan-Meier) method for censored data.
bBased on Cox regression model with the Efron method of tie handling with treatment as a covariate stratified by chemotherapy on study (taxane vs. gemcitabine/carboplatin) and prior treatment with same class of chemotherapy in the (neo)adjuvant setting (yes vs. no).
cOne-sided P value based on log-rank test stratified by chemotherapy on study (taxane vs. gemcitabine/carboplatin) and prior treatment with same class of chemotherapy in the (neo)adjuvant setting (yes vs. no).
Data cut-off date: June 15, 2021.
Source: Clinical Study Report.15
Table 37: Analysis of PFS Based on BICR Assessment in Patients With PD-L1 CPS ≥ 1 and All Patients — ITT Population
Analysis measurement | Patients with PD-L1 CPS ≥ 1 | All patients | ||
|---|---|---|---|---|
Pembrolizumab plus chemotherapy (N = 425) | Placebo plus chemotherapy (N = 211) | Pembrolizumab plus chemotherapy (N = 566) | Placebo plus chemotherapy (N = 281) | |
Number of events (%) | 299 (70.4) | 166 (78.7) | 406 (71.7) | 217 (77.2) |
Kaplan-Meier estimates (months)a | ||||
Median (95% CI) | 7.6 (6.6 to 8.0) | 5.6 (5.4 to 7.4) | 7.5 (6.3 to 7.7) | 5.6 (5.4 to 7.2) |
Q1, Q3 | 3.6 to 16.5 | 3.5 to 9.7 | 3.5 to 14.5 | 3.5 to 9.9 |
Person-months | 4,228.7 | 1,627.3 | 5,234.4 | 2,209.2 |
Event rate/100 person-months | 7.1 | 10.2 | 7.8 | 9.8 |
Hazard ratio (95% CI)b | 0.75 (0.62 to 0.91) | 0.82 (0.70 to 0.98) | ||
P valuec | 0.0016 | 0.0120 | ||
PFS rate at month 3 (%) (95% CI) | 78.1 (73.8 to 81.7) | 78.7 (72.5 to 83.7) | 76.9 (73.1 to 80.2) | 80.3 (75.1 to 84.5) |
PFS rate at month 6 (%) (95% CI) | 56.4 (51.3 to 61.2) | 46.6 (39.3 to 53.5) | 55.4 (51.0 to 59.6) | 47.4 (41.1 to 53.4) |
PFS rate at month 9 (%) (95% CI) | 43.1 (38.0 to 48.2) | 32.8 (26.0 to 39.7) | 42.0 (37.6 to 46.4) | 32.9 (27.0 to 38.9) |
PFS rate at month 12 (%) (95% CI) | 31.7 (26.8 to 36.6) | 19.4 (13.8 to 25.9) | 29.3 (25.2 to 33.5) | 20.8 (15.6 to 26.4) |
BICR = Blinded Independent Central Review; CI = confidence interval; CPS = combined positive score; ITT = intention-to-treat; PD-L1 = programmed cell death 1 ligand 1; PFS = progression-free survival; Q = quartile.
aFrom product-limit (Kaplan-Meier) method for censored data.
bBased on Cox regression model with the Efron method of tie handling with treatment as a covariate stratified by chemotherapy on study (taxane vs. gemcitabine/carboplatin) and prior treatment with same class of chemotherapy in the (neo)adjuvant setting (yes versus no).
cOne-sided P value based on log-rank test stratified by chemotherapy on study (taxane versus gemcitabine/carboplatin) and prior treatment with same class of chemotherapy in the (neo)adjuvant setting (yes versus no).
Data cut-off date: June 15, 2021.
Source: Clinical Study Report.15
Table 38: Analysis of ORR Based on BICR Assessment (RECIST 1.1) in Patients With PD-L1 CPS ≥ 1 and All Patients — ITT Population
Treatment | Patients with PD-L1 CPS ≥ 1 | All patients | ||
|---|---|---|---|---|
Pembrolizumab plus chemotherapy (N = 425) | Placebo plus chemotherapy (N = 211) | Pembrolizumab plus chemotherapy (N = 566) | Placebo plus chemotherapy (N = 281) | |
Number of objective responses | 191 | 82 | 231 | 104 |
ORR (%) (95% CI) | 44.9 (40.1, 49.8) | 38.9 (32.2, 45.8) | 40.8 (36.7 to 45.0) | 37.0 (31.4 to 42.9) |
Treatment difference versus comparator Estimate (95% CI)a | 6.1 (-2.1, 14.0) | 3.8 (-3.2 to 10.6) | ||
P value | 0.0725b | 0.1413b | ||
Number of complete responses, n | 55 | 19 | 77 | 31 |
CR, % (95% CI) | 12.9 (9.9 to 16.5) | 9.0 (5.5 to 13.7) | 13.6 (10.9 to 16.7) | 11.0 (7.6 to 15.3) |
Number of PR, n (%) | 136 | 63 | 207 | 108 |
PR, % (95% CI) | 32.0 (27.6 to 36.7) | 29.9 (23.8 to 36.5) | 36.6 (32.6 to 40.7) | 38.4 (32.7 to 44.4) |
BICR = blinded independent central review; CI = confidence interval; CPS = combined positive score; CR = complete response; ITT = intention-to-treat; ORR = overall response rate; PD-L1 = programmed cell death 1 ligand 1; PR = partial response; RECIST 1.1 = response evaluation criteria in solid tumours version 1.1.
aBased on Miettinen and Nurminen method stratified by chemotherapy on study (taxane vs. gemcitabine/carboplatin) and prior treatment with same class of chemotherapy in the (neo)adjuvant setting (yes vs. no).
bNominal P value. One-sided P value for testing. H0: difference in % = 0 versus H1: difference in % > 0. Confirmed responses are included.
Data cut-off date: June 15, 2021.
Source: Clinical Study Report.15
Table 39: Summary of Time to Response and DOR Based on BICR Assessment (RECIST 1.1) in Patients With PD-L1 CPS ≥ 1 and Confirmed Response — ITT Population
Analysis measurement | Patients with PD-L1 CPS ≥ 1 | All patients | ||
|---|---|---|---|---|
Pembrolizumab plus chemotherapy (N = 425) | Placebo plus chemotherapy (N = 211) | Pembrolizumab plus chemotherapy (N = 566) | Placebo plus chemotherapy (N = 281) | |
Objective response | ||||
Number of Patients with objective response | 191 | 82 | 231 | 104 |
Time to response (months) | ||||
Mean (SD) | 2.4 (1.4) | 3.1 (3.2) | 2.5 (1.5) | 3.7 (5.7) |
Median (range) | 1.9 (1.2 to11.7) | 2.0 (1.6 to 28.4) | 1.9 (1.2 to 11.7) | 2.0 (1.6 to 42.1) |
Response durationa (months) | ||||
Median (range) | 10.1 (1.0+ to 45.9+) | 6.8 (1.5 to 46.6+) | 10.1 (1.0+ to 45.9+) | 6.5 (1.5 to 46.6+) |
Number (%b) of patients with extended response duration | ||||
≥6 months | 124 (76.2) | 41 (59.0) | 152 (76.9) | 50 (56.8) |
≥ 12 months | 67 (46.8) | 20 (29.6) | 81 (46.1) | 26 (33.3) |
BICR = Blinded Independent Central Review; CPS = combined positive score; DOR = duration of response; ITT = intention to treat; PD-L1 = programmed cell death 1 ligand 1; RECIST = response evaluation criteria in solid tumours version 1.1.; SD = standard deviation.
aIncludes patients with confirmed complete response or partial response.
bFrom product-limit (Kaplan-Meier) method for censored data.
"+" indicates there is no progressive disease by the time of last disease assessment.
Data cut-off date: June 15, 2021.
Source: Clinical Study Report.15
Appendix 3: Description and Appraisal of Outcome Measures
Note that this appendix has not been copy-edited.
Aim
To describe the following outcome measures and review their measurement properties (validity, reliability, responsiveness to change, and minimal important difference [MID])
European Organisation for Research and Treatment of Cancer Quality of Life Questionnaire Core 30 (EORTC QLQ-C30)
The European Organisation for Research and Treatment of Cancer Quality of Life Questionnaire – Breast Module 23 (EORTC QLQ-BR23)
Findings
Table 40: Summary of Outcome Measures and Their Measurement Properties
Outcome measure | Type | Conclusions about measurement properties | MID |
|---|---|---|---|
EORTC QLQ-C30 | A 30-item, patient-reported, cancer-specific, HRQoL questionnaire using 4- and 7-point Likert scales.28 | Validity: Content validity: When mapping to the World Health Organization’s ICF framework, 25 of the 30 items in the EORTC QLQ-C30 were endorsed by the experts.41 Discriminant validity: As represented by correlation with external parameters such as ECOG performance status (Spearman’s rank correlation values ranging from 0.02 to 0.56) in patients with metastatic breast cancer.42 Convergent validity: As represented by correlation with scores on the Profile of Mood States and Psychosocial Adjustment to Illness Scale, was also deemed to be acceptable (Spearman rank correlation values ranging from 0.02 to 0.76) in patients with metastatic breast cancer.42 Reliability: Inter-rater reliability: As represented by patient-observer agreement on the EORTC QLQ-C30 questionnaire, the median kappa coefficient for agreement across the 30 items in the EORTC QLQ-C30 was 0.86 with a range of 0.48 to 1.00 in patients with metastatic breast cancer, representing substantial to near-perfect agreement for most items.43,44 Responsiveness: No literature was identified that assessed responsiveness in patients with breast cancer. | For patients with advanced or metastatic breast cancer, using anchor-based method, estimated MIDs for within-group changes ranged from 5 to 15 points for improvements and from -17 to -4 points for deterioration across the individual scales. For between-group differences, MIDs ranged from 4 to 11 points for improvements and from -18 to -4 points for deterioration across the individual scales.45,46 |
EORTC QLQ-BR23 | A 23-items patient-reported, breast cancer-specific, HRQoL questionnaire using scales range in score from 0 to 100.30 | Validity: Content validity: When mapping to the World Health Organization’s ICF framework, 21 of the 23 items in the EORTC QLQ-BR23 were endorsed by the experts.41 Convergent validity: The EORTC QLQ-BR23 demonstrated weak to moderate item-scale correlations (ranging from 0.09 to 0.90) for all scales in patients with breast cancer.30 Discriminant validity: In patients with breast cancer, the EORTC QLQ-BR23 demonstrated the ability to discriminate between patients from mutually exclusive subgroups with medium to large effect sizes (ranging from 0.42 to 1.1).30 Reliability: Internal consistency was adequate in patients with breast cancer. Cronbach alpha coefficients for the multiitem scales of the EORTC QLQ-BR23 ranged from 0.46 to 0.94 across all samples.30 Responsiveness: No literature was identified that assessed responsiveness in patients with breast cancer. | In patients with breast cancer or suspicious breast cancer, the minimal of observed MID at 6 months (ranging from 0.4 to 4) was smaller in case of deterioration for EORTC QLQ-BR23 compared to 3 months (ranging from 7 to 20). Similar trend was observed in the case of improvement, where the observed MID was 2 or less at 6 months (ranging from 0.7 to 2) while the observed at 3 months was greater than or equal to 2 (ranging from 2 to 15).47 |
ECOG = Eastern Cooperative Oncology Group; EORTC QLQ-BR23 = The European Organisation for Research and Treatment of Cancer Quality of Life Questionnaire – Breast Module 23; EORTC QLQ-C30 = European Organisation for Research and Treatment of Cancer Quality of Life Questionnaire Core 30; HRQoL= health-related quality of life; ICF = International Classification of Functioning; MID = minimal important difference.
European Organisation for Research and Treatment of Cancer Quality of Life Questionnaire Core 30
Description and Scoring
The EORTC QLQ-C30 is one of the most used patient-reported outcome measures in oncology clinical trials. It is a multidimensional, cancer-specific, self-administered, measure of HRQoL.28
The EORTC QLQ-C30 is composed of both multi-item scales and single-item measures. These include 5 functional scales (physical, role, cognitive, emotional, and social), 3 symptom scales (fatigue, pain, and nausea and vomiting), a global health status/HRQoL scale, and 6 single items assessing additional symptoms commonly reported by cancer patients (dyspnea, loss of appetite, insomnia, constipation and diarrhea) as well as perceived financial impact of the disease.28
The EORTC QLQ-C30 uses a 1-week recall period to assess functional status and symptoms. All scales and single-item measures are scored from 0 to 100. Most questions have 4 response options (“not at all,” “a little,” “quite a bit,” “very much”), with scores on these items ranging from 1 to 4. For the 2 items that form the global HRQoL scale, the response format is a 7-point Likert-type scale with anchors at 1 = “very poor” and 7 = “excellent.” Raw scores for each scale are computed as the average of the items that contribute to a particular scale. Scale sum scores are transformed such that a high score on the functional scales represents a high/healthy level of functioning, a high score on the symptom scales represents a high level of symptomatology, and a high score on the global health status/HRQoL scale represents a high HRQoL.29
According to the EORTC QLQ-C30 scoring algorithm, if there are missing items for a scale (i.e., the patient did not provide a response), the score for the scale can still be computed if there are responses for at least half of the items. The values for missing items are interpolated with the average of the respondent-completed items.29
Assessment of Validity, Reliability, and Responsiveness
One study41 assessed the content validity of the EORTC QLQ-C30 based on the opinions of 21 experts. When mapping to the World Health Organization’s International Classification of Functioning framework, 25 of the 30 items in the EORTC QLQ-C30 were endorsed by the experts: 15 items mapping to impairment of body function, 7 mapping to activity limitations/participation restrictions, and 1 item mapping to both components. There were only 2 items of the EORTC QLQ-C30 tapped content outside of functioning: Item 29 mapping to perceived health and item 30 mapping to global quality of health. The authors stated that the fact that most items from the EORTC QLQ-C30 can be linked to the ICF framework means that the instrument’s content reflects functioning, which is a key component of HRQoL.41
No studies were identified that investigated the validity, reliability, or responsiveness of the EORTC QLQ-C30 among patients with early-stage TNBC. Among patients with metastatic breast cancer, a 1997 study investigated the inter-rater reliability using patient-observer agreement on the EORTC QLQ-C30 questionnaire. The median kappa coefficient for agreement across the 30 items in the EORTC QLQ-C30 was 0.86 with a range of 0.48 to 1.00,44 representing substantial to near-perfect agreement for most items.43 Another study42 investigated the discriminative and convergent validity of the psychosocial subscales of EORTC QLQ-C30 in patients with breast cancer. The study found acceptable discriminative validity represented by correlation with external parameters such as Eastern Cooperative Oncology Group (ECOG) performance status (Spearman’s rank correlation values ranging from 0.02 to 0.56). A correlation of 0.2 represented significance at the 0.01 level. The convergent validity, as represented by correlation with scores on the Profile of Mood States and Psychosocial Adjustment to Illness Scale, was also deemed to be acceptable (Spearman’s rank correlation values ranging from 0.08 to 0.76).42
Minimal Important Difference
One study from 1998,48 conducted in patients with breast cancer and small-cell lung cancer, estimated that a change in score on any scale of the EORTC QLQ-C30 of 10 points would be clinically significant. This estimate was based on an anchor-based approach to estimate the MID in which patients who reported “a little” change (for better or worse) on the Patientive significance questionnaire (SSQ) had corresponding changes on a function or symptom scale of the EORTC QLQ-C30 of approximately 5 to 10 points. Patients who reported a “moderate” change had corresponding changes in the EORTC QLQ-C30 of about 10 to 20 points, and those who reported “very much” change had corresponding changes in the EORTC QLQ-C30 of more than 20 points.48
A more recent study from 201945 aimed to estimate the MID for the EORTC QLQ-C30 in patients with advanced breast cancer. This study used anchor-based and distribution-based approaches, utilizing performance status and selected AEs as the anchor variables. MIDs for within-group changes ranged from 5 to 14 points for improvements and from –14 to –4 points for deterioration across the individual scales. For between-group differences, MIDs ranged from 4 to 11 points for improvements and from –18 to –4 points for deterioration across the individual scales.45 Kawahara and collogues46 analyzed a dataset of 154 metastatic breast cancer patients using anchors obtained from patients (transition items) and clinicians (performance status). MIDs were estimated in 8 of 15 scales of EORTC QLQ-C30. Estimated MIDs for within-group improvement varied from 7 to 15 and those for deterioration varied from –17 to −7. Estimated MIDs for between-group improvement varied from 5 to 11 and those for deterioration varied from –8 to −5 across EORTC QLQ-C30 scales.46 In addition, A study from 201647 aimed to investigate the effect of response shift on MID over time for the EORTC QLQ- C30 in patients with breast cancer or suspicious breast cancer. Three hundred eighty-one patients recruited from 4 hospitals and care centres participated in this study with a mean age of 58.4 years (standard deviation = 11 years). This study used an anchor-based approach utilizing deterioration improvement as the anchor variables. The minimal of observed MID at 6 months (ranging from 0.5 to 10) was smaller in case of deterioration for EORTC QLQ-C30 compared to 3 months (ranging from 5 to 26). With regards to improvement, the observed MID at 6 months (ranging from 0.8 to 7) was similar to the observed MID at 3 months (ranging from 0.3 to 10).47
European Organisation for Research and Treatment of Cancer Quality of Life Questionnaire — Breast Module 23
Description and Scoring
The EORTC QLQ-BR23 includes an additional 23 items that are specific to breast cancer, with 5 multi-item scales assessing systemic therapy side effects, group symptoms, breast symptoms, body image, and sexual functioning, as well as single items assessing sexual enjoyment, hair loss, and future perspective.49 All scales range in score from 0 to 100, and higher scores represent higher response thus a high score for functioning represents high functioning while a high symptom score represents a high symptom burden. The EORTC QLQ-BR23 should not be administered as a freestanding instrument as it does not measure a multidimensional construct of body image; instead, the EORTC QLQ-BR23 should be administered in conjunction with the EORTC QLQ-C30.49
Assessment of Validity, Reliability, and Responsiveness
One study41 assessed the content validity of the EORTC QLQ-BR23 based on the opinions of 13 experts. When mapping to the World Health Organization’s International Classification of Functioning framework, 21 of the 23 items in the EORTC QLQ-BR23 were endorsed by the experts: 20 at the impairment level and 1 at the activity and participation level. The authors stated that the fact that most items from the EORTC QLQ-BR23 can be linked to the ICF framework means that the instrument’s content reflects functioning, which is a key component of HRQoL.
Construct validity was assessed by investigating convergent validity and known-groups validity in 1 study30 of 496 patients aged 25 to 83 years with breast cancer from 3 countries (Netherlands, Spain, and the US). Overall, the EORTC QLQ-BR23 had weak to moderate item-scale correlations (ranging from 0.09 to 0.90) for all scales, among them, the body image and sexual functioning scales had demonstrated moderated to strong item-scale correlations (ranging from 0.30 to 0.83 for body image and from 0.77 to 0.90 for sexual functioning) across all samples. With regards to known-groups validity, the EORTC QLQ-BR23 demonstrated the ability to discriminate between patients from mutually exclusive subgroups differing in disease stage, previous surgery, performance status, and treatment modality. The study reported medium to large effect sizes (ranging from 0.42 to 1.1) of the significant group differences in sexual functioning, future perspective, group symptoms and systemic therapy side effects between patients from the abovementioned mutually exclusive subgroups.30
Internal consistency reliability was also investigated in the same study.30 Cronbach alpha coefficients for the multiitem scales of the EORTC QLQ-BR23 were, in general, lowest in the Spanish sample (ranging from 0.46 to 0.94), and highest in the American sample (range, 0.70 to 0.91), with the coefficients of the Dutch sample holding an intermediate position (range, 0.57 to 0.89).30
Minimal Important Difference
MIDs for EORTC QLQ-BR23 were also investigated in the same study that investigated the effect of response shift on MID over time for the EORTC QLQ-C30 in patients with breast cancer or suspicious breast cancer.47 The study used an anchor-based approach utilizing deterioration and improvement as the anchor variables. The minimal of observed MID at 6 months (ranging from 0.4 to 4) was smaller in case of deterioration for EORTC QLQ-BR23 compared to 3 months (ranging from 7 to 20). A similar trend was observed in the case of improvement, where the observed MID at 6 months ranged from 0.7 to 2, while the observed MID at 3 months ranged from 2 to 15.47
Pharmacoeconomic Review
Abbreviations
BIA
budget impact analysis
CPS
combined positive score
CUA
cost-utility analysis
HRQoL
health-related quality of life
ICER
incremental cost-effectiveness ratio
mTNBC
metastatic triple-negative breast cancer
NMA
network meta-analysis
OS
overall survival
PFS
progression-free survival
PD-L1
programmed cell death 1 ligand 1
QALY
quality-adjusted life-year
RDI
relative dose intensity
TNBC
triple-negative breast cancer
TOT
time on treatment
Executive Summary
The executive summary comprises 2 tables (Table 1 and Table 2) and a conclusion.
Item | Description |
|---|---|
Drug product | Pembrolizumab (Keytruda), IV solution |
Submitted price | Pembrolizumab, IV infusion, 100 mg per 4 mL: $4,400 per vial |
Indication | In combination with chemotherapy, for the treatment of adult patients with locally recurrent unresectable or metastatic triple-negative breast cancer who have not received prior chemotherapy for metastatic disease and whose tumours express PD-L1 as determined by a validated test (combined positive score ≥ 10) |
Health Canada approval status | NOC |
Health Canada review pathway | Advance consideration under NOC/c |
NOC date | November 19, 2021 |
Reimbursement request | As per indication |
Sponsor | Merck Canada Inc. |
Submission history | Pembrolizumab (Keytruda) has been reviewed for numerous indications at CADTH; this is the first submission review for metastatic triple-negative breast cancer |
NOC = Notice of Compliance; PD-L1 = programmed cell death 1 ligand 1.
Table 2: Summary of Economic Evaluation
Component | Description |
|---|---|
Type of economic evaluation | Cost-utility analysis Partitioned survival model |
Target population | Adults with locally recurrent inoperable or metastatic TNBC whose tumours expressed PD-L1 (CPS ≥ 10) and who have not received chemotherapy for recurrent inoperable or metastatic TNBC |
Treatment | Pembrolizumab in combination with chemotherapy (1 of nab-paclitaxel, paclitaxel, or gemcitabine plus carboplatin) |
Comparator | Chemotherapy (1 of nab-paclitaxel, paclitaxel, or gemcitabine plus carboplatin) |
Perspective | Canadian publicly funded health care payer |
Outcomes | QALYs, life-years |
Time horizon | Lifetime (20 years) |
Key data source | KEYNOTE-355, a phase III, randomized, placebo-controlled, double-blind trial informing PFS, OS, time on treatment, and utility values |
Submitted results | ICER = $175,414 per QALY (incremental costs = $124,946; QALYs = 0.71) |
Key limitations |
|
CADTH reanalysis results |
|
CPS = combined positive score; ICER = incremental cost-effectiveness ratio; OS = overall survival; PD-L1 = programmed cell death 1 ligand 1; PFS = progression-free survival; PSM = partitioned survival model; QALY = quality-adjusted life-year; TNBC = triple-negative breast cancer.
Conclusions
The CADTH clinical review found that, compared with chemotherapy (1 of nab-paclitaxel, paclitaxel, or gemcitabine plus carboplatin), the addition of pembrolizumab was associated with a statistically and clinically significant improvement in overall survival (OS) and progression-free survival (PFS) of patients with locally recurrent inoperable or metastatic triple-negative breast cancer (mTNBC) whose tumours expressed programmed cell death 1 ligand 1 (PD-L1) (combined positive score [CPS] ≥ 10) based on the KEYNOTE-355 study. The long-term clinical effectiveness of pembrolizumab beyond the trial period (4 years) is uncertain. The clinical review also found no significant difference in health-related quality of life (HRQoL) outcomes between the pembrolizumab and chemotherapy arms of the KEYNOTE-355 trial. However, the analyses of HRQoL were collected over a short duration of follow-up (15 weeks).
CADTH undertook a reanalysis that reweighted the distribution of chemotherapy drugs to align with Canadian clinical practice, assumed a relative dose intensity of 100% for all treatments, and modelled health utilities based on disease progression status in alignment with the manner in which disease-management costs were captured. CADTH’s base case was aligned with the sponsor’s results such that both analyses suggested that pembrolizumab plus chemotherapy was associated with higher costs and improved quality-adjusted life-years (QALYs) but was not cost-effective at a willingness-to-pay threshold of $50,000 per QALY gained. Based on publicly available list prices for all comparators, a price reduction for pembrolizumab of at least 81% would be required for it to be cost-effective in combination with chemotherapy at this threshold.
This estimate is sensitive to assumptions about the long-term comparative effectiveness of pembrolizumab plus chemotherapy and the manner in which health utilities and disease-management costs are captured. The incremental cost-effectiveness ratio (ICER) increased drastically when the treatment effect was assumed to wane and a time-to-death approach was taken to model utilities and disease-management costs, indicating a greater price reduction may be warranted given the uncertainty with the assumptions used in the CADTH base case.
Stakeholder Input Relevant to the Economic Review
This section is a summary of the feedback received from the patient groups, registered clinicians, and drug plans that participated in the CADTH review process that pertains to the economic submission.
Patient input was received from Rethink Breast Cancer and Canadian Breast Cancer Network, which collected perspectives of caregivers and patients with mTNBC through online surveys and interviews in Canada. Patients with mTNBC reported on the debilitating impact of symptoms — including fatigue, insomnia, physical pain, and emotional pain — which affects their daily quality of life, ability to care for family, employment, and social activities. Current treatments noted to be available to patients included chemotherapy, surgery, and radiation. Beyond first-line therapy, treatment options are limited. Treatment goals included delayed disease progression, prolonged survival without sacrificing quality of life, and fewer and less-severe adverse events. Patients were generally willing to tolerate side effects for long-term health benefits. Patients also expressed a need for treatment and diagnostic testing that is accessible and affordable.
Clinician input was received from breast cancer medical oncologists in Canada and provincial breast tumour groups in Alberta and Ontario. Given the incurable nature of mTNBC, treatment goals were noted to be primarily palliative in nature, with the primary goal being delayed disease progression and improved OS. Clinician input noted current first-line treatments include single-drug and combination chemotherapy. Subsequent lines of therapy include chemotherapy (taxane, anthracycline, platinum [carboplatin with or without gemcitabine], eribulin, vinorelbine, capecitabine) and sacituzumab govitecan. Treatment goals were improved OS and delayed relapse. Pembrolizumab is expected to be used as a first-line treatment in combination with chemotherapy (paclitaxel, nab-paclitaxel [uncommonly], or carboplatin plus gemcitabine). Candidates for pembrolizumab would be identified using PD-L1 CPS expression and Eastern Cooperative Oncology Group Performance Status. The clinicians described clinically meaningful response to treatment as a reduction in frequency or severity of symptoms, stabilization of symptoms, improved organ function, and radiographic tumour response with either stabilization of disease or response measured using Response Evaluation Criteria in Solid Tumours Version 1.1. Treatment response was recommended to be assessed at least every 3 months initially and discontinued in cases of toxicity, disease progression, and/or patient refusal.
The drug plans noted weight-based dosing of pembrolizumab (2 mg/kg every 3 weeks to a max of 200 mg, or 4 mg/kg up to 400 mg every 6 weeks) would be implemented, if reimbursed. The drug plans also noted concerns with the overall budget impact of pembrolizumab given the high volume of patients with triple-negative breast cancer (TNBC) and the cost of pembrolizumab. The plans raised concerns about the choice of backbone chemotherapy, noting that generic versions of all chemotherapy comparators included in the KEYNOTE-355 trial, with the exception of nab-paclitaxel, are available. Further, the plans noted the need for PD-L1 CPS testing to be operationalized for breast cancer and funded in jurisdictions on or before pembrolizumab implementation.
Two these concerns were addressed in the sponsor’s model:
Treatment goals of PFS and OS were modelled.
The cost of PD-L1 testing was included.
CADTH also addressed these concerns by considering a scenario analysis that assumed a weight-based dosing of pembrolizumab.
CADTH was unable to address 1 concern raised in stakeholder input:
Within the economic model, the sponsor incorporated a fixed-dosing approach (i.e., 200 mg every 3 weeks) for pembrolizumab according to the Health Canada indication and product monograph for pembrolizumab, which was implemented in the KEYNOTE-355 trial. As the sponsor did not include an option to assess the effects of extended dosing intervals for pembrolizumab, CADTH was unable to explore this option further.
Economic Review
The current review is for pembrolizumab (Keytruda) for adult patients with locally recurrent inoperable or metastatic TNBC whose tumours expressed PD-L1 (CPS ≥ 10) and who have not received chemotherapy for recurrent inoperable or metastatic TNBC.
Economic Evaluation
Summary of Sponsor’s Economic Evaluation
Overview
The sponsor submitted a cost-utility analysis (CUA) of pembrolizumab in combination with chemotherapy (consisting of either paclitaxel, nab-paclitaxel, or gemcitabine plus carboplatin based on the pivotal trial options) compared with chemotherapy alone for the treatment of adult patients with locally recurrent inoperable or metastatic TNBC whose tumours expressed PD-L1 (CPS ≥ 10) and who have not received prior chemotherapy for their recurrent or metastatic disease. The modelled population is aligned with the Health Canada indication and reimbursement request.
Pembrolizumab is available as a powder for solution for infusion (100 mg per 4 mL vial). The recommended dosage is 200 mg every 3 weeks in combination with chemotherapy.1 Chemotherapy drugs used in combination included paclitaxel (90 mg/m2 on days 1, 8 and 15 of every 28-day cycle), nab-paclitaxel (100 mg/m2 on days 1, 8 and 15 of every 28-day cycle) and gemcitabine plus carboplatin (1,000 mg/m2 and area under the curve 2, respectively, on days 1 and 8 of every 21-day cycle). At the submitted price of $4,400 per 4 mL vial and assuming 100% dose intensity, the per-cycle cost of pembrolizumab was estimated to be $8,800. When used in combination with chemotherapy at the sponsor’s assumed dose intensities, the total regimen cost of pembrolizumab plus chemotherapy was $11,400 per cycle. The total regimen cost for chemotherapy alone was $3,672 per cycle. The sponsor considered vial sharing (50%) and relative dose intensity (RDI) in the cost calculation for a first-line drug.
The submitted model reported both QALYs and life-years over a lifetime time horizon (20 years) in the modelled population. The base-case analysis was conducted from the perspective of the Canadian public health care payer. Both costs and health outcomes were discounted at an annual rate of 1.5%.
Model Structure
The sponsor submitted a partitioned survival model, including 3 health states: progression-free, progressive disease, and death (Appendix 3; Figure 1). The modelled cycle length was 1 week. All patients began in the progression-free health state; patients in this state were assumed to be stable or responding to therapy, as defined by the PFS measure assessed in the KEYNOTE-355 trial (Response Evaluation Criteria in Solid Tumours Version 1.1 criteria). During each cycle, patients in the progression-free health state either remained in the state, transitioned to death, or transitioned to the progressive-disease health state. The proportion of patients in the progressive-disease state was calculated by subtracting the proportion of patients alive and progression-free (based on the PFS curve) from the proportion of patients alive (based on the OS curve). Patients in the progressive-disease health state either remained in this state or transitioned to death.
Model Inputs
The modelled patient cohort comprised adult patients with mTNBC whose baseline characteristics mainly reflected the pivotal KEYNOTE-355 PD-L1 (CPS ≥ 10) pivotal trial.2 The median age of patients in the model was 52.7 years, with a mean weight of 71.0 kg, and a body surface area of 1.80 m2.
Key clinical efficacy inputs (OS and PFS) and time on treatment (TOT) for pembrolizumab in combination with chemotherapy and chemotherapy alone were derived from the KEYNOTE-355 trial (data cut-off was June 15, 2021). PFS, OS, and TOT outcomes were extrapolated beyond the trial duration by fitting parametric survival models to the trial data (maximum duration of follow-up: approximately 4 years). Model selection was based on statistical fit (Akaike information criterion, Bayesian information criterion, and visual inspection of goodness of fit to observed data), clinical plausibility, and external validation against real-world data. The sponsor selected a log-normal distribution to extrapolate the OS of patients on pembrolizumab plus chemotherapy and a log-logistic distribution for chemotherapy alone. For long-term extrapolations of PFS, Kaplan-Meier data were used for the first 9 weeks and log-logistic distributions were selected for both treatments considered in the model for the remainder of the time horizon. The plausibility of extrapolated PFS benefit was cross-validated with the OS extrapolations, with PFS capped at OS. Further, OS was capped using general-population mortality rates. The sponsor assumed that the efficacy of pembrolizumab persisted for the entire time horizon. The sponsor fitted gamma and log-logistic distributions to extrapolate TOT curves for pembrolizumab in combination with chemotherapy and chemotherapy alone, respectively, based on treatment-discontinuation data from the pivotal KEYNOTE-355 trial.
The sponsor assumed in its base case that health utility did not differ by health state or treatment. Instead, the sponsor employed a time-to-death approach for estimating utilities, which reflected the decline in the quality of life for patients with advanced or metastatic cancer as they approach death. Utilities were obtained from the KEYNOTE-355 trial, and pooled estimates from both the pembrolizumab plus chemotherapy and chemotherapy groups were used in the model. Key time points at which the utility decreased were more than 360 days, 180 to 360 days, 90 to 180 days, 30 to 90 days, and less than 30 days to death.3 The sponsor considered health state–based utilities in a scenario analysis.
The model included costs related to drug acquisition, administration, monitoring, diagnostic PD-L1 testing, and terminal care. The cost of PD-L1 testing was included in estimating the treatment cost of immunotherapy. The cost was applied in the model as a function of PD-L1 positive (CPS ≥ 10) prevalence rate (38%) and cost per test ($105), obtained from the KEYNOTE-355 trial and published literature.2,4 Drug acquisition costs were applied in the model based on the aforementioned TOT curves. Drug costs of pembrolizumab were capped at 2 years (104 weeks), whereas no cap was applied to the chemotherapy treatment options. Costs associated with chemotherapy were based on the distribution observed in the KEYNOTE-355 trial (pembrolizumab in combination with chemotherapy: ||||||||||||% gemcitabine plus carboplatin, ||||||||||||% nab-paclitaxel, and ||||||||||||% paclitaxel; chemotherapy alone: 54.37% gemcitabine plus carboplatin, 34.95% nab-paclitaxel, and 10.68% paclitaxel). Unit costs were obtained from the CADTH pan-Canadian Oncology Drug Review Expert Review Committee final economic guidance reports and dosing schedules from the KEYNOTE-355 trial and FDA prescribing information.2,5-8, A weekly disease-management cost was applied based on progression status for preprogression ($217) and postprogression ($531) health states, and a 1-time terminal-care cost was also applied at the end of life.9 Disease-management costs by time to death were considered in a scenario analysis.10 Patients were assumed to accrue the cost of subsequent treatments after disease progression, which included second-line treatments (capecitabine, cyclophosphamide plus doxorubicin, gemcitabine plus carboplatin, eribulin, and paclitaxel), third-line treatments (capecitabine, eribulin, capecitabine plus vinorelbine, cyclophosphamide plus doxorubicin, and paclitaxel) and fourth-line treatment (vinorelbine, capecitabine, eribulin, carboplatin, and nab-paclitaxel). These costs were estimated based on the distribution of treatments and mean treatment duration in the KEYNOTE-355 trial and incorporated as a 1-time cost for patients in the progressed health state.
The sponsor’s model included the costs associated with an adverse event of grade 3 or higher that had an incidence rate of 5% or more in 1 or more treatment group in the KEYNOTE-355 trial. Adverse events were assumed to occur during the first treatment cycle only. The costs of managing adverse events were obtained from published literature and the KEYNOTE-355 trial.5,11-13 Disutilities related to adverse events were not included in the sponsor’s base case.
Summary of Sponsor’s Economic Evaluation Results
All analyses were run probabilistically (2,500 iterations for the base-case and scenario analyses). The deterministic and probabilistic results were similar. The probabilistic findings are presented in the following section. Additional results from the sponsor’s submitted economic evaluation base case are presented in Appendix 3.
Base-Case Results
In the sponsor’s base-case analysis, pembrolizumab in combination with chemotherapy was associated with an incremental cost of $124,946 and 0.71 additional QALYs compared with chemotherapy over the lifetime horizon, resulting in an ICER of $175,414 per QALY (Table 3). Pembrolizumab in combination with chemotherapy had a 0% probability of being the most cost-effective strategy at a willingness-to-pay threshold of $50,000 per QALY. More than half (58%) of incremental QALYs associated with pembrolizumab plus chemotherapy compared with chemotherapy alone accrued beyond the trial follow-up period and were based on the sponsor’s extrapolation of trial data.
Table 3: Summary of the Sponsor’s Economic Evaluation Results
Drug | Total costs ($) | Incremental costs ($) | Total QALYs | Incremental QALYs | ICER vs. reference ($ per QALY) |
|---|---|---|---|---|---|
Chemotherapy | $117,445 | Reference | 1.66 | Reference | Reference |
Pembrolizumab plus chemotherapy | $242,390 | $124,946 | 2.37 | 0.71 | $175,414 |
ICER = incremental cost-effectiveness ratio; QALY = quality-adjusted life-year.
Note: Chemotherapy includes gemcitabine plus carboplatin, nab-paclitaxel, and paclitaxel.
Source: Sponsor’s pharmacoeconomic submission.14
Sensitivity and Scenario Analysis Results
The sponsor provided scenario analyses exploring the impact of adopting alternative time horizons, alternative methods of incorporating health utilities, assuming no vial sharing and including indirect costs. Pembrolizumab was not cost-effective in any of these scenario analyses, and conclusions remained robust to alternative inputs and assumptions. The cost-effectiveness results were most sensitive to applying disease-management costs by death, assuming 100% RDI and applying a treatment-waning effect.
CADTH Appraisal of the Sponsor’s Economic Evaluation
CADTH identified several key limitations to the sponsor’s analysis that have notable implications on the economic analysis:
The long-term comparative efficacy of pembrolizumab is uncertain: The sponsor submitted a partitioned survival model in which the long-term clinical efficacy of pembrolizumab is based on the sponsor’s extrapolations of PFS and OS using efficacy data from the KEYNOTE-355 trial. In the intention-to-treat analysis, the median OS and PFS improved by 6.9 months and 4.1 months, respectively, for patients with a PD-L1 CPS of 10 or higher who were treated with pembrolizumab plus chemotherapy compared with those treated with chemotherapy alone. In the pharmacoeconomic analysis, the long-term extrapolation of OS and PFS resulted in an incremental gain of 10.92 months and approximately 13.51 months, respectively. Approximately 58% of QALYs derived from pembrolizumab treatment accrued after the trial duration and, as a result, represent an outcome of modelling instead of real-world data. The results of this cost-effectiveness analysis are sensitive to the sponsor’s extrapolation assumptions, which were based on a limited sample size and a high rate of censoring near the end of the trial. This adds uncertainty in the long term clinical efficacy of pembrolizumab treatment.
In the absence of a direct head-to-head comparison, the sponsor submitted a network meta-analysis (NMA) for comparators (docetaxel, carboplatin, nab-paclitaxel plus carboplatin, and nab-paclitaxel plus gemcitabine) that did not provide strong clinical evidence on comparable clinical efficacy between pembrolizumab and these comparators. The CADTH appraisal of the NMA identified several limitations, including sparse data, uncontrolled heterogeneity, and a small number of trials. Both internal and external validity were questionable. As such, the comparative clinical efficacy and cost-effectiveness of pembrolizumab and these comparators is highly uncertain. As the clinical experts consulted for this review noted these treatments are not commonly used in Canadian clinical practice, CADTH focused its review on the comparators considered in the KEYNOTE-355 trial.
In scenario analyses, CADTH explored the impact of different assumptions on the duration of treatment effect of pembrolizumab plus chemotherapy compared with chemotherapy alone. These scenarios included assuming no treatment effect after the trial period and a treatment-waning effect beginning at the end of trial follow-up over 4 years.
Limitations are associated with the sponsor’s chosen approach to model utilities and costs: In the sponsor’s base case, health utilities were applied based on a patient’s proximity to death, whereas disease-management costs were applied based on progression status. The CADTH guidelines recommend a health state–based approach to modelling utilities,15 and there are a few concerns with the sponsor’s approach. The sponsor modelled a decline in health utility at certain time points from death (≥ 360 days, 180 to 360 days, 90 to 180 days, 30 to 90 days, and < 30 days). Whether the selected time points represent the time points at which health utility declines for patients with mTNBC and how these declines align with changes in health status, such as disease progression or changes in treatment, is an area of uncertainty. The sponsor’s approach assumed that patients who have progressed experience the same health utility as patients who have not progressed. Additionally, the modelling approach should be consistent with regard to the manner in which costs and benefits are measured, and, in the sponsor’s base case, disease-management costs and the primary measure of utility were not aligned. Furthermore, the sponsor did not include disutilities of adverse events; however, the cost of treating adverse events was considered. It is unclear whether patients experience a decline in health utility due to adverse events and how these declines are linked with costs in the sponsor’s model. The sponsor’s approach to selecting health-state utilities had a limited impact on the results; however, the approach to disease-management costs influence the ICER.
In the CADTH reanalysis, both utilities and disease-management costs were based on progression status. CADTH explored the impact of modelling utilities and disease-management costs based on a patient’s proximity to death in a scenario analysis.
The use of RDI may not estimate actual drug costs: The sponsor’s base case reduced doses for pembrolizumab and chemotherapy drugs using RDI data obtained from the KEYNOTE-355 trial. Consistent with previous reviews, and given the inability to link reduced dose intensity with outcomes, the CADTH base case does not incorporate RDIs. The use of RDIs reduces dosage; however, this approach is problematic as dose delays, missed doses, dose reductions to manage toxicity, and subsequent dose re-escalation have differing impacts on drug costs.
In the CADTH reanalysis, an RDI of 100% was assumed for pembrolizumab and all comparators. CADTH explored the impact of assuming sponsor’s adopted RDIs on the CADTH base case in a scenario analysis.
The distribution of chemotherapy drugs is not reflective of clinical practice in Canada: In its base case, the sponsor estimated the costs associated with chemotherapy, in combination with pembrolizumab and alone, based on the distribution of drugs observed in the KEYNOTE-355 trial. In the trial, pembrolizumab was administered in combination with gemcitabine plus carboplatin in 57.08% of the patients, nab-paclitaxel in 27.85% of the patients, and paclitaxel in 15.7% of the patients. In the control group, the proportions of patients administered gemcitabine plus carboplatin, nab-paclitaxel, and paclitaxel were 54.37%, 34.95% and 10.68%, respectively. These distributions of chemotherapy drugs were not aligned with clinical practice in Canada, according to expert feedback obtained by CADTH; paclitaxel is used in nearly half of patients, whereas the other drugs are each used in a quarter of eligible patients. Expert feedback obtained by CADTH also indicated the use of pembrolizumab would not alter this distribution.
The clinical experts consulted by CADTH considered the chemotherapy drugs used in the trial to be interchangeable and the sponsor’s combined approach in the base case to be appropriate. However, the experts did note the existence of a signal when stratified analyses of PFS and OS were considered based on the chemotherapy received.
In the CADTH reanalysis, the proportions of patients administered gemcitabine plus carboplatin, nab-paclitaxel, and paclitaxel were revised to 25%, 25%, and 50%, respectively. In a scenario analysis, CADTH explored the cost-effectiveness of pembrolizumab in combination with and in comparison to each individual chemotherapy drug from the trial.
Weight-based dosing and extended dosing intervals for pembrolizumab are missing: Pembrolizumab dosing in the KEYNOTE-355 trial was a fixed dose of 200 mg administered intravenously every 3 weeks or 400 mg every 6 weeks. Input from participating public drug plans indicated that jurisdictions would likely implement a weight-based dose for pembrolizumab of 2 mg/kg (up to a cap of 200 mg) every 3 weeks with the possibility of extending dosing intervals to every 6 weeks (4 mg/kg up to a 400 mg cap). The clinical experts noted pembrolizumab dosing in clinical practice would follow the dosing strategy implemented by public drug plans. However, extending dosing intervals to every 6 weeks reduces resource use such as chair and nursing time, and would be more likely used in clinical practice. CADTH notes that weight-based dosing will reduce the ICER associated with pembrolizumab and give greater flexibility in dosing. However, CADTH notes that it is not possible to make the direct assumption that the use of weight-based dosing or extending dosing intervals will lead to the same outcomes as the trial’s fixed dose, as patients will be exposed to a lower dose which may impact treatment efficacy.
No changes were made to the sponsor’s base case. In a scenario analysis, CADTH explored the impact of implementing weight-based dosing. However, in the pharmacoeconomic model, the sponsor did not include an option to assess the effects of extending the dosing interval for pembrolizumab and as such, CADTH was unable to explore this option further.
Additionally, the following key assumptions were made by the sponsor and have been appraised by CADTH (Table 4).
Table 4: Key Assumptions of the Submitted Economic Evaluation (Not Noted as Limitations to the Submission)
Sponsor’s key assumption | CADTH comment |
|---|---|
Subsequent therapy | Uncertain. A higher proportion of patients received second-line therapy in the pembrolizumab group compared with chemotherapy alone. The cost of subsequent treatments was higher for patients in the pembrolizumab group compared with chemotherapy alone. This uncertainty may have minimal impact on the results. |
Percentage hospitalized for adverse events | Uncertain. The sponsor applied pooled hospitalization rates from both trial groups in the pharmacoeconomic model. The incidence of common adverse events in the KEYNOTE-355 trial were similar between the 2 treatment groups. However, the incidence of hypothyroidism was greater in the pembrolizumab plus chemotherapy group (15.8%) compared to the placebo plus chemotherapy group (3.2%). This uncertainty may have minimal impacts on the results. |
Drug wastage | Uncertain. The sponsor assumed some vial sharing, with 50% of the vial wasted when vial sharing is allowed. Vial sharing is common in large centres; however, there are no data on the percentage of excess drugs wasted when vial sharing is allowed. As such, the sponsor’s assumption regarding 50% drug wastage when vial sharing is allowed is uncertain. Assuming vial sharing with 0% drug wastage had minimal impact on the results. |
CADTH Reanalyses of the Economic Evaluation
Base-Case Results
The CADTH base case was derived by making changes in model parameter values and assumptions, in consultation with clinical experts. CADTH’s base case adopted health state–based utilities and assumed 100% RDI for pembrolizumab and comparators. CADTH also revised the distribution of chemotherapy drugs to align with clinical practice in Canada.
Table 5: CADTH Revisions to the Submitted Economic Evaluation
Stepped analysis | Sponsor’s value or assumption | CADTH value or assumption |
|---|---|---|
Corrections to sponsor’s base case | ||
None. | — | — |
Changes to derive the CADTH base case | ||
1. Utilities | Time to death–based approach | Health state–based approach |
2. Relative dose intensity | < 100% (varies by drug) | 100% |
3. Distribution of chemotherapy drugs | Pembrolizumab plus chemotherapy:
Chemotherapy:
| Pembrolizumab plus chemotherapy:
Chemotherapy:
|
CADTH base case | — | 1 + 2 + 3 |
In the CADTH base case, pembrolizumab plus chemotherapy was associated with estimated total costs of $275,583 and 2.31 QALYs, compared with total costs of $133,490 and 1.59 QALYs for patients receiving chemotherapy alone. The ICER associated with pembrolizumab plus chemotherapy compared with chemotherapy alone was $198,317 per QALY for the adult patients with locally recurrent inoperable or metastatic TNBC whose tumours expressed PD-L1 (CPS ≥ 10) and who have not received chemotherapy for recurrent inoperable or metastatic TNBC. The probability of cost-effectiveness at a willingness-to-pay threshold of $50,000 per QALY was 0%. More than half (58%) of incremental QALYs associated with pembrolizumab plus chemotherapy compared with chemotherapy alone accrued beyond the trial follow-up period and were based on the sponsor’s extrapolation of trial data. Results of the stepped reanalysis are available in Table 6, with full disaggregated results available in Appendix 4, Table 10.
Table 6: Summary of the Stepped Analysis of the CADTH Reanalysis Results
Stepped analysis | Drug | Total costs ($) | Total QALYs | ICER ($ per QALY) |
|---|---|---|---|---|
Sponsor’s base case (probabilistic) | Chemotherapya | 117,445 | 1.66 | Reference |
Pembrolizumab plus chemotherapy | 242,390 | 2.37 | 175,414 | |
CADTH reanalysis 1 | Chemotherapya | 117,217 | 1.58 | Reference |
Pembrolizumab plus chemotherapy | 241,554 | 2.30 | 173,327 | |
CADTH reanalysis 2 | Chemotherapya | 122,250 | 1.64 | Reference |
Pembrolizumab plus chemotherapy | 261,389 | 2.36 | 194,479 | |
CADTH reanalysis 3 | Chemotherapya | 127,170 | 1.64 | Reference |
Pembrolizumab plus chemotherapy | 253,169 | 2.36 | 176,113 | |
CADTH base case (1 + 2 + 3, probabilistic) | Chemotherapya | 133,490 | 1.59 | Reference |
Pembrolizumab plus chemotherapy | 275,583 | 2.31 | 198,317 |
ICER = incremental cost-effectiveness ratio; QALY = quality-adjusted life-year.
Note: All stepped analyses were conducted deterministically.
aReference product is the least costly alternative.
Scenario Analysis Results
A series of scenario analyses were conducted on CADTH’s base case. These analyses explored the impact of altering the following model parameters and assumptions: estimating health-state utilities and disease-management costs according to proximity to death; including RDIs as in the sponsor’s base case; assuming no treatment effect after the trial period (at 4 years); assuming a delayed treatment-waning effect (gradual decrease in treatment effect from 4 years to 8 years); adopting weight-based dosing for pembrolizumab; and considering the cost-effectiveness of pembrolizumab in combination with and in comparison to each individual chemotherapy drug from the trial.
Results from scenario analyses (Appendix 4, Table 11) demonstrated that the cost-effectiveness findings were sensitive to treatment-waning assumptions and the approach used to estimate costs and QALYs. When treatment-waning was considered, the ICER increased to $285,155 per QALY when treatment was assumed to wane gradually (scenario 4, delayed treatment-waning) and to $364,253 per QALY when treatment was assumed to wane immediately at the end of trial follow-up (scenario 3, immediate treatment-waning). In these scenarios, approximately 17% to 38% of incremental QALYs associated with pembrolizumab plus chemotherapy compared with chemotherapy alone accrued beyond the trial follow-up period via extrapolation. The ICER was also influenced by the approach used to estimate health-utility values and disease-management costs, with the ICER increasing to $273,252 per QALY when adopting a proximal time-to-death approach. When considering paclitaxel as the chemotherapy drug, the ICER associated with pembrolizumab plus paclitaxel compared with paclitaxel alone was the lowest of the available stratified comparisons ($131,648 per QALY) but still not cost-effective.
CADTH undertook a price-reduction analysis based on the sponsor’s base case and the CADTH’s base case (Figure 1). The results show that a price reduction of 81% is required for pembrolizumab plus chemotherapy to be considered cost-effective at a willingness-to-pay threshold of $50,000 per QALY when considering the CADTH base case. The price reduction required decreases to 77% when considering pembrolizumab at a weight-based dose.
Table 7: CADTH Price-Reduction Analyses
Analysis | ICERs for pembrolizumab plus chemotherapy vs. chemotherapy ($ per QALY) | |
|---|---|---|
Price reduction | Sponsor base case | CADTH reanalysis |
No price reduction | 175,414 | 198,317 |
10% | 157,358 | 178,967 |
20% | 140,818 | 160,827 |
30% | 124,278 | 142,688 |
40% | 107,738 | 124,549 |
50% | 91,199 | 106,409 |
60% | 74,659 | 88,270 |
70% | 58,119 | 70,131 |
80% | 41,579 | 51,992 |
81.1% | 39,737 | 50,000 |
ICER = incremental cost-effectiveness ratio; QALY = quality-adjusted life-year.
Issues for Consideration
Based on drug plan feedback, accompanying PD-L1 CPS testing for breast cancer needs to be operationalized and funded to identify the patients eligible for treatment with pembrolizumab. Testing costs were included in the CADTH base case and had minimal impact on the results.
The submitted economic model did not include an option to assess extending the dosing interval for pembrolizumab from 3 weeks to 6 weeks. The clinical experts consulted by CADTH for this review noted that an extended dosing interval for pembrolizumab may be preferred in clinical practice. The impact of extending the dosing interval to every 6 weeks on the cost-effectiveness of pembrolizumab in this population is likely negligible.
Overall Conclusions
The CADTH clinical review found that, compared with chemotherapy (1 of nab-paclitaxel, paclitaxel, or gemcitabine plus carboplatin), the addition of pembrolizumab was associated with a statistically and clinically significant improvement in OS and PFS of patients with locally recurrent inoperable or metastatic TNBC whose tumours expressed PD-L1 (CPS ≥ 10), based on the KEYNOTE-355 study. The long-term clinical effectiveness of pembrolizumab beyond the trial period (4 years) is uncertain. The clinical review also found no significant difference in HRQoL outcomes between the pembrolizumab and chemotherapy groups in the KEYNOTE-355 trial. However, the analyses of HRQoL were collected over a short duration of follow-up (15 weeks).
In the absence of direct head-to-head comparison, the sponsor submitted an NMA for other comparators (docetaxel, carboplatin, nab-paclitaxel plus carboplatin, and nab-paclitaxel plus gemcitabine) that did not provide strong clinical evidence on comparable clinical efficacy between pembrolizumab and these comparators due to limitations identified with the NMA. The clinical experts consulted for this review noted these treatments are not commonly used in Canadian clinical practice. As such, CADTH focused its review on the comparators considered in the KEYNOTE-355 trial for which there was direct comparative evidence.
CADTH undertook a reanalysis that reweighted the distribution of chemotherapy drugs to align with Canadian clinical practice, assumed an RDI of 100% for all treatments, and modelled health utilities based on disease progression status in alignment with the manner in which disease-management costs were captured. CADTH’s base case was aligned with the sponsor’s results such that both analyses suggested that pembrolizumab plus chemotherapy was associated with higher costs and improved QALYs but was not cost-effective at a willingness-to-pay threshold of $50,000 per QALY. Based on publicly available list prices for all comparators, a price reduction for pembrolizumab of at least 81% would be required for it to be cost-effective in combination with chemotherapy at this threshold.
This estimate is sensitive to assumptions about the long-term comparative effectiveness of pembrolizumab plus chemotherapy and the manner in which health utilities and disease-management costs are captured. The ICER increased drastically when the treatment effect was assumed to wane and a time-to-death approach was taken to model utilities and disease-management costs, indicating a larger price reduction may be warranted given the uncertainty with the assumptions used in the CADTH base case.
References
1.Keytruda (pembrolizumab): solution for infusion 100 mg/4 mL vial; Antineoplastic agent, monoclonal antibody [product monograph]. Kirkland (QC): Merck Canada Inc.; 2021 Nov 19.
2.Clinical Study Report: P355V03MK3475. A randomized, double-blind, phase iii study of pembrolizumab (MK-3475) plus chemotherapy vs placebo plus chemotherapy for previously untreated locally recurrent inoperable or metastatic triple negative breast cancer – (KEYNOTE-355) [internal sponsor's report]. Rahway (NJ): Merck Sharp & Dohme Corp.; 2021 Sep 13.
3.Hatswell AJ, Pennington B, Pericleous L, Rowen D, Lebmeier M, Lee D. Patient-reported utilities in advanced or metastatic melanoma, including analysis of utilities by time to death. Health Qual Life Outcomes. 2014;12:140. PubMed
4.Répertoire québécois et système de mesure des procédures de biologie médicale 2021-2022: les annexes. Québec (QC): Ministère de la Santé et des Services Sociaux; 2021: https://publications.msss.gouv.qc.ca/msss/fichiers/2020/20-922-05W.pdf. Accessed 2022 Jun 20.
5.Drug Reimbursement Review sponsor submission: Keytruda (pembrolizumab), 100 mg/4 mL vial; solution for infusion [internal sponsor's package]. Kirkland (QC): Merck Canada Inc.; 2022 Jun 20.
6.CADTH pan-Canadian Oncology Drug Review final economic guidance report: daratumumab (Darzalex) + VMP for multiple myeloma. Ottawa (ON): CADTH; 2019 Aug 29: https://www.cadth.ca/sites/default/files/pcodr/Reviews2019/10148Daratumumab%2BVMPforMM_fnEGR_NOREDACT-ABBREV_Post_29Aug2019_final.pdf. Accessed 2022 Jun 20.
7.CADTH pan-Canadian Oncology Drug Review final economic guidance report: panitumumab (Vectibix) for left sided metastatic colorectal cancer. 2018 Mar 29; https://www.cadth.ca/sites/default/files/pcodr/pcodr_panitumumab_vectibix_ls_mcrc_fn_egr%20.pdf. Accessed 2022 Jun 20.
8.Reaume MN, Leighl NB, Mittmann N, et al. Economic analysis of a randomized phase III trial of gemcitabine plus vinorelbine compared with cisplatin plus vinorelbine or cisplatin plus gemcitabine for advanced non-small-cell lung cancer (Italian GEMVIN3/NCIC CTG BR14 trial). Lung Cancer. 2013;82(1):115-120. PubMed
9.Beauchemin C, Letarte N, Mathurin K, Yelle L, Lachaine J. A global economic model to assess the cost-effectiveness of new treatments for advanced breast cancer in Canada. J Med Econ. 2016;19(6):619-629. PubMed
10.Sieluk J HA, Huang M, Yang L, K H. Early triple-negative breast cancer in women aged >65: retrospective study of outcomes, resource use and costs, 2010-2016. Future Oncology. 2020;17(9). PubMed
11.Schedule of benefits for physician services under the Health Insurance Act: effective October 1, 2021. Toronto (ON): Ontario Ministry of Health; 2022: https://www.health.gov.on.ca/en/pro/programs/ohip/sob/physserv/sob_master.pdf. Accessed 2022 Jun 20.
12.Ontario Case Costing Initiative (OCCI). Toronto (ON): Ontario Health and Long-Term Care; 2017: https://data.ontario.ca/dataset/ontario-case-costing-initiative-occi. Accessed 2022 Jun 20.
13.Dranitsaris G, Maroun J, Shah A. Severe chemotherapy-induced diarrhea in patients with colorectal cancer: a cost of illness analysis. Support Care Cancer. 2005;13(5):318-324. PubMed
14.Pharmacoeconomic evaluation [internal sponsor's report]. In: Drug Reimbursement Review sponsor submission: Keytruda (pembrolizumab), 100 mg/4 mL vial; solution for infusion [internal sponsor's package]. Kirkland (QC): Merck Canada Inc. 2022 Jun 20.
15.Guidelines for the economic evaluation of health technologies: Canada. 4th ed. Ottawa (ON): CADTH; 2017: https://www.cadth.ca/guidelines-economic-evaluation-health-technologies-canada-4th-edition. Accessed 2022 Oct 18.
16.DeltaPA. [Ottawa (ON)]: IQVIA; 2022: https://www.iqvia.com/. Accessed 2022 Aug 22.
17.Budget Impact Analysis [internal sponsor's report]. In: Drug Reimbursement Review sponsor submission: Keytruda (pembrolizumab), 100 mg/4 mL vial; solution for infusion [internal sponsor's package]. Kirkland (QC): Merck Canada Inc. 2022 Jun 20.
18.Brenner DR, Weir HK, Demers AA, et al. Projected estimates of cancer in Canada in 2020. CMAJ. 2020;192(9):E199-E205. PubMed
19.Brezden-Masley C, Fathers KE, Coombes ME, Pourmirza B, Xue C, Jerzak KJ. A population-based comparison of treatment patterns, resource utilization, and costs by cancer stage for Ontario patients with triple-negative breast cancer. Cancer Med. 2020;9(20):7548-7557. PubMed
20.Canadian Cancer Statistics Advisory Committee. Canadian cancer statistics 2021. Toronto (ON): Canadian Cancer Society; 2021: https://cdn.cancer.ca/-/media/files/research/cancer-statistics/2021-statistics/2021-pdf-en-final.pdf. Accessed 2022 Aug 30.
21.Canadian Partnership Against Cancer. Breast cancer control in Canada. A system performance special focus report. 2012; https://www.partnershipagainstcancer.ca/topics/breast-cancer-control-canada/. Accessed 2022 Aug 30.
22.Colzani E, Johansson AL, Liljegren A, et al. Time-dependent risk of developing distant metastasis in breast cancer patients according to treatment, age and tumour characteristics. Br J Cancer. 2014;110(5):1378-1384. PubMed
23.Canadian Cancer Statistics Advisory Committee. Canadian cancer statistics 2019. Toronto (ON): Canadian Cancer Society; 2019: https://cdn.cancer.ca/-/media/files/research/cancer-statistics/2019-statistics/canadian-cancer-statistics-2019-en.pdf. Accessed 2021 Nov 21.
24.Non-Isured Health Benefits. First Nations and Inuit Health Branch. Drug Benefit List September 2020. Ottawa (ON): Indigenous Services Canada; 2020: https://www.sac-isc.gc.ca/DAM/DAM-ISC-SAC/DAM-HLTH/STAGING/texte-text/nihb_benefits-services_drugs_dbl-index_1573154657223_eng.pdf. Accessed 2022 Jun 20.
25.CADTH Reimbursement Review: pembrolizumab (Keytruda) final clinical and pharmacoeconomic review. Ottawa (ON): CADTH; 2021: https://www.cadth.ca/sites/default/files/DRR/2021/PC0236%20Keytruda-combined-report.pdf. Accessed 2022 Jun 20.
26.CADTH Reimbursement Review: sacituzumab govitecan (Trodelvy) final clinical and pharmacoeconomic review. Ottawa (ON): CADTH; 2022: https://www.cadth.ca/sites/default/files/DRR/2022/PC0254-Trodelvy-CombinedReport.pdf. Accessed 2022 Jun 20.
27.CADTH pan-Canadian Oncology Drug Review. Initial economic guidance report: pertuzumab-trastuzumab for early breast cancer. Ottawa (ON): CADTH; 2018: https://www.cadth.ca/sites/default/files/pcodr/pcodr_pertuzumab-trastuzumab_perjeta-herceptin-combo_ebc_in_egr.pdf. Accessed 2022 Jun 20.
28.INESSS. Keytruda. Cancer de l'oesophage ou de la jonction gastro-oesophagienne: avis transmis au ministre en janvier 2022 https://www.inesss.qc.ca/fileadmin/doc/INESSS/Inscription_medicaments/Avis_au_ministre/Mars_2022/Keytruda_2022_01.pdf. Accessed 2022 Jun 20.
29.Répertoire québécois et système de mesure des procédures de biologie médicale; 2021-2022 - Les annexes. Annexe D: valeur pondérée des codes 60040, 60046. Québec (QC): Ministère de la Santé et des Services Sociaux; 2021: https://publications.msss.gouv.qc.ca/msss/fichiers/2020/20-922-05W.pdf. Accessed 2022 Jun 20.
Appendix 1: Cost-Comparison Table
Note that this appendix has not been copy-edited.
The comparators presented in the following table have been deemed to be appropriate based on feedback from clinical expert(s) and drug plan. Comparators may be recommended (appropriate) practice or actual practice. Existing Product Listing Agreements are not reflected in the table and, as such, the table may not represent the actual costs to public drug plans.
Table 8: CADTH Cost-Comparison Table for mTNBC
Treatment | Strength / concentration | Form | Price ($) | Recommended dosage | Average daily cost ($) | Average 28-day cost ($) |
|---|---|---|---|---|---|---|
Pembrolizumab (Keytruda)a | 100 mg/4mL | Vial IV Infusion | 4,400.0000 | 200 mg q.3.w. | 419.05 | 11,733 |
Pembrolizumab + paclitaxel | 611.90 | 17,133 | ||||
Pembrolizumab + nab-paclitaxel | 627.12 | 17,559 | ||||
Pembrolizumab + gemcitabine + carboplatin | 503.81 | 14,107 | ||||
Chemotherapy | ||||||
Carboplatin | 50 mg 150 mg 450 mg 600 mg | IV infusion Vial | 70.0000 210.0000 599.9985 775.0000 | AUC 2 on days 1 and 8, q.3.w. | 33.33 | 933 |
Gemcitabine | 40 mg/mL | 200 mg 1,000 mg 2,000 mg IV infusion Vial | Not availableb 270.0000 540.0000 | 1,000 mg/m2 on days 1 and 8, q.3.w. | 51.43 | 1,440 |
Nab-paclitaxel | 100 mg | IV infusion Vial | 971.000 | 100 mg/m2 on days 1, 8, and 15, q.4.w. | 208.07 | 5,826 |
Paclitaxel | 6 mg/mL | 30 mg 96 mg 150 mg 300 mg IV infusion Vial | 300.0000 1,196.8000 1,870.0000 3,740.0000 | 90 mg/m2 on days 1, 8, and 15, q.4.w. | 192.86 | 5,400 |
Gemcitabine + carboplatin | 84.76 | 2,373 | ||||
AUC = area under the curve; q.3.w. = every 3 weeks; q.4.w. = every 4 weeks; mTNBC = metastatic triple-negative breast cancer.
aPembrolizumab price is based on the sponsor’s submission; dosage is based on the draft product monograph.1,16 Pembrolizumab treatment is capped at 24 months (35 doses of 200 mg or 18 doses of 400 mg).
bOnly expired price was available from IQVIA Delta PA (accessed August 2022).
Note: All prices are from wholesale prices from IQVIA Delta PA (accessed August 2022),16 unless otherwise indicated, and do not include dispensing fees. All cost calculations for drugs with weight- or height-based dosing were calculated using the mean body surface area of 1.8 m2 and mass of 75 kg. Daily and 28-day costs include drug wastage. The recommended dosage was obtained from the KEYNOTE-355 trial. Other chemotherapy drugs and combination therapies such as carboplatin (monotherapy), docetaxel, nab-paclitaxel + carboplatin, and nab-paclitaxel + gemcitabine are not commonly used treatments for mTNBC in first-line setting.
Appendix 2: Submission Quality
Note that this appendix has not been copy-edited.
Description | Yes/no | Comments |
|---|---|---|
Population is relevant, with no critical intervention missing, and no relevant outcome missing. | Yes | No comment. |
Model has been adequately programmed and has sufficient face validity. | No | Refer to CADTH appraisal section regarding uncertainty with approach to modelling health-state costs and utilities. |
Model structure is adequate for decision problem. | Yes | No comment. |
Data incorporation into the model has been done adequately (e.g., parameters for probabilistic analysis). | Yes | No comment. |
Parameter and structural uncertainty were adequately assessed; analyses were adequate to inform the decision problem. | Yes | No comment. |
The submission was well organized and complete; the information was easy to locate (clear and transparent reporting; technical documentation available in enough details). | Yes | No comment. |
Appendix 3: Additional Information on the Submitted Economic Evaluation
Note that this appendix has not been copy-edited.
Appendix 4: Additional Details on the CADTH Reanalyses and Sensitivity Analyses of the Economic Evaluation
Note that this appendix has not been copy-edited.
Detailed Results of CADTH Base Case
Table 10: Disaggregated Summary of CADTH’s Economic Evaluation Results
Parameter | Pembrolizumab plus chemotherapy | Chemotherapy | Incremental |
|---|---|---|---|
Discounted LYs | |||
Total | 3.17 | 2.26 | 0.91 |
Progression-free | 2.17 | 1.05 | 1.13 |
Progressive disease | 1.00 | 1.21 | –0.22 |
Discounted QALYs | |||
Total | 2.30 | 1.58 | 0.72 |
Progression-free | 1.65 | 0.80 | 0.86 |
Progressive disease | 0.64 | 0.78 | –0.14 |
AE disutility | 0.00 | 0.00 | 0.00 |
Discounted costs | |||
Total | $274,788 | $133,266 | $141,522 |
Regimen-related | $183,672 | $49,745 | $133,927 |
Drug acquisition | $181,977 | $48,688 | $133,289 |
Drug administration | $1,420 | $1,058 | $362 |
Testing | $275 | $0 | $275 |
Subsequent therapy | $6,601 | $5,494 | $1,108 |
AE management | $1,958 | $1,642 | $316 |
Disease management (health state–based) | $52,198 | $45,418 | $6,780 |
Terminal care | $30,358 | $30,966 | –$608 |
ICER ($ per QALY) | 197,285 | ||
AE = adverse event; ICER = incremental cost-effectiveness ratio; LY= life-year; QALY = quality-adjusted life-year.
Scenario Analyses
Table 11: Disaggregated Summary of CADTH’s Economic Evaluation Results — Scenario Analyses
Scenario analysis | Drug | Total costs ($) | Total QALYs | ICER ($ per QALY) |
|---|---|---|---|---|
CADTH base case | Chemotherapy | 133,490 | 1.59 | Reference |
Pembrolizumab plus chemotherapy | 275,583 | 2.31 | 198,317 | |
Scenario 1: Adopting utilities and disease-management costs based on a patient’s proximity to death | Chemotherapy | 225,388 | 1.64 | Reference |
Pembrolizumab plus chemotherapy | 420,885 | 2.36 | 273,252 | |
Scenario 2: Assuming sponsor’s adopted RDI | Chemotherapy | 127,170 | 1.58 | Reference |
Pembrolizumab plus chemotherapy | 253,169 | 2.30 | 175,646 | |
Scenario 3: Immediate treatment-waning (at 4 years) | Chemotherapy | 133,266 | 1.58 | Reference |
Pembrolizumab plus chemotherapy | 265,267 | 1.94 | 364,253 | |
Scenario 4: Delayed treatment-waning (gradual decrease in treatment effect from 4 years to 8 years) | Chemotherapy | 133,266 | 1.58 | Reference |
Pembrolizumab plus chemotherapy | 268,864 | 2.06 | 285,155 | |
Scenario 5: Weight-based dosing of pembrolizumab (2 mg/kg every 3 weeks) | Chemotherapy | 133,266 | 1.58 | Reference |
Pembrolizumab plus chemotherapy | 255,315 | 2.30 | 170,139 | |
Scenario 6a: Chemotherapy is paclitaxel | Paclitaxel | 93,604 | 0.92 | Reference |
Pembrolizumab + paclitaxel | 274,788 | 2.30 | 131,648 | |
Scenario 6b: Chemotherapy is nab-paclitaxel | Gemcitabine + nab-paclitaxel | 135,389 | 1.58 | Reference |
Pembrolizumab + nab-paclitaxel | 274,788 | 2.30 | 193,279 | |
Scenario 6c: Chemotherapy is gemcitabine + carboplatin | Gemcitabine + carboplatin | 104,672 | 1.67 | Reference |
Pembrolizumab + gemcitabine + carboplatin | 274,788 | 2.30 | 272,129 |
ICER = incremental cost-effectiveness ratio; QALY = quality-adjusted life-year; RDI = relative dose intensity.
Appendix 5: Submitted Budget Impact Analysis and CADTH Appraisal
Note that this appendix has not been copy-edited.
Table 12: Summary of Key Take-Aways
Key take-aways of the budget impact analysis |
|---|
|
CPS = combined positive score; PD-L1 = programmed cell death 1 ligand 1; RDI = relative-dose intensity; TNBC = triple-negative breast cancer.
Summary of Sponsor’s Budget Impact Analysis
The sponsor submitted a budget impact analysis (BIA) estimating the incremental budget impact of reimbursing pembrolizumab in combination with chemotherapy for use by patients aged 18 years and older with locally recurrent unresectable mTNBC who have not received prior chemotherapy for metastatic disease and whose tumours express PD-L1 (CPS ≥10) as determined by a validated test.17 The BIA was undertaken from the perspective of the Canadian public drug plans over a 3-year time horizon (2023 to 2026), and the sponsor’s pan-Canadian estimates reflect the aggregated results from provincial budgets (excluding Quebec). Key inputs to the BIA are documented in Table 13.
The sponsor estimated the number of eligible patients using an epidemiologic approach with data obtained from various sources including: Canadian Cancer Statistics Reports, Canadian Partnership Against Cancer, and published literature.18-24 The sponsor adopted an average annual growth rate of 2.23% in estimating the total number of breast cancer cases over the time horizon. The eligible population included new patients with breast cancer who develop TNBC and patients at early-stage breast cancer who progressed to metastatic disease. The proportion of new patients diagnosed with metastatic stage cancer (stage IIIC and stage IV) was 7.5%.21 The remaining 92.5% of the population had early-stage breast cancer who progressed to metastatic disease. The sponsor adopted estimates of the proportion of early-stage cases progressing to first distant metastases since time from diagnosis using data from published literature.22 The sponsor assumed that all patients with TNBC were referred to a medical oncologist and, of the referred patients, 90% were treated in order to estimate the number of patients eligible for pembrolizumab treatment.
Costs included drug acquisition costs, testing costs and subsequent treatment costs, which were obtained from IQVIA Delta PA database, pCODR final economic guidance reports and published literature.5,25-29 Accompanying PD-L1 testing is required to identify patients with the indication of interest. In estimating testing costs, the sponsor assumed that PD-L1 testing rate increased from 0% to 85% over a 52-week period based on a linear model and obtained testing cost from the published literature.28,29 To calculate treatment costs, drug costs were multiplied by treatment duration, which was based on Kaplan-Meier time‑on‑treatment (TOT) data from the KEYNOTE-355 (KN-355) pivotal trial.2 Recommended dosage were obtained from the KEYNOTE-355 trial. Drug wastage and administration costs were not included in the base case.
The BIA outcomes were estimated using the number of patients expected to be treated each week, which was modelled to increase over time. The sponsor estimated that pembrolizumab will reach peak market share by 78-weeks based on a linear model and applied market share assumptions to a population unrestricted by PD-L1 CPS status, while also accounting for the proportion of patients expected to be tested for PD-L1 status over time. The model also captured the impact of the pembrolizumab on the number of patients receiving subsequent treatments, which was modelled to be lower in the reimbursement scenario. The sponsor expected pembrolizumab to be added to current standard of care for first-line TNBC. As such, pembrolizumab was not a subsequent treatment option.
Table 13: Summary of Key Model Parameters
Parameter | Sponsor’s estimate (reported as year 1 / year 2 / year 3, if appropriate) |
|---|---|
Target population | |
Annual growth rate | 2.23% |
Incident cases — breast cancer | 22,439 / 22,941 / 23,453 |
Proportion of patients diagnosed with metastatic stage | 7.5% |
Stage IIIC | 3.0% |
Stage IV | 4.5 |
Number of patients diagnosed with metastatic stage | 1,683 / 1,721 / 1,759 |
Prevalent cases — early-stage progressing to metastatic disease | 2,047 / 2,093 / 2,139a |
Number of breast cancer cases — total locally recurrent or metastatic (sum of incidence and prevalent cases) | 3,730 / 3,813 / 3,898 |
Proportion of patients with TNBC | 9.5% |
TNBC — total number of locally recurrent or metastatic | 354 / 362 / 370 |
Referral rate for treatment | 100.0% |
Treatment rate by medical oncologist | 90.0% |
Number of patients with TNBC receiving treatment | 319 / 326 / 333 |
PD-L1 testing rate (at peak) | 85.0% |
Proportion of patients with PD-L1 expression CPS ≥10 | 38.9% |
Number of patients eligible for drug under review with a PD-L1 expression CPS ≥ 10 | 54 / 108 / 110 |
Market uptake (3 years)b | |
Uptake (reference scenario) Paclitaxel Gemcitabine + carboplatin Nab-paclitaxel | 11% / 11% / 11% 54% / 54% / 54% 35% / 35% / 35% |
Uptake (new drug scenario) Pembrolizumab plus chemotherapy Paclitaxel Gemcitabine + carboplatin Nab-paclitaxel | 9% / 24% / 26% 10% / 8% / 8% 49% / 41% / 40% 32% / 26% / 26% |
Cost of treatment (per patient) | |
Cost of treatment per cycle Pembrolizumab plus chemotherapy Paclitaxel Gemcitabine + carboplatin Nab-paclitaxel | $10,227c $4,233 $771 $4,798 |
Cost of subsequent treatment (per patient) | |
Cost of treatment per cycle Capecitabine Cyclophosphamide + doxorubicin Gemcitabine + carboplatin Eribulin Paclitaxel | $192 $1,110 $1,029 $2,127 $3,150 |
Cost of testing (per patient) | |
PD-L1 testing | $105d |
CPS = combined positive score; PD-L1 = programmed cell death 1 ligand 1; TNBC = triple-negative breast cancer.
Note: Cost estimation assumed average weight of 69.70 kg and body surface area of 1.80 m2. Cost was adjusted by relative dose intensities.
aThe proportion of first distant metastasis by time was 1.7% for years 1 and 2, 1.39% for years 3 to 5 and 0.58% for years 6 through 10.22
bThe market share presented are for the eligible population with mTNBC receiving treatment, not restricted by PD-L1 status. In the subpopulation of patients with PD-L1 [CPS] ≥ 10, the market share of pembrolizumab was 80%.
cCost of chemotherapy included 54.37% of gemcitabine + carboplatin, 34.95% of nab-paclitaxel and 10.68% of paclitaxel.2
dPublished literature.28,29
Summary of the Sponsor’s BIA Results
The sponsor estimated the net 3-year budget impact of introducing pembrolizumab in combination with chemotherapy for treatment of patients aged 18 years and older with locally recurrent unresectable or mTNBC, who have not received prior chemotherapy for metastatic disease and whose tumours express PD‐L1 (CPS ≥ 10) to be $18,176,162 (Year 1: $1,261,628; Year 2: $6,427,327; Year 3: $10,487,207).
CADTH Appraisal of the Sponsor’s BIA
CADTH identified several key limitations to the sponsor’s analysis that have notable implications on the results of the BIA:
Use of RDI to estimate actual drug costs is not appropriate: The sponsor’s base case incorporated reduced dose intensities for pembrolizumab and chemotherapy using data from the KEYNOTE-355 trial. The consideration of RDI is problematic as this parameter can be influenced by several factors. The dose received by a patient may differ from the full planned dose of the drug due to dose delays, missed doses, dose reductions to manage toxicity, or subsequent dose re-escalation; each of these have differing impacts on drug costs. The CADTH reanalysis of the CUA assumes 100% RDI, and the BIA and CUA should be aligned.
In the CADTH reanalysis, 100% RDI was assumed. CADTH explored the impact of assuming the sponsor’s adopted RDIs in a scenario analysis.
The weighted cost of chemotherapy, market share of chemotherapy drugs at baseline and market displacement assumptions are not aligned with the expected clinical practice: The sponsor weighted treatment cost of chemotherapy using the proportion of drugs in the KEYNOTE-355 trial. However, the clinical experts consulted for this review noted these proportions do not align clinical practice in Canada. The clinical experts noted that paclitaxel is the commonly used treatment for mTNBC and is funded in most jurisdictions. The sponsor assumed that 54% of market share of pembrolizumab would be captured from gemcitabine + carboplatin, followed by nab-paclitaxel (35%) and paclitaxel (11%). However, the clinical experts noted that if pembrolizumab is reimbursed, the majority of market share of pembrolizumab would be captured from the commonly used treatment, paclitaxel. The market share of chemotherapy drugs was revised to reflect Canadian clinical practice in the CADTH reanalysis of the CUA as well.
In the CADTH reanalysis, the market share and displacement of gemcitabine plus carboplatin, nab-paclitaxel, and paclitaxel were 25%, 25%, and 50%, respectively.
Market share and uptake of pembrolizumab is underestimated: The sponsor assumed a linear increase in the market share of pembrolizumab to a maximum of 80% at 78 weeks for mTNBC patients with PD‐L1 expression and CPS greater than or equal to 10. The clinical experts consulted by CADTH for this review anticipated a rapid uptake of pembrolizumab in this patient group and estimated a maximum market share of 95%. The clinical expects noted that only patients with poor performance status or those who decline treatment would not receive pembrolizumab, if reimbursed, which would represent a small proportion of the eligible population.
In CADTH reanalysis, the market share of pembrolizumab was assumed to increase logarithmically and reach a maximum of 95%.
PD-L1 testing uptake is uncertain and its cost is not relevant to adopted perspective: The sponsor assumed a maximum PD-L1 testing rate of 85% at 52 weeks after pembrolizumab is funded. Although the clinical experts agreed with the sponsor’s assumption, the drug plan input noted that PD-L1 testing should be operationalized and funded for breast cancer before pembrolizumab is used to treat patients. Given that PD-L1 testing is available in current clinical practice and this test is needed to identify patients eligible for pembrolizumab treatment, PD-L1 testing may become a routinely performed test as part of standard practice, and uptake may be higher than anticipated in clinical practice.
Additionally, as the analysis is focused on treatments funded by the drug plans, the cost of PD-L1 testing is not relevant to the drug plan perspective. The PD-L1 testing costs are, however, relevant to the health care payer perspective.
In CADTH reanalysis, PD-L1 testing cost was excluded. CADTH explored the impact of including PD-L1 testing cost and assuming 100% of PD-L1 testing uptake immediately after pembrolizumab is funded in scenario analysis.
Weight-based dosing for pembrolizumab: Pembrolizumab dosing in the KEYNOTE-355 trial used a fixed dose of 200 mg intravenously every 21 days for adult patients. Based on drug plan input, CADTH notes that jurisdictions would likely implement a weight-based dose of 2 mg/kg (up to a cap of 200 mg) every 3 weeks, and clinical experts consulted by CADTH noted the possibility of extending the dosing interval every 6 weeks (4mg/kg up to a 400 mg cap).
In a scenario analysis, CADTH assumed pembrolizumab would be provided using a weight-based dose. The sponsor did not include an option to assess the effects of extending the dosing interval for pembrolizumab and, as such, CADTH was unable to explore this option further.
The budget impact model has limited transparency and flexibility: The sponsor’s submitted BIA model is overly complex, using circular referencing and hard coding which increases validity issues when making changes to the model and ensuring consistency throughout the budget impact model. The derivation of the eligible population is highly uncertain. The sponsor applied market share assumptions to a population unrestricted by PD-L1 CPS status. The model lacks transparency and has limited flexibility to allow the reviewers to assess the impact of changing the sponsor’s base assumptions solely in a population whose tumours express PD‐L1 (CPS ≥10).
CADTH could not address the limitations with the sponsor’s model structure and applied all assumptions to a population unrestricted by PD-L1 CPS status. CADTH notes that the BIA results presented should be treated with a degree of caution, however, the incremental impact is reflective of the population with mTNBC whose tumours express PD‐L1 (CPS ≥10).
CADTH Reanalyses of the BIA
CADTH revised the sponsor’s base case by aligning model inputs with the CUA (adopting RDI of 100%, revising the distribution of chemotherapy drugs to reflect Canadian clinical practice), excluding PD-L1 testing costs, revising market share displacement assumptions, assuming a rapid increase in market share of pembrolizumab, and increasing the market share of pembrolizumab.
Table 14: CADTH Revisions to the Submitted BIA
Stepped analysis | Sponsor’s value or assumption | CADTH value or assumption |
|---|---|---|
Corrections | ||
None. | — | — |
Changes to derive the CADTH base case | ||
1. Relative dose intensity | < 100% (varies by drug) | 100% |
2. Distributions used to estimate weighted cost of chemotherapy and market share of comparators | Pembrolizumab plus chemotherapy:
Chemotherapy:
| Pembrolizumab plus chemotherapy:
Chemotherapy:
|
3. Market share displacement | Market share of pembrolizumab was captured mostly from market share of gemcitabine + carboplatin, followed by nab-paclitaxel and paclitaxel | Market share of pembrolizumab was captured from market share of gemcitabine + carboplatin, nab-paclitaxel, and paclitaxel by 25%, 25% and 50%, respectively |
4. Market share of pembrolizumab in patients with CPS ≥10 | Pembrolizumab has a peak market share of 80% (at week 78) | Pembrolizumab has a peak market share of 95% (at week 78) |
5. Market uptake of pembrolizumab | Linear uptake | Logarithmic uptake (rapid at first and plateaus at 78 weeks) |
6. PD-L1 testing costs | Include | Exclude |
CADTH base case | Reanalysis 1 + 2 + 3 + 4 + 5 + 6 | |
CPS = combined positive score; PD-L1 = programmed cell death 1 ligand 1.
The results of the CADTH stepwise reanalysis are presented in summary format in Table 15 and a more detailed breakdown is presented in Table 16.
Based on the CADTH base case, the budget impact of the reimbursement of pembrolizumab plus chemotherapy for the treatment of adult patients with locally recurrent unresectable or mTNBC expressing PD-L1 (CPS ≥10), who have not received prior chemotherapy, is expected to be $4,346,142 in year 1, $12,528,377 in year 2, and $16,258,217 in year 3, with a 3-year total of $33,132,736.
Table 15: Summary of the CADTH Reanalyses of the Budget Impact Analysis
Stepped analysis | Three-year total |
|---|---|
Submitted base case | $18,176,162 |
CADTH reanalysis 1 | $20,479,223 |
CADTH reanalysis 2 | $20,331,098 |
CADTH reanalysis 3 | $18,259,023 |
CADTH reanalysis 4 | $21,570,430 |
CADTH reanalysis 5 | $22,670,175 |
CADTH reanalysis 6 | $18,102,765 |
CADTH base case | $33,132,736 |
CADTH also conducted additional scenario analyses to address remaining uncertainty, using the CADTH base case:
assuming sponsor’s adopted RDIs
including PD-L1 testing costs
assuming immediate 100% PD-L1 testing rate
weight-based dosing of pembrolizumab
price reduction of pembrolizumab by 81.1%.
In scenarios adopting a weight-based dosing of pembrolizumab and 100% PD-L1 testing rate, the estimated 3-year budget impact increased to $24,867,869 and $38,979,689, respectively. Results are provided in Table 16.
Table 16: Detailed Breakdown of the CADTH Reanalyses of the BIA
Scenario | Drug | Year 0 (current situation) | Year 1 | Year 2 | Year 3 | Three-year total |
|---|---|---|---|---|---|---|
Submitted base case | Reference | $4,063,247 | $7,126,157 | $8,182,501 | $8,731,918 | $24,040,577 |
New drug | $4,063,247 | $8,387,785 | $14,609,827 | $19,219,126 | $42,216,739 | |
Budget impact | $0 | $1,261,628 | $6,427,327 | $10,487,207 | $18,176,162 | |
CADTH base case | Reference | $5,624,197 | $9,220,358 | $10,439,954 | $10,950,730 | $30,611,043 |
New drug | $5,624,197 | $13,566,501 | $22,968,331 | $27,208,947 | $63,743,779 | |
Budget impact | $0 | $4,346,142 | $12,528,377 | $16,258,217 | $33,132,736 | |
CADTH scenario analysis: assuming sponsor’s adopted RDIs | Reference | $4,952,662 | $8,137,513 | $9,212,818 | $9,669,081 | $27,019,411 |
New drug | $4,952,662 | $11,964,130 | $20,246,851 | $23,992,349 | $56,203,330 | |
Budget impact | $0 | $3,826,617 | $11,034,033 | $14,323,269 | $29,183,919 | |
CADTH scenario analysis: including PD-L1 testing costs | Reference | $5,624,197 | $9,220,358 | $10,439,954 | $10,950,730 | $30,611,043 |
New drug | $5,624,197 | $13,581,056 | $22,997,427 | $27,238,692 | $63,817,175 | |
Budget impact | $0 | $4,360,698 | $12,557,472 | $16,287,962 | $33,206,132 | |
CADTH scenario analysis: 100% PD-L1 testing rate | Reference | $5,624,197 | $9,220,358 | $10,439,954 | $10,950,730 | $30,611,043 |
New drug | $5,624,197 | $14,333,467 | $25,179,221 | $30,078,044 | $69,590,732 | |
Budget impact | $0 | $5,113,109 | $14,739,267 | $19,127,314 | $38,979,689 | |
CADTH scenario analysis: weight-based dosing of pembrolizumab | Reference | $5,624,197 | $9,220,358 | $10,439,954 | $10,950,730 | $30,611,043 |
New drug | $5,624,197 | $12,431,123 | $19,847,573 | $23,200,216 | $55,478,912 | |
Budget impact | $0 | $3,210,765 | $9,407,618 | $12,249,485 | $24,867,869 | |
CADTH scenario analysis: pembrolizumab price reduction by 81.1% | Reference | $5,624,197 | $9,220,358 | $10,439,954 | $10,950,730 | $30,611,043 |
New drug | $5,624,197 | $10,527,586 | $14,615,410 | $16,479,306 | $41,622,303 | |
Budget impact | $0 | $1,307,228 | $4,175,455 | $5,528,576 | $11,011,260 |
PD-L1 = programmed cell death 1 ligand 1; RDI = relative dose intensity.
Stakeholder Input
Patient Input
Canadian Breast Cancer Network
About the Canadian Breast Cancer Network
The Canadian Breast Cancer Network (CBCN) is a leading, patient-directed, national health charity committed to ensuring the best quality of care for all Canadians affected by breast cancer through the promotion of information, education and advocacy activities. www.cbcn.ca
As a member of the Canadian Cancer Action Network, the Canadian Breast Cancer Network is committed to adhering to the Code of Conduct Governing Corporate Funding.
Information Gathering
Information for this submission was collected via:
CBCN’s 2017 Lived Experience Breast Cancer Patient Survey: An online survey was distributed in English and French to patients living with breast cancer. No patients surveyed had direct experience with the treatment under review. Survey questions comprised of a combination of scoring options and free form commentary. Patients were contacted through the membership databases of CBCN and other patient organizations.
Patient Respondents Profile
In this submission, CBCN specifically utilizes the data provided by the 14 patients from the survey who identified as being diagnosed with metastatic triple negative breast cancer (mTNBC).
The respondents all identified as female and all spoke English as a first-language. The majority of respondents were from Ontario (6) and British Columbia (2). The rest of the respondents were from New Brunswick (1), Alberta (1), Quebec (1), Nova Scotia (1). Saskatchewan (1) and Newfoundland and Labrador (1).
Most of the respondents (5) were between the ages of 50-59 when they were diagnosed with metastatic breast cancer, 4 respondents were in the 40-49 age range, 3 were between 30-39 years, and 2 were between 60-69 years of age.
All but 1 respondent was in a relationship. 13 of the mTNBC patients had children, with the majority (7) having children 20 years or older. 4 had children between the ages of 13-19, 3 had children 2-5 years of age, and 3 had children between 6-12 years old.
CBCN’s 2012 Metastatic Breast Cancer Patient and Caregiver Survey Report: An online survey, conducted in collaboration with ReThink Breast Cancer, was distributed to patients living with metastatic breast cancer (mBC) and their caregivers. No patients surveyed had experience with the treatment under review. Survey questions comprised of a combination of scoring options and free form commentary. Patients were contacted through the membership databases of CBCN and other patient organizations.
71 patients participated in the survey
16 caregivers participated in the survey
Printed sources: A review was conducted of current studies and grey literature to identify issues and experiences that are commonly shared among many women living with breast cancer.
Disease Experience
Metastatic breast cancer is the spread of cancerous cell growth to areas of the body other than where the cancer first formed, and is often more severe than earlier stages of breast cancer. It is commonly spreads to the bones, but can include the lungs, liver, brain and skin. In our 2017 Lived Experience Breast Cancer Patient Survey (2017 Survey), of the 14 patients who indicated that they are living with mTNBC, the majority of respondents (10) experienced metastases to their lungs. This was followed by metastases to other parts of their bodies (6), their bones (5), their liver (3) and their brain (2).
Current treatment options for metastatic breast cancer are only effective at prolonging progression-free disease, and most cases of advanced disease will progress and symptoms will worsen. Patients with a diagnosis of metastatic breast cancer understand the limitations of current treatment options and seek to live their remaining months and years with the best possible quality of life that they can achieve.
Triple negative breast cancer (TNBC) is an aggressive form of breast cancer whose growth is not driven by estrogen, progesterone, or by the overexpression of HER2 (human proteins epidermal growth factor receptor). While anyone can be diagnosed with triple negative breast cancer, this subtype of breast cancer has been found to be higher in young people, Black and Hispanic women, and those with a BRCA1 mutation. (Triple-Negative Breast Cancer. Breastcancer.org. Accessed June 28, 2021. https://www.breastcancer.org/symptoms/types/triple-negative) Individuals in Canada, and in general, who are diagnosed with TNBC have a poor prognosis and poor survival outcomes. According to the American Cancer Society, the 5-year survival rate is 65% for regional mTNBC and 12% for distant mTNBC. This is compared to the 5-year survival rate for localized TNBC. (Triple-negative Breast Cancer. American Cancer Society. Accessed June 28, 2021. https://www.cancer.org/cancer/breast-cancer/understanding-a-breast-cancer-diagnosis/types-of-breast-cancer/triple-negative.html)
The Physical Impact of Metastatic Breast Cancer
How the disease presents itself through symptoms, how it progresses, and how it is experienced varies by patient, but many effects of metastatic breast cancer represent a significant or debilitating impact on their quality of life. In our 2012 Metastatic Breast Cancer Patient and Caregiver Survey (2012 Survey), patients were asked what impact cancer-related symptoms had on their quality of life:
54% of patients reported that fatigue resulted in a significant or debilitating impact, and 40% reported some or moderate impact;
39% of patients reported that insomnia resulted in a significant or debilitating impact, and 46% reported some or moderate impact;
37% of patients reported that pain resulted in a significant or debilitating impact, and 44% reported some or moderate impact.
These results were further reinforced in our 2017 Survey.
The Social Impact of Metastatic Breast Cancer
The impact of this disease touches all aspects of a patient’s life, restricting an individual’s employment and career, ability to care for children and dependents, and their ability to be social and meaningfully participate in their community. When asked in the 2012 Survey what kind of impact living with metastatic breast cancer has had on their quality of life:
Among those who were employed, 71% of patients identified significant restrictions to their ability to work;
Among those with children or dependents, 21% identified significant restrictions and 53% reported some or moderate restrictions to their caregiving responsibilities;
49% of patients identified significant restrictions and 38% identified some or moderate restrictions to their ability to exercise;
42% of patients identified significant restrictions and 42% identified some or moderate restrictions to their ability to pursue hobbies and personal interests;
41% of patients identified significant restrictions and 41% identified some or moderate restrictions to their ability to participate in social events and activities;
22% of patients identified significant restrictions and 52% identified some or moderate restrictions to their ability to spend time with loved ones.
Other experiences identified by patients included: guilt, the feeling of being a burden on caregivers, fear of death, poor body image, not knowing what functionality will be lost, fear of the impact of cancer and the loss of a parent on children, not knowing what will happen to children, the loss of support of loved ones, as well as marital stress/loss of fidelity and affection from husband.
Experiences With Currently Available Treatments
The Goals of Current Therapy
As with all treatment for metastatic breast cancer, the goal of treatment for metastatic triple negative breast cancer is to control disease progression (extending life) and to manage cancer-related symptoms (extending or stabilizing quality of life). Treatment options for mBC and their effectiveness vary among type of cancer, location of cancer, and how symptoms are experienced.
Patients diagnosed with mTNBC have very limited treatment options. Targeted therapies that treat HR-positive and HER2-positive breast cancers are usually ineffective in treating TNBC. Because of the lack of effective treatment options for mTNBC, patients with this subtype of metastatic breast cancer face much lower overall survival (OS) rates than patients with other subtypes of metastatic breast cancer. Currently, treatment for TNBC is very limited and usually involves chemotherapy, surgery and radiation. In the case of mTNBC however, the standard of care is single-agent chemotherapy. Unfortunately, as the disease continues to progress and treatment stops responding, individuals must move to second- and third-line treatments, making their treatment options even more limited as they require newer lines of treatment. In the treatment of metastatic breast cancer, when a treatment regimen with chemotherapy does not work, a new regimen is used. Each new regimen is called a ‘line’. As more lines of treatment are tried, the likelihood of the cancer to shrink becomes less. If the cancer does shrink, it is a short period of time until a new line is needed, with the time period getting shorter and shorter as more lines are used. (Treatments for Metastatic Breast Cancer. Susan G. Komen. Accessed March 12, 2022. https://www.komen.org/breast-cancer/treatment/by-diagnosis/metastatic/)
While immunotherapy can be helpful as a first-line treatment, single-agent chemotherapy is the standard treatment beyond first-line therapies but it is associated with low response rates (<20%) and short median progression-free survival 2-3 months). (Bardia, A., et al. Sacituzumab Govitecan in Metastatic Triple-Negative Breast Cancer. N Engl J Med. 384, 1529-41 (2021). (2016). https://doi.org/10.1056/NEJMoa2028485) Eribulin is usually used for previously treated mTNBC but its PFS is low (>3 months). (Ibid) In addition to this, chemotherapy in general has a very high toxicity profile and is often associated with significant adverse events.
Among the metastatic triple negative breast cancer patients in our 2017 Survey, all had been or were currently being treated with chemotherapy, 11 patients previously had surgery, 12 patients had or were receiving radiation therapy and 2 patients had or were currently receiving hormone therapy.
Key Factors for Decision-Making Around Treatment
Metastatic breast cancer patients in our 2017 Survey discussed the importance of the following factors in influencing their decision-making around treatments:
Effectiveness of the treatment – how well the treatment stabilized their disease and delayed progression of their disease.
Prolonging life without sacrificing quality of life – being able to maintain productive, active lives with minimal disruption to daily routines.
Side effect management – minimizing risk while stabilizing their disease.
Cost and accessibility of treatments – affordability and ease of accessing treatments.
Treatment Efficacy
When asked how important progression-free survival was in considering treatments, the mTNBC patients in our 2017 Survey revealed that efficacy of the treatment is an important consideration to their decision-making. Of the 13 mTNBC patients who responded to the question:
69% indicated that progression-free survival of less than 3 months was important or very important, and
86% indicated that progression-free survival of 3-5 months was important or very important.
Of all of the 14 mTNBC patients in our 2017 Survey, 85% indicated that progression-free survival of 6 months or longer very important. When asked about overall survival, 85% of all mTNBC patients indicated that overall survival was very important when considering treatment options.
Metastatic breast cancer patients in our 2017 Survey with all types and subtypes of breast cancer also spoke on the importance of treatment effectiveness in their decision-making anecdotally:
“The most important factors for me are progression free survival and quality of life.” – mBC patient respondent
“Anything to prolong my survival and maintain quality of life.” – mBC patient respondent
“Quality of life, efficacy of the drug to stabilize my TNBC” – mTNBC patient respondent
“Survival is of upmost importance to me.” – mBC patient respondent
Quality of Life
Quality of life was routinely cited by patients as an important factor in making treatment decisions. In our 2017 Survey, quality of life was rated as important by 43% of mTNBC patients and very important by 50% of them. More specifically, patients reported on the importance of minimal side effects, mobility, and productivity when making decisions regarding treatment options. Among mTNBC patients in our 2017 Survey:
Minimal side effects was rated as somewhat important by 43% of patients, important by 36% of patients and very important by 14% patients
Productivity was rated as important by somewhat important by 36% of patients and important by 57% patients
Mobility was rated as important by 79% of patients and very important by 14% of patients
This consideration for quality of life was reiterated anecdotally in our 2017 Survey:
“Making sure I have some quality of life so I can [spend] as much time with my kids and family[.] I don't want them to watch me suffer” – mTNBC patient respondent
“Trying to balance the most effective treatment regime with the least impact on my day to day living/quality of life. Maintaining a certain level of independence is important to me.” – mTNBC patient respondent
Patient willingness to tolerate treatment side effects
In our 2012 Metastatic Patient and Caregiver Survey, the responses to what level of side effects and how much impact on one’s quality of life would be worth extending progression-free disease by six months was shown to be determined at the personal level.
When asked to rate how much impact different symptoms of cancer and cancer treatment would be considered tolerable:
Almost two-thirds of patients indicated that when it comes to fatigue, nausea, depression, problems with concentration, memory loss, diarrhea and insomnia, some or a moderate impact on one’s quality of life would be considered acceptable, and approximately one quarter of patients indicated that a strong or debilitating impact would be considered acceptable.
70% of patients indicated that when it comes to pain, some or a moderate impact on one’s quality of life would be considered acceptable, and 27% of patients indicated that a strong or debilitating impact would be considered acceptable.
In our 2017 Survey, we asked metastatic triple negative breast cancer patients about the level of acceptable symptoms in exchange for 6 months or less of benefits from breast cancer treatment. Among those who responded:
Pain was rated as not acceptable by 31% of patients, somewhat acceptable by 62% of patients, and very acceptable by 8% of patients.
Fatigue was rated as somewhat acceptable by 77% of patients and as very acceptable by 23% of patients.
15% of patients rated nausea as not acceptable, 77% rated it as somewhat acceptable, and 8% rated it as very acceptable.
Depression was rated as not acceptable by 31% of patients and somewhat acceptable by 69% of patients.
85% of patients rated lack of concentration as somewhat acceptable, 15% rated it as very acceptable.
Memory loss was rated as not acceptable, somewhat acceptable, and very acceptable by 15%, 69%, and 15% of patients, respectively.
23%, 69%, and 8% of patients rated diarrhea as not acceptable, somewhat acceptable, and very acceptable, respectively.
Insomnia was rated as somewhat acceptable by 92% of patients and very acceptable by 8% of patients.
Vomiting was rated as somewhat acceptable by 77% of patients, somewhat by 15% of patients, and as very acceptable by 8% of patients.
62% and 38% of patients rated hair loss as somewhat acceptable and very acceptable, respectively.
This willingness to tolerate side effects was also reflected on anecdotally by other patients in our 2017 Survey:
“Definitely the balance of quality of life vs side effects with the [effectiveness].” – mTNBC patient respondent
“Mom so just want to live – high tolerance for SE as long as management options provided.” – metastatic HER2-positive breast cancer patient respondent
The financial burden of treating and managing breast cancer
The financial burden associated with living with metastatic breast cancer extends far beyond any loss of income during a temporary or permanent absence from employment. In addition to the loss of income during illness, metastatic breast cancer patients can incur substantial costs associated with treatment and disease management. Research on the financial impact of breast cancer on patients identified the following (Janet Dunbrack, Breast Cancer: Economic Impact and Labour Force Re-entry. Canadian Breast Cancer Network, 2010):
80% of breast cancer patients report a financial impact due to their illness.
44% of patients have used their savings, and 27% have taken on debt to cover costs.
These findings were consistent with the responses in our 2012 Survey:
Nearly one-third of patients indicated that the cost of medication, the cost of alternative treatments (i.e. massage, physiotherapy, etc.) to manage symptoms and side effects, and the time required to travel to treatment had a significant or debilitating impact on their quality of life.
24% of patients indicated that the costs associated with travel had a significant or debilitating impact on their quality of life, and 41% of patients indicated that it had some or moderate impact on their quality of life.
In our 2017 Survey, mTNBC patients reported that their diagnosis had some (57%) or a very large (43%) impact on their finances. In addition to this, 79% of mTNBC respondents indicated that the time required to travel to treatment had some or a significant impact of their quality of life. 71% reported the same in regard to the cost of other treatments (i.e. massage, physiotherapy, etc.) and 79% reported the same in regard to costs associated with travel.
Respondents in our 2017 Survey discussed the financial impacts of a metastatic breast cancer diagnosis:
“Always a concern as you never know if the next drug will be covered or how long it takes to get approval from private coverage. Many times it delays treatment and this weighs on one's mind.” – mTNBC patient respondent
“If my community did not raise the money for my [treatment] I would likely not be here today. When I contacted every group or charity NOONE offered financial assistance for treatment.” – metastatic HER2-positive breast cancer patient respondent
“Many of the next step treatments are very expensive [and not covered by government programs] and it is a HUGE struggle to get [coverage]. […] When dealing with an incurable disease the last thing you want to have to do is spend time on a letter writing campaign to argue about whether or not you should receive the drugs [recommended by your physician]. At about $1500.00 a week, I don't know many who can afford that.” – mBC patient respondent
“I wanted to try [immunotherapy], but it is [$]7500.00 every 3 weeks not covered by private insurance, now will probably have to go on chemo again, and the last ones were very hard on me causing toxicity and having to get blood transfusions.” – mTNBC patient respondent
“Just because I am not in the lowest income bracket does not mean I don't need assistance. I am excluded from all programs I have tried to access.” – mTNBC patient respondent
Other financial barriers that metastatic breast cancer patients mentioned include: not qualifying for insurance at work, inability to change employers due to loss of insurance, and the prohibitive cost of new treatment options.
Patient Access to Local Resources and Supports During Treatment
When living with cancer, many patients experience significant barriers and challenges around availability of health care services and quality childcare in their community. In response to the 2012 Survey questions about the availability of supports such as childcare, transportation and alternative treatments in their community:
Among patients with children or other dependents, 53% indicated that there is minimal or no access to appropriate care for their loved ones when they are experiencing debilitating symptoms related to their cancer, and 40% identified barriers to accessing quality care during cancer treatment.
In our 2017 Survey among mTNBC patients with children at the time of their diagnosis:
7 reported that finding appropriate care for their children/dependents when experiencing side effects of cancer treatments was not accessible
7 indicated that finding appropriate care for their children/dependents during cancer treatment was not accessible
Among all mTNBC patients from our 2017 Survey, 43% indicated that finding symptom management options in or around their community was not accessible and 36% indicated that it was somewhat accessible.
Patient Willingness to Tolerate Risk
When asked in the 2012 Survey about their willingness to tolerate risk with a new treatment:
34% of respondents were willing to accept serious risk with treatment if it would control the disease
45% of respondents were willing to accept some risk with treatment
21% of respondents were very concerned and felt less comfortable with serious risks with treatment
Need for Personal Choice
The open-ended questions and the key informant interviews showed that it is imperative that women with metastatic breast cancer have access to, and the option of what drugs they take. Most patients are well aware of the adverse effects of treatment up front and they want to make a personal choice that works for them. 57% percent of mTNBC patients in our 2017 Survey expressed being very comfortable in treatment decisions.. Metastatic breast cancer patients expressed the need for personal choice and autonomy in our 2012 Survey as well as in the 2017 Survey:
“I think patients (ESPECIALLY young patients) should be given more decision making power in terms of access to radical treatments to control disease. […] With two small [children] I am determined to access any treatment that can extend my life and I hate struggling with doctors for this access.” – 2012 Survey
“I believe that I would prefer to tolerate severe restrictions in the quality of my life, if it meant that I would be able to have a longer period without progression.” – 2012 Survey
“It would be nice to have more choices and more information about them. I was lucky to get on a clinical trial perhaps because my oncologist was a research oncologist and involved in many. While I knew friend and acquaintances that had Stage IV BC and never informed of clinical trials, and sadly several did not survive the disease.” – 2017 Survey mBC patient respondent
“I am frustrated that ALL the treatment choices aren't given to me... I am told what I am taking next with no option or discussion on other options. My oncologist has assured me there are many treatments available, but have never shared which, so I have to turn to Facebook groups for guidance.” – 2017 Survey mTNBC patient respondent
“I wish my doctor would present me with options.” – 2017 Survey mBC breast cancer respondent
“Accessibility to new drugs- not limiting choices.” – 2017 Survey mBC patient respondent
“Complete access to drug treatment choices and trials.” – 2017 Survey mBC patient respondent
Improved Outcomes
For metastatic patients, extension of progression-free survival (PFS) is of critical concern. Like any other treatment for metastatic breast cancer, patients have an expectation that pembrolizumab (Keytruda) will extend their PFS with good quality of life when first-line therapies stop working.
KEYNOTE-355 is a phase III multicentre, randomized, double-blind study . The aim of the study is to examine whether the combination of pembrolizumab and chemotherapy to the treatment of patients with untreated locally recurrent inoperable or metastatic triple-negative breast cancer would increase the anti-tumour activity of chemotherapy . A total of 847 patients were randomly assigned, in a 2:1 ratio, to either receive pembrolizumab every 3 weeks plus chemotherapy (nab-paclitaxel; paclitaxel; or gemcitabine plus carboplatin) (566 patients) or to receive placebo plus chemotherapy (281 patients) (Ibid). Patients were stratified by chemotherapy type (taxane or gemcitabine-carboplatin), PD-L1 status (CPS ≥1 or <1) and prior (neo)adjuvant treatment with same-class chemotherapy.(Rugo, H.S., et al. KEYNOTE-355: Final results from a randomized, double-blind phase III study of first-line pembrolizumab + chemotherapy vs placebo + chemotherapy for metastatic TNBC. Ann of Onc. 32(5). (2021). https://oncologypro.esmo.org/meeting-resources/esmo-congress/keynote-355-final-results-from-a-randomized-double-blind-phase-iii-study-of-first-line-pembrolizumab-chemotherapy-vs-placebo-chemotherapy-for)
Dual primary efficacy endpoints for KEYNOTE-355 were progression-free survival (PFS) and overall survival (OS). These were assessed in patients whose tumours were strongly positive for PD-L1, with a CPS (combined positive score) of 10 or more, patients with a CPS of 1 or more, and in an intention-to treat population (Cortes, J., et al. Pembrolizumab plus chemotherapy versus placebo plus chemotherapy for previously untreated locally recurrent inoperable or metastatic triple-negative breast cancer (KEYNOTE-355): a randomised, placebo-controlled, double-blind, phase 3 clinical trial. The Lancet. 396 (10265), 1817-1828 (2020). https://doi.org/10.1016/S0140-6736(20)32531-9). Overall response rate (ORR) was a secondary endpoint. (Rugo, H.S., et al. KEYNOTE-355: Final results from a randomized, double-blind phase III study of first-line pembrolizumab + chemotherapy vs placebo + chemotherapy for metastatic TNBC. Ann of Onc. 32(5). (2021). https://oncologypro.esmo.org/meeting-resources/esmo-congress/keynote-355-final-results-from-a-randomized-double-blind-phase-iii-study-of-first-line-pembrolizumab-chemotherapy-vs-placebo-chemotherapy-for)
Interim analysis (data cut-off in December 2019) showed a median follow-up of 25.9 months in the pembrolizumab-chemotherapy group and 26.3 in the placebo-chemotherapy group (Cortes, J., et al. Pembrolizumab plus chemotherapy versus placebo plus chemotherapy for previously untreated locally recurrent inoperable or metastatic triple-negative breast cancer (KEYNOTE-355): a randomised, placebo-controlled, double-blind, phase 3 clinical trial. The Lancet. 396 (10265), 1817-1828 (2020). https://doi.org/10.1016/S0140-6736(20)32531-9). Median PFS for the pembrolizumab-chemotherapy group and the control group in the intention-to-treat population was 7.5 and 5.6 months, respectively (Ibid).
Overall, results from KEYNOTE-355 showed that the benefits of adding pembrolizumab to the treatment of patients with TNBC were enhanced based on PD-L1 status (Ibid). For patients with CPS of 10 or more, median PFS was 9.7 months in the pembrolizumab-chemotherapy group and 5.6 months in the placebo-chemotherapy group (Ibid). Median OS in patients with a CPS of 10 or more who were in the treatment group was 23.0 months, for those in the control group, OS was 16.1 months (KEYNOTE-355 Final Analysis Reveals Survival Benefit With Pembrolizumab in Triple-Negative Breast Cancer. The ASCO Post. Accessed June 22, 2022. https://ascopost.com/issues/december-10-2021/keynote-355-final-analysis-reveals-survival-benefit-with-pembrolizumab-in-triple-negative-breast-cancer/). This difference was statistically significant (p = 0.0093) (Ibid). There was a no reported benefit of adding pembrolizumab in patients with a CPS of 1 or more (Ibid). Among patients with a CPS of 1 or more, median PFS was 7.6 in the pembrolizumab-chemotherapy group and 5.6 months in the control group (Cortes, J., et al. Pembrolizumab plus chemotherapy versus placebo plus chemotherapy for previously untreated locally recurrent inoperable or metastatic triple-negative breast cancer (KEYNOTE-355): a randomised, placebo-controlled, double-blind, phase 3 clinical trial. The Lancet. 396 (10265), 1817-1828 (2020). https://doi.org/10.1016/S0140-6736(20)32531-9), a non-significant difference .(KEYNOTE-355 Final Analysis Reveals Survival Benefit With Pembrolizumab in Triple-Negative Breast Cancer. The ASCO Post. Accessed June 22, 2022. https://ascopost.com/issues/december-10-2021/keynote-355-final-analysis-reveals-survival-benefit-with-pembrolizumab-in-triple-negative-breast-cancer/)
At data cut-off as of June 2021, median follow-up was 44.1 months (Rugo, H.S., et al. KEYNOTE-355: Final results from a randomized, double-blind phase III study of first-line pembrolizumab + chemotherapy vs placebo + chemotherapy for metastatic TNBC. Ann of Onc. 32(5). (2021). https://oncologypro.esmo.org/meeting-resources/esmo-congress/keynote-355-final-results-from-a-randomized-double-blind-phase-iii-study-of-first-line-pembrolizumab-chemotherapy-vs-placebo-chemotherapy-for). These analyses showed a consistent PFS benefit in the treatment group as with prior analyses (Ibid). There was an improved ORR for patients with a CPS of 10 or more in the pembrolizumab-chemotherapy group (Ibid).
Adverse Effects
As of December 2019, rates of treatment-related adverse events (TRAEs) of grade 3 to 5 were 68% in the pembrolizumab-chemotherapy group and 67% in the control group (Cortes, J., et al. Pembrolizumab plus chemotherapy versus placebo plus chemotherapy for previously untreated locally recurrent inoperable or metastatic triple-negative breast cancer (KEYNOTE-355): a randomised, placebo-controlled, double-blind, phase 3 clinical trial. The Lancet. 396 (10265), 1817-1828 (2020). https://doi.org/10.1016/S0140-6736(20)32531-9). Results showed a statistically significant 27% reduction in the risk of death for patients whose tumours had a CPS of 10 or more and who received pembrolizumab in addition to chemotherapy (KEYNOTE-355 Final Analysis Reveals Survival Benefit With Pembrolizumab in Triple-Negative Breast Cancer. The ASCO Post. Accessed June 22, 2022. https://ascopost.com/issues/december-10-2021/keynote-355-final-analysis-reveals-survival-benefit-with-pembrolizumab-in-triple-negative-breast-cancer/). As of June 201, TRAEs of grade 3 to 5 were 68.1% in the pembrolizumab-chemotherapy group and 66.9% in the placebo-chemotherapy group (Rugo, H.S., et al. KEYNOTE-355: Final results from a randomized, double-blind phase III study of first-line pembrolizumab + chemotherapy vs placebo + chemotherapy for metastatic TNBC. Ann of Onc. 32(5). (2021). https://oncologypro.esmo.org/meeting-resources/esmo-congress/keynote-355-final-results-from-a-randomized-double-blind-phase-iii-study-of-first-line-pembrolizumab-chemotherapy-vs-placebo-chemotherapy-for). There were 2 deaths in the treatment group and 0 deaths in the placebo group. (Rugo, H.S., et al. KEYNOTE-355: Final results from a randomized, double-blind phase III study of first-line pembrolizumab + chemotherapy vs placebo + chemotherapy for metastatic TNBC. Ann of Onc. 32(5). (2021). https://oncologypro.esmo.org/meeting-resources/esmo-congress/keynote-355-final-results-from-a-randomized-double-blind-phase-iii-study-of-first-line-pembrolizumab-chemotherapy-vs-placebo-chemotherapy-for)
Impact of Treatment Options to Patients
By delaying the progression of the disease, pembrolizumab can relieve cancer-related symptoms, and improve a patient’s quality of life. Analyzed data from KEYNOTE-355 show support for pembrolizumab, in combination with chemotherapy, to be used in the first-line setting as a new standard-of-care for this patient population.
When living with no or with minimal cancer-related symptoms, and with minimal side effects from treatment, patients are able to reduce the impact of cancer on their ability to care for children and dependents, continue with their employment and earn income, spend time with loved ones and participate in their life in a meaningful way by engaging in social activities, travelling, maintaining friendships, and pursuing personal interests.
Value to Patients
The value to patients of extending the time that their cancer is progression-free cannot be overestimated. Patients living with metastatic breast cancer are aware that their advanced disease will progress with worsening symptoms until death, and embrace opportunities to try new treatments, even if benefits may be as little as a six month extension of progression-free disease. It is also very important for patients to have good quality of life when receiving treatment for metastatic disease. Patients that we speak to on a regular basis acknowledge the importance to have the energy to attend their children’s activities and to spend time with family and friends.
Experience With Drug Under Review
Given that this treatment is not yet widely accessible in Canada, CBCN was unfortunately unable to connect with, and interview, breast cancer patients with experience on the treatment.
Companion Diagnostic Test
At this time PD-L1 testing is not implemented routinely in breast cancer care in Canada. Accessing testing and treatment is of great importance for metastatic, triple negative breast cancer patients. It is imperative that all triple-negative metastatic/advanced breast cancer patients who could benefit from this therapy are being identified and offered PD-L1 testing to assess their eligibility for treatment with Keytruda. It is critical that access to adequate testing does not create a barrier for access to effective therapies for metastatic patients.
Anything Else?
We note that Keytruda , treats cancer patients based on the presence of a specific tumour biomarker. We hope that CADTH will consider continuing to engage the manufacturer and other stakeholders to develop novel approaches to support translation into models of assessment for potential value in clinical practice in Canada. Funding this type of molecularly targeted therapeutic would provide an important therapeutic option for metastatic and advanced triple-negative breast cancer patients who are in need of further treatment options.
Conflict of Interest Declaration — Canadian Breast Cancer Network
Did you receive help from outside your patient group to complete this submission? If yes, please detail the help and who provided it.
CBCN did connect with the manufacturer, Merck, to identify clinicians that could connect us with patients with experience on the treatment.
All other research, interviews and outreach to patients was conducted independently by the Canadian Breast Cancer Network, as was the compilation of information and data for the writing of this submission.
As a member of the Canadian Cancer Action Network, the Canadian Breast Cancer Network is committed to adhering to the Code of Conduct Governing Corporate Funding.
Did you receive help from outside your patient group to collect or analyze data used in this submission? If yes, please detail the help and who provided it.
No. The Canadian Breast Cancer Network compiled and wrote this submission independently.
List any companies or organizations that have provided your group with financial payment over the past two years AND who may have direct or indirect interest in the drug under review.
Table 1: Financial Disclosures for Canadian Breast Cancer Network (CBCN)
Company | Check Appropriate Dollar Range | |||
|---|---|---|---|---|
$0 to 5,000 | $5,001 to 10,000 | $10,001 to 50,000 | In Excess of $50,000 | |
Merck Canada | — | — | X | — |
Rethink Breast Cancer
About Rethink Breast Cancer
Rethink Breast Cancer (Rethink) is a Canadian charity known for making positive change. Rethink educates, empowers and advocates for system changes to improve the experience and outcomes of those with breast cancer, focusing on historically underserved groups: people diagnosed at a younger age, those with metastatic breast cancer and people systemically marginalized due to race, income or other factors. We foster spaces to connect, listen, empower and rethink breast cancer, together. Rethink’s strategic priorities and organizational direction are guided by the unique, unmet needs identified by breast cancer patients and their families.
Programs and Activities
Rethink Breast Cancer builds community, bringing patients with various stages of breast cancer together through our private and public social spaces as well as in-person events
Rethink runs patient retreats and provides peer-support and professional support
Rethink creates and runs education forums and conferences
Rethink creates support and education tools, resources and content
Rethink funds and supports breast cancer research
You can find out more by visiting:
Rethink Breast Cancer Instagram
Table 2: Financial Disclosure for Rethink Breast Cancer
Company | Check Appropriate Dollar Range | |||
|---|---|---|---|---|
$0 to 5,000 | $5,001 to 10,000 | $10,001 to 50,000 | In Excess of $50,000 | |
Merck (2021) | — | — | X | — |
Patient Profiles
Jen Pogue’s Profile
In June of 2020 I discovered a strange lump in my breast.
The next 8 months of medical check-ins, misdiagnoses and dismissals ultimately led to the blow that was February 2021. After months of hearing, “Don’t worry, it will go away, it’s just hormone related,” and, “You’re too young, no cancer in your immediate family so don’t sweat,” to eventually, “You should do a biopsy just to rule out cancer,” to the worst possible words I could hear: the mysterious lump was du novo stage 4 triple metastatic negative breast cancer (MTNBC) that had metastasized to my lung and sternum. Not only did I have one of the most aggressive types of cancer, it had already spread to my organs and spine.
I had recently turned 37, in the prime of my life, shortly after my second wedding anniversary with my amazing husband and the midst of trying to start our future family. And even in the middle of the pandemic, I was at the height of my career in the film and television industry, juggling multiple projects that I loved. I had no previous health conditions or qualms. I was, by all accounts, happy.
February 2021 changed all of that.
The weight of this shocking diagnosis completely knocked me off my feet. It turned my life upside down. As I learned more about breast cancer and what this kind of staging meant, it got even worse. Surgery and radiation were not on the table since it had already spread. Hormone therapy doesn’t apply to triple negative breast cancer since it won’t respond. The very nature of MTNBC made the small lump aggressively grow to more than 11 centimeters in such a short time span. “The size of a baseball,” as my husband put it. This was the very real weight and metaphorical heaviness that I carried.
My healthcare team said standard of care for stage 4 MTNBC was chemotherapy, but realistically it was just to slow the spread and would never fully stop it. Each chemo treatment has a shelf life of time until cancer will learn to work through it. Maybe 2-5 years of response for the most fortunate. I don’t really know how one reacts to hearing you likely have 2-5 years left to live, that statement is so surreal. Every Google search, every blog post, every breast cancer survivor I reached out to for advice confirmed what I could not fathom: stage 4 MTNBC has no cure, just the faint hope that medicine can slow it down, through a barrage of qualityof-life compromising treatments, praying to get the maximum amount of time from each chemo course as you can.
Living your life in this kind of existential dread is not living. Not knowing your un-confirmed departure date, but knowing you’ve already purchased a ticket is the most harrowing way to live. It is navigating a tornado of desperation, hysteria, grief, fear, resentfulness, and daily depression, all while grasping at straws of hope you can never really get a grip on. You mourn the loss of tomorrows and are incessantly plagued by the dark cloud of inevitability.
I immediately left my jobs and unloaded all responsibilities I carried so I could focus on this one thing: to get better against all odds. In this, I acknowledge that I am in a privileged position of being a white cis-female with a loving family and supportive friends. I know not everyone has this economic privilege, and their MTNBC journey is even more difficult. This is why hope needs to be for everyone, but in cancer, it is so elusive and fleeting.
I began mourning my dreams for family planning and so much more. My loved ones and I started preparing for what now would likely be my so-called, short-term future, one that revolved around constant sickness and impeding frailness until the inevitable end… Until the very slight glimmer of hope that I desperately sought, showed itself.
In a miracle of timing, I was accepted into a clinical trial at Princess Margaret Cancer Centre that studies that combination of chemotherapy (carboplatin and gemcitabine) + pembrolizumab (Keytruda) immunotherapy, which are intervened together on a regular schedule. As I came to learn, the goal of this study is for the less-harsh-on your-body Keytruda to teach my immune system to fight new cancer cells on its own. A treatment so new that there are no survival rate statistics, but there are several patients who have gone through Keytruda trials and have been off any treatment entirely for a few years now, the nurses assured me. I cannot explain the kind of game-changing information this was to me; it changed EVERYTHING. Just knowing that the possibility of a treatment-free future was there again, no matter how long it was going to take, no matter the effects, was the fuel I needed to grin and bear, suit up and get to work at it.
When I finally started the clinical trial course in April 2021, the results from Keytruda were almost immediate: my then 11 cm primary breast tumour immediately shrunk 50% of what it was. Within 6 months, my CT scans could not trace the primary tumour whatsoever, and my lymph nodes and lung lesions had shrunk to practically nothing and stabilized. I was eventually told that my spine lesions had likely become benign, and the scans were just picking up the scarring. These results revitalized me. I slowly felt human again, after months of being a pincushion.
I’m now 16 months into the trial that will continue until September 2023, and the disease has stayed asleep and in ironic medical terms, unremarkable. My amazing team at Princess Margaret make no promises, but have stated, “This is the best possible response you could have hoped for.” I’m far from my treatment-free goal, but the relief of having little to no side effects makes this prolonged process completely manageable. And there’s that word again: I feel hopeful.
When I was originally diagnosed, my oncologist told me there was nothing I did to cause this, that I was just “lucky.” I certainly didn’t feel lucky to have been blindsided with a sudden disease this extreme, but luck showed itself with the opportunity for Keytruda. I now know how fortunate I am to have had access to this trial treatment exactly right when I needed it and have it as my first line of treatment before the trial doors shut. Lucky to have responded as rapidly as I did. Lucky to now sit in routine oncology appointments where we talk about my future and my options, rather than the prominent doom and gloom of early 2021. Lucky to remain relatively healthy and mentally strong as Keytruda has allowed me to bounce back to my pre-cancer days of running, biking, hiking, hosting friends, staying mentally engaged in my work, and much more. Lucky that Keytruda allowed me to move around my world with the same healthy appearance, rather than coping with extreme hair-loss or neuropathy or other adverse-chemo related side effects I hear about from many others. Beyond lucky to be back to some normalcy, having my working and everyday life scheduled around my treatments, rather than finalizing my goodbyes. Keytruda has been clinically, emotionally, physically transformative for me. And I feel this could be true for others too.
As one of the rarer forms of breast cancer, the MTNBC community is small, but has a mighty voice and presence. Through support organizations such as Rethink, online forums, and social media, I have connected to so many others at varying degrees of treatments who share very openly and honestly. As far as I’ve found, I am the only one I know who has access to Keytruda in Canada, and has their sights set on a treatment-free future. I am both lucky and hopeful, when so many aren’t either. While I personally and privately celebrate my wins, it’s devastating to witness my MTNBC friends suffer through one ineffective chemo treatment to the next, while knowing first-hand that there’s a Keytruda immunotherapy treatment that exists that could literally change their lives.
Hope should not be tied with how lucky you are.
In Canada, this “Universal Hope” should be accessible to all. And in the form of Keytruda immunotherapy as standard of care, this would give the metastatic triple negative breast cancer community the hope it deserves.
Jen Pogue
Kim Angell’s Profile
My name is Kim Angell and I am a metastatic breast cancer thriver, patient advocate and avid hiker from Vancouver Island, BC. I was originally diagnosed with stage 2 hormone positive breast cancer in 2016 and was nearing the 5-year mark when my life came crashing down. On March 12, 2021, I found out the cancer had returned as metastatic with multiple lesions scattered through my spine, hips and ribs. I was young, healthy, and felt like I was just starting to put the thoughts of cancer behind me. Yet, suddenly I was now having to face my own mortality at just 38 years old.
My life quickly changed from being focused on advancing my career to focusing on keeping myself alive. I suddenly found myself entrenched in the world of MBC, educating myself on the disease, what treatments were available, finding connections and stories of hope from others while also being faced with the harsh reality as I watched this disease take their lives.
I was quickly thrown back into the life of a cancer patient, this time as a forever patient, and was put on what was considered to be the latest and greatest treatment for hormone receptor positive disease. I was encouraged by the advances in research and the fact that others like me were living with this disease for over 5+ years. A bittersweet glimmer of hope in the grand scheme of things.
As I went through a series of scans though following my diagnosis, I found out that the cancer wasn’t just confined to the bones, it had now spread to my liver as well. I advocated to have a liver biopsy done to determine if the cancer was still hormone positive even though I was told that it was rare to lose receptors. After an unsuccessful biopsy attempt and more progression in my liver, they went in a second time and were able to finally get the sample they needed.
My stomach dropped as I read the pathology report – the cancer had lost all hormone expression and I had now flipped to triple negative disease with a much poorer prognosis. It’s already hard enough going through this disease knowing the average median survival for MBC patients but knowing that I now had triple negative disease felt like an immediate death sentence. It’s not only a more aggressive breast cancer subtype, but it also meant I no longer had access to targeted therapies such as CDK4/6 inhibitors and hormone therapies. My only option at this point was chemotherapy.
Chemotherapy would kill the rapidly dividing cancer cells, but also kill other healthy cells. It brings side effects like the trauma of losing my hair, dealing with chronic skin and nail infections, and struggling to absorb any nutrients due to the lining of my gut being damaged from treatment — chemotherapy is not the option that gives me the best quality of life. All of this added to an already traumatic experience.
So, I tried desperately to get on a clinical trial but faced a series of roadblocks. Since I had been previously treated for MBC, I was excluded from numerous trials despite having a completely different subtype. I lost hope as the doors kept closing on me, feeling like I was being excluded from access to potentially life extending medications because of my own unique situation with MBC.
I began running out of time. The cancer was progressing rapidly in my liver and I risked it spreading elsewhere in my body being off treatment for weeks but what felt like an eternity. I ultimately had to accept the fact that I could not access these same treatments that others had access to in neighbouring countries due to the length of time that it was taking to be approved through our medical system and due to the restricting nature of the inclusion/exclusion criteria of these trials.
I often wonder if I had access to immunotherapy, if it would have provided another treatment option and extended my overall survival. Worrying with the limited amount of treatment options for MTNBC, that I will run out of treatment options one day. That my team will have to face me one day and tell me that they’ve done all they can do but there’s nothing else available. It’s a devastating reality knowing that I still have so much fight in me left but that I could reach the end one day because there was one less option to give me more time.
Kim Angell
MBC Patient Survey Results
Information for this report was gathered through an online survey published in English and circulated through communications from Rethink Breast Cancer as well as the Rethink Network and other partner organizations. Messages were also posted on Facebook and Twitter as well as the Breastcancer.org, Cancer Connection and Cancer Survivors Network online discussion forums. 78 metastatic breast patients completed the survey between September 2018 and April 2019.
An independent contractor was hired to develop this survey and present the results. Survey questions were all reviewed by Rethink staff and Metastatic Patient Advisory Board prior to being posted online.
Rethink Breast Cancer asked respondents to evaluate the importance of different outcomes for their breast cancer treatment on a scale of 1 (not important) to 5 (very important). All the listed outcomes were considered important with no average scores lower than 4.4. However, controlling disease and extending life expectancy were rated as the most important results suggesting that patient values prioritize long-term health outcomes over immediate concerns like reducing symptoms or managing side effects.
Table 3: Importance of Outcomes
Importance of outcome | 1 - not important | 2 | 3 | 4 | 5 – very important | Average |
|---|---|---|---|---|---|---|
Controlling disease progression | 0.00% 0 | 0.00% 0 | 0.00% 0 | 2.60% 2 | 97.40% 75 | 4.97 77 |
Reducing symptoms | 1.30% 1 | 0.00% 0 | 12.99% 10 | 19.48% 15 | 66.23% 51 | 4.49 77 |
Maintaining quality of life | 0.00% 0 | 0.00% 0 | 1.30% 1 | 12.99% 10 | 85.71% 66 | 4.84 77 |
Managing side effects | 1.30% 1 | 1.30% 1 | 12.99% 10 | 19.48% 15 | 64.94% 50 | 4.45 77 |
Achieving NED (no evidence of disease) | 1.32% 1 | 1.32% 1 | 1.32% 1 | 6.58% 5 | 89.47% 68 | 4.82 76 |
Extending life expectancy | 0.00% 0 | 0.00% 0 | 0.00% 0 | 2.63% 2 | 97.37% 74 | 4.97 76 |
Comments included:
Symptoms and shrinking the cancer is the most important thing. Living well is the next most important thing.
Keep me alive for my kids.
I want to live, LIVE and enjoy my life for many more years and not be so afraid.
When asked if they would be willing to tolerate new side effects from drugs that can control disease progression or prevent recurrence on a scale of 1 (will not tolerate side effects) to 10 (will tolerate significant side effects), respondents gave an average score of 7.5 (n=78) with only four respondents giving a score lower than 5. When asked the same question about new drugs that could prolong life expectancy, the average score was 7.7 (n=77) with only five respondents giving a score below 5. These results would support the conclusion that patient values prioritize long-term health outcomes.
However, it should be noted that a number of respondents indicated that this tolerance was not absolute - there was a limit to how much they could take. Some of the comments include:
I will take on the most shitty things this disease can through at me.....until I am ready to go. I love my life .
I’ll try so long as I can remain mobile and find joy in things.
I can tolerate side effects but I need it to be tolerable.
If it means a longer, better life I would be willing.
Conflict of Interest Declaration — Rethink Breast Cancer
To maintain the objectivity and credibility of the CADTH reimbursement review process, All Patients in the drug review processes must disclose any real, potential, or perceived conflicts of interest. This Patient Group Conflict of Interest Declaration is required for participation. Declarations made do not negate or preclude the use of the patient group input. CADTH may contact your group with further questions, as needed.
Did you receive help from outside your patient group to complete this submission? If yes, please detail the help and who provided it.
No.
Did you receive help from outside your patient group to collect or analyze data used in this submission? If yes, please detail the help and who provided it.
No.
List any companies or organizations that have provided your group with financial payment over the past 2 years AND who may have direct or indirect interest in the drug under review.
Table 4: Financial Disclosure for Rethink Breast Cancer
Company | Check Appropriate Dollar Range | |||
|---|---|---|---|---|
$0 to 5,000 | $5,001 to 10,000 | $10,001 to 50,000 | In Excess of $50,000 | |
Merck | — | — | X | — |
Clinician Group Input
Canadian Breast Cancer Medical Oncologists, Lead by The Ottawa Hospital Cancer Centre
About Canadian Breast Cancer Medical Oncologists, Lead by The Ottawa Hospital Cancer Centre
We are medical oncologists treating breast cancer at the Ottawa Hospital Cancer Centre, BC Cancer Agency, and the Tom Baker Cancer Centre (Calgary AB). The group consists of medical oncologists throughout Canada with an expertise in breast oncology and in particular systemic therapies in advanced, triple negative breast cancer.
Information Gathering
Ongoing review of emerging data relevant to this file, including from ASCO,ESMO, and SABCS conferences in 2021 and 2022, and the associated publication of the Keynote 355 data. Local and regional consensus meetings/rounds and shared online development of input into this submission’s content.
Current Treatments and Treatment Goals
Current Canadian treatment paradigm: Patients with metastatic or locoregionally advanced unresectable metastatic triple negative breast cancer are treated:
In the first line, previously untreated setting: o If a brca mutation is present, PARP inhibition is considered but not yet publicly funded (olaparib), and can be applied in later lines with less established value. It is unlikely that our patients will receive local jurisdiction funding for PARP inhibition and therefore this is not a viable option given the expensive out of pocket cost for patients.
otherwise, we use chemotherapy:
in the setting of aggressive disease with visceral crisis (life threatening disease burden), doublets of 2 chemotherapy agents such as anthracycline/taxane or platinum/taxane combinations
for other cases, sequential single agents are used
If previous (neo)/adjuvant systemic chemotherapy (eg a taxane and anthracycline) received over 12 months prior, one of those agents can be initially used with crossover to the other upon disease progression (unless there are contraindications, disease progression in the early disease setting, or persisting toxicities of that agent). If anthracyclines and taxanes had been used in the early disease setting within 12 months, we move on to the agents listed in (3) below
In the 3rd line setting (or 2nd line if taxane used recently in the early disease setting), sacituzumab-govitecan, an antibody drug conjugate, is now the standard of care but it also is not yet funded publicly.
Subsequent lines of chemotherapy include sequential single agents including: platinum (carboplatin ± gemcitabine), eribulin, vinorelbine, capecitabine
For any line, participation in relevant and applicable clinical trials is always considered.
With every disease progression event, there is a dramatic attrition rate of patients no longer well enough to try the “next line” of therapy, limiting the value of later lines.
Treatment Gaps (Unmet Needs)
Considering the treatment goals, please describe goals (needs) that are not being met by currently available treatments.
Metastatic triple negative breast cancer has the worst outcomes of all of the major subtypes of breast cancer, in terms of duration of response and overall survival (median ~1.5 years). There has long been a desperate need for more effective therapy in this setting. There is also a greater propensity for mTNBC patients to develop visceral crises and brain metastases. Current chemotherapy drugs offer modest short term benefits and public funding for olaparib and sacituzumab-govitecan are still not realities.
Place in Therapy
How would the drug under review fit into the current treatment paradigm?
For patients fitting the indication described above, pembrolizumab would be offered in the first line metastatic (or locally advanced unresectable) setting together with chemotherapy (with either paclitaxel, nab-paclitaxel (uncommonly) or carboplatin/gemcitabine), supplanting standard first line chemotherapy options listed above in 3 (subsections 1 and 2). The use of pembrolizumab is also biomarker driven with efficacy seen in tumours expressing PD-L1 CPS score >10.
Which patients would be best suited for treatment with the drug under review? Which patients would be least suitable for treatment with the drug under review?
Patients best suited for first line pembrolizumab with chemotherapy (as in KN 355) would include any patient with a PD-L1 CPS expression of ≥ 10 (using a validated assay), regardless of organ involvement, if ECOG performance status 0-2 and in the absence of absolute or strong relative contraindications to immunotherapy.
Patients least suitable would be those in other lines of therapy, those who had received neo/adjuvant pembrolizumab for early stage disease within 12 months, and those with pre-existing active uncontrolled autoimmune disorders. Immunotherapies have been well established in the treatments of other cancers (melanoma, lung cancer, …) and practitioners are adept at selecting patients whose pre-existing conditions would likely make the risk:benefit ratio for pembrolizumab unacceptable (myasthenia gravis, multiple sclerosis, cardiac/liver transplants on immunosuppressants). Treated or inactive past autoimmune diseases (rheumatoid arthritis, psoriasis, thyroid disorders, colitis) would not be absolute contraindications.
What outcomes are used to determine whether a patient is responding to treatment in clinical practice? How often should treatment response be assessed?
Responses are determined based on symptoms, laboratory markers, radiographic scans and tumour measurements, with scans usually performed at least every 3 months initially. Treatment is continued if disease is either stable or responding radiographically (by RECIST criteria) or clinically. Clinically meaningful responses would be suggested by:
Reduction in the frequency or severity of symptoms (eg pain, dyspnea…)
Improvement of organ function (bone, liver, lung)
Stabilization of symptoms
Maintenance or improvement of performance status
Tumour radiographic response with either stabilization of disease or response by RECIST criteria
What factors should be considered when deciding to discontinue treatment with the drug under review?
Disease progression
Intolerable or dangerous toxicity, esp immune mediated adverse events of grade 3 (if not resolving with treatment to grade 1) or any grade 4 events
Patient preference or refusal
What settings are appropriate for treatment with [drug under review]? Is a specialist required to diagnose, treat, and monitor patients who might receive [drug under review]?
Hospital setting or specialty clinic that has expertise and staffing (chemotherapy nurses, oncology pharmacists) to administer systemic cancer therapies and monitor / manage treatment-related toxicities
Additional Information
The benefits seen in the KN 355 study are meaningful and practice changing. Median progression free survival was 4 months longer, and median overall survival was improved by 5 months and benefit was seen across subgroups analyzed. This approach has been accepted as a new standard of care in internationally accepted guidelines (European Society of Medical Oncology, NCCN). When the regimen has been used in practice (through private pay or compassionate mechanisms), we have found it to be tolerated well with a manageable toxicity profile and highly accepted and valued by patients. There is a very favorable risk/benefit (efficacy vs toxicity) ratio with this drug and improving median survival by 5 months is not only clinically meaningful, but also desired by most patients given the very aggressive nature of this breast cancer subtype. This is a step in the right direction for our patients and oncologists alike.
Immunotherapy trials over the last several years have clearly demonstrated that any additional value is noted when applied in the first line metastatic setting. When used with subsequent lines, it’s additional value is very limited.
Conflict of Interest Declarations — Canadian Breast Cancer Medical Oncologists, lead by The Ottawa Hospital Cancer Centre
To maintain the objectivity and credibility of the CADTH drug review programs, all participants in the drug review processes must disclose any real, potential, or perceived conflicts of interest. This conflict of interest declaration is required for participation. Declarations made do not negate or preclude the use of the clinician group input. CADTH may contact your group with further questions, as needed. Please see the Procedures for CADTH Drug Reimbursement Reviews (section 6.3) for further details.
Did you receive help from outside your clinician group to complete this submission? If yes, please detail the help and who provided it.
No
Did you receive help from outside your clinician group to collect or analyze any information used in this submission? If yes, please detail the help and who provided it.
No
List any companies or organizations that have provided your group with financial payment over the past two years AND who may have direct or indirect interest in the drug under review.
Declaration for Clinician 1
Name: Dr Sandeep Sehdev
Position: MD FRCPC Medical Oncologist, Assistant Professor, The Ottawa Hospital Cancer Centre, lead of breast cancer disease site group
Date: July 10, 2022
Table 5: Conflict of Interest Declaration for Canadian Breast Cancer Medical Oncologists — Clinician 1
Company | Check appropriate dollar range | |||
|---|---|---|---|---|
$0 to $5,000 | $5,001 to $10,000 | $10,001 to $50,000 | In Excess of $50,000 | |
Gilead | X | — | — | — |
Merck | X | — | — | — |
AstraZeneca | — | X | — | — |
Declaration for Clinician 2
Name: Dr Katherine Cole
Position: MDCM FRCPC Medical Oncology The Ottawa Hospital Cancer Centre
Date: July 12, 2022
Table 6: Conflict of Interest Declaration for Canadian Breast Cancer Medical Oncologists — Clinician 2
Company | Check appropriate dollar range | |||
|---|---|---|---|---|
$0 to $5,000 | $5,001 to $10,000 | $10,001 to $50,000 | In Excess of $50,000 | |
Gilead | X | — | — | — |
Merck | X | — | — | — |
AstraZeneca | X | — | — | — |
Declaration for Clinician 3
Name: Dr Jan-Willem Henning
Position: Medical Oncologist, Breast and Sarcoma Tumour Groups, Tom Baker Cancer Centre, Calgary AB, Cumming School of Medicine, U of Calgary. Medical Co-Lead, Sarcoma Tumour Group and Adolescent and Young Adult Southern Alberta Program, Alberta Health Services, Cancer Care Alberta
Date: July 13 2022
Table 7: Conflict of Interest Declaration for Canadian Breast Cancer Medical Oncologists — Clinician 3
Company | Check appropriate dollar range | |||
|---|---|---|---|---|
$0 to $5,000 | $5,001 to $10,000 | $10,001 to $50,000 | In Excess of $50,000 | |
Gilead | X | — | — | — |
Merck | X | — | — | — |
AstraZeneca | X | — | — | — |
Pfizer | X | — | — | — |
Novartis | X | — | — | — |
Seagen | X | — | — | — |
Lilly | X | — | — | — |
Declaration for Clinician 4
Name: Dr Mark Clemons
Position: Medical Oncologist, Ottawa Hospital Cancer Centre, Professor U of Ottawa
Date: July 13 2022
Table 8: Conflict of Interest Declaration for Canadian Breast Cancer Medical Oncologists — Clinician 4
Company | Check appropriate dollar range | |||
|---|---|---|---|---|
$0 to $5,000 | $5,001 to $10,000 | $10,001 to $50,000 | In Excess of $50,000 | |
None | — | — | — | — |
Declaration for Clinician 5
Name: Dr Moira Rushton-Marovac
Position: MD FRCPC, Assistant Professor, U of Ottawa, Medical Oncologist (Ottawa Hospital Cancer Centre). Senior investigator, Canadian Cancer Trials Group
Date: July 13 2022
Table 9: Conflict of Interest Declaration for Canadian Breast Cancer Medical Oncologists — Clinician 5
Company | Check appropriate dollar range | |||
|---|---|---|---|---|
$0 to $5,000 | $5,001 to $10,000 | $10,001 to $50,000 | In Excess of $50,000 | |
None | — | — | — | — |
Declaration for Clinician 6
Name: Dr Karen Gelmon
Position: MD FRCPC Medical Oncologist, Professor, Univ of British Columbia, BC Cancer Agency, Vancouver BC
Date: July 10, 2022
Table 10: Conflict of Interest Declaration for Canadian Breast Cancer Medical Oncologists — Clinician 6
Company | Check appropriate dollar range | |||
|---|---|---|---|---|
$0 to $5,000 | $5,001 to $10,000 | $10,001 to $50,000 | In Excess of $50,000 | |
Gilead | X | — | — | — |
Merck | X | — | — | — |
AstraZeneca | — | X | — | — |
Ontario Health (CCO) Breast Cancer Drug Advisory Committee
About the Ontario Health (CCO) Breast Cancer Drug Advisory Committee
OH-CCO’s Drug Advisory Committees provide timely evidence-based clinical and health system guidance on drug-related issues in support of CCO’s mandate, including the Provincial Drug Reimbursement Programs (PDRP) and the Systemic Treatment Program.
Information Gathering
Information was jointly discussed at a DAC meeting.
Current Treatments and Treatment Goals
Treatment of TNBC is challenging, as these tumours lack targets for therapeutic intervention. Cytotoxic chemotherapy remains the standard systemic treatment for most patients; however, the benefit may be limited. The DAC would like to highlight that there are issues with pathology testing turnaround times within some centers. Clinicians should be allowed to prescribe chemotherapy while waiting for a CPS test and adding in pembrolizumab if the CPS is greater than or equal to 10.
Treatment Gaps (Unmet Needs)
Considering the treatment goals, please describe goals (needs) that are not being met by currently available treatments.
TNBC behaves more aggressively, with earlier relapses and poorer survival outcomes. The median survival in the KEYNOTE-355 study control group was only 16 months. The addition of pembrolizumab had a clinically very meaningful impact.
Currently, there is a lack of CPS testing within the province and test results may be delayed.
Place in Therapy
How would the drug under review fit into the current treatment paradigm?
Pembrolizumab would fit into first line.
Which patients would be best suited for treatment with the drug under review? Which patients would be least suitable for treatment with the drug under review?
Patients best suited for the treatment would align with the KEYNOTE trial inclusion criteria; including CPS greater than or equal to10 and time from completion of adjuvant treatment, which is greater than 6 months.
Patients least suited would include patients that are high risk of adverse toxicity related to immunotherapy.
What outcomes are used to determine whether a patient is responding to treatment in clinical practice? How often should treatment response be assessed?
As per standard of care. Treatment response should be assessed at least every 3 months at the beginning of treatment.
What factors should be considered when deciding to discontinue treatment with the drug under review?
Disease progression and toxicity.
What settings are appropriate for treatment with [drug under review]? Is a specialist required to diagnose, treat, and monitor patients who might receive [drug under review]?
Hospital (outpatient clinic) is an appropriate setting. Patients should have access to clinicians experienced in the assessment and management of immunotherapy toxicity.
Additional Information
N/A
Conflict of Interest Declarations — Ontario Health (CCO) Breast Cancer Drug Advisory Committee
To maintain the objectivity and credibility of the CADTH drug review programs, all participants in the drug review processes must disclose any real, potential, or perceived conflicts of interest. This conflict of interest declaration is required for participation. Declarations made do not negate or preclude the use of the clinician group input. CADTH may contact your group with further questions, as needed. Please see the Procedures for CADTH Drug Reimbursement Reviews (section 6.3) for further details.
Did you receive help from outside your clinician group to complete this submission? If yes, please detail the help and who provided it.
Yes. Ontario Health provided secretariat function to the DAC.
Did you receive help from outside your clinician group to collect or analyze any information used in this submission? If yes, please detail the help and who provided it.
No.
List any companies or organizations that have provided your group with financial payment over the past two years AND who may have direct or indirect interest in the drug under review. Please note that this is required for each clinician who contributed to the input — please add more tables as needed (copy and paste). It is preferred for all declarations to be included in a single document.
Declaration for Clinician 1
Name: Dr. Andrea Eisen
Position: Ontario Health (CCO) Breast Cancer Drug Advisory Committee Lead
Date: 11/07/2022
Table 11: Conflict of Interest Declaration for Ontario Health (CCO) Breast Cancer Drug Advisory Committee — Clinician 1
Company | Check appropriate dollar range | |||
|---|---|---|---|---|
$0 to $5,000 | $5,001 to $10,000 | $10,001 to $50,000 | In Excess of $50,000 | |
N/A | — | — | — | — |
Provincial Breast Tumour Group (Alberta)
About the Provincial Breast Tumour Group (Alberta)
We represent medical oncologists in Alberta, with representation from Tom Baker Cancer Centre (Dr. Nancy Nixon) and Cross Cancer Institute (Dr. Karen King). The provincial breast tumour group is responsible for treating patients with triple negative breast cancer (TNBC) in Alberta.
Information Gathering
Thorough review of the literature and treatment guidelines.
Current Treatments and Treatment Goals
The current standard of care treatment in the first line for metastatic triple negative breast cancer (TNBC) is single agent chemotherapy. The choice of chemotherapy would depend on whether the patient received treatment in the adjuvant setting, and the duration of time between adjuvant therapy and recurrence. Typically, we would consider a taxane (i.e. paclitaxel) or non-taxane if the patient had a recurrence within 12 months of their curative intent treatment. Patients may also be eligible for radiation if they have symptomatic disease for palliation. There are not any drugs currently being supported by clinical guidelines that do not have Health Canada approval.
Current treatments are given with the goal to delay progression and improve both duration and quality of life. Since metastatic disease is not curable, the goal of the treatments are palliative in nature.
Treatment Gaps (Unmet Needs)
Considering the treatment goals, please describe goals (needs) that are not being met by currently available treatments.
The current available options for patients with advanced TNBC have limitations both in efficacy, and tolerability. Therefore, there is an urgent need for treatments that have better efficacy in addition to fewer toxicities.
Place in Therapy
How would the drug under review fit into the current treatment paradigm?
Pembrolizumab is a checkpoint inhibitor that blocks the interaction between PD-1 and PD-L1, which is a mechanism by which tumour cells evade the immune system. Blocking this interaction allows for tumour cells to be targeted by the body’s own immune system. It is used in combination with chemotherapy for first line therapy. This combination treats the underlying disease process by effectively killing cancer cells.
Pembrolizumab would be expected to shift the current treatment paradigm as indicated by current treatment guidelines (ASCO, ESMO) which consider this to be standard of care. Based on this, it would not be appropriate to try patients on other treatments before initiating a standard of care therapy.
Which patients would be best suited for treatment with the drug under review? Which patients would be least suitable for treatment with the drug under review?
Patients who have tumours that express PD-L1 (with a combined positive score >10) are those that would be eligible for treatment on the basis that they have the greatest response. Thus the companion diagnostic of PD-L1 measurement is required to select patients for treatment. For patients with metastatic TNBC that do not have a CPS≥10 would not be suitable for treatment.
What outcomes are used to determine whether a patient is responding to treatment in clinical practice? How often should treatment response be assessed?
Clinical and radiographic means will be used to determine patient response. Symptoms related to disease burden (e.g. pain) should improve on treatment. Radiographically, we would expect disease stability or response.
What factors should be considered when deciding to discontinue treatment with the drug under review?
Factors that would lead to discontinuation:
Disease progression
Intolerance to medication
Grade III or higher immune-mediated toxicity (e.g. adrenal insufficiency, liver enzyme elevation, diarrhea, pneumonitis)
What settings are appropriate for treatment with [drug under review]? Is a specialist required to diagnose, treat, and monitor patients who might receive [drug under review]?
Treatment would be provided under the guidance of a medical oncologist at a cancer clinic. This would be in the outpatient setting.
Additional Information
Triple negative breast cancer is an aggressive subtype of a common disease. One in 8 women is diagnosed with breast cancer in the course of her lifetime, close to 30% of which experience a metastatic recurrence. Of these, 10-15% are triple negative. Pembrolizumab is now recognized as a global standard for first line therapy, and it is imperative that Canadians have access to this medication in order to meet this standard.
Conflict of Interest Declarations — Provincial Breast Tumour Group (Alberta)
To maintain the objectivity and credibility of the CADTH drug review programs, all participants in the drug review processes must disclose any real, potential, or perceived conflicts of interest. This conflict of interest declaration is required for participation. Declarations made do not negate or preclude the use of the clinician group input. CADTH may contact your group with further questions, as needed. Please see the Procedures for CADTH Drug Reimbursement Reviews (section 6.3) for further details.
Did you receive help from outside your clinician group to complete this submission? If yes, please detail the help and who provided it.
No
Did you receive help from outside your clinician group to collect or analyze any information used in this submission? If yes, please detail the help and who provided it.
No
List any companies or organizations that have provided your group with financial payment over the past two years AND who may have direct or indirect interest in the drug under review. Please note that this is required for each clinician who contributed to the input — please add more tables as needed (copy and paste). It is preferred for all declarations to be included in a single document.
Declaration for Clinician 1
Name: Nancy Nixon
Position: Medical Oncologist
Date: 11-Jul-2022
Table 12: Conflict of Interest Declaration for Provincial Breast Tumour Group (Alberta) — Clinician 1
Company | Check appropriate dollar range | |||
|---|---|---|---|---|
$0 to $5,000 | $5,001 to $10,000 | $10,001 to $50,000 | In Excess of $50,000 | |
Astra Zeneca | X | — | — | — |
Pfizer | X | — | — | — |
Merck | X | — | — | — |
Novartis | X | — | — | — |
Roche | X | — | — | — |
Seagen | X | — | — | — |
Exact Sciences | X | — | — | — |
Gilead | X | — | — | — |
Declaration for Clinician 2
Name: Karen King
Position: Medical Oncologist
Date: 12 July 2022
Table 13: Conflict of Interest Declaration for Provincial Breast Tumour Group (Alberta) — Clinician 2
Company | Check appropriate dollar range | |||
|---|---|---|---|---|
$0 to $5,000 | $5,001 to $10,000 | $10,001 to $50,000 | In Excess of $50,000 | |
Astra Zeneca | X | — | — | — |
Novartis | X | — | — | — |
Roche | X | — | — | — |
Pfizer | X | — | — | — |
Merck | X | — | — | — |
Exact Sciences | X | — | — | — |
Gilead | X | — | — | — |
ISSN: 2563-6596
Disclaimer: The information in this document is intended to help Canadian health care decision-makers, health care professionals, health systems leaders, and policy-makers make well-informed decisions and thereby improve the quality of health care services. While patients and others may access this document, the document is made available for informational purposes only and no representations or warranties are made with respect to its fitness for any particular purpose. The information in this document should not be used as a substitute for professional medical advice or as a substitute for the application of clinical judgment in respect of the care of a particular patient or other professional judgment in any decision-making process. The Canadian Agency for Drugs and Technologies in Health (CADTH) does not endorse any information, drugs, therapies, treatments, products, processes, or services.
While care has been taken to ensure that the information prepared by CADTH in this document is accurate, complete, and up-to-date as at the applicable date the material was first published by CADTH, CADTH does not make any guarantees to that effect. CADTH does not guarantee and is not responsible for the quality, currency, propriety, accuracy, or reasonableness of any statements, information, or conclusions contained in any third-party materials used in preparing this document. The views and opinions of third parties published in this document do not necessarily state or reflect those of CADTH.
CADTH is not responsible for any errors, omissions, injury, loss, or damage arising from or relating to the use (or misuse) of any information, statements, or conclusions contained in or implied by the contents of this document or any of the source materials.
This document may contain links to third-party websites. CADTH does not have control over the content of such sites. Use of third-party sites is governed by the third-party website owners’ own terms and conditions set out for such sites. CADTH does not make any guarantee with respect to any information contained on such third-party sites and CADTH is not responsible for any injury, loss, or damage suffered as a result of using such third-party sites. CADTH has no responsibility for the collection, use, and disclosure of personal information by third-party sites.
Subject to the aforementioned limitations, the views expressed herein are those of CADTH and do not necessarily represent the views of Canada’s federal, provincial, or territorial governments or any third party supplier of information.
This document is prepared and intended for use in the context of the Canadian health care system. The use of this document outside of Canada is done so at the user’s own risk.
This disclaimer and any questions or matters of any nature arising from or relating to the content or use (or misuse) of this document will be governed by and interpreted in accordance with the laws of the Province of Ontario and the laws of Canada applicable therein, and all proceedings shall be subject to the exclusive jurisdiction of the courts of the Province of Ontario, Canada.
The copyright and other intellectual property rights in this document are owned by CADTH and its licensors. These rights are protected by the Canadian Copyright Act and other national and international laws and agreements. Users are permitted to make copies of this document for non-commercial purposes only, provided it is not modified when reproduced and appropriate credit is given to CADTH and its licensors.
Redactions: Confidential information in this document may be redacted at the request of the sponsor in accordance with the CADTH Drug Reimbursement Review Confidentiality Guidelines
Stakeholder Input: The views expressed in each submission are those of the submitting organization or individual; not necessarily the views of CADTH or of other organizations. As such, they are independent of CADTH and do not necessarily represent or reflect the view of CADTH. No endorsement by CADTH is intended or should be inferred. By filing with CADTH, the submitting organization or individual agrees to the full disclosure of the information. CADTH does not edit the content of the submissions.
CADTH does use reasonable care to prevent disclosure of personal information in posted material; however, it is ultimately the submitter’s responsibility to ensure no identifying personal information or personal health information is included in the submission. The name of the submitting organization or individual and all conflict of interest information are included in the submission; however, the name of the author, including the name of an individual patient or caregiver submitting the patient input, are not posted.
Accessibility: CADTH is committed to treating people with disabilities in a way that respects their dignity and independence, supports them in accessing material in a timely manner, and provides a robust feedback process to support continuous improvement. All materials prepared by CADTH are available in an accessible format. Where materials provided to CADTH by a submitting organization or individual are not available in an accessible format, CADTH will provide a summary document upon request. More details on CADTH’s accessibility policies can be found here.
About CADTH: CADTH is an independent, not-for-profit organization responsible for providing Canada’s health care decision-makers with objective evidence to help make informed decisions about the optimal use of drugs, medical devices, diagnostics, and procedures in our health care system.
Funding: CADTH receives funding from Canada’s federal, provincial, and territorial governments, with the exception of Quebec.